Horrific Problems Caused By Having A Torn Retina
In most cases, a torn retina or retinal detachment will need to be surgically repaired by sealing the back wall of the eye to the retina with either laser surgery or a type of freezing treatment called cryotherapy. Both procedures create a scar to help the retina seal itself to the back of the eye wall, preventing fluid from traveling under the retina through the tear. For the most part, patients tolerate these procedures well. However, it is crucial to note there can be some side effects, and there are also some painful and serious issues a torn retina can still cause prior to the surgery.
Eye Pain

Retinal detachment might sound like a condition in which the affected individual experiences excruciating eye pain; however, in many cases, there might be no direct eye pain or no symptoms at all, which makes it hard to detect a tear. In some cases, retinal detachment may cause pain or headaches. Pain may be felt deep in the eye area where the damage is located or may present itself in the form of a headache behind the eyes. Pain is the first indication something is wrong, and treatment should follow if it persists for longer than a few days. Eye pain is particularly concerning if treatment does not occur in a timely manner, making prompt diagnosis and action even more crucial.
Tissue Damage
A torn retina is a serious problem because it may cause harm to the tissue surrounding the eye, which can permanently affect vision. One of these tears may extend and allow fluid to enter through the damaged area. The accumulation of fluid may separate the retina from the underlying tissue, which results in retinal detachment. Retinal detachment may cause harm to the tissue or nerves surrounding the eye. If treatment is not obtained promptly, the tissue and nerve damage can extend and eventually result in the loss of the patient's vision. Thankfully, surgery to repair the retina is able to mitigate the risk of this from happening if it is employed in good time.
Bleeding
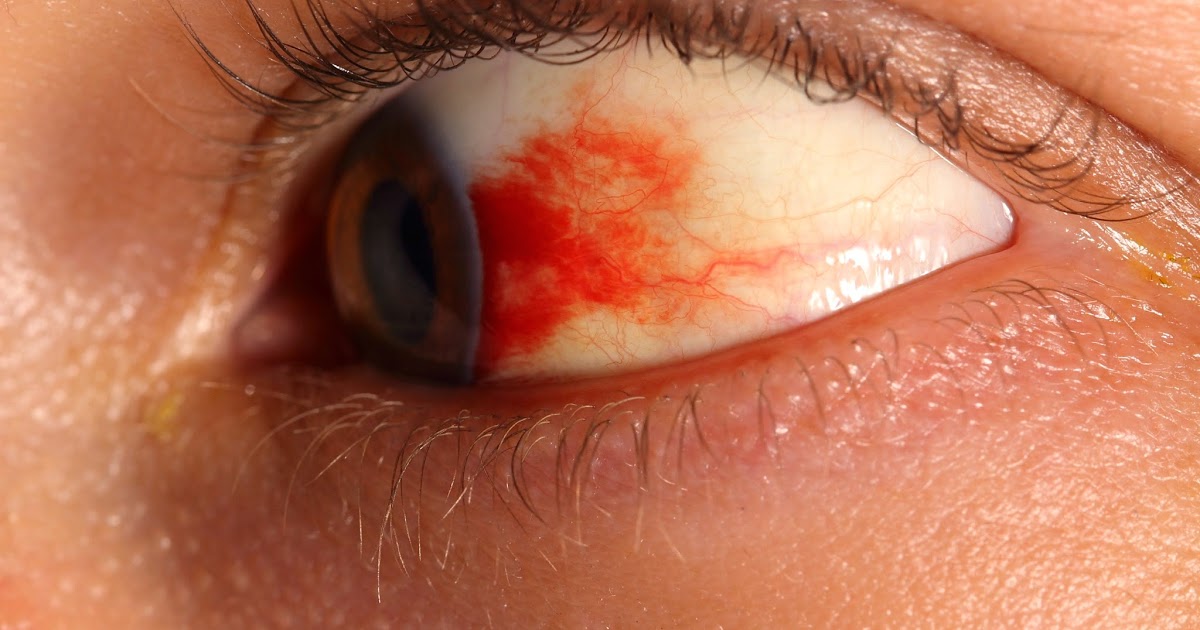
In some cases, a torn retina results in vitreous hemorrhage or bleeding in the transparent cavity of the eye. It occurs when blood leaks into areas around the eye and mixes in with the clear liquid attached to the back of the retina. It is the most common cause of sudden and painless vision loss. Although a torn retina may sometimes be hard for individuals to detect, it is important to seek treatment at the first sign of one or any other vision or eye problems, as this will help patients prevent complications such as bleeding in or around the eye as well as vision loss.
Inflammation Or Infection
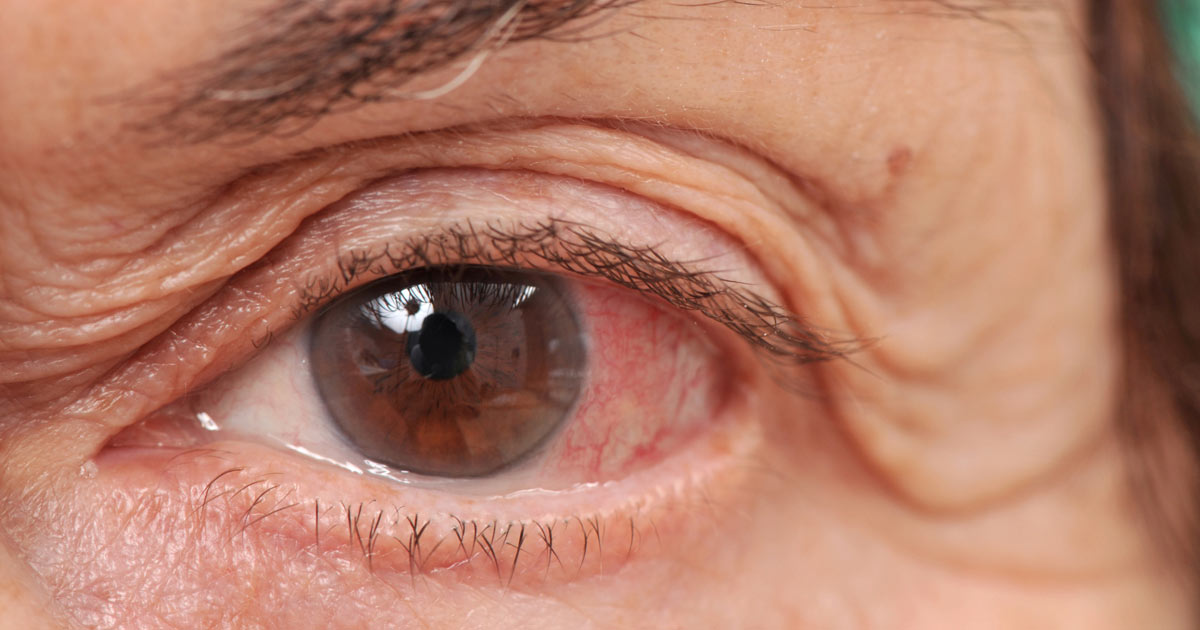
The middle of the eye is filled with a layer of clear gel attached to the retina. This is called the vitreous body. When retinal detachment occurs, this fluid may leak through the tear in the eye, where it is prone to developing an infection. The vitreous body may also cause excess irritation or inflammation of the eye, which can quickly become infected or cause nerve damage. Eye infections can often result in pain, itching, or photosensitivity, which can impact an affected individual's long-term vision if it is left untreated.
Cataracts After Surgery
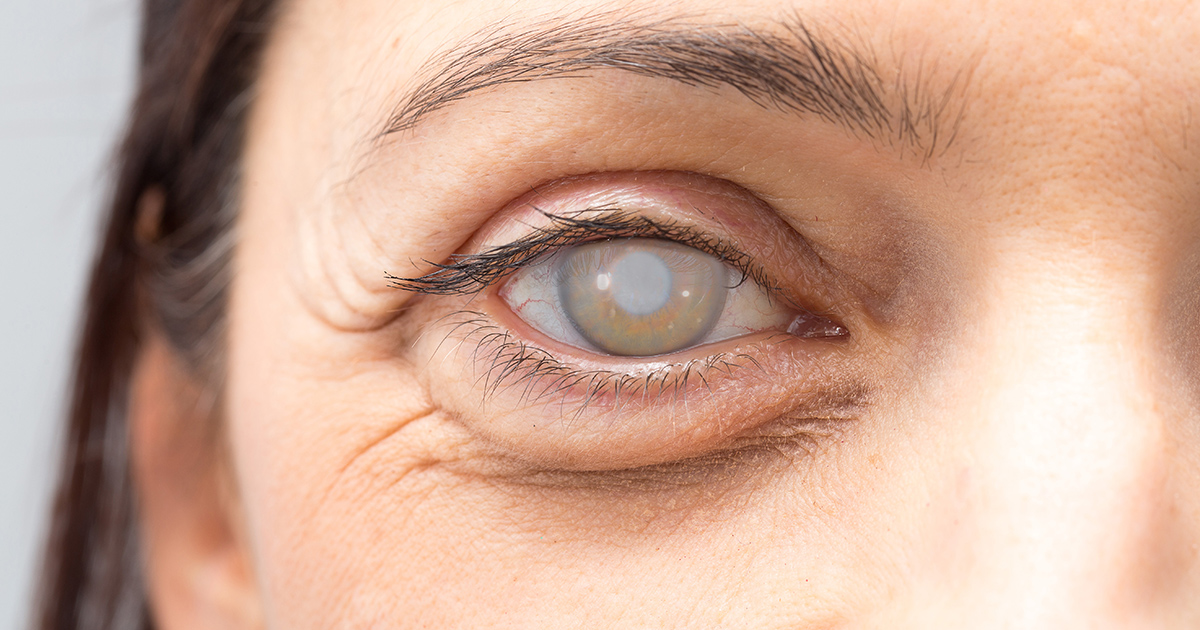
Patients who have an operation to repair a torn retina might develop cataracts after surgery on the affected eye. A cataract occurs when the lens of the eye, which is normally clear, becomes cloudy. Cataracts cause blurry vision, and the patient may feel as though they are seeing everything through a frosted window. Over time, the patient might notice additional symptoms, including sensitivity to light, double vision in the affected eye, and difficulty seeing at night. Bright colors could also appear as though they are faded.
Cataracts can form at the center of the lens of the eye, and they may develop at the back of the lens or at the edges of the lens too. Individuals who have recently had retinal surgery will have frequent follow-ups with their ophthalmologist, and the clinician will carefully check for signs of cataracts at these appointments. To do so, they will examine the retina with a slit-lamp examination and an ophthalmoscope. If cataracts are present, surgery to remove the cataract may be recommended once the patient has recovered from the previous operation.
Glaucoma After Surgery

Some individuals who have operations on their torn retina may develop glaucoma after surgery. Glaucoma occurs when the optic nerve is damaged, and this is typically caused by elevated pressure within the eye. Left untreated, glaucoma can lead to blindness. With open-angle glaucoma, the patient may not have any symptoms, and vision loss happens gradually. Closed-angle glaucoma is considered a medical emergency, and patients may experience a sudden onset of blurry vision, headaches, and severe eye pain. The patient might also see halos when looking at lights, and some individuals have nausea and vomiting.
Patients who have undergone surgery on their retina will be advised of these warning signs, and an emergency appointment with the patient's ophthalmologist should be made if these symptoms develop. To screen patients for glaucoma, doctors perform a test known as tonometry to measure eye pressure. Pachymetry, an exam that measures the thickness of the cornea, may also be performed. Treatment for glaucoma typically includes eye drops to lower eye pressure, and patients may need to have conventional surgery or a laser trabeculoplasty to help fluid drain from the eye.
Photopsia
Photopsia refers to the presence of floaters or flashes of light in the patient's visual field. Patients can experience photopsia in a variety of ways. Some patients might see shimmering or flickering lights, moving dots, or floating shapes in their visual fields, and other patients could develop fuzzy, snowy, or static areas in their vision. Photopsia is a symptom associated with several underlying eye conditions, and one of the most common causes of this symptom is retinal detachment. This occurs when the retina moves outside of its normal position.
Tears in the retina may also lead to photopsia. Any floaters or flashing lights that appear regularly in the patient's visual field and that increase in number should be promptly investigated, as they may be indicative of retinal problems that need surgery. Patients who have had eye surgery should inform their surgeon immediately if they notice floaters or flashes in the eye on which the surgery was performed.
Significant Increase In Eye Floaters

Patients who have retinal tears or other retinal issues often have a significant increase in eye floaters, which are moving dots or shapes that appear to float in the patient's visual field. They may appear as cobwebs or strings of floating material that eventually drift outside of the visual field, and they are often most noticeable when looking at a solid, bright background such as a white wall or a blue sky. Eye floaters that occur along with flashing lights or a loss of peripheral (side) vision may indicate retinal issues that could threaten the patient's sight, and they should have an urgent eye exam with an ophthalmologist.
They will dilate the patient's eyes, check the patient's eye pressure, and perform tests to measure peripheral vision. The patient's retina will be photographed, and a detailed retina examination will be conducted to determine if there are any tears or if the retina has become detached. If any abnormalities are detected, the doctor will discuss possible surgical options and other treatment methods with the patient. Eye floaters may occur for several months after a surgical procedure on the eyes, and patients will be monitored closely for possible complications during this time.
Dense Shadow In Vision

A dense shadow in vision is likely indicative of a loss of peripheral vision, and this appears as dark spots or shadows at the sides or edges of the patient's visual field. This symptom is common in patients with retinal tears and detachments, and it usually indicates the patient's retinal issues are becoming more serious. If the patient notices a dense shadow in their vision that does not go away or that becomes larger, they should seek an urgent evaluation from an eye health professional.
This is especially necessary for anyone who has known pre-existing retinal or other eye issues and for those who have recently had eye surgery. To assess the location and severity of shadows within a patient's visual field, doctors will perform a test known as the visual field test. This painless exam can help clinicians map the patient's entire visual field, identifying blank areas, and planning the most appropriate treatment options.
