Ways To Treat And Prevent Charcot Foot
Charcot foot is a progressive condition that often affects individuals with diabetes. It is caused by peripheral neuropathy, a disorder commonly diagnosed in diabetes patients that causes nerve damage and loss of sensation in the lower legs and feet. Individuals who have Charcot foot often initially notice symptoms of redness, warmth, and swelling in their feet. The condition weakens the bones, soft tissues, and joints in the feet and ankles, and fractures and dislocations of foot or ankle bones are common as the disease progresses. The joints of the foot may collapse, resulting in foot deformities that can lead to the development of ulcers. If the ulcers become infected, individuals with Charcot foot may require amputation. Charcot foot can be difficult to diagnose, and patients may need to see several specialists before the condition is confirmed. Diagnosis is often made with a physical examination, and x-rays and blood tests are sometimes needed. The condition usually affects only one foot. The steps below may be beneficial in the prevention and treatment of Charcot foot.
Get Weight Off The Affected Foot
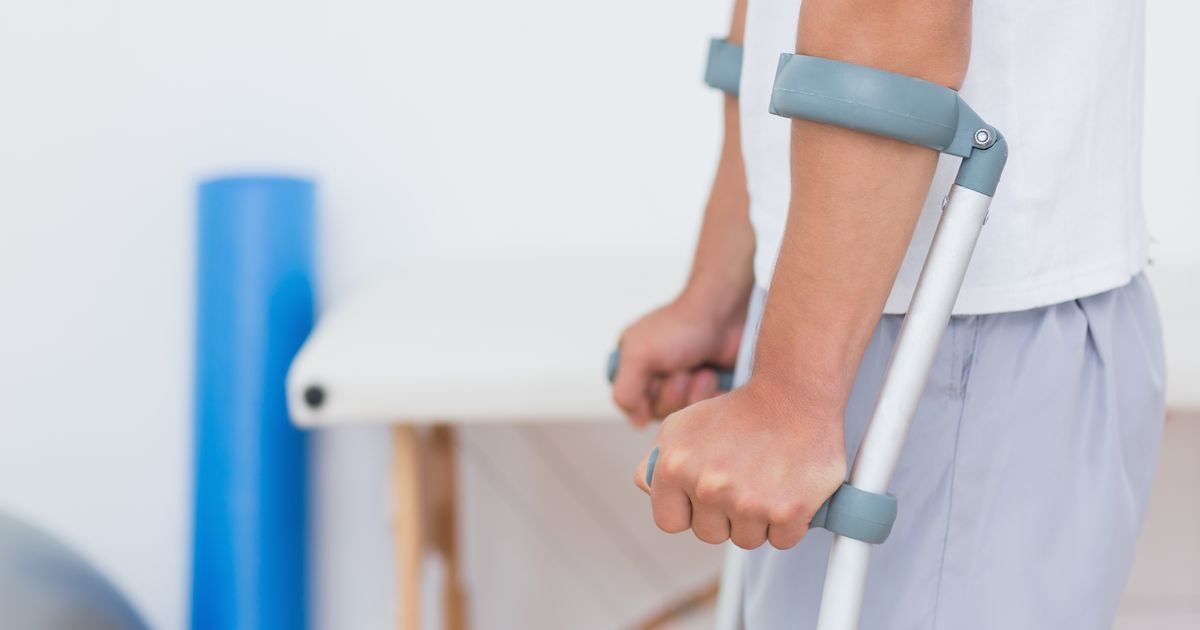
The weakening of the bones and joints associated with Charcot foot can easily lead to the development of foot deformities. It is especially important to get weight off the affected foot. Pressure from walking can lead patients to break a bone in their foot, and peripheral neuropathy means they most often will not notice they have this fracture. Continuing to walk on the broken foot can lead to the collapse of the middle part of the foot, creating a rounded appearance on the bottom of the foot known as a 'rocker bottom' deformity. In addition, when this disorder affects the ankle, it can result in a deformity known as 'floppy foot.' This occurs because tissue has replaced what was once bone, and it often results in ankle instability, which can lead to ankle fractures. To get weight off of the affected foot, doctors may recommend resting the foot, using crutches, or wearing a soft orthopedic boot. In advanced cases, a total contact cast made of plaster is used, and a new cast must be placed at least every two weeks.
Wear Supportive Shoes

Patients are encouraged to wear supportive shoes to counteract the instability caused by Charcot foot. Supportive shoes can make walking easier and may alleviate some of the pressure walking naturally places on the foot. Flat shoes are generally recommended, and they should have a sole that is firm without being rigid. Athletic shoes often provide a high level of support for many patients. Doctors may recommend patients use orthotic shoe inserts in their footwear. These gel or foam cushions protect the foot and toes from friction and pressure by redistributing weight in a balanced manner. Orthotic inserts can be purchased at drugstores and specialist shoe stores. Podiatrists and orthopedic surgeons are generally able to make custom shoe inserts for patients who need them, and these medical professionals can also provide custom footwear for patients who cannot get adequate support with regular shoes.
Surgical Repair
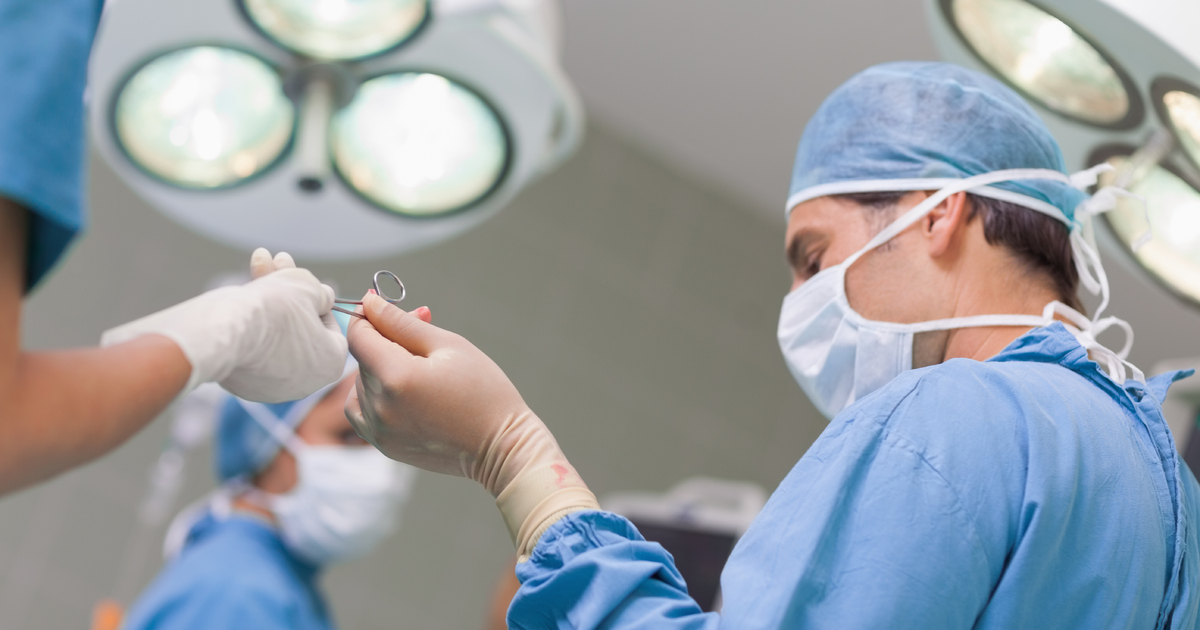
Surgical repair for Charcot foot is used in advanced stages of the disease. The surgery is done to reshape deformities and remove bony protrusions caused by the condition. Several different operations may be used depending on the severity of the deformities. One of the most commonly performed surgical procedures is the osteotomy, which can be done with either local or general anesthesia. While an osteotomy can be done on an outpatient basis, it usually requires an overnight stay in the hospital. The procedure is completed by making an incision along the bottom of the foot and removing bone fragments, cartilage, and abnormal growths. Following the procedure, a cast is often worn for one month.
In more advanced cases, a midfoot realignment arthrodesis is used. Performed under general anesthesia, this operation removes bony growths and repairs the collapsed arch in the foot. Plates and screws are placed during the procedure to stabilize the foot. After the surgery, patients have to wear a cast preventing the foot from bearing weight, typically for three months. Another type of procedure, the hindfoot and ankle realignment arthrodesis, is performed when Charcot foot has made it impossible for a patient to walk. The operation requires general anesthesia and multiple nights in the hospital. During the surgery, fragments of bone and cartilage are removed, and both screws and plates are inserted at specific points to give stability to the bones. Patients must wear a cast for three months after the procedure, and a brace must be worn for three months after the cast is removed.
Check Feet Regularly

Doctors encourage all diabetes patients to check their feet regularly for any changes. This is particularly important for patients who developed peripheral neuropathy and may not otherwise feel pressure or pain in their feet. Ideally, patients should inspect their feet at least once a week, and each foot should always be compared to the other. Any redness, increased warmth, swelling, sores, or pain should be closely monitored and reported to the patient's medical team. Patients should check all areas of their feet, including the toes, soles of the feet, sides of the feet, and ankle area. If needed, patients can ask a caregiver, family member, or friend to help them examine their feet. All diabetes patients are urged to have a yearly foot examination performed by a podiatrist or orthopedic surgeon to catch problems they may not notice.
Wash Feet Daily

Open sores, infections, and ulcers are common foot problems diabetes patients can experience. These problems can often go unnoticed. For this reason, doctors recommend all patients with diabetes wash their feet daily. This gives them time to examine their feet closely for any changes, and washing the feet can help protect against infections that could develop into ulcers.
Diabetes patients may wish to use soap and water to wash their feet, and special soaps are available on with a doctor's recommendation to provide additional cleansing. They should use warm water and a soft clot as well. It's also important to rub the dirt from the soles, grime from between the toes, and dust and other dirtiness from the tops of the feet. As individuals wash, they should take the time to look for redness, sores, and swelling. Many patients prefer to wash their feet in the evenings, and some may also wish to wash their feet following exercise or time spent outdoors. Foot baths can be used for cleansing and are especially soothing. When these individuals wash their feet, they have a chance to observe and take care of them. Patients might install a chair in their shower or take baths so they can focus on washing their feet.
Always Wear Socks With Shoes

Individuals should always wear socks with shoes and make sure they get comfortable shoes that offer a lot of support. Individuals dealing with advanced neuropathy in their feet may find it may help to talk to a podiatrist or orthopedist about the footwear that's best for them. Socks are important because they add another level of support and protection. The socks must fit comfortably and should not be tight enough to cut off circulation. If an individual has Charcot foot that's significantly changed the shape of their foot, they may need to change their sock size or get custom socks. Socks and shoes can provide support around the house as well as outside.
Keep Monitoring Feet
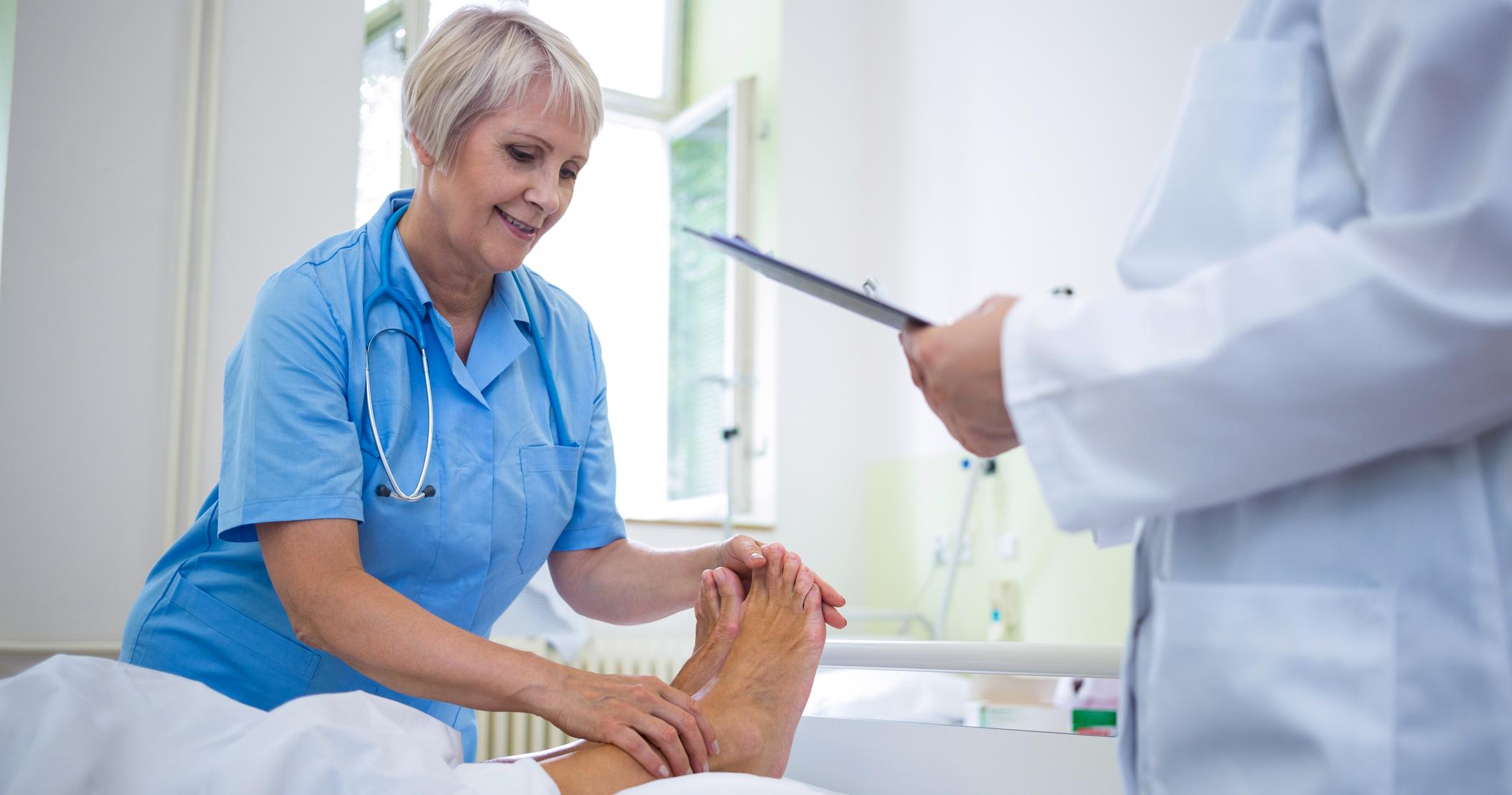
Charcot foot patients should keep monitoring their feet on an ongoing basis, which means having regular checkups with a foot doctor who knows how to treat neuropathy-related foot issues. There should be daily checks performed, and patients should make note of any areas of redness, swelling, unusual warmth, or sores. It's also important to not forget to check between the toes. As mentioned, this is a good thing to do while individuals wash their feet each day. If a patient notices anything unusual, they should speak to a doctor as soon as they can. Early detection makes a huge difference when treating Charcot foot, whether this is a new or recurrent issue.
