How to Treat Catecholaminergic Polymorphic Ventricular Tachycardia
Catecholaminergic polymorphic ventricular tachycardia is a rare cardiac condition that causes the heart to beat irregularly and abnormally fast. The disorder is genetic and develops due to mutations on the RYR2 or CASQ2 gene. While this type of ventricular tachycardia can be treated, it is linked with an increased risk of sudden cardiac death. Symptoms of this ailment typically present during childhood, and most patients are seven or eight years old at the time of diagnosis. Catecholaminergic polymorphic ventricular tachycardia is very difficult to detect, and it may go unrecognized even by cardiologists. The earliest symptom is usually fainting (syncope), and patients may also experience dizziness and lightheadedness. The symptoms usually appear with exertion.
Physicians can do genetic tests to diagnose this condition, and these may be recommended for immediate and extended family members of patients with this disorder. Doctors will also perform a physical examination and additional tests, which include listening to the heartbeat to identify abnormal sounds, rates, or rhythms and doing an electrocardiogram to get more detailed information about a patient's cardiac rhythm. Some patients may have a continuous electrocardiogram recording for twenty-four hours. Other tests used to diagnose Catecholaminergic polymorphic ventricular tachycardia include an echocardiogram, an exercise stress test, and MRI scans of the heart.
The following steps are some of the most common treatments for patients with catecholaminergic polymorphic ventricular tachycardia.
Treatment Through Medication
The first line of treatment for catecholaminergic polymorphic ventricular tachycardia is treatment through medication. Patients with the condition will typically be prescribed beta blockers, which need to be taken daily, and work by slowing the heart rhythm and preventing the development of an irregular heartbeat. Examples of common beta blockers include acebutolol, propranolol, atenolol, bisoprolol, nebivolol, and metoprolol. Potential side effects include depression, cold hands and feet, fatigue, weight gain, shortness of breath, and trouble with sleeping. Beta blockers should not be used by patients who have asthma. Patients with catecholaminergic polymorphic ventricular tachycardia who cannot use beta blockers or who need additional medication may need calcium channel blockers. These drugs stop calcium from entering the blood vessels of the heart, and this reduces blood pressure. Calcium channel blockers for this particular condition also slow the heart rate and regulate heart rhythm. Examples of calcium channel blockers include felodipine, isradipine, diltiazem, amlodipine, and nicardipine. Like beta blockers, these are taken daily. Possible side effects include constipation, headaches, rash, fatigue, nausea, and palpitations.
Keep reading for more on how to treat catecholaminergic polymorphic ventricular tachycardia.
Sympathetic Denervation
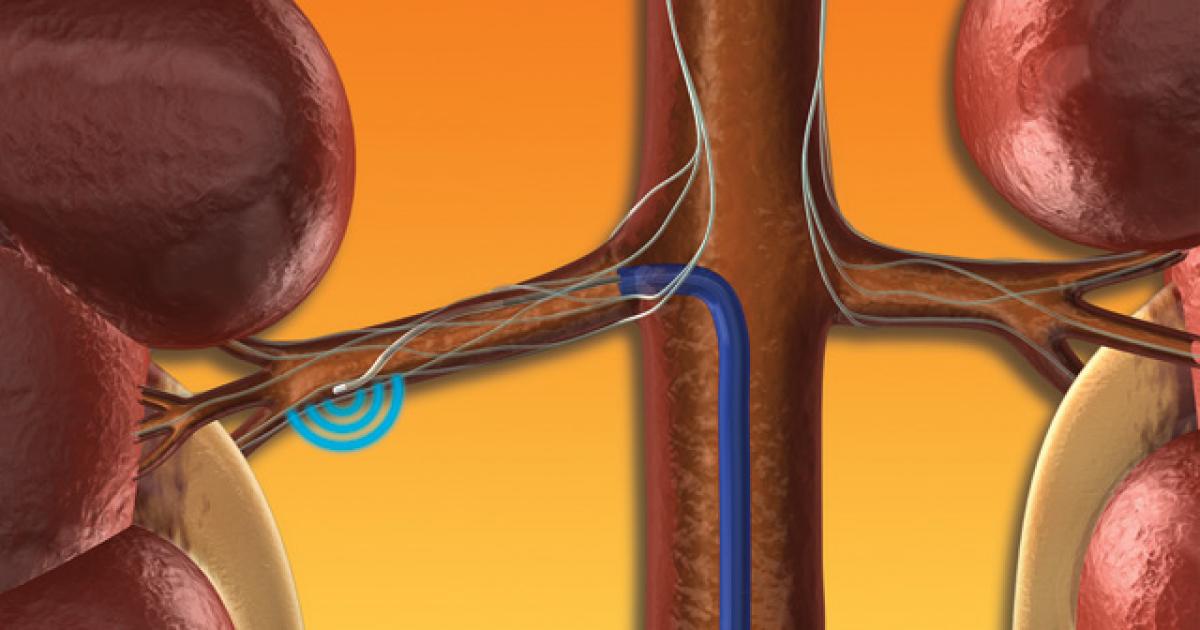
A surgical procedure known as left cardiac sympathetic denervation may be appropriate for patients who experience intolerable side effects from medication. This procedure is also recommended for patients who cannot control their symptoms through other methods. Sympathetic denervation involves removal of the nerves that supply adrenaline, a hormone that tells the heart to beat more quickly. This can reduce episodes of fainting and other symptoms caused by catecholaminergic polymorphic ventricular tachycardia. The procedure is performed under general anesthesia, and surgeons may use videoscopic equipment to assist them during the operation. The surgery usually lasts around forty minutes, and patients will be closely monitored with follow-up appointments. Before the procedure, patients will have a pre-op appointment, which may include a physical exam and tests such as an electrocardiogram.
Learn more about methods of treating catecholaminergic polymorphic ventricular tachycardia now.
Implantable Cardioverter-Defibrillator
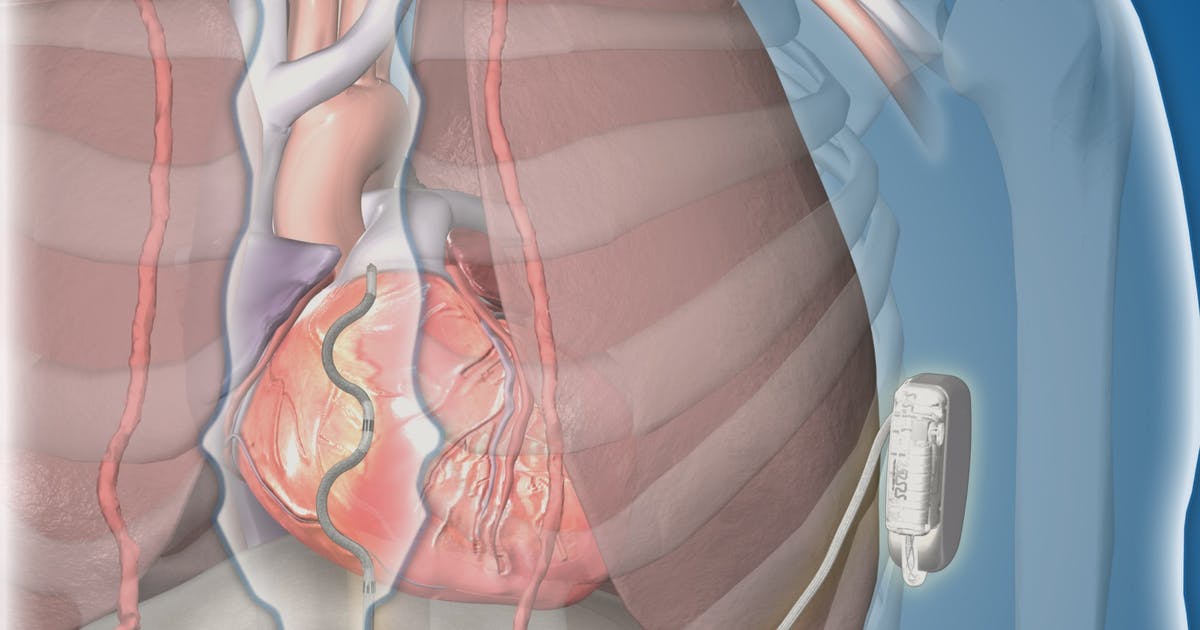
An implantable cardioverter-defibrillator is often advised for patients who have not responded to treatment with medications, and it is typically performed before more invasive treatments. Doctors generally recommend that an implantable cardioverter-defibrillator be considered when patients taking beta blockers continue to have fainting spells or experience an episode of cardiac arrest. Surgeons implant the cardioverter-defibrillator underneath the skin, and thin wires connect the device to the patient's heart. The device continuously monitors the patient's heart rate. If an abnormal rate is detected, the device generates an electric shock that restores the heart to a normal rhythm. Implantable defibrillators are crucial in preventing sudden cardiac death. After having the device placed, patients may need eight weeks to adjust. They may experience jerky arm movements during this time, but these will typically settle after eight weeks. Patients should also watch for any mood changes, depression, or anxiety after surgery and report these to their medical team.
Reveal the next strategy for treating catecholaminergic polymorphic ventricular tachycardia now.
Avoid Strenuous Exercise And Competitive Sports

Patients with catecholaminergic polymorphic ventricular tachycardia often experience fainting, rapid heartbeat, and irregular heart rhythms during and after exercise. Since exercise is such a strong trigger, patients with the disorder are advised to avoid strenuous exercise and competitive sports. Exercise is important for overall cardiac health, but patients with this form of ventricular tachycardia need to involve their doctors in the process of choosing a safe exercise routine. Before starting any exercise regimen, patients should visit their cardiologist for a checkup. The cardiologist can assess the patient's cardiac and overall health. They will listen to the patient's heart and lungs and may perform tests. The patient's cardiologist can recommend types of exercise that are safe and appropriate for each patient. Generally, lighter exercises such as yoga, tai chi, and gentle walking can be safely performed. Doctors will advise patients about safe exercise time limits and how often they should exercise each week. Patients may wish to exercise under the supervision of a personal trainer or join an exercise class for patients with chronic health conditions. Patients may want to monitor their heart rates while exercising.
Discover more ways to effectively treat catecholaminergic polymorphic ventricular tachycardia now.
Avoid High-Stress Environments

Stress is harmful to the heart and can increase heart rate and blood pressure. In some individuals, very high levels of stress may cause fainting, palpitations, irregular heart rhythms, or abnormally fast heart rates. For this reason, patients with catecholaminergic polymorphic ventricular tachycardia are advised to avoid high-stress environments. Patients need to be mindful of the stress they experience at work, home, and school. Patients can practice breathing exercises and healthy coping mechanisms to lower stress levels. Patients experiencing chronic or unmanageable stress may wish to see a counselor to learn practical methods for reducing stress and making healthy changes in their lives. Stress reduction methods include keeping a journal, practicing meditation, gentle yoga, massage therapy, and talking with friends.
