9 Ways to Stay Organized If You Take Multiple Medications Daily
Managing multiple daily medications presents a complex challenge that affects millions of people worldwide, particularly those with chronic conditions, elderly individuals, and patients recovering from serious illnesses. The statistics are sobering: medication errors contribute to approximately 125,000 deaths annually in the United States alone, with poor organization and adherence being primary contributing factors. When you're juggling multiple prescriptions, over-the-counter supplements, and various dosing schedules, the potential for confusion, missed doses, or dangerous interactions increases exponentially. This comprehensive guide explores nine evidence-based strategies that can transform your medication routine from a source of stress and confusion into a well-organized, manageable system. These methods aren't just theoretical concepts—they're practical, proven approaches that healthcare professionals recommend and patients successfully implement daily. Whether you're managing medications for yourself or a loved one, these organizational strategies will help ensure safety, improve adherence, and provide peace of mind in your healthcare journey.
1. Create a Comprehensive Medication List and Keep It Current

Establishing and maintaining a detailed, up-to-date medication list serves as the foundation of effective pharmaceutical organization and safety. This master document should include not only prescription medications but also over-the-counter drugs, vitamins, supplements, herbal remedies, and even occasional medications like pain relievers or allergy treatments. For each medication, record the generic and brand names, dosage strength, prescribing physician, pharmacy information, purpose of the medication, dosing instructions, and any special considerations such as "take with food" or "avoid sunlight." Research published in the Journal of Patient Safety demonstrates that patients who maintain comprehensive medication lists experience 40% fewer adverse drug events and medication errors. Additionally, include important dates such as when each medication was started, when prescriptions expire, and scheduled follow-up appointments with healthcare providers. Store copies of this list in multiple accessible locations: your wallet, smartphone, refrigerator, and with trusted family members. During medical emergencies, this information becomes invaluable for healthcare providers who need to make quick decisions about your care while avoiding potentially dangerous drug interactions.
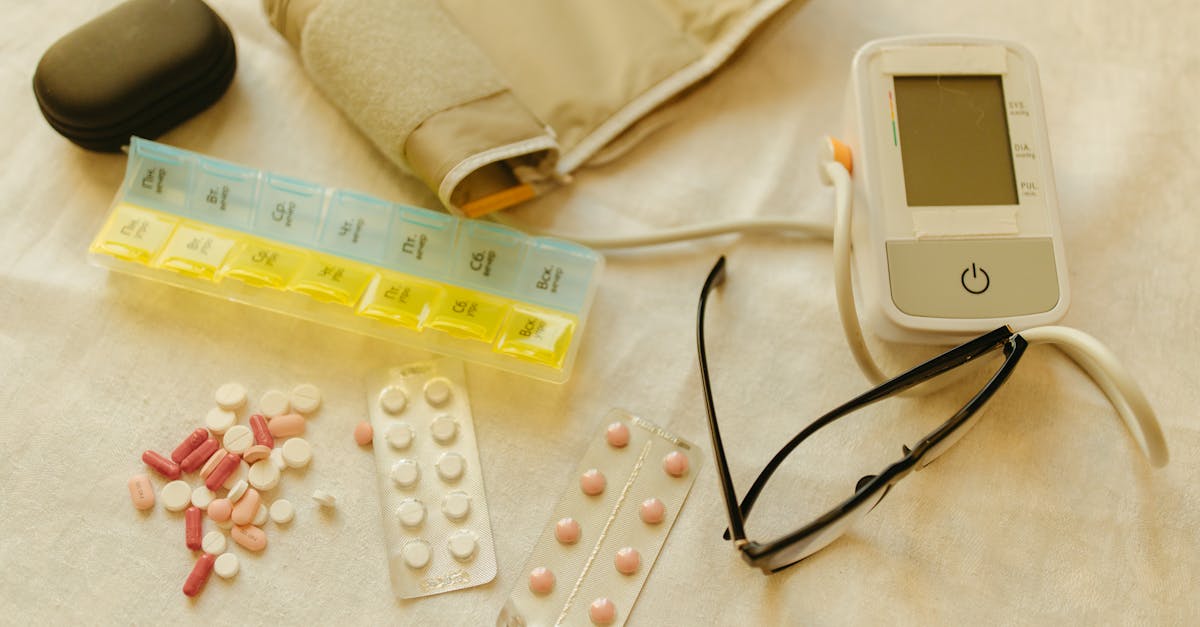
2. Invest in a Quality Pill Organizer System

A well-designed pill organizer system can dramatically reduce medication errors and simplify daily routines, particularly for individuals managing complex medication regimens. Modern pill organizers have evolved far beyond simple weekly containers, now offering sophisticated options including multiple daily compartments, monthly planning capabilities, and even electronic dispensers with alarms and locking mechanisms. Research from the American Journal of Managed Care shows that patients using organized pill systems demonstrate 85% better medication adherence compared to those managing medications from original bottles. When selecting an organizer, consider factors such as the number of daily doses, pill sizes, travel requirements, and any dexterity limitations that might affect your ability to open compartments. Large-compartment organizers work best for multiple medications or larger pills, while compact travel versions ensure continuity during trips. Some advanced systems feature clear, labeled compartments for morning, noon, evening, and bedtime doses, while others include separate organizers for each day of the week. The key is choosing a system that matches your specific needs and lifestyle, ensuring that the organizational tool enhances rather than complicates your medication routine.
3. Establish Consistent Daily Routines and Timing

Creating structured, consistent routines around medication timing transforms adherence from a challenging memory task into an automatic habit that integrates seamlessly with daily life. Behavioral psychology research demonstrates that linking medication times to established daily activities—such as brushing teeth, eating meals, or watching a favorite television program—significantly improves long-term adherence rates. The concept of "habit stacking," where new behaviors are attached to existing strong habits, proves particularly effective for medication management. For morning medications, consider taking them immediately after waking up or with your first cup of coffee. Evening medications might be paired with dinner preparation or bedtime routines. Consistency in timing also optimizes medication effectiveness, as many drugs are designed to maintain steady levels in your bloodstream. For medications requiring specific timing intervals, such as antibiotics every eight hours, use smartphone alarms or medication reminder apps to maintain precise schedules. Document your chosen routine and stick to it even on weekends, holidays, or during travel. This consistency helps prevent the common problem of missed doses that occur when normal routines are disrupted, ensuring therapeutic levels remain stable and treatment goals are achieved.
4. Utilize Technology and Smartphone Applications

Modern technology offers powerful tools for medication management that can significantly enhance organization and safety for individuals taking multiple daily medications. Smartphone applications like Medisafe, MyMedSchedule, and PillPack provide comprehensive platforms for tracking medications, setting customized reminders, monitoring adherence patterns, and even connecting with healthcare providers or family members. These applications often include features such as pill identification tools, drug interaction checkers, and medication history tracking that can prove invaluable during medical appointments or emergencies. Research published in the Journal of Medical Internet Research indicates that patients using medication management apps show 68% better adherence rates and report feeling more confident about their medication routines. Many apps also offer family connectivity features, allowing caregivers or family members to receive notifications if medications are missed, which is particularly valuable for elderly patients or those with cognitive challenges. Advanced features include photo documentation of medications, integration with pharmacy refill systems, and the ability to generate comprehensive reports for healthcare providers. Some applications even sync with smart pill dispensers or wearable devices to provide additional layers of monitoring and support, creating a comprehensive digital ecosystem for medication management.
5. Coordinate with Healthcare Providers and Pharmacists

Effective communication and coordination with your healthcare team creates a crucial safety net that helps prevent medication errors, dangerous interactions, and organizational confusion. Establishing a primary pharmacy relationship allows pharmacists to maintain comprehensive medication profiles, monitor for potential drug interactions, and provide valuable counseling about proper administration techniques and potential side effects. Research from the American Pharmacists Association shows that patients who consistently use the same pharmacy and maintain regular communication with their pharmacist experience 45% fewer medication-related problems. Schedule regular medication reviews with your primary care physician, especially when new medications are added or existing ones are modified. During these appointments, bring your complete medication list, pill organizers, and any questions or concerns about your regimen. Many healthcare systems now offer medication therapy management (MTM) services, where specialized pharmacists conduct comprehensive reviews of all medications to optimize therapy and identify potential improvements. Don't hesitate to ask questions about the purpose of each medication, potential side effects, proper timing, and what to do if doses are missed. Establish clear communication channels for reporting side effects or concerns, and ensure all healthcare providers involved in your care have access to your complete medication list to prevent prescribing conflicts.
6. Implement a Reliable Refill and Inventory Management System
Developing a systematic approach to medication refills and inventory management prevents the stress and health risks associated with running out of essential medications. Create a tracking system that monitors remaining pill counts and refill dates, allowing for timely prescription renewals before supplies are exhausted. Many successful patients use a simple calendar system, marking refill dates two weeks in advance to account for potential pharmacy delays, insurance issues, or shipping problems for mail-order prescriptions. Research from the National Community Pharmacists Association indicates that patients who maintain proactive refill systems experience 60% fewer treatment interruptions due to medication shortages. Consider enrolling in automatic refill programs offered by many pharmacies, which can eliminate the need to remember refill dates while ensuring continuous medication availability. For patients using mail-order pharmacies, factor in shipping times and potential delays, especially during holidays or severe weather. Maintain a small emergency supply of critical medications when possible, following your healthcare provider's guidance about appropriate quantities. Keep track of insurance formulary changes that might affect medication costs or availability, and work with your healthcare provider to identify suitable alternatives if your preferred medications become unavailable or prohibitively expensive.
7. Organize Physical Storage Spaces Effectively

Creating well-organized, safe storage spaces for medications is essential for maintaining drug effectiveness, preventing accidental ingestion, and ensuring easy access when needed. Medications should be stored according to their specific requirements—some need refrigeration, others must be kept in dark, dry places, and certain medications require room temperature storage away from humidity and heat. The bathroom medicine cabinet, despite its traditional use, is often the worst place for medication storage due to heat and humidity from showers and baths. Instead, consider a dedicated medication storage area in a bedroom, kitchen pantry, or other climate-controlled space. Research from the Food and Drug Administration emphasizes that proper storage can extend medication effectiveness and prevent degradation that might reduce therapeutic benefits or create harmful byproducts. Use clear, labeled containers or drawer organizers to separate different types of medications, making them easy to locate quickly. For households with children or visitors, invest in lockable storage solutions to prevent accidental ingestion. Keep medications in their original containers when not using pill organizers, as these containers provide important information about expiration dates, lot numbers, and storage instructions. Regularly clean storage areas and check for expired medications, disposing of them properly through pharmacy take-back programs or following FDA guidelines for safe disposal.
8. Develop Emergency Preparedness and Backup Plans

Creating comprehensive emergency preparedness plans ensures medication continuity during unexpected situations such as natural disasters, travel delays, power outages, or sudden illness that might disrupt normal routines. Emergency preparedness begins with maintaining current medication lists in multiple accessible formats and locations, including digital copies stored in cloud services and physical copies in emergency kits, vehicles, and with trusted family members. The Federal Emergency Management Agency recommends keeping at least a seven-day supply of essential medications in emergency kits, along with copies of prescriptions and pharmacy contact information. For patients dependent on refrigerated medications, develop plans for maintaining cold storage during power outages, including battery-powered cooling devices or arrangements with nearby facilities that have backup power. Establish relationships with multiple pharmacies in different geographic areas, particularly if you travel frequently or live in areas prone to natural disasters. Research shows that patients with comprehensive emergency medication plans experience 70% fewer health complications during crisis situations. Include contact information for all healthcare providers, insurance companies, and specialty pharmacies in your emergency documentation. For patients using medical devices or equipment, ensure backup power sources and alternative suppliers are identified. Consider the specific challenges your medical conditions might present during emergencies and work with healthcare providers to develop detailed contingency plans that address these unique needs.
9. Monitor and Track Medication Effectiveness

Systematic monitoring and documentation of medication effectiveness provides valuable information for healthcare providers while helping identify potential problems or needed adjustments in your treatment regimen. Maintain a medication diary or use smartphone apps to track not only when medications are taken but also how you feel, any side effects experienced, and changes in symptoms or condition markers. This information becomes invaluable during medical appointments, providing objective data that can guide treatment decisions and optimize therapeutic outcomes. Research published in the Journal of Clinical Medicine demonstrates that patients who actively monitor and document medication effects experience 55% better treatment outcomes and faster identification of problems requiring medical attention. Include information about factors that might influence medication effectiveness, such as food intake, exercise, stress levels, sleep patterns, and other medications or supplements. For conditions with measurable parameters—such as blood pressure, blood sugar, or pain levels—record these measurements regularly and note their relationship to medication timing and dosing. Pay attention to patterns that might indicate the need for dosage adjustments, timing changes, or alternative medications. Document any unusual symptoms or side effects, even if they seem minor, as these might indicate developing problems or drug interactions that require medical evaluation. This proactive approach to monitoring helps ensure that your medication regimen continues to meet your health needs effectively while minimizing risks and side effects.
10. Build Support Networks and Communication Systems

Establishing strong support networks and communication systems creates multiple layers of safety and assistance that can be crucial for successful long-term medication management. Family members, friends, caregivers, and healthcare providers all play important roles in supporting medication adherence and identifying potential problems before they become serious. Research from the American Geriatrics Society shows that patients with strong medication support networks demonstrate 80% better adherence rates and experience fewer medication-related hospitalizations. Educate trusted family members or friends about your medication regimen, including the purpose of each medication, potential side effects to watch for, and emergency procedures if problems arise. Consider using shared smartphone apps or communication platforms that allow supporters to receive notifications about missed doses or concerning symptoms. For elderly patients or those with cognitive challenges, daily check-in calls or visits can provide both social support and medication reminders. Establish clear protocols for what supporters should do if they notice concerning symptoms, missed medications, or other problems. Include contact information for all healthcare providers, pharmacies, and emergency services in shared communication systems. Many communities offer medication management support groups where individuals facing similar challenges can share strategies, provide mutual encouragement, and learn from each other's experiences. Professional services such as visiting nurses, medication therapy management programs, or specialized pharmacy services can provide additional layers of professional support when needed, ensuring that complex medication regimens are managed safely and effectively.
