Guide To Atrial Fibrillation Treatment
Atrial fibrillation is a condition characterized by a rapid and irregular heartbeat that can produce life-threatening complications, including heart failure, strokes, and numerous other heart conditions. For the heart to beat properly, the upper two chambers or atria and the lower two chambers or ventricles have to be in sync with each other. Atrial fibrillation occurs when the atria experience irregular and chaotic beating that discords from the ventricle rhythm. Symptoms of atrial fibrillation include breathlessness, heart palpitations, and weakness. Atrial fibrillation can be transient, or it may be chronic and consistent. Because atrial fibrillation causes blood stagnation in the atria, there is increased concern with the development of blood clots in these chambers. Blood clots travel around the body and cut off blood supply at the location where they become lodged.
Cardioversion

An individual affected by atrial fibrillation due to certain underlying causes may need to undergo cardioversion as part of their treatment plan. Cardioversion is a procedure that intends to reset a patient's heart rhythm and rate to normal. There are two ways cardioversion can be accomplished. Electrical cardioversion is a type of cardioversion that utilizes electrical impulses to stop the electrical activity in the heart so it can restart at a normal rhythm. Cardioversion with drugs is a process where medications referred to as antiarrhythmics are utilized to revert the rhythm of the patient's heart back to normal. This process most often occurs in the setting of a hospital where the patient receives the antiarrhythmic drugs intravenously or by mouth. They are then closely monitored for some time to see if their heart rhythm reverts to normal. If the drug is successful at alleviating atrial fibrillation, it will be prescribed for the patient to take when they experience episodes of atrial fibrillation.
Anti-Arrhythmic Medication

Patients with chronic atrial fibrillation may need to take certain antiarrhythmic medication long-term daily to stop episodes before they can occur. This type of medication is typically only prescribed when the patient's heart rhythm has already been corrected with the use of electrical cardioversion. The most common antiarrhythmic medications used include flecainide, amiodarone, dofetilide, propafenone, and sotalol. Different antiarrhythmic drugs utilize different mechanisms to restore and maintain a patient's healthy heart rhythm and function. Some of these drugs work by increasing or decreasing the velocity of electrical conduction in the tissues. Others work by changing the excitability of the cells that make up the heart through the alteration of the effective refractory period duration. Another mechanism antiarrhythmic medications use to help maintain a patient's heart rhythm is by inhibiting the abnormal automaticity that occurs in the tissues and is known to trigger atrial fibrillation.
Maze Procedure
A maze procedure is known to be an effective way to treat a patient who experiences atrial fibrillation frequently due to the abnormal and excessive transmission of electrical impulses through the heart tissues. The maze procedure is typically one of the last resort treatments because it is not minimally invasive and requires open-heart surgery. During a maze procedure, the surgeon uses cryotherapy, radiofrequency, or a scalpel to produce a particular pattern that will form into scar tissue. Scar tissue is denser than normal tissue and does not conduct electricity as healthy tissues do. The scar tissue is produced in a certain part of the patient's heart muscle to stop the ability of stray and erratic electrical impulses to flow through these tissues and cause the patient to have atrial fibrillation. The maze procedure can be done at the same time as another major open-heart surgical procedure, like a heart valve repair or coronary artery bypass. Maze procedures for atrial fibrillation are generally successful, but it is also not unheard of for atrial fibrillation to eventually return.
Catheter Ablation
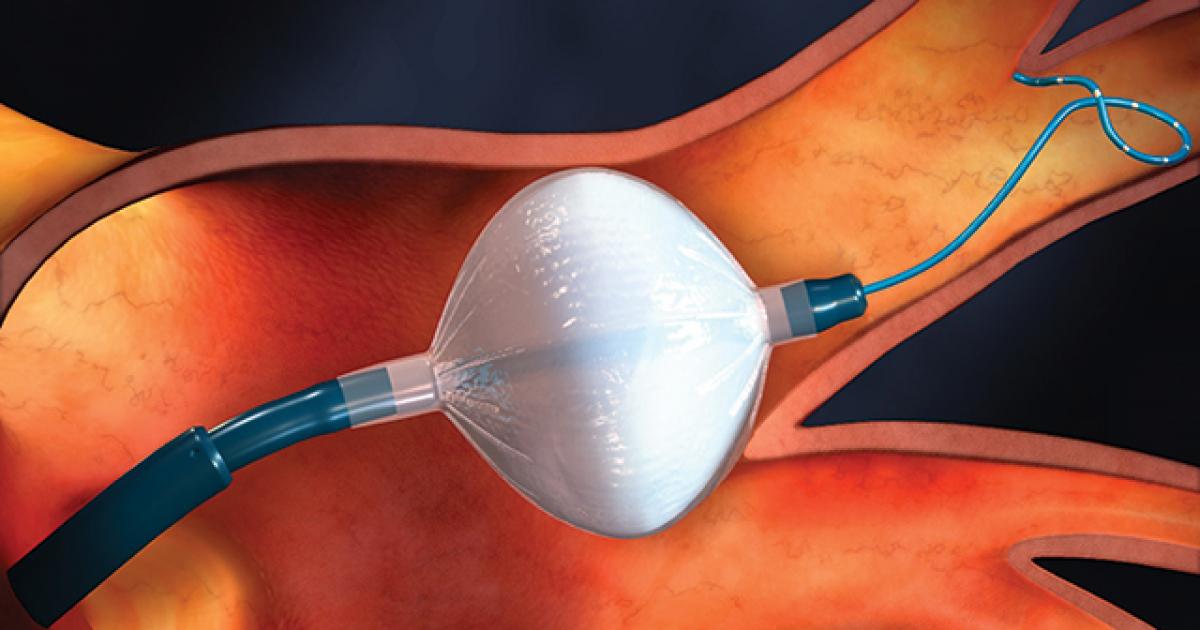
When methods of cardioversion and medications are not effective at treating atrial fibrillation, catheter ablation is usually the next method used. Catheter ablation is a minimally invasive procedure used to destroy the sections of tissue in the patient's heart causing atrial fibrillation. During a catheter ablation procedure, a catheter or long thin tube is inserted into a large vessel in the patient's groin and is threaded up to their heart. The places in the heart causing the inappropriate conduction of electricity are then identified and located. The surgeon then uses the catheter to apply cryotherapy, radiofrequency, or heat to destroy these tissues. This process causes scar tissue to form as a replacement for the tissue that was destroyed. Scar tissue is stiffer and denser than normal tissue, making it unable to conduct electricity. This scar tissue helps redirect the electrical impulses in the patient's heart back to a healthy and normal path and pattern.
Atrioventricular Node Ablation
When atrial fibrillation does not respond appropriately to cardioversion, medications, and catheter ablation, patients may need to undergo atrioventricular node ablation when they are not a suitable candidate for the maze procedure. During atrioventricular node ablation, a long thin tube or catheter is inserted to a large vessel in the patient's groin and threaded to the heart. The surgeon identifies their atrioventricular node and uses radiofrequency energy to destroy the small part of the tissue that makes up the node. The atrioventricular node is the pathway that runs between the heart's lower chambers (ventricles) and the upper chambers (atria). The formation of scar tissue and the destruction of the node helps stop the abnormal impulses from the atria to the ventricles. However, the quivering of the atria will still occur after the procedure. Patients who have an atrioventricular node ablation will need a pacemaker installed to maintain the proper contraction of the ventricles.
