Common Side Effects Of Analgesics
Analgesics are specialized medications designed to alleviate pain, with some available over-the-counter and others requiring a prescription. In certain formulations, analgesics combine two drugs within the analgesic class to enhance pain relief. The body possesses specific receptors on cells in the spinal cord, brain, and gastrointestinal tract, playing a crucial role in transmitting pain signals. Analgesics operate by binding to these receptors, impeding the transmission of pain signals to the brain. They are particularly beneficial for individuals experiencing moderate to severe chronic or acute pain, especially for those who cannot use nonsteroidal anti-inflammatory drugs to avoid gastrointestinal bleeding.
It's important to recognize the specific conditions that warrant analgesic use and the considerations surrounding alternative pain management strategies. Understanding the mechanisms of action and limitations of analgesics contributes to informed decision-making in pain management.
Upset Stomach

Individuals taking acetaminophen or opioid-based analgesics may encounter an upset stomach and nausea as potential side effects. The activation of the chemoreceptor trigger zone and alterations in gastric motility contribute to these symptoms. Dopamine receptors in the chemoreceptor zone play a crucial role in nausea induction, while decreased gastric motility can lead to food stagnation in the digestive system, causing stomach upset. Some patients may also experience heightened sensitivity in their vestibular system, impacting balance and further contributing to nausea. Notably, the combination of acetaminophen with other medications can increase the likelihood of nausea and vomiting.
Understanding the gastrointestinal effects of analgesics is vital for both healthcare providers and individuals seeking pain relief. Managing these side effects requires a comprehensive approach that considers individual tolerance and potential adjustments to the analgesic regimen.
Dry Mouth

Saliva in the oral cavity serves crucial functions, including protecting teeth and gums from decay and disease. Opioid-based analgesics, however, exert a depressive effect on the nervous system, specifically the autonomic nervous system responsible for gland activity regulation. Reduced autonomic system activity leads to decreased saliva production, resulting in dry mouth (xerostomia). While this side effect may be less pronounced in well-hydrated individuals, maintaining proper fluid intake becomes essential. Understanding the impact of analgesics on saliva production helps individuals anticipate and manage the associated dry mouth symptoms.
Addressing the issue of dry mouth requires a holistic approach, considering hydration levels, oral hygiene practices, and potential adjustments to the analgesic regimen. Collaborative efforts between healthcare providers and patients enhance overall oral health during analgesic use.
Constipation

Constipation is a prevalent side effect in individuals using acetaminophen and opioid-based analgesics, primarily due to the concentrated opioid receptors in the digestive tract. Activation of these receptors leads to impaired gastric emptying, prolonged food transit time, decreased mucous secretions, and increased fluid reabsorption, resulting in dry and hard stool. Long-term analgesic use often necessitates additional medications to manage constipation effectively. Understanding the complex mechanisms contributing to constipation helps healthcare providers tailor interventions for individual patients.
Educating patients on the potential gastrointestinal effects of analgesics and implementing proactive measures, such as dietary modifications and prescribed medications, can enhance overall treatment outcomes. Monitoring and addressing constipation are integral aspects of comprehensive pain management.
Fatigue

Fatigue, characterized by reduced energy levels and decreased efficiency, is a common side effect in individuals taking acetaminophen and analgesics containing opioids. While opioids suppress pain signals, they concurrently exert a suppressive effect on the central, peripheral, and autonomic nervous systems. This suppression impacts subconscious functions regulated by the autonomic nervous system, influencing an individual's alertness and energy levels. Fatigue may persist with continued medication use or gradually subside as the body adapts to the effects on the nervous system.
Recognizing the relationship between analgesic use and fatigue is crucial for healthcare providers when managing pain in their patients. Open communication and monitoring help tailor treatment plans to minimize fatigue-related disruptions to daily functioning.
Rash Or Itching
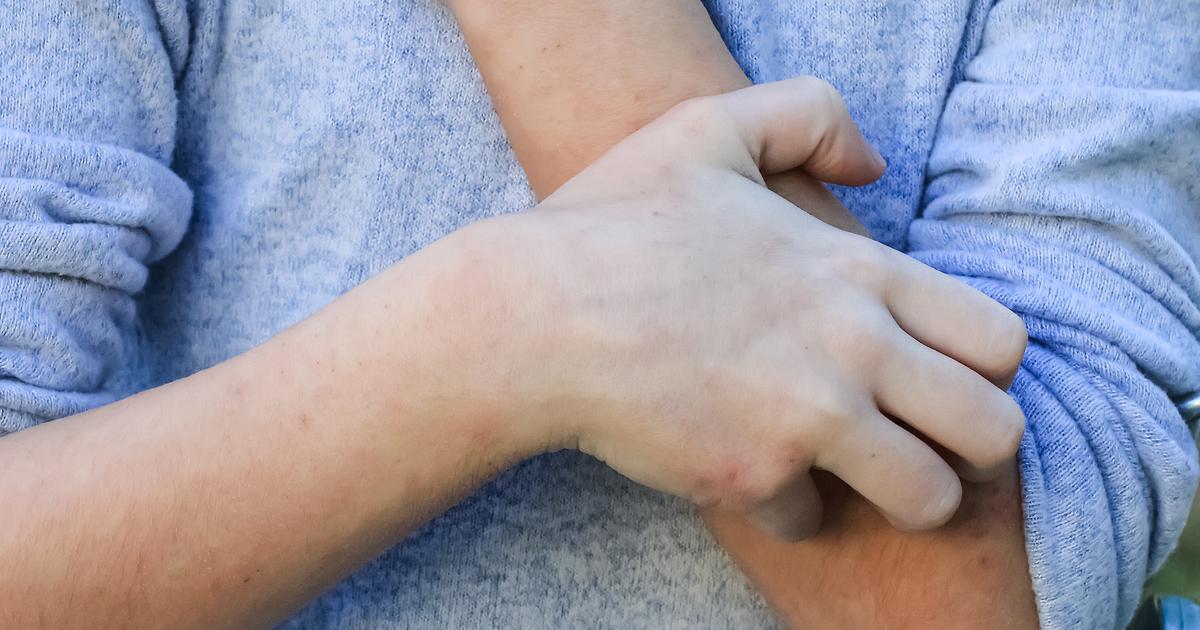
The development of a rash or itching is a potential side effect for individuals using acetaminophen and opioid-based analgesics. While allergic reactions are rare with opioids, pseudoallergic or hypersensitivity reactions are more common. These reactions may occur on the first use of the drug, with itching sensations triggered by opioid receptors in the brain and spinal cord. Understanding the distinction between true allergies and hypersensitivity reactions is essential for accurate diagnosis and appropriate management.
Patient education on potential skin-related side effects, vigilant monitoring for early signs of reactions, and collaboration with healthcare providers enhance the safety and efficacy of analgesic use. Adjustments to the analgesic regimen may be considered based on the individual's response and tolerance.
