Risks Associated With Endotracheal Intubation
Endotracheal intubation is an emergency procedure needed when an individual is unable to breathe on their own or is unconscious. Endotracheal intubation stops the individual from experiencing suffocation and keeps their airway open. The trachea (windpipe) is a structure that runs from the throat to the lungs, serving as a path for oxygen. An individual's trachea stretches down to behind their sternum or breastbone and divides into two tubes referred to as the bronchi.
Endotracheal intubation is performed when an individual is undergoing a major surgical procedure to ensure oxygen delivery while being operated on. It is also used in individuals who have to be placed under heavy sedation or in a medically induced coma so they can recover from a serious illness or injury. Most individuals who have endotracheal intubation tolerate it well, but it does carry some risks.
Risks Related To Anesthesia
When an individual has endotracheal intubation performed, they are almost always sedated with anesthesia for the tube insertion or are intubated because they will be under general anesthesia. Anesthesia is required for endotracheal intubation so the patient does not feel the tube being inserted. General anesthesia does not usually produce any problems in healthy individuals, but complications do occur in some cases. Patients who have had previous chronic problems with vital organs like their heart, lungs, or kidneys are at an increased risk of having anesthesia complications.
Individuals who have sleep apnea, drink alcohol frequently, have allergies to certain foods, family or personal history of anesthesia reactions, have allergies to certain drugs, a history of seizures, have diabetes, and smoke frequently are also more likely to experience complications with anesthesia while undergoing endotracheal intubation. Possible complications that can occur from the use of general anesthesia for any type of surgical procedure include lung infections, a stroke, temporary mental confusion, heart attack, and death.
Lung Injury

The physician who performs the patient's endotracheal intubation is responsible for choosing the correctly sized equipment to minimize injury to all of the patient's body structures that are involved. They are also responsible for making sure the tubes do not become kinked while in the patient's airways and the tube makes it to the correct place in the airway. Sometimes the tube can be misplaced in the right mainstem bronchus, which causes the left lung to collapse due to the lack of enough air in the tissues to maintain its structure.
Another lung complication associated with endotracheal intubation is referred to as barotrauma, which occurs when endotracheal intubation is combined with mechanical ventilation. Sometimes the air sacs in the patient's lungs can rupture from a rapid pressure change, and the air from the ventilator can enter the patient's pleural space. This condition is called pneumothorax, which injures the lung further and causes other severe complications.
Aspiration
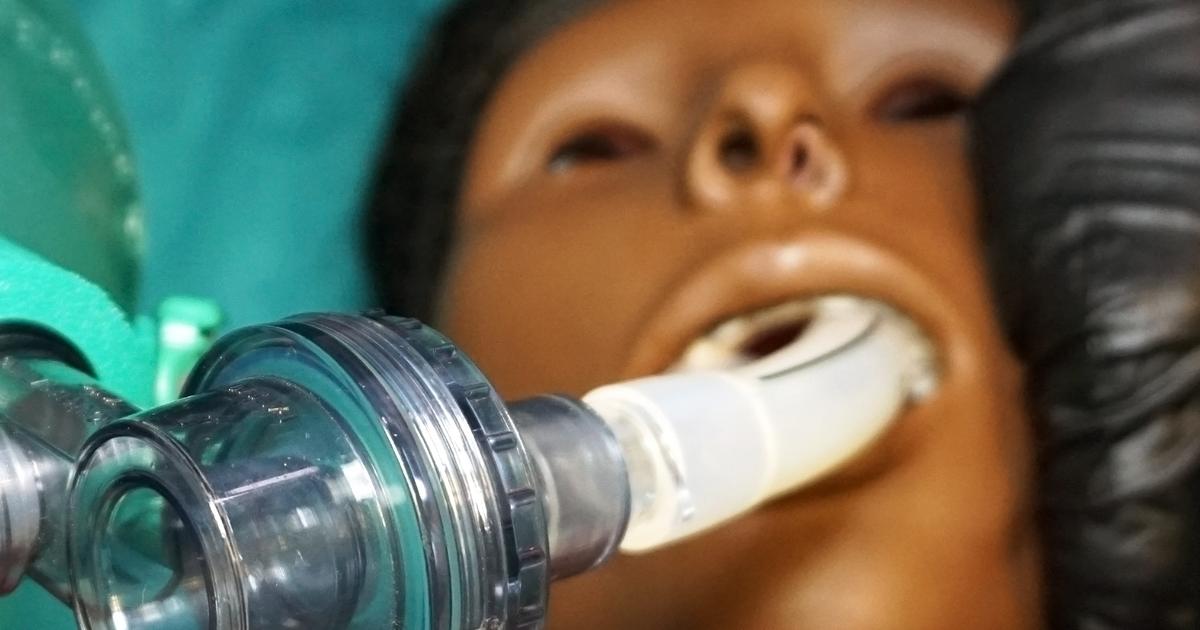
Individuals who have to undergo endotracheal intubation emergently are at risk of experiencing the aspiration of gastric contents. During regurgitation and vomiting, the contents of the stomach travel up through the esophagus and then move into the pharynx. From there, the contents have two paths they can take. The contents can continue up the throat and be expelled from the mouth, or they enter the larynx and trachea. The flow of an individual's gastric contents is dependent on the difference between the vertical height of the larynx and mouth.
Using the technique of a head-down tilt in the supine position with the mouth at a position lower than the larynx can prevent the aspiration of contents into the trachea. When a patient having an endotracheal intubation experiences aspiration of stomach contents into the lungs, it can cause chemical pneumonitis, pneumonia, or death. Death may occur if the particulate part of the aspirate obstructs the airway and leads to arterial hypoxemia. Flora in the aspirate can allow bacteria into the lungs that cause the development of pneumonia, and acidic material can induce an inflammatory response in the lungs.
Throat Or Trachea Injury
Throat or trachea injury can occur when an individual undergoes endotracheal intubation. The most common location for an injury caused by the procedure is the patient's larynx. The cartilage in the trachea that supports the main airway can become damaged from inaccurate movements of the endotracheal tube, putting the patient at risk for airway collapse and obstruction when the tube is removed. The instruments used to compress the tongue and epiglottis to get the endotracheal tube into the correct position may cause lacerations and bruises to the patient's throat or tracheal tissues.
It is possible for large blood vessels nearby the trachea and throat to become damaged or lacerated if there is a preexisting but unknown vulnerability in the blood vessels. The pressure of the cuff placed in the trachea can be excessive and cause damage to the tissues surrounding it, including the nerves. The blood supply to the patient's tracheal mucosa can also become obstructed as a result of the over-inflation of the cuff. The throat and trachea can also experience other injuries due to long-term endotracheal intubation.
Injury To The Teeth
One of the most common complications of endotracheal intubation is injuries to the teeth and other dental structures. The most common dental injuries associated with this procedure include but are not limited to broken bridges, fractures to the enamel, loosened teeth, chipped teeth, subluxated teeth, crown fracture, tooth avulsion, fracture of the tooth root, dislodged implants, broken teeth, and chipped veneers. The patients who are most at risk of experiencing injury to their teeth during endotracheal intubation are those who practice poor dental hygiene, have preexisting dental problems, or have a history of poor oral health.
The most common cause of dental injury during endotracheal intubation is laryngoscopy. The next most common cause of dental injury with endotracheal intubation is during extubation. The most common teeth injured in patients who undergo endotracheal intubation are the upper left and right incisors. Most injuries to the teeth are discovered by the performing anesthesiologist, while fewer are discovered later on by the patient who underwent the procedure.
