How To Treat Paroxysmal Supraventricular Tachycardia
Paroxysmal supraventricular tachycardia (PSVT) is a type of irregular heart rhythm or heart arrhythmia where an individual's heart rate becomes excessively fast, starting and stopping suddenly. This irregularity typically occurs when an abnormal electrical pathway in the heart muscle causes a type of short-circuit in the heart's electrical system that results in episodes characterized by a rapid and symptomatic elevated heart rate. Symptoms of PSVT include sudden rapid pulse, anxiety, heart palpitations, chest pain or tightness, shortness of breath, dizziness, and fainting in some cases. While paroxysmal supraventricular tachycardia itself is typically not a life-threatening type of heart condition, it can cause an individual to experience debilitating symptoms and complicate other heart problems. Diagnosis of paroxysmal supraventricular tachycardia is made using an electrocardiogram, echocardiogram, Holter monitor evaluation, or electrophysiology study..
Catheter Ablation
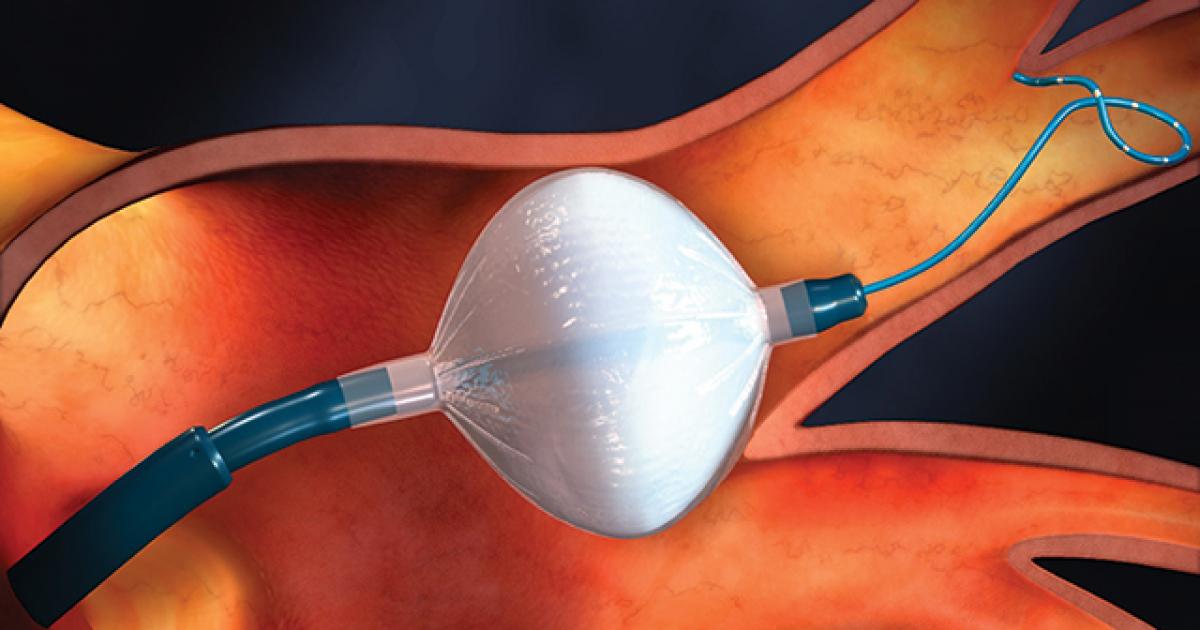
Severe cases of PSVT causing debilitating symptoms in an affected individual may require catheter ablation for treatment. Paroxysmal supraventricular tachycardia patients have an abnormality of the tissues separating the upper and lower chambers of the heart. Healthy individuals have an atrioventricular septum that is made up of fibrous tissue that is not contractile like regular muscle tissue. Individuals who have PSVT have an extra muscular section of cells connecting the atria and ventricles that allow for the inappropriate conduction of electrical signals. The signals can cause a contraction and may quickly circle back up to the atria, resulting in PSVT.
Catheter ablation is a procedure involving the use of a catheter and tool that emits high-frequency radio wave energy. The tool is threaded by the catheter to the identified abnormal muscle tissue and then used to destroy the cells that make up these fibers. This procedure had a lower success rate before the introduction of technological advances and endocardial mapping. These tools allow cardiologists to map out the heart tissue and locate the atypical fibers for better precision during the ablation procedure. The success rate of this procedure current day is ninety percent in individuals who have a confirmed and mapped atypical connection causing their condition.
Vagal Maneuvers

Vagal maneuvers can be used to treat PSVT. Vagal maneuvers are utilized at the time the affected individual is having an episode. This treatment method involves the use of certain actions a patient is instructed to take at the onset of an episode to disrupt the symptoms they are experiencing. Vagal maneuvers work by attempting to increase vagal tone (the activity of the vagus nerve). The vagus nerve is a critical component of the autonomic nervous system responsible for cardiac regulation alongside numerous other functions.
The Valsalva maneuver is characterized by an attempt to forcefully exhale air through an airway that is closed during a paroxysmal supraventricular tachycardia episode. Other vagal maneuvers commonly used during episodes include coughing while bending the torso forward in a sitting position, and rinsing the face numerous times with ice water. These uncomplex maneuvers have been proven to decelerate the conduction of electrical impulses through the atrioventricular node of the individual's heart, effectively interrupting their symptomatic episode.
Carotid Sinus Massage
In settings where a medical professional is present and an affected individual experiences a PSVT episode, a carotid sinus massage may be able to treat their symptoms. The carotid sinus is a spot of local swelling in the carotid artery that manages and adjusts an individual's blood pressure at times when it becomes too high or low. This type of massage is performed by placing pressure with a circular motion on the carotid sinus for approximately ten seconds. This technique should only be used when administered by a physician and with monitoring of the patient's heart rate and blood pressure throughout. This maneuver is used to stimulate a decrease in heart rate at times when an individual has symptoms to produce an effective interruption and termination of the episode. Not all PSVT patients are good candidates for this type of maneuver. Individuals also affected by chronic hypotension, carotid arterial stenosis, history of blood clots, and a history of smoking should not use this method as a treatment for their symptoms.
Cardioversion

Some cases of symptomatic PSVT in affected individuals require treatment through a procedure called electrical cardioversion. Electrical cardioversion is the use of electrical shocks to restore a normal heart rhythm. This is a procedure performed in a hospital setting under the effects of intravenous sedation. Large patches containing electrodes are placed on the patient's chest and are connected to a device called a cardioversion machine. This machine is a type of specialized defibrillator with the ability to record the patient's heart rhythm during the procedure. It also delivers electrical shocks to the heart to help restore a normal heart rhythm. This machine is also capable of correcting bradycardia following the cardioversion procedure if that complication occurs. Some individuals with PSVT will require repeat cardioversion procedures to maintain normal heart rhythm. The concept behind this treatment is similar to how a portable defibrillator works in the event of a cardiac emergency, but it is done in a more carefully controlled and monitored process.
Medication

Medication can be used to treat individuals affected by symptomatic paroxysmal supraventricular tachycardia. Both short term and long term management methods of PSVT can include the use of certain medications to mediate symptoms. For immediate treatment, verapamil or adenosine may be used. Intravenous adenosine begins working between ten and twenty-five seconds following administration to a vein. This type of drug is helpful to mediate PSVT episodes, but it does not stay in the body long enough to produce adverse side effects. Verapamil is a calcium channel blocker that is just as effective as adenosine, but it has a later onset and inotropic impacts contraindicated in those who are hypotensive or have congestive heart failure. Other calcium channel blockers that may be used in the short-term management of PSVT symptoms include esmolol and diltiazem. For long term treatment, medications such as procainamide, verapamil, atenolol, amiodarone, diltiazem, and metoprolol may be utilized. Oral forms of these beta-adrenergic blockers and calcium channel blockers have been successful in managing recurrent symptoms associated with paroxysmal supraventricular tachycardia.
