Guide To The Best Multiple Sclerosis Medications
Multiple sclerosis is a condition in which the body's immune system attacks myelin. This is the protective covering for nerve fibers. Symptoms include numbness on one side of the body, tremors, unsteady gait, vision problems, slurred speech, and dizziness. Symptoms vary depending on the extent of nerve damage. Some individuals with the condition eventually lose the ability to walk. MRI scans and lumbar punctures are used to diagnose the condition.
Although there is no cure, there are multiple sclerosis treatments out there that help patients manage symptoms, including some MS treatment breakthroughs. Patients may receive plasmapheresis for multiple sclerosis or even physical therapy for multiple sclerosis. MS support groups are also vital components to the various MS treatment options out there. The most common, though, are medications for multiple sclerosis. Patients should understand their various options first.
Methylprednisolone
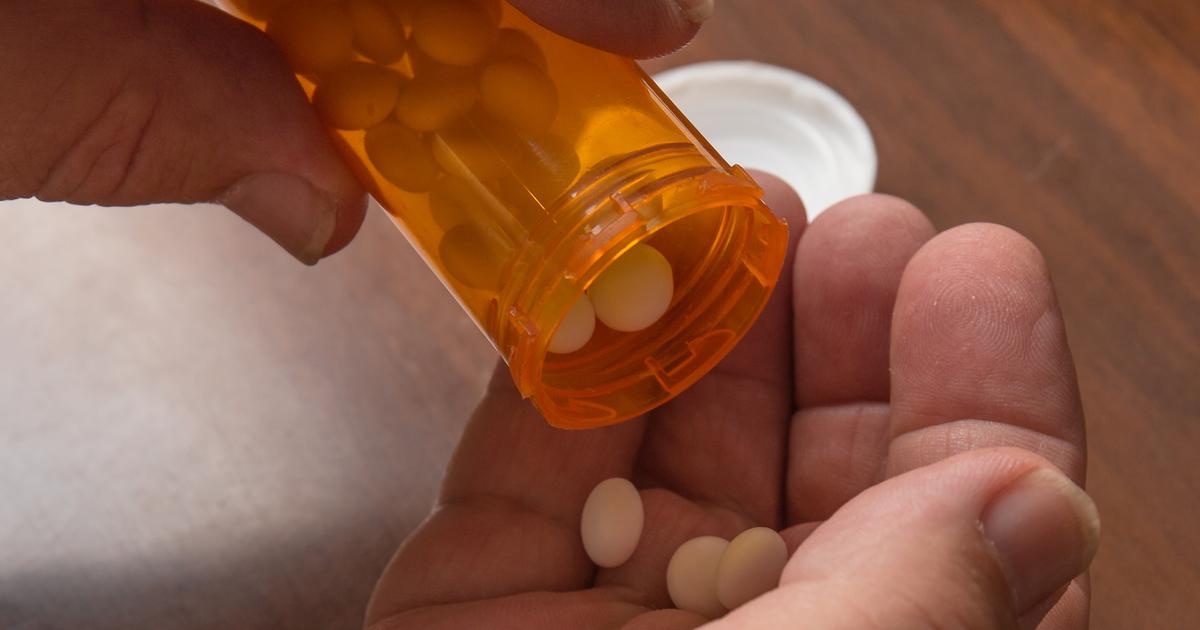
Methylprednisolone belongs to a class of medicines called glucocorticoids. Before using this drug, patients should tell their doctor if they have high blood pressure, osteoporosis, depression, thyroid issues, or cirrhosis. This helps doctors determine if this medication is safe and how to proceed with dosages. Individuals with fungal infections should not take methylprednisolone. As a steroid, this medicine makes patients more vulnerable to infections. Thus, it is important to avoid contact with ill individuals during treatment.
Patients may experience dizziness, fluid retention, bloating, stomach pain, muscle weakness, and changes in menstruation while taking this medication. In rare cases, this medicine can cause seizures, low potassium, rapid weight gain, and shortness of breath. If these serious effects develop, patients need to let their doctor know right away.
Glatiramer Acetate
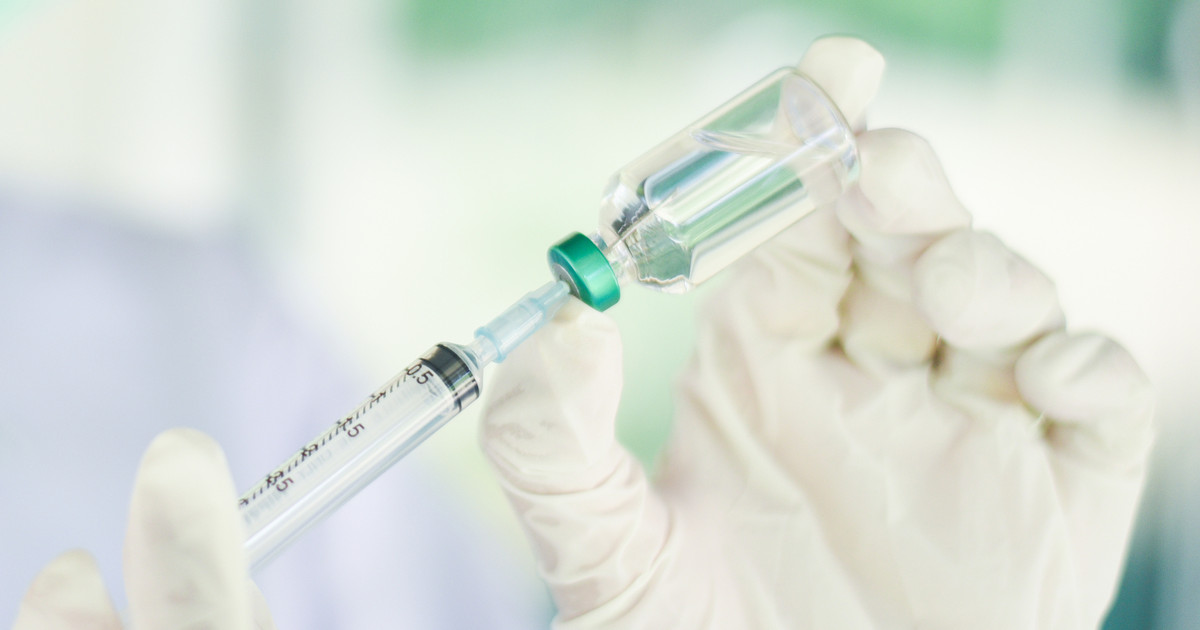
Glatiramer acetate helps reduce the number of multiple sclerosis relapses a patient experiences. However, it does not slow the progression of the condition. It is given as an injection, and patients can learn how to self-inject the medication at home. The upper arm, stomach, thigh, and outer hip can be used as injection sites. Patients should only inject this medication when it is at room temperature. It should never be heated. If the solution looks cloudy, it is unsafe to use.
During treatment with glatiramer acetate, patients have reported back pain, tiredness, vomiting, weakness, and irritation at the injection site. Less commonly, some individuals may experience anxiety, shortness of breath, swollen lymph nodes, chest pain, or a rapid heart rate. If these side effects are present, the patient should call their doctor immediately. Ideally, glatiramer acetate should be stored in a refrigerator. It cannot be kept for more than thirty days at room temperature.
Diroximel Fumarate

Diroximel fumarate is appropriate for the treatment of relapsing multiple sclerosis. It can also help with clinically isolated syndrome, relapsing-remitting disease, and secondary progressive disease. Blood tests are necessary before treatment with this medicine. Doctors will need to know if the patient has infections, kidney issues, liver issues, or a low white blood cell count. When taking this drug, patients must swallow the capsule whole. They should never crush or open it. Some individuals may want to take this medication with food. In this case, it is best to take it with a meal that has no more than seven hundred calories. In addition, the meal should not contain more than thirty grams of fat.
Indigestion, diarrhea, skin rashes, nausea, vomiting, flushing, and stomach pain are common side effects of diroximel fumarate. Patients should avoid meals that are high in calories or fat to reduce these side effects. In rare cases, this medicine can cause a dangerous infection in the brain. Patients should contact their doctor right away if they develop problems with thinking, movement, speech, or vision. These problems could worsen very rapidly.
Ocrelizumab
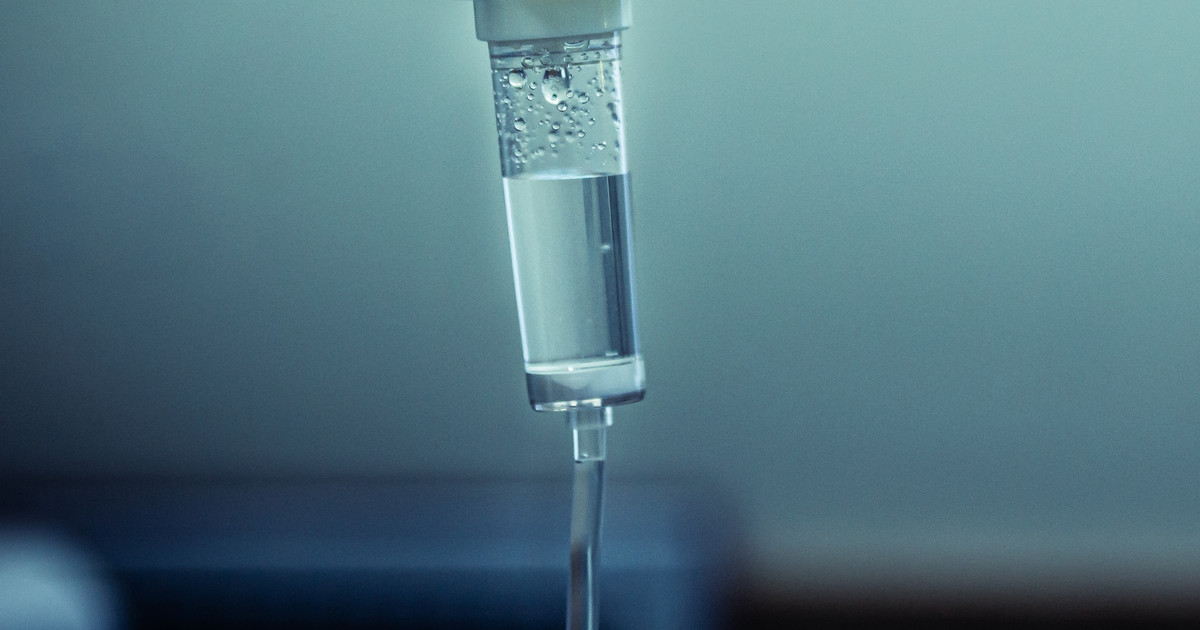
Ocrelizumab is given as an intravenous infusion. It helps treat primary multiple sclerosis and relapsing forms of the condition. This medication is a monoclonal antibody, and it targets specific lymphocytes that cause nerve damage. The first dose is given as two infusions that are fourteen days apart. After the initial dose, patients usually have one infusion every six months. Each infusion takes two and a half hours. Patients who have an active hepatitis B infection should not use ocrelizumab.
Infusion reactions are among the most commonly reported side effects of this medicine. After the infusion, patients are monitored for at least one hour in case they experience a reaction. Symptoms of infusion reactions may include dizziness, fast heart rate, fever, shortness of breath, hives, breathing difficulties, and coughing. Patients must alert their doctor if they notice any of these symptoms. This medication increases the risk of developing upper and lower respiratory tract infections, herpes, and skin infections. Finally, this drug weakens the immune system. It may cause a reactivation of hepatitis B in patients who have had the virus.
Natalizumab

Natalizumab treats relapsing forms of multiple sclerosis in adults. It is given as an infusion. Currently, it is only available to the participants of special programs. Before using this medicine, patients should let their doctor know if they have ever had leukemia, liver issues, herpes, shingles, lymphoma, or an organ transplant. They should also tell their doctor if they have an active infection.
Most patients have an infusion of natalizumab once a month. Joint pain, diarrhea, headaches, nausea, stomach pain, and arm pain are some of the most frequently reported side effects of this medication. During treatment, patients should alert their doctor immediately if they notice painful urination, easy bruising, jaundice, nausea, fever, or chills.
