Symptoms And Treatments For Heart Conditions You Didn't Know Existed
When most individuals think of heart conditions, their minds tend to immediately think of heart attacks and the umbrella term 'heart disease.' While these heart conditions are serious, they are not the only ones individuals may encounter throughout their lives. Curious about some of the rare heart conditions out there? Here are all the details on what they are, how they occur, and what the symptoms are. There is also information about the various treatment options available to patients who have been diagnosed with a particular condition.
Pericarditis

Pericarditis occurs when the pericardium, the sac-like tissue surrounding the heart and helping hold it in place so it can work, becomes inflamed. Typically, the two layers of the pericardium are separated by a little fluid to prevent them from rubbing together. However, when the pericardium becomes inflamed, the layers are likely to rub against the heart, causing chest pain. Chest pain with pericarditis is typically sharp and more intense when breathing in, and appears over the center of or on the left side of the chest. It can often be mistaken for a heart attack. Other symptoms include shortness of breath, heart palpitations, swelling in the abdomen or legs, a cough, low-grade fever, as well as fatigue or weakness.
Unfortunately, the cause behind pericarditis is frequently unknown, though it often appears following a viral infection, particularly when the respiratory system is involved. Autoimmune disorders, such as rheumatoid arthritis or lupus, are common causes of chronic pericarditis. Aside from these, other potential causes include kidney failure, cancer, tuberculosis, heart attack or surgery, as well as specific medications.
Treatment For Pericarditis

The good news is pericarditis is often mild and goes away with rest. When cases do require treatment, doctors usually start with medication such as pain relievers. Often over-the-counter options work, particularly if they are also classified as an anti-inflammatory, such as ibuprofen. However, in severe cases, doctors may recommend prescription-strength pain relievers and anti-inflammatories, such as colchicine, or corticosteroids.
If patients experience cardiac tamponade as a complication of pericarditis, they are often hospitalized. Treatments for this case typically includes either pericardiocentesis or pericardiectomy. The former is a procedure in which the surgeon uses a needle or catheter to drain the excess fluid while the patient is under local anesthesia. A pericardiectomy is a procedure where the surgeon will remove the entirety of the pericardium that has become rigid, is recommended for patients with constrictive pericarditis.
Cardiomyopathy

There are a few overarching types of cardiomyopathy, including hypertrophic, dilated, restrictive, and arrhythmogenic. Hypertrophic is when the heart muscle thickens without a discernible cause, dilated is when the enlarged heart ventricles weaken, and restrictive is when the ventricles become rigid and weaken, but do not thicken. Arrhythmogenic right ventricular dysplasia is a rare form in which fatty or fibrous tissue replaces the muscle in the right ventricle. All types of cardiomyopathy, save for restrictive, can be inherited through gene mutations or other gene indicators. Other causes of dilated cardiomyopathy include alcohol, late-stage pregnancy complications, viral infections, heart attack, illegal drugs, diabetes, and HIV. Causes of restrictive cardiomyopathy include hemochromatosis, amyloidosis, sarcoidosis, connective tissue disorders, and specific cancer treatments, such as chemotherapy.
Symptoms vary based on the specific type of cardiomyopathy, and some individuals may never experience symptoms. However, symptoms when the condition worsens often mimic heart failure and include fatigue, shortness of breath, and swelling in various parts of the body, such as the ankles and feet, legs, abdomen, and neck veins. Other signs include dizziness, irregular heartbeats, heart murmurs, chest pain, and fainting during or after physical exertion. Chest pain in this condition typically occurs after eating a heavy meal or physical activity.
Treatment For Cardiomyopathy

Patients who do not experience symptoms do not require treatment. When treatment is needed, however, it varies based on type, severity, as well as the patient's age and overall health. Standard treatments include making lifestyle changes for heart health, medication, and surgery. Examples of heart-healthy lifestyle changes are managing stress, eating a balanced and healthy diet, maintaining a healthy weight, and quitting smoking. Medications doctors prescribe include those to prevent blood clots, balance electrolytes, lower blood pressure, maintain a normal heartbeat, remove excess sodium, reduce inflammation, and slow heart rate.
Surgical options include surgically implanted devices, a heart transplant, and septal myectomy. The devices are all intended to assist the heart in pumping the blood sufficiently and evenly throughout the body, and include a pacemaker, left ventricular assist device, cardiac resynchronization therapy device, and an implantable cardioverter-defibrillator. Septal myectomy is open-heart surgery, recommended for severe hypertrophic cardiomyopathy, in which the surgeon removes the piece of the thickened septum interfering with the left ventricle. A heart transplant is typically the last resort and, as the name suggests, involves replacing the diseased heart with a new, donor heart.
Ebstein's Anomaly
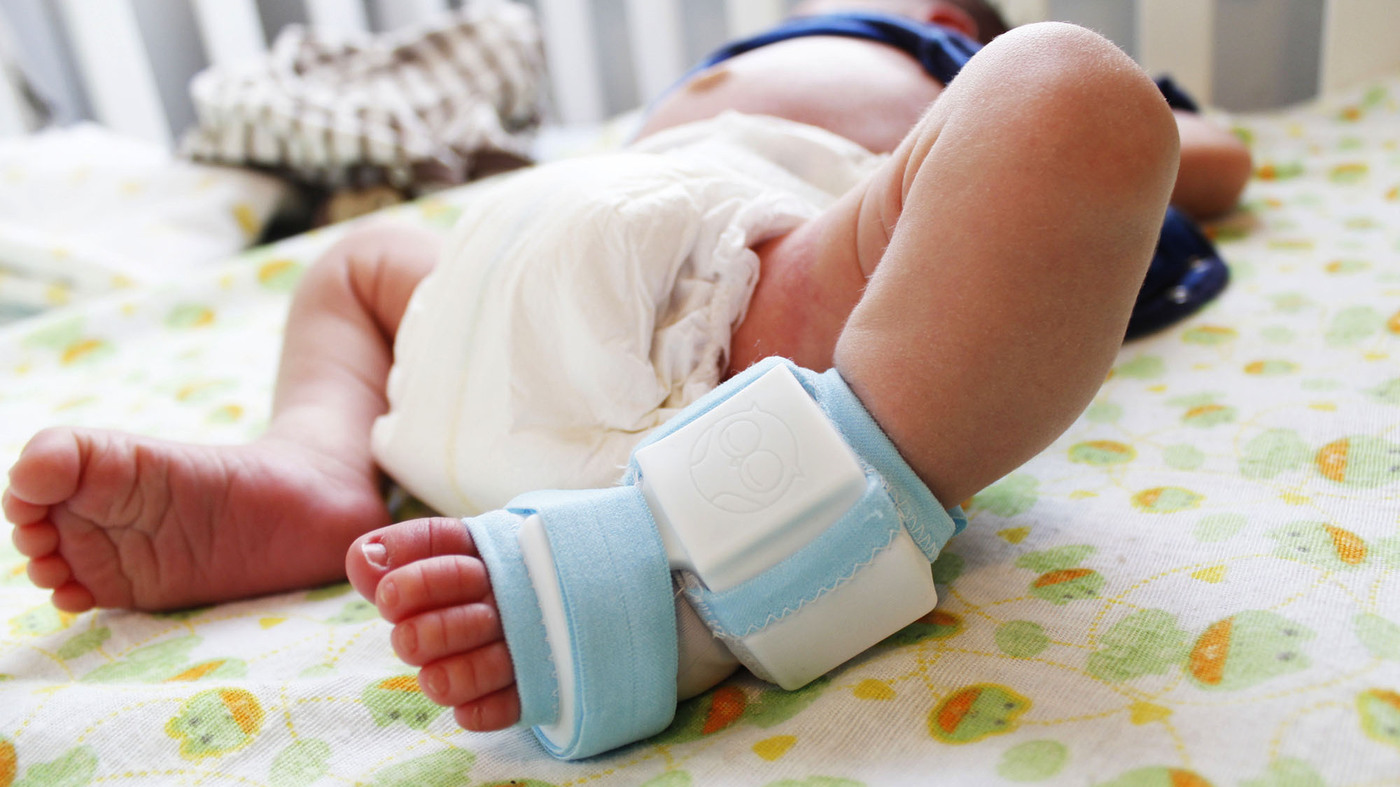
When it comes to potential birth defects, congenital heart defects are the most common. However, Ebstein's anomaly is a rare heart defect, and research indicates it only appears in one out of every twenty thousand children, though symptoms can be minor and many cases go undiagnosed. This heart defect affects the right side of the heart and precisely when the tricuspid valve, which divides the two chambers on the right side of the heart, forms too far down in the right ventricle and thus does not function as it should in controlling blood flow.
Research has not adequately identified a cause, though it suspects a combination of environmental factors and genetics, given the condition, is present at birth. Symptoms of Ebstein's anomaly include swelling in the patient's belly and legs, trouble breathing, an enlarged liver, cyanosis (blue discoloration of fingers and lips), abnormal heartbeats, dizziness, fainting, and shortness of breath.
Treatment For Ebstein’s Anomaly
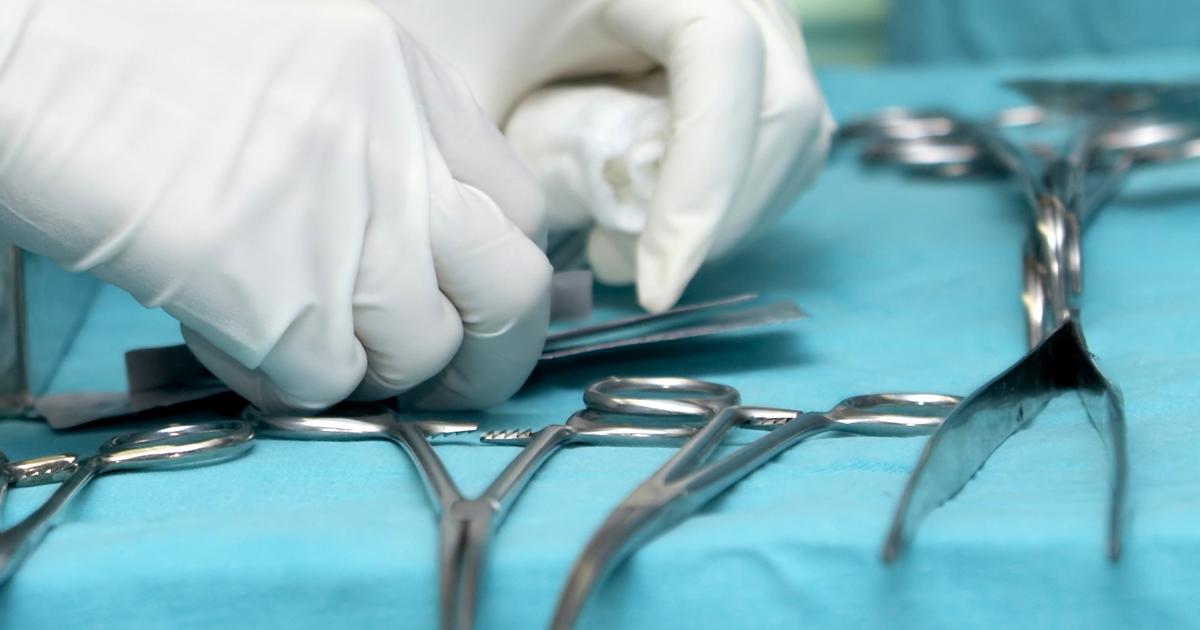
Mild cases of Ebstein's anomaly may only require regular monitoring with a specialist or medication to help adjust compromised blood flow. The more severe cases may need surgery, which includes repairing or replacing the tricuspid valve, closing connections between the atria, and repairing the pieces of the right ventricle acting as the right atrium. Surgeons may also fix abnormal heartbeats at this time by removing the muscle causing the issue or destroying the muscle through the use of catheterization and high energy radio waves. A heart transplant for Ebstein's anomaly only occurs for the most severe cases with poor heart function, and where other options have failed.
Cardiac Sarcoidosis
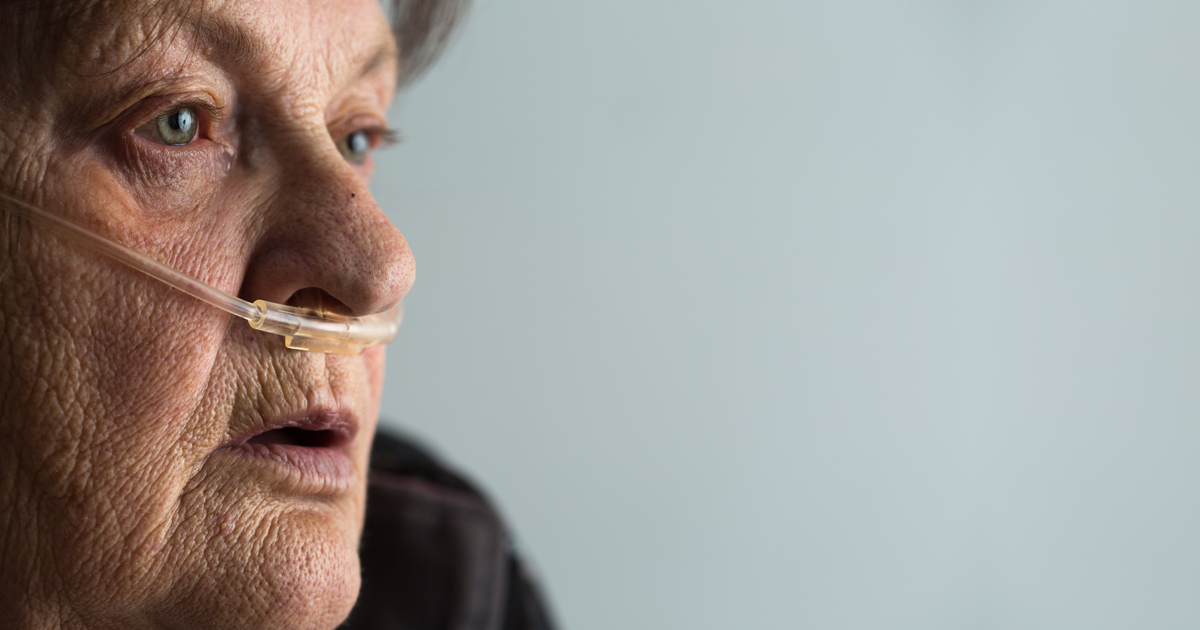
Sarcoidosis is an inflammatory condition that can affect a variety of organs. Cardiac sarcoidosis affects the heart and only occurs in a small number of those who already suffer from another type (e.g., pulmonary sarcoidosis). In this condition, granulomas (clusters of white blood cells) form within the heart tissue, most commonly where they can affect the heart’s electrical system. In severe cases, it can cause heart failure. This is considered a young person's disease, as it typically affects those between twenty-five and forty-five years old. Unfortunately, the cause is unknown, though genetics may play a part since individuals appear to be at a higher risk if they have a relative with the condition. Another possible cause is an overreaction of the immune system to an infectious agent, such as an allergen.
Symptoms include chest pain, shortness of breath, fatigue, heart palpitations, fainting, arrhythmias, and swelling from excess fluid. Most often, cardiac sarcoidosis does not require treatment. When it does, however, it includes reducing inflammation in the body through corticosteroids and managing irregular heartbeats with anti-arrhythmic drugs, catheter ablation, or an implantable cardioverter-defibrillator. A transplant may occur in the most severe cases.
Endocarditis

Endocarditis is where the endocardium, the inner lining of the heart valves and chambers, becomes infected from bacteria or other germs entering the blood, though the term has also been used to refer to endocardium inflammation resulting from other conditions. It is quite rare among individuals with healthy hearts. Risk factors for the condition include artificial or damaged heart valves, medical devices implanted in the heart or blood vessels, as well as the presence of congenital heart defects. Other factors increasing the risk of endocarditis include poor dental hygiene or using intravenous (IV) drugs.
Symptoms of this condition include shortness of breath, persistent coughing, flu-like symptoms, blood in the urine, a new heart murmur or change in an existing one, nausea or vomiting, and a loss of appetite. Skin changes include spots from broken blood vessels under the fingernails, on the chest, on the whites of the eyes, or inside the mouth, and painful red or purple bumps under the skin around the fingers and toes. Dark, flat, and painless spots on the soles of the feet or palms of the hands may also occur.
Treatment For Endocarditis
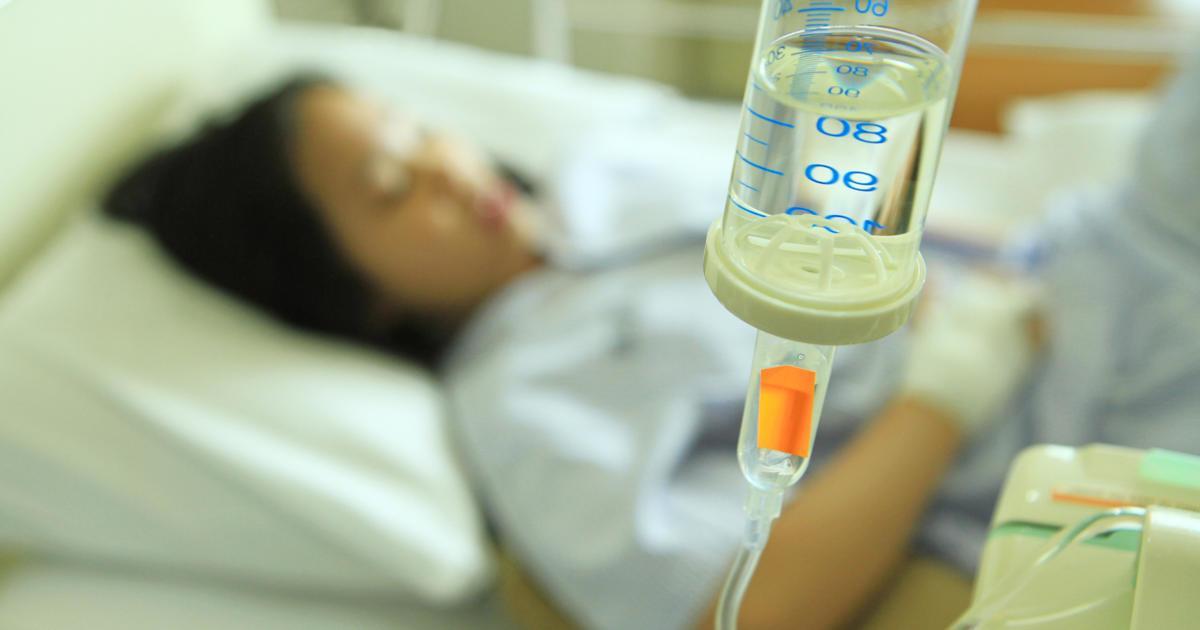
Doctors will typically treat endocarditis with antibiotics administered through an IV line in a hospital setting. This form of treatment usually lasts between two to six weeks, depending on the severity as well as the patient's response. Though it begins in a hospital setting, patients are sometimes allowed to continue the treatment at home after the first week, if they are doing well, though they will need special care to continue the IV antibiotics. Follow-up treatment usually includes a cardiologist, a doctor specializing in infectious diseases, as well as a heart surgeon. Surgery, such as replacing the heart valve or clearing the infection, is also used to treat endocarditis where antibiotics are not effective. It is particularly common for endocarditis to result from fungi since this is harder to manage than bacteria.
Eisenmenger Syndrome

Eisenmenger syndrome is a rare complication stemming from congenital heart defects. It occurs when a congenital heart defect results in a hole developing between the two major heart chambers. This hole causes abnormal blood circulation in the heart and lungs, specifically increasing pressure in the lungs and reversing the direction of blood flow. In turn, this narrows and stiffens the arteries in the lungs, causing permanent damage. Symptoms include chest pain, heart palpitations, fainting, coughing up blood, shortness of breath, and blue or gray skin. However, the most common symptom is the clubbing of hands, which means the patient has large, rounded fingernails.
Treatment for Eisenmenger syndrome includes medication, lifestyle adjustments, and frequent monitoring by a cardiologist. Lifestyle adjustments involve avoiding high altitudes, restricting strenuous exercise, avoiding situations that may lower blood pressure (e.g., saunas), always consulting about supplements and medication, and avoiding smoking. Surgery is never recommended once Eisenmenger syndrome develops, as any surgery is life-threatening with this condition. A heart-lung transplant will only be considered if no other treatments have proven effective. Women with Eisenmenger syndrome should also avoid becoming pregnant, and they should not go on birth control, as both of these raise the risk of serious complications.
