Treatment Methods For Diabetes Mellitus
Diabetes mellitus is a chronic medical condition in which there is too much sugar in the blood. This is medically referred to as having high blood glucose and can result from several different mechanisms. In Type 1 diabetes, high blood glucose is caused by the inability of the pancreas to produce sufficient levels of insulin, a hormone which regulates glucose. In Type 2 diabetes, high blood glucose is triggered because the body is unable to respond properly to insulin. Other forms include gestational diabetes, which occurs during pregnancy, and prediabetes, which involves higher than normal blood glucose readings that are not yet high enough to be classified as Type 2 diabetes, which is the most common form of diabetes mellitus and affects more than twenty-nine million Americans. Each year, more than one million new cases of Type 2 diabetes are diagnosed.
Some diabetes mellitus patients may not know they have it because it sometimes produces no symptoms. When symptoms are present, they generally include frequent urination, thirst, fatigue, weight loss, and blurry vision. Complications include chronic renal failure, cardiovascular disease, high blood pressure, eye problems, heart disease, dental issues, and depression. Diabetes mellitus can be diagnosed with blood tests and controlled with lifestyle modifications and medication. The interventions discussed below can help patients keep their blood sugar under control and reduce the risk of complications from this condition.
Control Blood Pressure
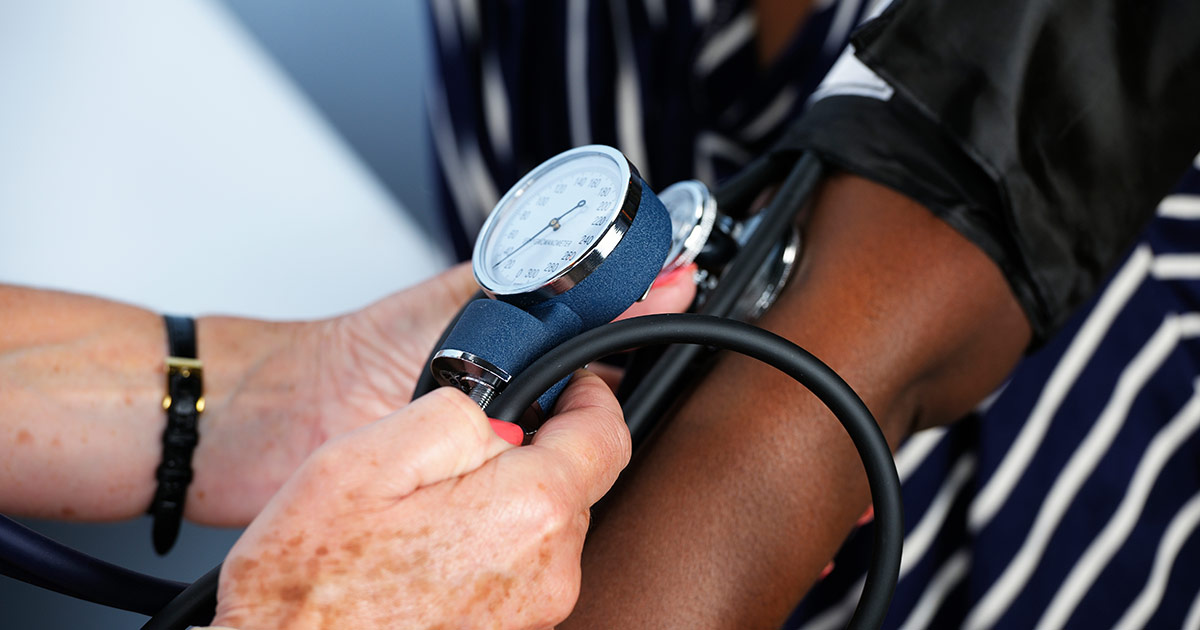
Hypertension, also known as high blood pressure, is one of the most common complications of diabetes mellitus and places patients at an elevated risk of developing heart disease. Blood pressure control is, therefore, a high priority for patients. Blood pressure is measured as a series of two numbers, one when the heart beats (systolic) and the other when it is between beats (diastolic). A normal blood pressure reading is below 120/80, with 120 being the systolic number and 80 being the diastolic number. Blood pressure can be affected by stress, caffeine, and certain medications. A diagnosis of hypertension is made after three consistently high readings taken by a doctor on separate days. Patients usually try to make lifestyle modifications to control their blood pressure first, including limiting salt, losing weight, following stress management techniques, and adopting a diet with fewer processed foods. If these measures do not bring blood pressure readings down, doctors will likely suggest patients begin taking beta blockers, diuretics, ACE inhibitors, or other classes of blood pressure lowering medication to normalize their readings. These medications are generally well tolerated and have few side effects.
Keep reading for more on treating diabetes mellitus.
Follow A Balanced Diet

Doctors encourage all patients who have diabetes mellitus to follow a balanced diet. Proper diet can help patients naturally lower their blood glucose and potentially avoid or reduce their need for oral medicines or insulin. The healthiest, most balanced diet for patients to adopt is one rich in fruits, vegetables, and complex carbohydrates and low in refined sugar, saturated fats, and processed foods. Doctors may also ask patients to monitor their carbohydrate intake. Choosing complex carbohydrates such as those found in brown rice, whole wheat bread, oatmeal, and legumes can help keep patients feeling satiated for longer than simple carbohydrates such as white rice and white pasta. Healthy fats such as the kind found in avocados and other vegetables help lower cholesterol levels and are a much better choice than fat from meat. When planning their diet, patients may wish to keep a food diary and take blood sugar readings before and after meals to determine how certain foods affect their levels.
Get to know the next method of treating diabetes mellitus now.
Exercise Regularly

Diabetes mellitus patients who choose to exercise regularly have a lower risk of cardiovascular disease and can better control their blood glucose and blood pressure naturally and with less medication. Regular physical activity helps the body become more responsive to insulin, and this lowers blood glucose and A1C numbers (a measure of long-term blood glucose). Experts recommend at least 150 minutes of moderate or vigorous activity a week, and diabetes mellitus patients should aim to do more if possible. Examples of beneficial exercises for patients are swimming, ballroom dancing, strength training, brisk walking, jogging, and yoga. In addition to better blood glucose control, regular exercise helps patients lose weight, sleep more soundly, relieve stress, increase energy levels and circulation, and prevent falls.
Continue reading to learn more about treating diabetes mellitus.
Take Medication

While diet and exercise are certainly beneficial, many patients with diabetes mellitus will need to take medication to lower their blood sugar to suitable levels. Oral medications are a common first line of treatment. Alpha-glucosidase inhibitors, SGLT2 inhibitors, sulfonylureas, biguanides, and meglitinides are some examples of the types of oral medicines generally used. Some patients may need to use several of these medicines together to control their symptoms. Side effects of these types of medications are typically mild and include diarrhea, constipation, and nausea.
If adequate control cannot be obtained with oral therapies, doctors may recommend adding insulin or other medications patients can self-administer with specially designed injection pens. For ease of use, the pens are prefilled so patients do not have to handle or even see a needle. Some of the most commonly used injectable medications for diabetes mellitus include exenatide albiglutide, dulaglutide, and liraglutide. These help the body use insulin more effectively, and many are administered just once per week. If insulin is needed, patients may be able to use an insulin pump; this can sometimes be an easier and less invasive method of taking insulin.
Uncover another method of treating diabetes mellitus now.
Monitor Blood Glucose Consistently

It is essential for patients to monitor blood glucose consistently to achieve optimal control over the numbers. This is done at home using a small lancet and a blood glucose meter. A drop of blood is taken from the finger or another testing site such as the forearm and placed on a test strip, which is then inserted into the meter to produce a reading. Some newer testing devices can monitor glucose continually with fewer finger sticks than older devices. Type 1 patients may need to test their blood sugar as often as ten times per day. Daily testing is recommended for type 2 patients, especially those who are using insulin and multiple medications, and some may even need to test two or three times a day if they are taking insulin. For patients not taking insulin, blood glucose monitoring can be done on a less frequent basis. The doctor will recommend an appropriate at-home monitoring schedule based on the needs of the individual patient.
