Options For Treating Diabetic Ulcers
Diabetic ulcers are open wounds that most commonly develop on the feet. While anyone can get an ulcer, individuals with diabetes are particularly at risk for them due to poor circulation in the extremities. Approximately fifteen percent of diabetes patients will develop a foot ulcer at some point during their lives. Of these, six percent will need treatment at the hospital due to complications from the ulcer. Diabetic ulcers typically form following a minor injury to the foot. Blisters, small cuts, and scrapes all have the potential to develop into ulcers. While foot ulcers can be painful, many patients with diabetes have trouble sensing pain in their feet and often do not report any pain from their ulcers.
One of the first signs of an ulcer is usually fluid or discharge a patient notices on their socks. The tissue around an ulcer may also be discolored and can even turn black. If not treated, foot ulcers may lead to amputation. Older men with diabetes and patients who take insulin are at a higher risk of developing ulcers. Foot ulcers can be prevented, and all diabetics are urged to see a podiatrist for a yearly foot exam. In addition, the steps outlined below can help with the prevention and treatment of these ulcers.
Wear Compression Socks

Compression socks help keep blood circulating in areas of the body prone to reduced circulatory activity. Patients with diabetes are often encouraged to wear compression socks because they often have reduced sensitivity and circulation in their legs and feet. These socks keep blood moving and can help prevent patients from developing serious medical issues such as deep vein thrombosis and foot ulcers.
In particular, diabetes patients are urged to wear them if they are traveling long distances or if they have to spend long periods in bed while recuperating from an illness. Several sizes and gauges of compression socks are available to purchase at pharmacies as well as online. Patients should ask their doctors about what level of compression would be most appropriate for them. It is important the socks provide adequate protection but avoid being too tight.
Use Orthotic Shoe Inserts

Foot ulcers often arise due to a combination of reduced circulation with friction. Ill-fitting shoes can introduce unwanted friction, which can lead to the development of blisters and broken skin with the potential to form an ulcer. Diabetes patients are often encouraged to use orthotic shoe inserts. These inserts make shoes fit better and feel more comfortable, reducing both friction and the likelihood of ulcers. Shoe inserts are typically made of gel or foam and come in a variety of styles. Depending on individual needs, patients can select inserts that fill their entire shoe or just one particular area. Shoe inserts can be purchased at pharmacies or online, and podiatrists can also make custom inserts for patients as needed.
Debridement
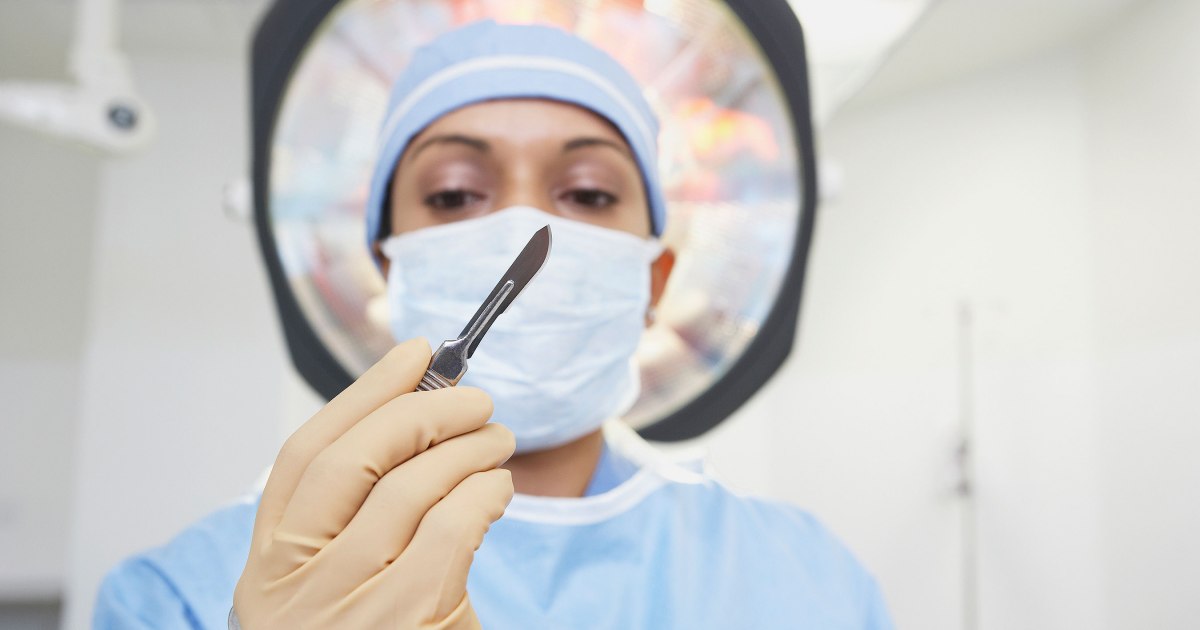
Debridement is a standard procedure used to treat diabetic foot ulcers that must be completed by a doctor. It involves removing dead tissue from the site of the ulcer and can be done using a variety of methods. Nonsurgical methods of debridement include using antiseptics and other chemicals and pastes to remove the dead skin. If these methods fail or are not appropriate for a particular patient, doctors will use surgical debridement.
For this type of the procedure, doctors administer a local anesthetic and use a scalpel to cut away the layers of dead tissue. The wound is covered with a sterile dressing. The procedure stimulates the body's natural healing mechanisms. Most patients wear a soft cast or orthopedic boot to keep pressure off the ulcer. The wound is checked at regular appointments, and for ulcers that have not healed in one month, doctors typically recommend more advanced treatment options.
Antibiotics And Anti-Clotting Medication

Both antibiotics and anti-clotting medication are useful in the treatment of foot ulcers. Antibiotics, which can be taken orally or applied topically, help fight infection and allow wounds to heal more quickly. In very early stages, an over-the-counter ointment containing antibiotics like neomycin may help heal the ulcer. A doctor can recommend more powerful antibiotics if needed.
Anti-clotting medication prevents blood clots and is particularly helpful if a foot ulcer has advanced deep into the skin. Many patients with diabetes may already take anticoagulants for other reasons. Doctors can prescribe different anti-clotting medication to help with foot ulcers, and they may also recommend a change in the patient's normal dose of the usual anticoagulants during this time. In the most advanced cases of foot ulcers, intravenous anticoagulants and antibiotics may be needed to help the ulcer heal. Some of the most commonly used anticoagulants include heparin, warfarin, and rivaroxaban.
Surgical Removal Of Foot Deformities
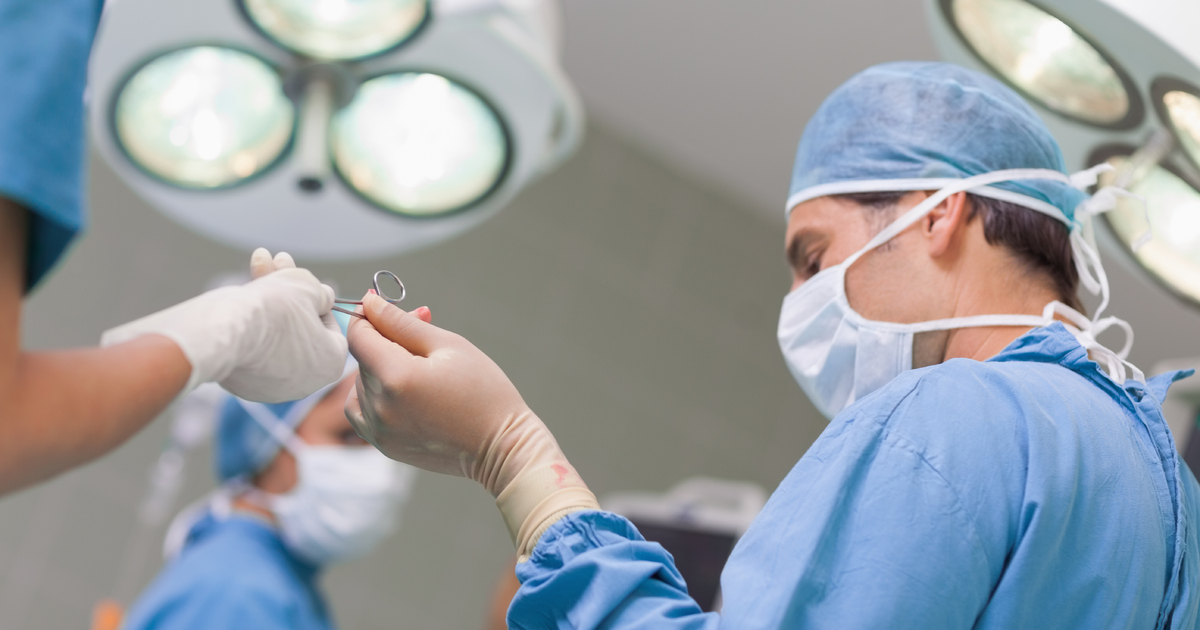
Wound healing techniques have advanced considerably in the last decade, and doctors try numerous techniques to avoid the need for surgery. Medical-grade honey, silver ointments, and other new methods can often get an ulcer under control without surgical intervention. If other methods have failed, doctors may still recommend the surgical removal of foot deformities. This is generally used in cases where an ulcer has become infected so severely that it has spread to the bones of the ankles, feet, or legs. Before surgery, doctors will order x-rays to assess the full extent of the infection. Surgery may be done with local anesthetics, and some patients will need general anesthesia.
Surgery may simply involve removing dead tissue and cleaning the wound. During the operation, doctors may also surgically remove any corns, calluses, blisters, and other foot deformities with the potential to form ulcers. For more advanced infections, it is sometimes necessary to amputate toes or another part of the foot. Following any foot surgery, patients will need to change dressings regularly and will likely be wearing a cast or orthopedic boot.
