Guide To Treating Glomerulonephritis
Glomerulonephritis is defined as a range of inflammatory conditions that affect the glomeruli or the tiny blood vessels inside of the kidneys, which are the organs responsible for filtering the blood of excess fluids and wastes. The glomeruli are the millions of tiny filters that allow the kidneys to perform this function. Individuals with glomerulonephritis have kidneys that cannot remove excess fluids and wastes efficiently because the glomeruli have become damaged. In addition, the blood of a glomerulonephritis patient will be lacking in protein. This happens because this condition causes proteins to be expelled in the urine rather than entering the bloodstream. Often, an infectious disease such as tuberculosis will result in glomerulonephritis. Viral infections, long term use of certain medications, sickle cell disease, HIV, and other systemic diseases can also bring about glomerulonephritis. Treatment of this type of condition will be based on the underlying cause and the severity of symptoms.
Get to know the most common options for treating glomerulonephritis now.
Kidney Dialysis
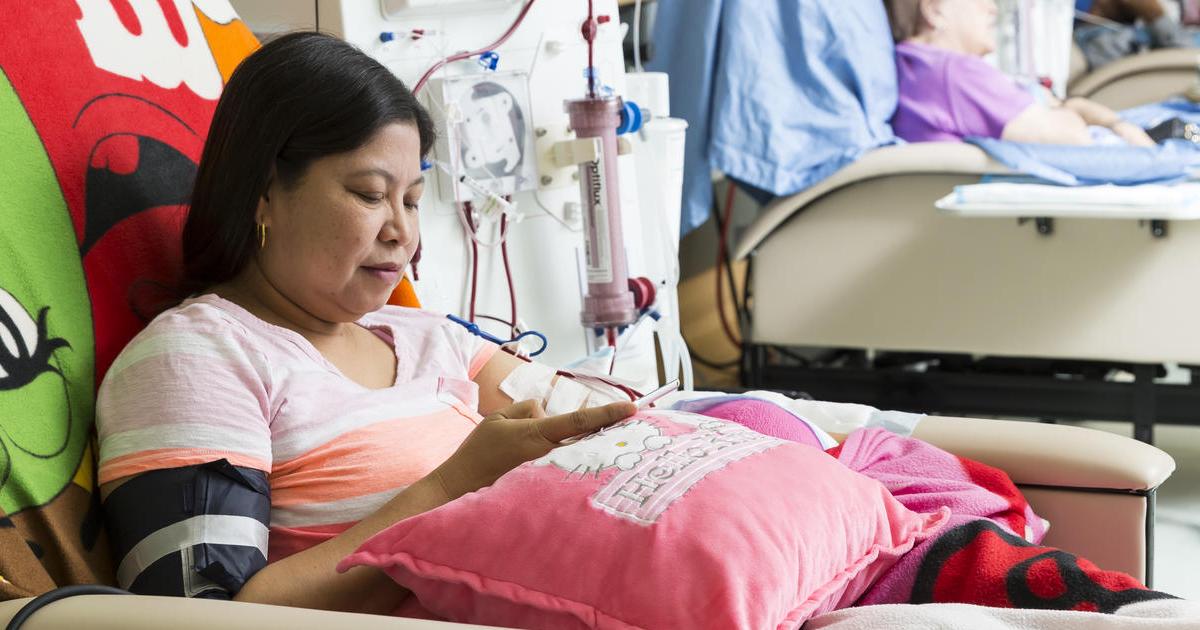
In particularly severe cases of glomerulonephritis, a patient may develop acute kidney failure, which occurs when the kidneys suddenly stop functioning. Because glomerulonephritis is inflammation of the tiny filters in the kidneys, it can cause them to temporarily stop working. In addition, when glomerulonephritis is left untreated over a long period, the patient can develop chronic kidney disease. In both cases, kidney dialysis will be needed to take over the duty of the kidneys until they can function properly again. Hemodialysis is the type of dialysis most commonly used in patients who have glomerulonephritis. When an individual undergoes hemodialysis for this condition, a catheter is inserted into a vein in the groin or neck. A pump in the dialysis machine draws out the patient's blood and filters out extra wastes, fluid, and salt. The filtered blood is then sent back to the patient's body. It takes around three to five hours for the machine to filter all the blood, and this process is done three times a week. If the acute kidney failure and glomerulonephritis improves, the patient may be able to come off of dialysis at some point.
Uncover more treatments for glomerulonephritis now.
Kidney Transplant
Glomerulonephritis may cause permanent damage to the glomeruli. If this occurs, depending on the extent of the damage the individual may develop chronic kidney disease. In extremely severe cases, a patient who started off with glomerulonephritis may end up with end-stage renal disease. Individuals who have chronic kidney disease or end-stage renal disease may require a kidney transplant in order to live. Because of the shortage in healthy donor kidneys and the tedious matching process, most patients end up on dialysis while waiting for a donor kidney. A donor kidney may come from someone who has just died or a deceased donor. The organ may also come from a live donor since individuals are able to survive with one healthy kidney. Living donor transplants last on average between fifteen and twenty years, while a deceased donor transplant lasts on average between ten and fifteen years. In terms of glomerulonephritis, the underlying medical condition or disease may still affect the patient's body. Unless steps are taken to effectively treat the underlying problem, there will always be a risk of developing glomerulonephritis in the newly transplanted kidney.
Continue reading to reveal more ways to treat glomerulonephritis now.
Reduce Consumption Of Salt

Patients may be told to reduce their consumption of salt to help treat glomerulonephritis. Salt or sodium is an electrolyte that regulates the quantity of fluid within the body. When the blood sodium levels are high, the kidneys respond by retaining water. This causes the blood volume to increase, and blood pressure follows suit. This results in the worsening of kidney disease due to the strain high blood pressure puts on the impaired kidneys. To help prevent further kidney damage, a patient will be instructed to refrain from putting salt in any of their foods. Additionally, processed foods, canned foods, processed meats, and salted snacks will need to be completely eliminated from the patient's diet. The physician will recommend using sodium-free spices and fresh herbs in the place of salt. While most individuals on a low salt diet would jump for salt substitutes, those who have glomerulonephritis should avoid them entirely because they only replace sodium with potassium.
Get the details on more options for treating glomerulonephritis now.
Lessen Protein And Potassium In The Diet

A physician may recommend for patients with glomerulonephritis to lessen protein and potassium in their diet. The objective of this restriction is to reduce the risk of developing chronic kidney disease or end-stage renal failure. When protein is digested in the body it forms a byproduct called urea. In a healthy individual, urea is transported by the bloodstream to the kidneys where it is removed from the body through the urine. The kidneys of a glomerulonephritis patient, however, cannot extract urea out of the blood properly. The excess urea puts a strain on the already compromised kidneys. In addition, a patient with glomerulonephritis may develop what is called uremia, or a toxic accumulation of urea in the blood. Limiting the consumption of protein can help keep urea levels at an acceptable level that does not cause harm to the kidneys. When an individual has glomerulonephritis, their kidneys also cannot properly filter potassium out of the blood. An excess of potassium in the blood can result in the disruption of nerve and muscle function, a heart attack, or an arrhythmia. Avoiding potassium-rich foods like sweet potatoes, spinach, nuts, oranges, bananas, tomatoes, dairy products, and legumes can help keep potassium levels from becoming dangerously high.
Learn more about treating glomerulonephritis effectively now.
Control Blood Sugar
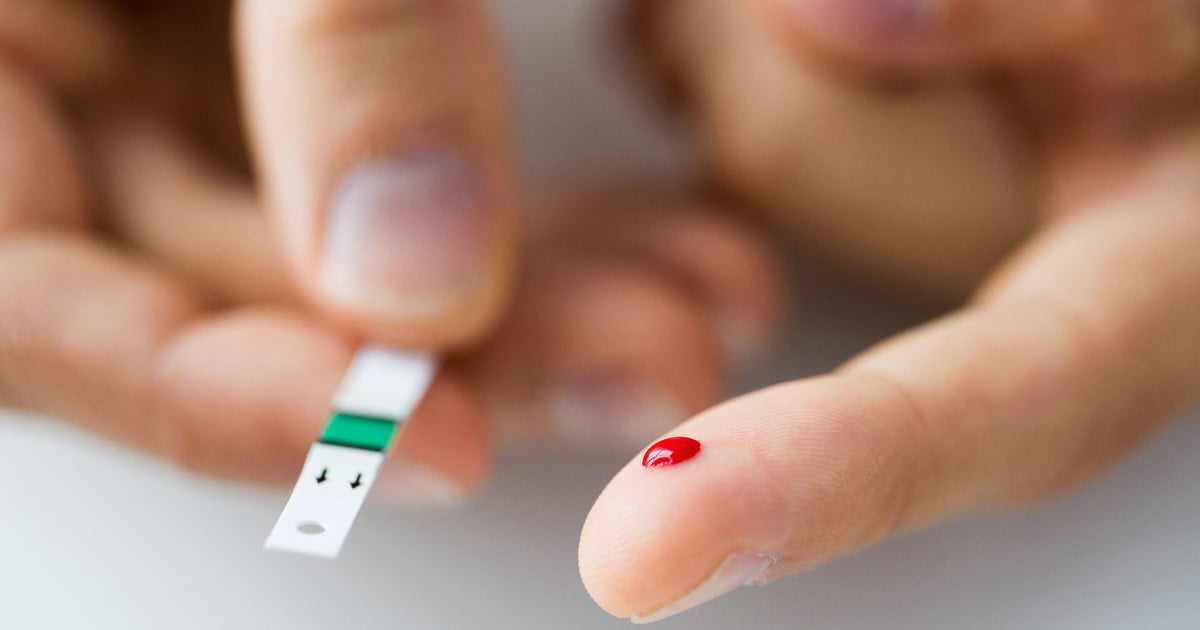
Anyone who has diabetes and glomerulonephritis will be strongly advised to closely monitor and control their blood sugar. This is imperative to prevent further permanent damage to the kidneys. When glucose levels in the blood are too high, blood flows into the kidneys at a higher velocity. This is a problem because it causes an increase in blood pressure, and it also strains the kidneys' filtering process. A combination of these factors causes the collapse of the small capillaries in the glomerulus. When that happens, scarring develops on the glomeruli. Scarring of the glomeruli can cause and exasperate glomerulonephritis and chronic kidney disease. When an individual with diabetes does not control their condition properly, the progression of chronic kidney disease to end-stage renal disease becomes expedited. At the very minimum, high blood pressure that results from poor diabetes management can easily inflict damage on the glomeruli and speed up the development of chronic kidney disease.
