A Step-By-Step Guide To Performing CPR
Cardiopulmonary resuscitation, better known as CPR, is an essential tool everyone should learn. Why? Minutes matter in an emergency. By performing CPR on someone, before paramedics arrive, you can give the person a better chance of survival. A loved one or a stranger would benefit significantly from a fast action. Besides, wouldn't it be better to not run around looking for someone certified in CPR? You are already there. You most likely saw the events that led to the need for resuscitation. If you are not certified in CPR, or your skills are a bit rusty, then keep reading for an instructional guide on the steps to perform this life-saving technique.
Check Your Surroundings Before You Begin

Calling 911 is essential in every emergency. The technician on the other end of the line will walk you through the steps, while emergency personnel is being dispatched. It is essential to check your surroundings before beginning to administer CPR to make sure there is no eminent danger. When you call, you will need to describe your location and what is going on around you. Make sure to be more specific than 'I'm in the food court at the mall.' Every detail matters during an emergency, especially location. Verify the crisis by checking the patient for signs of choking or chest pains. Once you determine the emergency warrants CPR, gently lay the person on the floor. They will need to be on a solid surface. Continue calling out to them if they appear unconscious. Make sure that their path is clear of doorways or other people. In addition to clearing pathways, check for dangerous materials on the floor or near the person, especially if you were not present when the victim collapsed. Emergencies tend to draw crowds. Instead of letting them stand there watching, put them to work. Ask someone to look for an automated external defibrillator (AED). Remember to always focus on the person who needs help.
Uncover more details on how to do CPR now.
Check Their Airways & Pulse

Listen to their breathing. If their breathing sounds or appears to be very shallow or they are gurgling, then perform CPR immediately. If there are no visible breathing signs, check for a pulse by placing your two fingers on one side of their windpipe. Slide your fingers down their neck, between the two muscles close to the base of the neck. The carotid artery should be pulsating. If you do not feel a pulse, perform CPR immediately. It is important to check their airways and pulse before performing CPR. If the pulse is present but the breathing is gurgling or nonexistent, then only lifesaving breaths are needed.
Keep reading to learn more about how to correctly and effectively perform CPR now.
The Importance Of Compressions

Chest compressions are the most essential part of CPR. Correct hand placement is also important for the safety of the patient. With two fingers, locate the point where both sides of the bottom of the ribcage come together. This is the bottom of the sternum or breastplate. Holding your fingers as a place marker, place the heel of your other hand just above your fingers. Then remove your two fingers and place that hand on top of the other hand, interlacing your fingers. Straighten your arms. Using your upper body, press down on the person's chest. You will want to push about two inches inward. Allow your hands to raise enough, after each compression, for the chest to fully expand. Keep contact with your hand placement so your hands do not move out of place to minimize injury. Your goal is to perform thirty presses. You are imitating the beat of a heart. Some paramedics suggest humming the tunes 'Staying Alive' by the Bee Gees or 'Another One Bites The Dust' by Queen, to keep the correct rhythm. Please try not to sing out loud.
Learn more about performing CPR now.
Airway: Opening Up The Airway
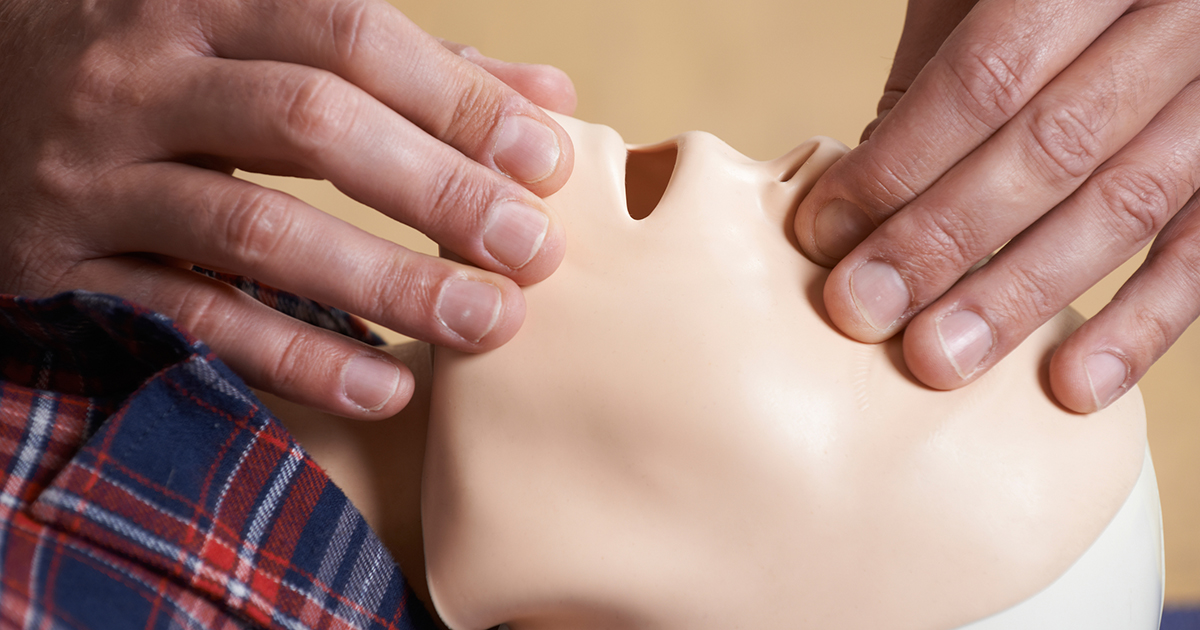
After every thirty chest presses, you will need to give two lifesaving breaths to the person. To perform this technique, make sure to open their airway. Tilt the person's head back by gently placing your hand behind their neck and lifting slightly. At the same time take two fingers and place them below their chin, tilting their chin upward. Their chin should be aimed at the ceiling to open the airway. The importance of physically opening the airway is structural. When we lay on our backs, the soft tissue of our throat relaxes and can obstruct the airway. If you wonder why your spouse snores at night, this is probably the reason.
Get the details on breaths in CPR next.
Breathing: Breathe For The Patient

Pinch their nose and open their mouth. Place your mouth on theirs and breath in. You will want to use enough force to cause the chest to rise. Keep your eyes open and watch the chest cavity during this technique. Mouth to mouth can be intimidating, but you are helping the individual breath, do not forget that. You may also be able to use a one-way barrier, if available. Have someone check the AED case for one. The barrier prevents the passage of bodily fluids, including vomit, from passing between two individuals. Once you have performed the two lifesaving breaths, then repeat the thirty compressions again. This cycle should be repeated five times. You may get tired during the process. If you notice you cannot continue at the same pace or strength, ask if someone else knows CPR. You can take turns to keep up the pace. Hopefully, help has arrived by this time. Advise the 911 technician of the person's status. When it is all said and done, you may have just saved someone's life.
Read about more tips for performing CPR effectively now.
Compressions Must Be Hard

To effectively pump blood throughout the body, CPR compressions must be hard. Generally, experts suggest individuals performing CPR aim for a depth of 5.5 centimeters (approximately two inches) for each compression. It takes roughly sixty pounds of force to compress the chest by this amount. Compressions deeper than two inches could cause damage to the patient's internal organs, and compressions that are too shallow will be ineffective. If there is doubt about whether the compressions are hard enough, it can be helpful to err on the side of being too forceful. While forceful compressions could break some of the patient's ribs, they may be necessary in order for the patient to live. CPR training courses and practice sessions with CPR dummies are recommended so providers can receive individualized guidance on achieving an appropriate compression depth.
Discover how CPR can be performed on children and babies next.
CPR On Children And Babies

Performing CPR on children and babies requires a slightly different technique than adult CPR. For CPR purposes, a baby is under one year old. CPR for babies should be performed using two fingers instead of interlocking hands, and compressions need to be approximately 1.5 inches deep. After placing the baby on a hard, flat surface, the provider should administer thirty compressions at a rate of about two compressions per second. Next, two rescue breaths should be given, and the provider should then give another thirty compressions. This cycle should be repeated until paramedics arrive. For CPR, children are individuals between one and eight years old. When administering chest compressions to this age group, the provider should place the heel of one hand in the center of the child's chest. The heel of the other hand should be placed on top, and the fingers of both hands should be laced together. Each compression should be two inches deep. After giving thirty compressions, the provider can choose to give two rescue breaths after pinching the child's nose closed. It is also acceptable to give hands-only CPR without rescue breaths for this age group.
Learn more about compressions and CPR now.
Interlocking Hands For Compressions
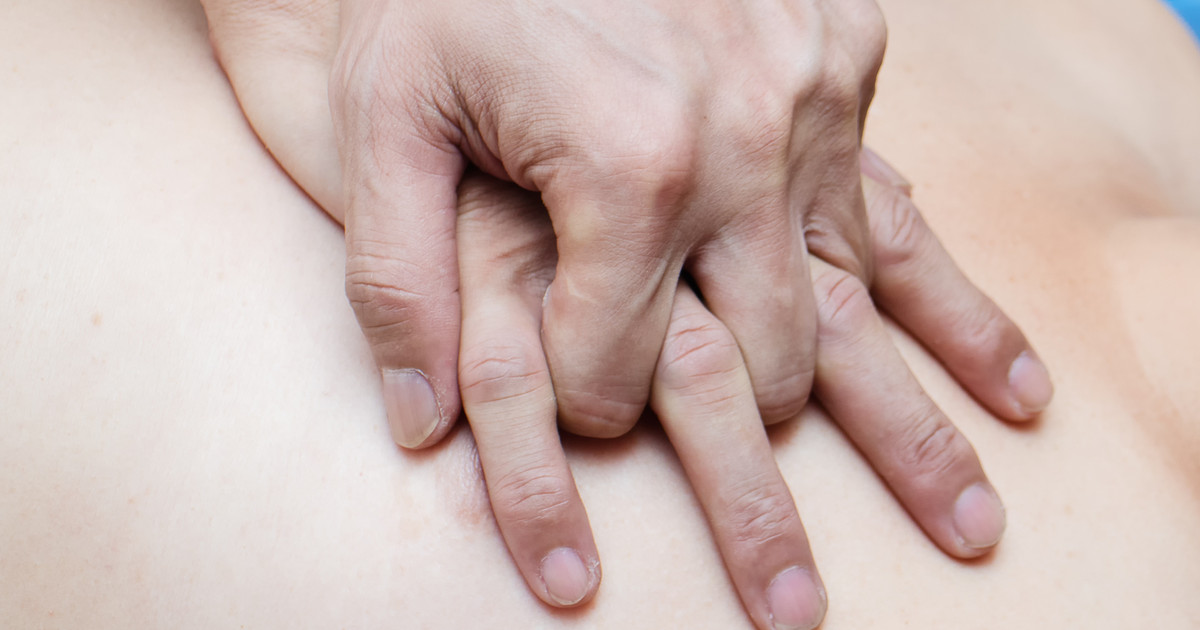
When performing CPR on children and adults, providers should use interlocking hands for compressions. This technique creates more powerful compressions and helps center the motion of each compression so it is delivered in the correct location. To correctly place the hands for CPR, the provider should start by placing the heel of one hand on the patient's sternum (breastbone) at the center of the chest. The other hand should be placed on top, and the fingers of both of the provider's hands should be intertwined to keep them off of the patient's chest. Using interlocking hands, the provider should then deliver the compressions by pressing straight down into the patient's chest. If the provider has difficulty interlocking their fingers, it is okay to simply hold the fingers in an upward position so they are off of the patient's chest. Providers with arthritis or small wrists can safely administer compressions by holding the wrist of the hand positioned on the patient's chest with their other hand.
A recent study suggests CPR providers deliver deeper compressions using their right hand as the bottom hand (the hand in contact with the patient's sternum) when they are on the patient's right side. The research found when providers are positioned on the patient's left side, they give deeper compressions when they place their left hand on the patient's sternum as the bottom hand. Experts recommend that CPR providers approach the patient from the side of their dominant hand. Left-handed providers should position themselves on the patient's left side, and right-handed providers should position themselves on the patient's right side. Providers should place their dominant hand on the patient's sternum, and their non-dominant hand should be placed on top.
Uncover information on the most common mistakes made when giving CPR next.
Common Mistakes

One of the most common mistakes CPR providers make is forgetting to call for help before beginning CPR. Most individuals are unable to give CPR for more than two minutes at a time, and calling for help first means paramedics can arrive more quickly to take over. Additionally, some providers may use improper CPR techniques. For example, they may give compressions that are not deep enough, and they might give compressions too rapidly. They could also forget to keep their elbows straight while administering compressions. Although CPR advice used to include rescue breaths, current guidelines now recommend that providers prioritize continuous chest compressions instead. Rescue breaths are no longer recommended when administering CPR to adults, particularly if the provider is a novice or has not been certified in CPR.
Keep reading for more on performing CPR now.
Don't Stop Until Paramedics Take Over

In most cases, healthcare experts recommend that individuals administering CPR don't stop until paramedics take over. Administering CPR is very tiring, and it is helpful if a second CPR provider is available to assist. It can sometimes take thirty to ninety minutes of continuous CPR for the patient to be successfully revived, and long resuscitation times are associated with improvements in brain function in cases where the victim survives. In urban areas, paramedics will generally arrive within five to ten minutes of receiving an emergency call. However, in rural areas, it could take thirty minutes or more for emergency personnel to arrive. Once paramedics arrive, CPR providers should continue giving compressions until the medical team asks them to stop. CPR should also be stopped if the patient begins exhibiting obvious signs of life. For example, CPR should be discontinued if the patient grimaces, lifts their head, or moves an arm or leg. If the patient blinks, looks around, and focuses their eyes on objects, it is safe to stop CPR as well.
