Symptoms, Risk Factors, And Causes Of Congenital Heart Diseases
When many individuals think of heart diseases, they go to the worst-of-the-worst: heart attacks, embolisms, and heart failure. However, there is a myriad of heart diseases that present themselves with a wide variety of symptoms. Some heart diseases are congenital, meaning they present at birth rather than develop later in life due to lifestyle or health complications. Some of these congenital heart diseases go undetected for years because the symptoms are not severe and can easily go unnoticed. Identifying the symptoms of congenital heart diseases can prevent these often undiagnosed conditions from causing serious health complications.
Circulation Problems
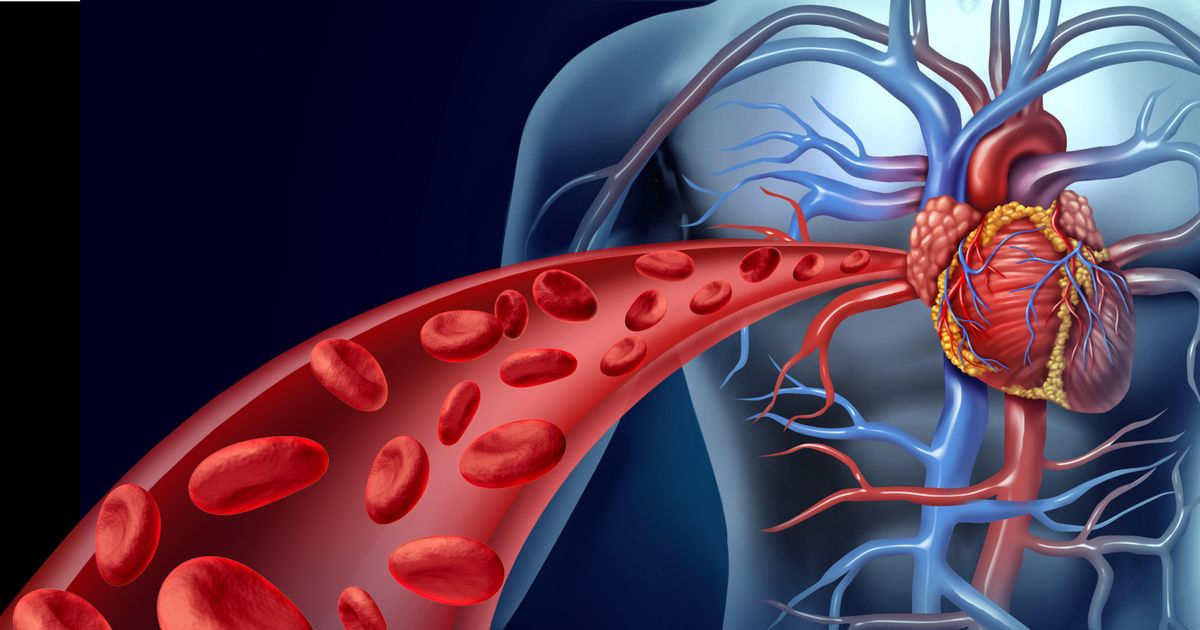
Congenital heart diseases can create a variety of circulatory issues. Any circulation problems present at birth usually can be diagnosed if an infant's skin, lips, or fingernails have a bluish hue, or if babies fall asleep while feeding. If circulation problems develop later in life, they usually present themselves in the form of swollen feet, ankles, or legs. Some individuals with circulatory issues develop painful swelling and hardness in the abdomen or neck, both of which indicate serious medical complications.
Excessive Fatigue After Physical Activity

Blood is responsible for carrying the body's various cellular waste products generated by natural processes to different organs, such as the liver, where they can be filtered out. Blood, likewise, carries various cells and proteins throughout the body, which aid in recovery after physical exertion. When blood flow throughout the body is decreased due to congenital heart diseases, wastes and toxins can build up in the blood which can create abnormal levels of fatigue, particularly after exercise. Individuals who are excessively tired after physical activity should visit the doctor to get an evaluation and determine if it is a congenital heart condition causing their symptoms or not.
Shortness Of Breath

The oxygen absorbed by the lungs is carried throughout the body by a protein called hemoglobin, which is found in red blood cells. When individuals have a congenital heart disease or defect, their overall volume of blood flow is decreased. Less blood flow means less hemoglobin, creating a slightly hypoxic state in some patients with a congenital heart disease. This slight hypoxia usually presents itself as shortness of breath, not only when exercising but also when at rest. Any chronic, unexplained shortness of breath should be reported to a doctor as soon as possible.
Frequent Buildup Of Fluid In The Lungs

The heart contains four massive valves known as the pulmonary arteries and veins, which are responsible for pumping blood in and out of the lungs. Congenital heart diseases can restrict the volume of blood flowing through these valves, creating complications throughout the respiratory system. Individuals with undiagnosed congenital heart diseases often report a chronic buildup of fluid in the lungs due to this decreased blood flow. This fluid often presents itself as chronic coughs, wheezing, or even pneumonia.
Heart Murmurs
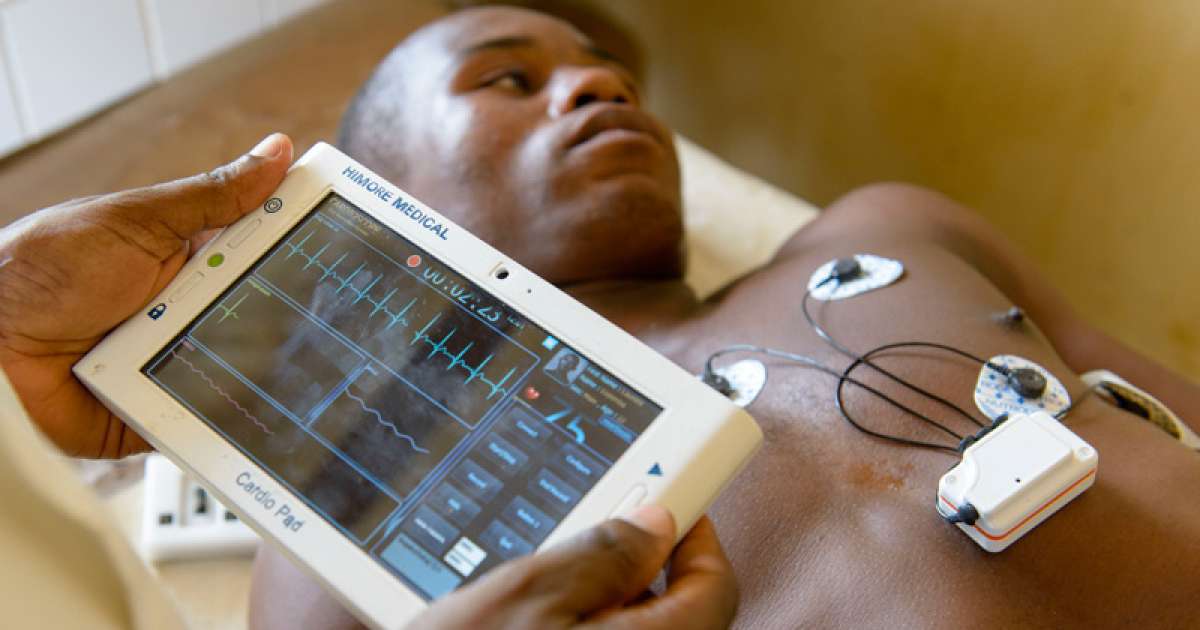
Heart murmurs are one of the primary indicators of latent congenital heart diseases or defects. A heart murmur is what medical professionals call the rushing sound of blood through the heart, and can indicate some kind of fault in the heart valves, which can lead to leaking or inefficient blood flow. For that reason, individuals should undergo routine physical examinations conducted by a doctor at least once a year. Non-invasive cardiovascular exams including auditory analysis of one's heartbeat with a stethoscope can often identify murmurs associated with congenital heart diseases. In some cases, these heart diseases are only identified after blood samples are analyzed, which is a common aspect of many annual examinations.
Cyanosis
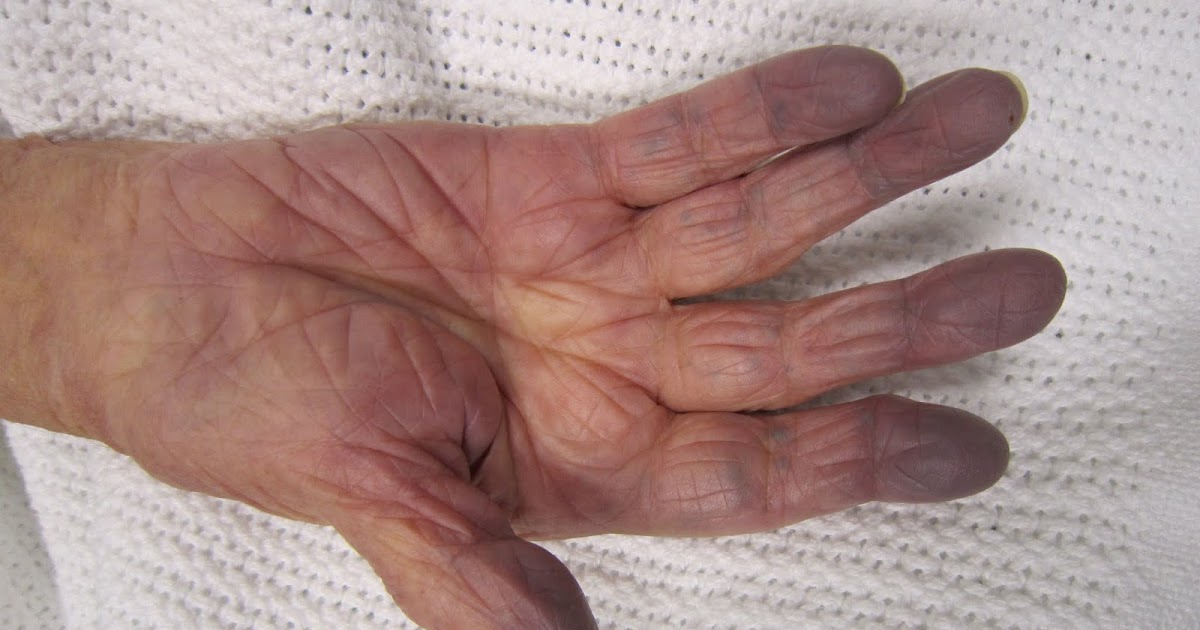
An individual who experiences cyanosis may be affected by a congenital heart disease. Cyanosis is a medical term used to describe a blueish hue to the mucous membranes or skin. Cyanosis caused by congenital heart diseases develops slowly over time. The mechanism behind cyanosis has to do with the way light reflects off the blood through the skin. Poorly oxygenated blood is a very dark red color. Blood rich with oxygen appears as a bright red color in the body. It is this difference in the color of the blood that causes light to reflect off oxygen-rich and oxygen-poor blood through the skin differently. While oxygen-rich blood yields a healthy pink skin color, the way light reflects off the dark color of oxygen-poor blood yields a grey-blue skin color.
An individual who has a congenital heart disease has a heart that does not work as it should because of structural or functional abnormalities. These abnormalities can make it difficult for the heart to pump oxygen-rich blood to all distant regions of the body. As a result, the blood inside of the small capillaries that run through the mucous membranes, to the tips of the fingers, and to the toes may have a near-constant low blood oxygen content. This malfunction causes cyanosis in an affected individual.
Edema

Individuals who experience edema may be affected by a congenital heart disease. The heart is responsible for pumping oxygen-poor blood into the lungs for gas exchange, and then back to the rest of the body once it has been re-oxygenated. The kidneys are responsible for carefully maintaining the body's balance of fluids, ensuring there is not too much or too little fluid in circulation. When the kidneys see there is excess fluid, they are responsible for filtering it out of the blood into the urine for excretion. However, the blood must be able to adequately reach the kidneys in order for fluid to be filtered from it. A heart with structural or functional defects cannot circulate blood throughout the body adequately.
As a result, the kidneys are unable to filter out fluid from poorly circulating blood properly. Poor circulation also directly contributes to the functional impairment of the kidneys from a shortage of oxygen to the kidney tissues themselves. Excess fluid in the blood leeches through the small capillaries and into surrounding tissues as a homeostatic mechanism response to fluid overload or hypervolemia. This accumulation of fluids in the tissues of the limbs and other regions is called edema.
Heredity Component
An individual is at an increased risk of having a congenital heart disease if a heredity component is present, such as a parent or sibling being affected as well. The manner of inheritance is different among different types of defects in the heart. Autosomal-dominant defects mean if one parent has a congenital heart disease, there is a fifty percent chance their offspring will also have it. Genetic syndromes that are the result of abnormalities in an individual's set of chromosomes can also increase the risk of having a congenital heart disease.
Chromosome abnormalities include missing chromosome pieces or duplicate chromosome pieces. Because the genetic code in the human chromosomes originates from an individual's parents, the majority of such defects are inherited. Around one-third of all infants with chromosomal issues that result in genetic syndromes are affected by a congenital heart defect. An individual who has a single gene defect is also at an increased risk of having a congenital heart disease. Congenital heart diseases can typically be detected while an individual is in utero during the second or third trimester of pregnancy.
Rubella
An unborn child of an individual with rubella has a greater risk of having congenital heart disease. Rubella is an infection caused by a virus characterized by the red rash it produces on the skin. While rubella is closely associated with the measles, it is caused by a different virus. Rubella is contagious and able to be transmitted from one person to the next through coughing, sneezing, saliva, and mucus. While a rubella infection is a relatively mild infection that does not usually have any long-term effects on healthy individuals, it can be particularly dangerous for an unborn child. A pregnant woman with rubella is able to give it to her unborn child through her blood.
Out of all infants born to mothers who were affected by rubella within the first twelve weeks of pregnancy, over eighty percent develop congenital rubella syndrome. The greatest risk of congenital rubella syndrome occurs within the first trimester, but it is also serious later in pregnancy. Congenital heart defects are a common complication that occurs in an unborn child affected by congenital rubella syndrome.
Diabetes

An unborn child to a mother affected by diabetes is at a greater risk of having a congenital heart disease. An estimated five percent of infants born to mothers with diabetes are affected. The risk of heart defects is even greater when the mother develops insulin resistance in the third trimester as a result of gestational diabetes. The exact mechanism of how this happens is not clear, but it is known to have to do with the effects of maternal diabetes on metabolism.
However, studies also show the degree of control the mother has over her gestational diabetes is not an influencing factor. The most common forms of congenital heart diseases in such cases include transposition of great arteries, ventricular septal defect, and aortic stenosis. Oftentimes, there is a delay in the closure of the ductus arteriosus in infants with a congenital heart disease related to maternal diabetes. Fetal echocardiograms can help detect a congenital heart disease in unborn children of mothers affected by diabetes.
