Everything You Need To Know About Atrial Fibrillation
Atrial fibrillation is an irregular, sometimes rapid heart rate that increases an individual's risk of heart-related complications including stroke and heart failure. The atria, the heart's upper chambers, beat out of sync with the ventricles, the lower chambers of the heart. Atrial fibrillation is the most common condition of irregular heart rhythm and exists in at least one percent of the population. The condition becomes more common as age increases. It is rare in young people and more common in individuals over eighty years old.
Symptoms Of Atrial Fibrillation

Not all patients experience symptoms of atrial fibrillation, but those who do may experience the following: shortness of breath, dizziness, fatigue, weakness, confusion, light-headedness, poor exercise tolerance, and sweating. These symptoms are usually related to insufficient blood flow. Patients may also feel racing or flip-flopping sensations in their heart that cause discomfort. The feeling of pressure or pain in the chest may indicate a heart attack is about to occur, and immediate emergency medical attention should be sought out. Symptoms of atrial fibrillation may be occasional, persistent, or permanent. Occasional symptoms may be felt for minutes or hours, disappear and return later, persistent symptoms do not go away and require medical attention, and permanent symptoms will always be present and require medication for heart rate control.
Causes Of Atrial Fibrillation

Atrial fibrillation can be caused by many different diseases, and some cases do not have any identifiable cause. Some of the most common causes of atrial fibrillation include pulmonary embolism, heart bypass surgery, pneumonia, decongestant medications, diet pills, caffeine consumption, tobacco use, illegal drug use, alcohol abuse, congenital heart disease, heart attack, cardiomyopathy, valvular heart disease, heart failure, and coronary artery disease. All of these conditions cause some type of interference with or damage to the patient's electrical system within their heart. Mechanisms that cause hypoxia, a lack of oxygen, in the coronary arteries can cause permanent damage the body attempts to repair. Damaged heart tissue is repaired with dense and fibrous scar tissue that can cause problems with the electrical system in the atria of the heart, leading to the development of atrial fibrillation.
Atrial Fibrillation Risk Factors

An individual may be at an increased risk of developing atrial fibrillation if certain factors apply to them. Risk factors for atrial fibrillation are a blend of lifestyle choices, individual characteristics, and certain medical conditions. Patients affected by diabetes, high blood pressure, coronary artery disease, chronic obstructive pulmonary disease, prior heart attacks, congestive heart failure, structural heart disease, thyroid disease, chronic lung disease, sleep apnea, and chronic kidney disease are at a higher risk of developing atrial fibrillation than unaffected individuals. Individuals who are overweight, obese, smoke regularly, drink excessive amounts of alcohol, are physically inactive, consume excessive amounts of caffeine, use illegal stimulants, and consume a high-fat diet are also at a higher risk than others of developing atrial fibrillation. Certain genetics that cause individuals to have higher levels of lipids in their blood, high blood pressure, abnormal vascular makeup, a higher risk of autoimmune disease, and many others can cause an individual to be at an increased risk of developing atrial fibrillation.
Complications Of Atrial Fibrillation
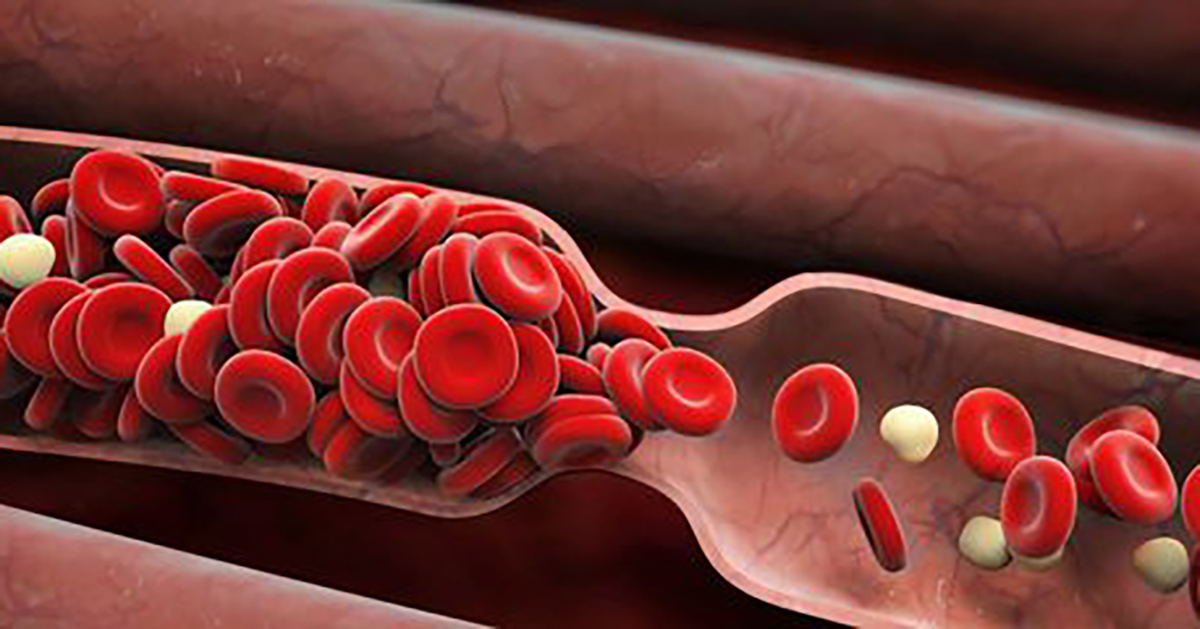
If individuals experience symptoms of atrial fibrillation, it is important to be checked by a doctor so the condition can be ruled out or diagnosed. If atrial fibrillation is left untreated, numerous possible complications may occur, including stroke, cardiomyopathy, and Alzheimer's disease. Atrial fibrillation left untreated increases the risk of blood clots forming in the heart, which can then travel to the brain where it blocks blood flow, resulting in a stroke. Patients with atrial fibrillation are at least four to five times more likely to have a stroke than individuals without the condition. Cardiomyopathy is a group of diseases that affect the heart and occur as a result of the weakening of heart muscles when atrial fibrillation is left untreated. Cardiomyopathy often leads to heart failure. Experts suggest atrial fibrillation also increases the risk of Alzheimer's disease. Studies have shown cognitive decline at a younger age is more prevalent among atrial fibrillation patients.
Atrial Fibrillation And Stroke Facts

When atrial fibrillation remains untreated, the potential for blood clots forming in the heart is increased, and these blood clots can then travel to the brain and block blood flow, resulting in a stroke. Atrial fibrillation patients are four to five times more likely to experience a stroke, and up to fifteen percent of strokes are caused by untreated atrial fibrillation. Researchers do not know the length of time it takes for untreated atrial fibrillation to result in a blood clot in the brain, but studies have shown an electrical shock to the heart for atrial fibrillation increases stroke risk for two to four weeks afterward. It is presumed that the shock causes previously formed clots to dislodge and lead to stroke.
Diagnosing Atrial Fibrillation

If a doctor suspects their patient may be affected by atrial fibrillation, they may refer them to a physician who specializes in heart conditions and diseases to confirm a diagnosis. Patients may also be referred to a physician who specializes in irregular heartbeats. Both of these types of physicians will likely perform a physical examination on the patient to listen to the rate and rhythm of their heart, take blood pressure and pulse, listen to their lungs, and check for other signs indicative of valve or muscle problems. An individual may need to have an electrocardiogram or EKG so their doctor can see the rhythm of their heartbeat, speed of their heartbeat, the strength of electrical signals in the heart, and the timing of the electrical signals in the heart. An individual may need to wear a Holter monitor for between twenty-four to forty-eight hours to record the electrical activity of their heart. Other tests can assist with the diagnosis of atrial fibrillation include an event monitor, stress test, mobile cardiac telemetry, echocardiogram, transthoracic echocardiogram, transesophageal echocardiogram, chest x-ray, blood tests, CT scan, MRI scan, portable electrocardiogram, fitness tracking, and a tilt table test.
Treatments For Atrial Fibrillation

Treatment for atrial fibrillation depends on several factors including the extent and severity of the disease. Generally, three types of treatment are required: treatment for a rapid heartbeat, treatment for an irregular heartbeat, and treatment to prevent blood clots. Doctors may prescribe medication to fix a rapid heartbeat and will sometimes prescribe medication for an irregular heartbeat. If the irregular heartbeat is not corrected by medication, the doctor may offer other treatments including low-intensity electric shock and surgery. To prevent blood clots, patients may be prescribed an anticoagulant if their risk of a stroke is high. The doctor may also advise patients on lifestyle changes to improve their condition including a healthy balanced diet, regular exercise, limiting salt and fat, and losing weight.
Medications Prescribed For Atrial Fibrillation

There are many medications to help treat atrial fibrillation. These medications help control the heart's rate and rhythm and reduce the risk of stroke. Some examples of medications prescribed for atrial fibrillation include antiarrhythmics, cardiac glycosides like digoxin, and anticoagulants like warfarin. Antiarrhythmics, such as propafenone and amiodarone, help restore the normal rhythm of the heart. The medications effectively treat atrial fibrillation but may come with some side effects like dizziness, nausea, and fatigue. Digoxin helps control the rate of the heart at rest. Some patients might require additional medication, such as beta-blockers, to help control their heart rate during activity. Patients on blood thinners like warfarin to treat their atrial fibrillation have an increased risk of severe bleeding so are closely monitored. Newer anticoagulants are more effective and safe than older ones.
Preventing Atrial Fibrillation

Individuals can take several steps to help prevent the development of atrial fibrillation. One of the best ways for an individual to lower their chances of developing atrial fibrillation and many other life-threatening conditions is to obtain and maintain a healthy body mass. A healthy weight can be achieved with a balanced diet and regular exercise. Individuals who are overweight have a twenty-five percent greater risk of developing atrial fibrillation, and individuals who are obese have a sixty percent greater risk of developing atrial fibrillation. Regular smokers can stop smoking to help prevent the development of atrial fibrillation. An individual can also lower their risk by limiting their consumption of substances that contain large amounts of caffeine and alcohol. An individual who wants to prevent atrial fibrillation should treat any underlying disorders or conditions that can cause electrical problems in their heart. Being aware of a family history of heart disease, diabetes, and other causative conditions can help patients identify the signs of atrial fibrillation before it can produce complications.
Atrial Flutter

Atrial flutter is a term used to describe when an individual has a short circuit in their heart that causes the atria to contract very rapidly in a regular pattern. A small area in the right atrium of an individual's heart called the sinus node is what initiates a heartbeat. A circular electrical pathway in the right atrium is what causes the upper chambers to contract between 240 and 340 times per minute. The chambers of an affected individual's heart cannot fill completely between heartbeats when the atria are rapidly contracting in this manner. Atrial fibrillation is another type of heart arrhythmia that occurs when an individual's atria beat irregularly. These two forms of atrial tachycardia can be identified individually because they are caused by different patterns of electrical impulses being produced in an affected individual's atria. Both of these arrhythmias are detrimental to the health of an individual's heart and can cause further complications in multiple systems within the body.
