The Basics Of Chronic Kidney Disease
An estimated 661,000 Americans are affected by chronic kidney disease and are dealing with kidney failure, and of these individuals, 468,000 patients are on dialysis and 193,000 are living with a functioning kidney transplant. Approximately half of the patients living with chronic kidney disease also have diabetes or cardiovascular disease, and some even have both. Learn more now about the causes, symptoms, available treatments, and preventative measures individuals should be aware of if they or a loved one are living with chronic kidney disease.
What Is Chronic Kidney Disease?
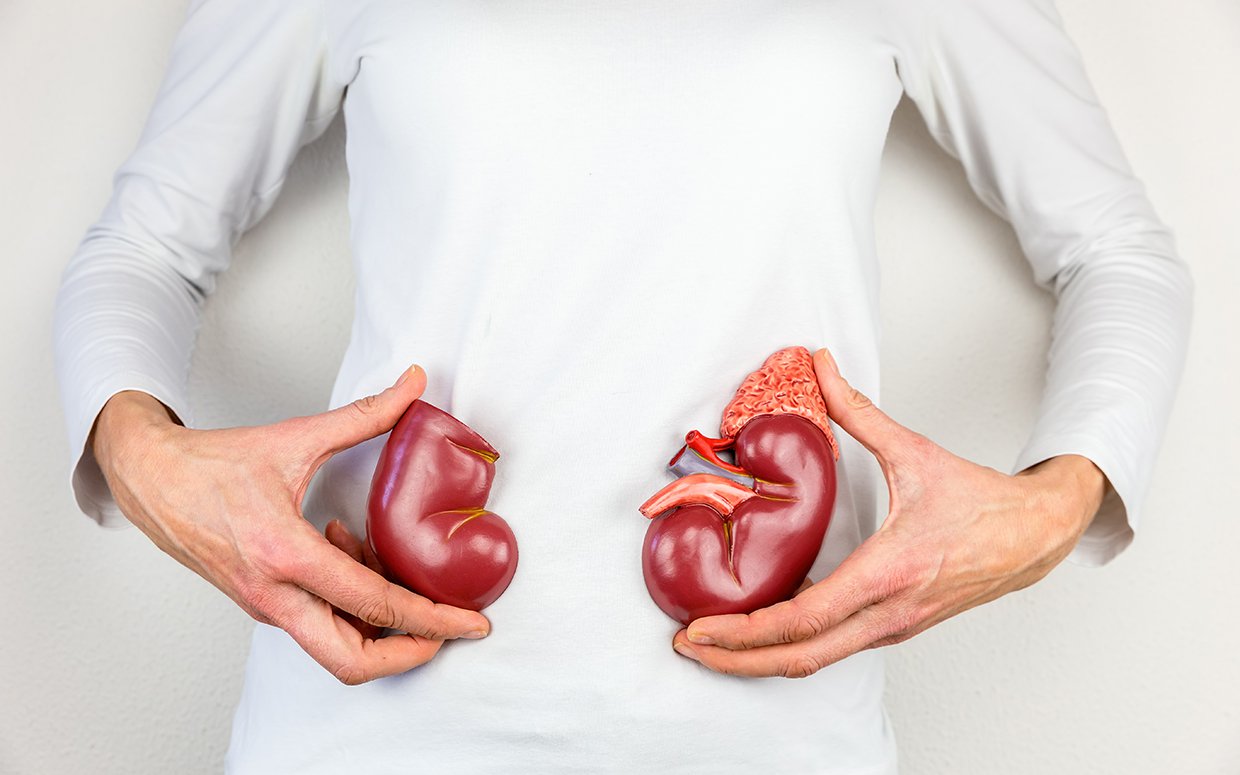
Chronic kidney disease, also known as chronic kidney failure, is characterized by the gradual loss of function of one or both kidneys. The kidneys are vital organs as they filter wastes and excess fluid from the blood, which are then excreted through urine. When chronic kidney disease has reached a progressive stage, incredibly hazardous levels of fluid, electrolytes and wastes can build within the body, which can lead to acute renal failure. It is essential for individuals to know if they are suffering from this illness, it may not become apparent until their kidney function is significantly impaired and has already progressed.
Treatment for chronic kidney disease focuses more on slowing the progression of kidney damage, typically with healthcare professionals focusing and controlling the underlying cause of the disease. Unfortunately, chronic kidney disease can progress to end-stage kidney failure, which can be fatal without the patient receiving dialysis or a kidney transplant.
Symptoms To Be Aware Of

Symptoms of chronic kidney disease develop slowly over an extended period, especially if damage to the kidneys progresses slowly. Signs and symptoms of this illness include nausea, vomiting, loss of appetite, fatigue and weakness, sleep issues, changes in urination, a decrease in mental sharpness and focus, muscle twitches and cramps, and swelling of the feet and ankles due to water retention.
Other symptoms include persistent itching, chest pain if enough fluid builds up around the lining of the heart, shortness of breath due to fluid buildup in the lungs, and high blood pressure that can be difficult to manage. These common symptoms are often nonspecific, meaning they can also be signs of other medical conditions. Due to the kidneys being highly adaptable and able to compensate if they begin to lose functioning abilities, symptoms may not appear until irreversible damage has been done to the organ.
Causes Of Chronic Kidney Disease
Chronic kidney disease is the result of another medical condition or other factor impairs the function of an individual's kidneys and causes kidney damage to worsen over an extended period. There are many potential conditions and other factors that contribute to this, including a urinary tract infection that becomes a kidney infection that further develops into kidney disease. Prolonged obstruction of the urinary tract, such as through kidney stones, some forms of cancer, and an enlarged prostate in men, can also result in chronic kidney disease. Another major factor is pyelonephritis, which refers to recurrent kidney infections.
Medical Risk Factors For Chronic Kidney Disease

Two of the most significant medical risk factors of chronic kidney disease include diabetes and high blood pressure. Diabetes is a disease where a patient's body cannot appropriately manage its blood sugar levels. Individuals affected by diabetes often have high blood sugar, which causes damage to the small blood vessels inside of their kidneys. The kidneys are not able to properly filter the blood without these healthy vessels, causing a decrease in function.
On the other hand, long-term hypertension causes an affected individual's renal arteries to become hardened, narrowed, or weakened. This malfunction results in reduced blood delivery to the tissues of the kidneys, reducing their function. Other less common medical risk factors for chronic kidney disease include glomerulonephritis or irritation of the small filters in the kidneys, interstitial nephritis (inflammation of the kidney's tubules and structures), injury to the kidney, vesicoureteral reflux (where urine backs up in the kidneys), lupus, IgA nephropathy, and polycystic kidney disease.
Other Risk Factors For Chronic Kidney Disease
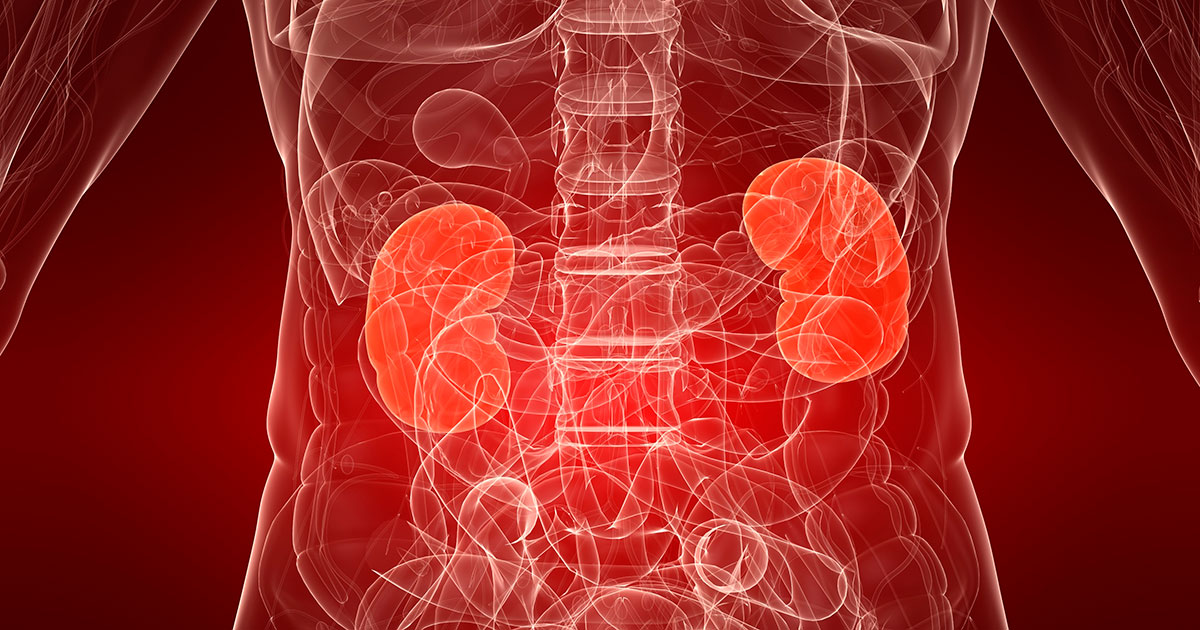
Some ethnicities are more likely to develop chronic kidney disease for unclear reasons. However, the increased risk is thought to be associated with a higher incidence of diabetes and high blood pressure in specific ethnic and racial populations. This risk factor may also be related to the geographic location of such individuals and their level of healthcare access. The groups at a higher risk include Hispanics, Asian-Americans, African Americans, and Native Americans.
Another risk factor that increases an individual's risk of developing chronic kidney disease is their age. As an individual goes through the natural aging process, their kidneys naturally but slowly decrease in their functionality. In addition, older individuals are more likely to be affected by high blood pressure and diabetes than younger individuals. Generally, individuals older than sixty are more likely to develop chronic kidney disease. Certain lifestyle choices also play a role in increasing an individual's risk for developing this disease, including poor diet, obesity, and smoking.
Complications Of Chronic Kidney Disease

Unfortunately, chronic kidney disease can affect almost every part of the body and even a patient's diet. Possible complications include fluid retention, which can lead to swelling of the arms or legs; high blood pressure; fluid in the lungs known as pulmonary edema; hyperkalemia or a sudden increase in potassium levels in the blood, which can impair the heart's ability to function; cardiovascular disease; and anemia.
Further complications include weak bones that increase the risk of bone fractures, a decreased libido, erectile dysfunction or reduced fertility, and focus or personality issues. Patients may also experience damage to their central nervous system, which can lead to seizures. There may also be a weakening of the immune system, inflammation of the saclike membrane surrounding the heart (pericarditis), pregnancy complications, and irreversible kidney damage.
Diagnosing Chronic Kidney Disease

The first step of diagnosing chronic kidney disease is a doctor will discuss personal and family medical history with the patient. This includes whether or not the patient has previously been diagnosed with high blood pressure, has taken any medications that can impair kidney function, and changes in their urinary habits, including frequency. Doctors will typically perform a physical exam and check for signs of issues with the heart or blood vessels. They will also conduct a neurological exam.
For an accurate kidney disease diagnosis, there are four different tests a doctor may perform on a patient including blood tests, urine tests, imaging tests, and even a biopsy on a piece of kidney tissue. Blood tests can determine the level of waste present in the blood, such as creatinine and urea, urine tests can reveal abnormalities associated with chronic kidney disease, and imaging tests, such as an ultrasound to assess the structure and size of the kidneys. A kidney tissue biopsy can be performed to determine if the patient does indeed have this illness or determine what else might be causing their kidney problems if they have visible symptoms.
Treatment Options

Currently, the only way to cure chronic kidney disease is with a kidney transplant. Treating chronic kidney disease is based on the individual's level of kidney function and other factors. Most often, an affected individual will be treated using medications to lower blood pressure, cholesterol levels, and inflammation levels in combination with hemodialysis or peritoneal dialysis. However, kidney damage can continue to worsen, even if the cause has been effectively controlled, such as with high blood pressure. Lifestyle changes include a lower protein diet to reduce waste within the blood, as well as patients reducing their intake or avoiding foods high in potassium and salt while increasing their iron consumption.
Potential Future Chronic Kidney Disease Treatments
There are still improvements to be made in the treatment of chronic kidney disease, and there are four potential technologies that could make groundbreaking improvement in the management of chronic kidney disease. The human nephron filter is an implantable artificial system of nephrons that functions on a continuous basis to filter the patient's blood. Membrane-free dialysis using micro-fluid technology is another possible mechanism to create a portable artificial kidney.
A wearable artificial kidney is a prototype of a portable hemodialysis device that would eliminate the need for an affected individual to come to a medical facility to have their dialysis. The wearable artificial kidney for peritoneal dialysis is another prototype that helps the at-home technique of peritoneal dialysis become more convenient and place less limitation on a patient's daily life.
Preventative Tips

Considering the severity of this illness, and how it can become fatal if left untreated or improperly cared for, individuals who are prone to developing chronic kidney disease should consider taking preventative measures to reduce their risk. One preventative tip, although common sense, is for patients to follow instructions on over-the-counter medications, such as nonprescription pain relievers such as ibuprofen and acetaminophen. Ingesting too many pain relievers could lead to kidney damage and should be avoided if the patient already has kidney disease. Another helpful piece of advice is to eat a healthy, balanced diet and maintain a healthy weight with regular exercise.
If an individual needs to shed a few pounds, they should consult their doctor about the best strategies for healthy weight loss. Also, it is important to quit smoking or not start in the first place, as cigarette smoke can damage the kidneys and worsen the pre-existing damage. Lastly, an individual should manage their medical conditions with the help of their doctor because if they have a pre-existing condition that increases their chances of developing kidney disease, they will need to work closely with their doctor to control them.
