How To Treat Primary Sclerosing Cholangitis
Primary sclerosing cholangitis is a disease where the tubes that transfer bile between the liver, gallbladder, and small intestine or the bile ducts become scarred as a result of repeated inflammation. Progression of this condition is characterized by bile build-up in the liver due to scar tissue obstructing the bile ducts. The bile build-up causes the liver to incur damage over time, and as a result, the liver also becomes scarred. Primary sclerosing cholangitis can lead to cirrhosis and failure of the liver.
The causes of this condition are not clear, but it is often linked to ulcerative colitis and inflammatory bowel disease. Symptoms that gradually appear as primary sclerosing cholangitis advances slowly include itchy skin, jaundice, and fatigue. Additionally, individuals with this condition may develop a bile duct infection that produces chills, abdominal pain, and a fever.
Vitamin Supplements

Part of treating primary sclerosing cholangitis includes the use of vitamin supplements for any deficiencies that may occur. Many essential nutrients and vitamins are water-soluble, while numerous others are fat-soluble. A healthy individual's body is able to use digestive processes involving the liver, gallbladder, and small intestine to break down fat and absorb the vitamins dissolved in it. The body requires bile from the liver to break down fat properly. Primary sclerosing cholangitis patients often have a partial or full blockage in their bile ducts from scar tissue.
The obstructed bile ducts prevent an adequate amount of bile from reaching the small intestine. This inadequacy causes a failure of the body to break down fats and stops the absorption of the vitamins and nutrients within them. The most common deficiencies in individuals with this condition include vitamins K, E, D, and A. Deficiencies of these vitamins each carry their own set of additional complications that may occur on top of primary sclerosing cholangitis if the deficiency goes unaddressed. Oral vitamin supplements are often prescribed for patients, and some severe cases necessitate intravenous vitamin infusions.
Stent Placement
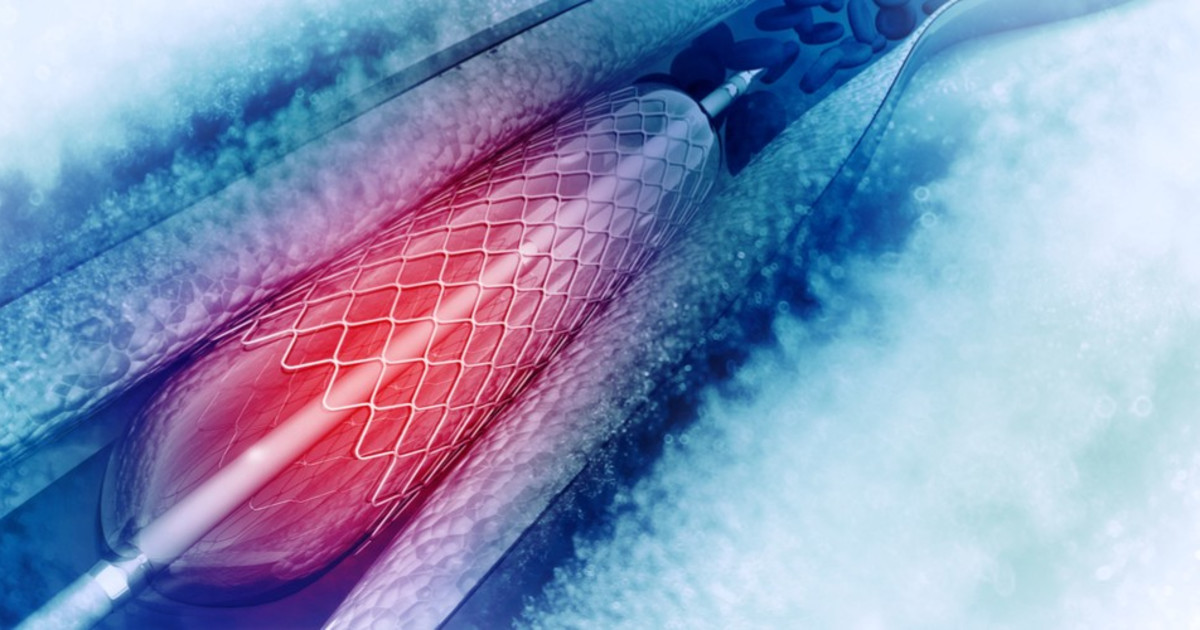
Individuals who have primary sclerosing cholangitis may need a stent placement in their bile ducts to widen them and allow for the easier passage of bile. Chronic inflammation of the bile ducts in patients results in sclerosis or scarring of the duct tissues. Scar tissue is fibrous tissue formed by a tough protein that is harder and stiffer than the normal bile duct tissues. As scar tissue builds up, the ducts become hardened and narrowed to where they only allow minimum bile passage. The surgical installation of a stent enables the surgeon to widen the bile ducts located outside of the liver and keep them open.
During this procedure, a catheter is threaded into the body through a series of small incisions to reach the bile ducts. Once in the correct part of the duct, the surgeon will insert a small balloon through the catheter into the narrowed bile duct. The balloon is then inflated to widen the duct mechanically. Once the duct has been expanded to the desired position, a stent or small plastic mesh tube is inserted. The balloon is then deflated and removed, and the stent stays secured in place. Stent placement is usually the most practical surgical procedure for cases of primary sclerosing cholangitis because traditional scar tissue removal can be highly invasive and result in more complications.
Bile Acid Binding Medication
Bile acid binding medication may be used to help treat the bothersome itchy skin that affects many primary sclerosing cholangitis patients. When bile begins to build up in the blood because something is stopping the body from eliminating it properly, it also begins to accumulate in the skin. There are several ways bile causes itching in the skin, including stimulating the release of histamine by the immune system. In a healthy individual, bile is released through the bile ducts and flows into the small intestine. Once there, bile acids are reabsorbed back into the blood by the small intestine. This normal circulation keeps bile levels in check for individuals who do not have primary sclerosing cholangitis.
Because bile accumulates quickly in patients with this condition, a medication that stops the reabsorption of bile acids in the intestine can be helpful. Bile acid binding medications essentially bind to the bile acids to keep the intestine from reabsorbing them. When bile acids are not absorbed, they exit the body through the stool. This mechanism allows for individuals affected by primary sclerosing cholangitis to eliminate excess bile from their body. When bile levels in the skin decrease back to normal, the skin stops itching.
Liver Transplant
Some individuals with primary sclerosing cholangitis will eventually require a liver transplant. While measures can be taken in those with this condition to slow its progression and prevent complications, no known treatment will actually stop its progression. Eventually, injury and inflammation of the liver will occur because the bile has nowhere to go. With each subsequent episode of liver inflammation and injury, the body heals itself by developing scar tissue in the liver. Excessive liver scarring is known as cirrhosis, and this causes liver failure. Aside from liver failure, another circumstance that may necessitate a liver transplant in an individual with primary sclerosing cholangitis is frequent infections of the biliary system or bacterial cholangitis.
In addition, primary sclerosing cholangitis patients are at a considerably higher risk of developing cancers of the liver, gallbladder, and bile ducts. If cancerous cells are found in any bile duct or liver tissues as a result of primary sclerosing cholangitis, a liver transplant may be warranted. When any symptoms of this condition become excessively debilitating and do not respond to other methods of treatment, a liver transplant may be considered.
Take Antibiotics

Individuals affected by primary sclerosing cholangitis will have to take antibiotics often and sometimes on a long-term basis. When the bile ducts become obstructed, and bacteria makes its way into the biliary, gallbladder, or liver tissues, an infection can develop. Antibiotics are often given to primary sclerosing cholangitis patients when any infections emerge. However, in some cases, it is better to place an individual with this condition on a long-term course of preventative antibiotics than it is to continue treating infections as they occur.
When bacterial infections are treated with numerous antibiotics in short periods, the infection causing bacteria will learn how to evade the action of each frequently used antibiotic. Another circumstance that calls for the use of antibiotics in the course of primary sclerosing cholangitis treatment is when an individual is undergoing any type of invasive procedure. Even minimally invasive procedures can significantly increase a patient's susceptibility to developing an infection. If antibiotics become ineffective at treating infections of the bile ducts, a liver transplant may be needed.
