Guide To The Most Common Antidepressants
Antidepressants are prescription medications primarily used to treat clinical depression. Antidepressants are generally taken orally at least once per day. Doctors can adjust the dosage depending on the patient's needs. Patients should have their progress monitored periodically by their doctor and report any side effects or new symptoms they experience. Patients who wish to discontinue this type of medication will need to speak to their doctor about how to do so properly.
As mentioned, most patients take antidepressant pills. Doctors often recommend this type of antidepressant treatment for major depression. However, patients may also need light therapy for depression or psychotherapy for depression. Of course, antidepressants may also act as an anxiety treatment or bipolar disorder treatment when depression also appears. The best way to use antidepressants, however, requires an understanding of the major types. Learn about them now.
Selective Serotonin Reuptake Inhibitors
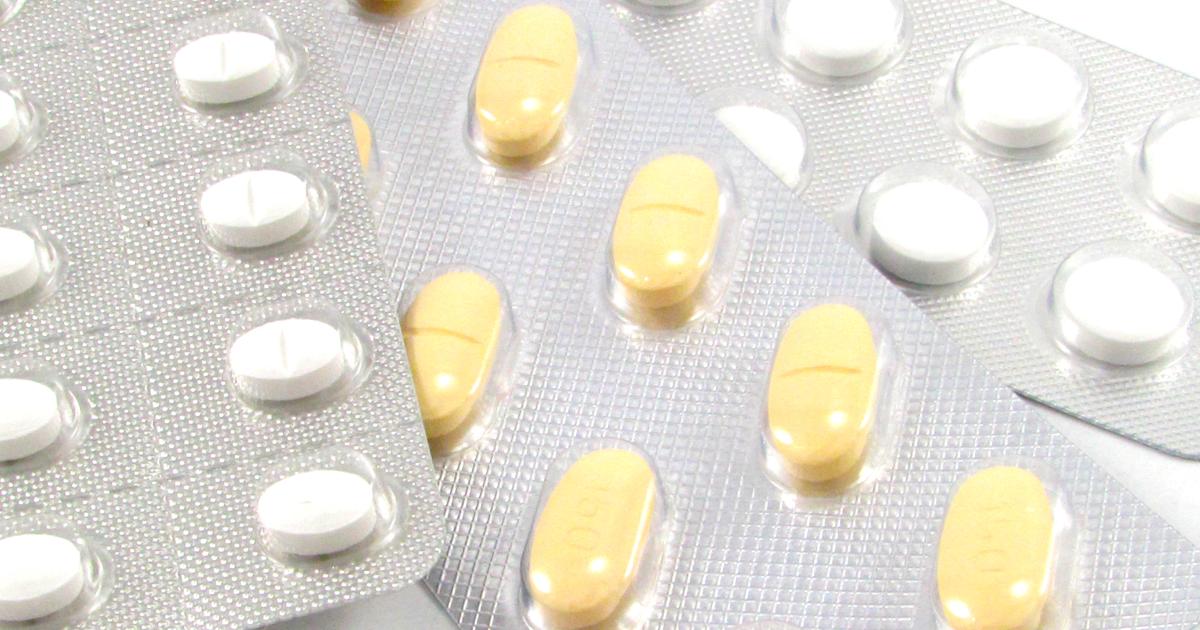
Selective serotonin reuptake inhibitors (SSRIs) are currently the most widely prescribed antidepressant. They work by increasing the level of serotonin in the brain, and they are beneficial for patients with moderate to severe depression. Examples include fluoxetine, and sertraline. In addition to treating depression, this type of medication may be prescribed to treat anxiety. SSRIs are a newer form of antidepressant, and they generally have fewer side effects than older ones. However, patients taking them should still be aware of the potential side effects. These side effects include headache, dry mouth, nausea, vomiting, insomnia, and dizziness. Some patients could notice restlessness, agitation, or weight changes. The side effects are most likely to occur within the first month of treatment.
Patients who find the side effects of a particular SSRI too troublesome may be able to successfully tolerate another one. Since this kind of medication could increase the risk of bleeding, patients should inform their doctor about any anticoagulants they take before SSRIs are prescribed. It may be necessary to avoid over-the-counter nonsteroidal anti-inflammatories during treatment.
Uncover more information on the most common medications for depression now.
Tricyclic Antidepressants

Tricyclic antidepressants were first discovered in the 1950s. They increase the levels of serotonin and norepinephrine in the brain, and are used to treat depression, bipolar disorder, obsessive-compulsive disorder, chronic pain, and insomnia. Amoxapine and amitriptyline are currently two of the most common tricyclic antidepressants. Before taking this type of antidepressant, patients should let their doctor know if they have recently had a heart attack or if they have glaucoma, liver disease, diabetes, cardiovascular issues, or a history of seizures. This medication may not be safe for patients with these conditions. Precautions may be necessary if this medication for depression is used in patients under twenty-five years old or over sixty-five years old.
Potential side effects associated with these medications include a racing heartbeat, sweating, urinary retention, blurry vision, and dizziness. Some patients could also experience weight gain, constipation, tremors, restlessness, and low blood pressure upon standing. In elderly patients, tricyclic antidepressants could cause confusion. This kind of antidepressant should not be used with MAOIs. Alcohol consumption should be avoided during treatment.
Read more about the most common types of antidepressants now.
Serotonin And Norepinephrine Reuptake Inhibitors
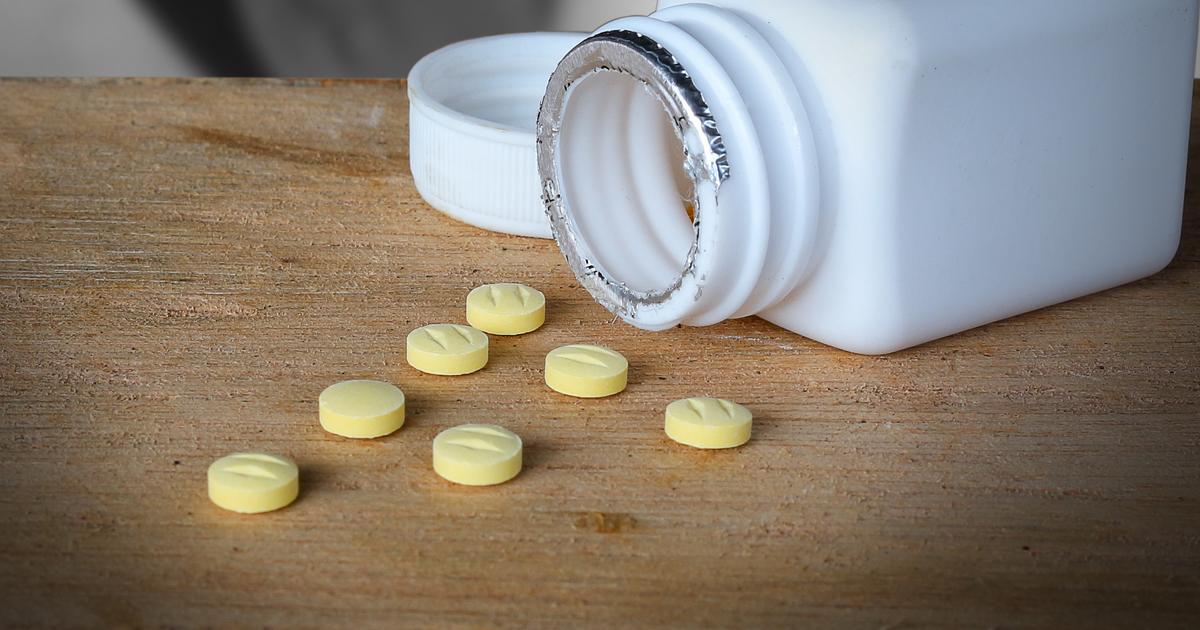
Serotonin and norepinephrine reuptake inhibitors (SNRIs) are quite self-explanatory. This antidepressant increases serotonin and norepinephrine. In addition to depression treatment, these drugs may be prescribed to treat chronic pain, especially pain that stems from the body's nerves. They are used to treat diabetic neuropathy, fibromyalgia, low back pain, and pain from osteoarthritis as well. This type of medication is also beneficial in the treatment of social phobia, panic disorder, anxiety, bipolar disorder, and major depressive disorder. Two examples of SNRIs are venlafaxine and duloxetine. Patients taking this type of antidepressant could experience side effects such as constipation, dry mouth, nausea, fatigue, and loss of appetite.
These drugs can also increase blood glucose levels in patients with diabetes. They may cause low blood pressure upon standing as well. In rare cases, patients who use SNRIs have reported seizures. They may also reduce the levels of sodium in the blood, especially in the elderly and patients who take diuretics. Some could worsen existing liver issues, or increase blood pressure in certain patients. Patients who use these medicines may need to have their blood pressure, blood glucose, and liver function monitored regularly.
Discover more types of antidepressants now.
Monoamine Oxidase Inhibitors

Monoamine oxidase inhibitors (MAOIs) were introduced in the 1950s. These medications are typically prescribed today after other antidepressants have been tried first. Examples of MAOIs include tranylcypromine, isocarboxazid, and selegiline. The effects of this type of antidepressant often take up to three weeks to be felt by the patient. They are generally continued for at least six months after the patient's depression resolves. MAOIs are especially beneficial for patients who have atypical depression. Those with this condition have features that are inconsistent with other recognized types of depression. They may include a heavy feeling in the arms and legs, excessive drowsiness, and an improvement in symptoms if a positive event occurs in the patient's life.
While taking MAOIs, patients should not consume any foods or drinks containing tyramine. Doing so could cause a dangerous and sudden increase in blood pressure. Patients should also avoid over-the-counter cough and cold remedies that contain dextromethorphan. Potential side effects of this type of depression medication include weight gain, hypertension, dizziness, lightheadedness, dry mouth, diarrhea, and difficulty urinating.
Keep reading to uncover more common types of antidepressants now.
Atypical Antidepressants

Atypical antidepressants include any antidepressants that work differently than the previously mentioned ones. Many types of atypical antidepressants work by increasing levels of dopamine and norepinephrine in the brain. They are often considered in cases of treatment-resistant depression that has not responded to other antidepressants. In addition, doctors may choose to prescribe atypical antidepressants for patients trying to quit smoking, as the drugs have been shown to reduce nicotine cravings. Bupropion is one of the most common atypical antidepressants in use today.
Patients who take these medications should be aware of potential side effects such as dry mouth, dizziness, constipation, diarrhea, and weight gain. Esketamine, a new nasal spray intended for use in patients with treatment-resistant depression, must be administered by a psychiatrist or a primary care doctor. Bupropion should not be used by patients who have a history of seizures or eating disorders. Patients should check in regularly with their healthcare team during treatment with atypical antidepressants. If troublesome side effects occur, it may be possible to switch to another medication in the same drug category.
Uncover another type of antidepressant now.
Noradrenaline And Specific Serotonergic Antidepressants

Some patients may take noradrenaline and specific serotonergic antidepressants (NASSAs). This type is common for individuals who cannot take SSRIs. They are also used to treat some personality disorders and anxiety in addition to depression. Ultimately, the effect of this medication is to enhance the transmission of adrenaline and serotonin in the brain, specifically when it comes to mood regulation.
Information surrounding NASSAs suggests they carry fewer side effects than SSRIs.However, side effects can happen, and typically include drowsiness, dry mouth, weight gain, dizziness, constipation, and blurry vision. Two common NASSAs are mirtazapine and mianserin. The former is quite sedating, and is particularly helpful for patients with insomnia or high anxiety as part of their condition.
Learn about more types of medication for depression now.
Tetracyclics
Tetracyclic antidepressants, invented in the 1970s, are quite similar to tricyclic antidepressants. However, they contain four rings of atoms instead of three. Two examples of tetracyclics are setiptiline and mirtazapine, the latter also being a NASSA. Most medications in this class inhibit the reuptake of noradrenaline and serotonin in the brain, thus elevating an individual's mood. These are incredibly effective antidepressants. However, as they are older, they also come with a longer list of potential side effects. They include weight gain, blurry vision, dry mouth, drowsiness, higher cholesterol, constipation, orthostatic hypotension, manic mood, seizures, and serotonin syndrome. In addition, stopping this antidepressant improperly can lead to serious withdrawal symptoms.
The result is that this type of antidepressant is often not prescribed as a first treatment for depression. Doctors often save them for severe cases, particularly when the patient has treatment-resistant depression. Some of them may be used off-label for obsessive-compulsive disorder and post-traumatic stress disorder. Of course, this medication interacts with other antidepressants, so patients often cannot take them together. It may also interact with many other medicines, including migraine medications, thyroid medications, blood thinners, and insulin.
Get more information on the types of antidepressants now.
Serotonin Antagonist Reuptake Inhibitors

Serotonin antagonist reuptake inhibitors (SARIs), as the name indicates, prevent the reuptake of serotonin. However, it is also vital to note that they prevent certain serotonin particles, those released in a synapse, from binding to undesired receptors. Instead, they redirect them to the receptors that will help the nerve cells that affect an individual's mood work better. Two examples of medicines in this class are trazodone and nefazodone. Medications in this class treat major depression, but also act as an off-label treatment for anxiety and insomnia.
They have fewer side effects than older antidepressants. However, common side effects include fatigue, dry mouth, constipation, headache, and blurred vision. SARIs may interact with several other medications, including anti-inflammatories, blood thinners, and other antidepressants, like MAOIs and SSRIs.
