Common Causes And Complications Of OCD
Obsessive-compulsive disorder (OCD) is a type of anxiety disorder, which is a category of mental illnesses that present with irrational or unusual levels of fear or worry. OCD is a chronic condition that causes uncontrollable and recurring thoughts called obsessions, along with compulsive behaviors the patient feels must be repeated. Each presentation of obsessive-compulsive disorder is different. The precise nature of the compulsions and obsessions is unique. The most well-known manifestation includes cleaning and fear of germs, but OCD often manifests in other ways.
There are several common causes of contributing factors to the development of obsessive-compulsive disorder. Get familiar with them now.
Certain Brain Abnormalities
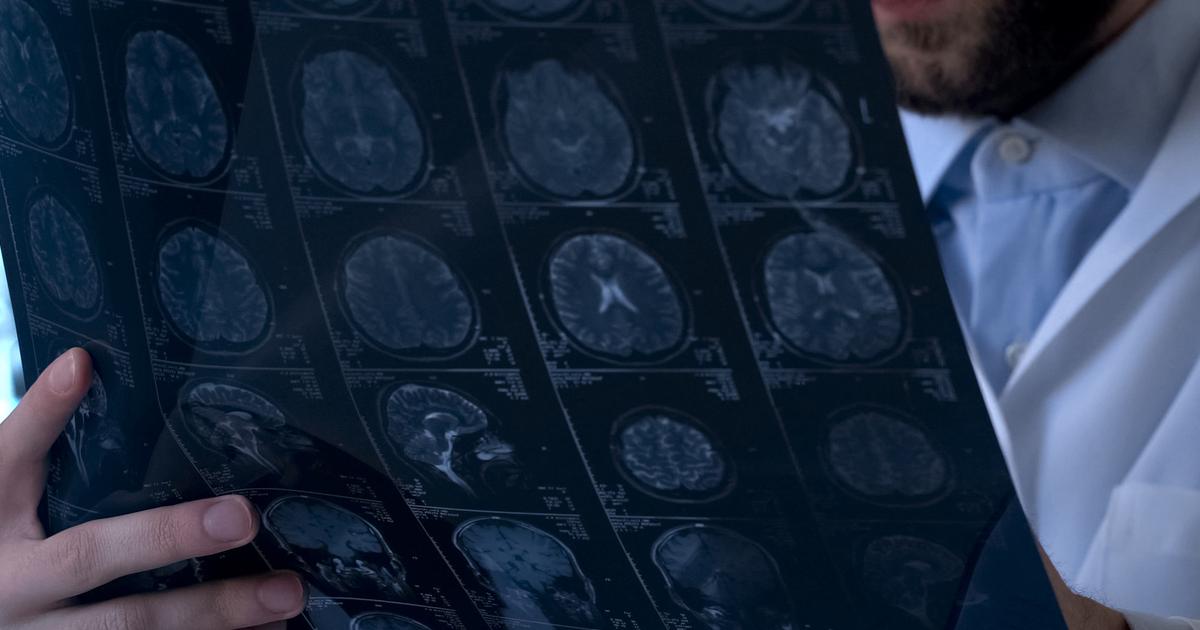
Certain brain abnormalities have been identified in individuals who have obsessive-compulsive disorder. Not everyone with this condition has the abnormalities, and not every person with the abnormalities has OCD. However, there's a marked correlation between them. The research was done by comparing hundreds of different brain scans, and researchers believe the processes and areas of the brain they've identified play a role in the repetitive compulsions that are part of obsessive-compulsive disorder. The study indicates OCD patients can sometimes get stuck in a repetitive cognitive loop that keeps them from stopping the behaviors even when they cause distress. In these patients, the brain has a disproportionately large response to errors, and a disproportionately small response to stop signals. Errors are cognitive processing issues or irrational thoughts. A person without obsessive-compulsive disorder can use 'stop' signals to stop an irrational or intrusive thought from repeating. But someone with this disorder can't stop obsessing over the error, even if they're aware the behavior is irrational and causing distress.
Read more about what can trigger the development of obsessive-compulsive disorder now.
Environmental Factors

While researchers believe obsessive-compulsive disorder has a basis in neurochemical abnormalities, the way symptoms present is often determined by environmental factors, as is the severity of symptoms. Researchers who study the way the environment shapes brain development believe behavioral conditioning might play a part in an individual's development of compulsions and obsessions. For example, if someone is afraid of germs, they might obsessively wash their hands to relieve the anxiety about germs. Some cognitive behavioral researchers believe the misinterpretation of intrusive thought leads to compulsions and obsessions. Intrusive thoughts happen to everyone. They may involve thoughts about perpetuating harmful behaviors or doing things that frighten the individual. In a neurotypical person, these thoughts can be put aside, but OCD patients become fixated on them. An individual can have dysfunctional beliefs about themselves shaped by their environment. One common belief is an individual can cause or prevent negative outcomes by following their compulsions. Another is the idea having a thought is the same as actually acting upon the thought.
Keep reading to learn more about the causes of obsessive-compulsive disorder now.
Genetics And Family History
Research shows genetics and family history play a large role in the development of obsessive-compulsive disorder. Some of this may be because the brain abnormalities involved in OCD can be passed down through families. Being raised in a household with family members with untreated obsessive-compulsive disorder can also increase an individual's risk of developing obsessions and compulsions. The National Institutes of Health funded a study to examine DNA and its correlation to this condition. The study drew a correlation between OCD, similar anxiety disorders, and a mutation of the serotonin transport gene found in humans. Some patients with severe cases of obsessive-compulsive disorder also have a second mutation within the same gene. Around one-fourth of OCD patients have an immediate member of the family who has the disorder. Studies done on twins indicated if one identical twin has OCD, the other is more likely to develop the condition than if the twins are fraternal. The findings in the twin studies suggest genetics are responsible for between forty-five and sixty-five percent of an individual's risk of developing OCD.
Get more details on what increases the risk of obsessive-compulsive disorder now.
Increased Stress

Increased stress can be a factor in how symptoms of obsessive-compulsive disorder present. Some individuals are under the impression stress itself is enough to cause OCD, but this isn't the case. An individual who already has the condition, though, will often see a worsening in symptoms when they experience stress. Illness, fatigue, and anxiety can have an impact on the severity of symptoms. Changes in routine can cause increased stress, leading to a vicious cycle of worsening symptoms. AN obsessive-compulsive disorder patient who hasn't experienced visible symptoms for a while might have a symptom flareup following a stressful life event. Severe trauma can cause symptoms to begin. Common traumas include the death of a loved one or abuse. Some life changes that can cause symptoms to recur include transitions to new schools or workplaces, moving into a new home or community, marriage, divorce, the birth of a child, or the birth of a sibling. Some individuals have developed new symptoms following the stress of natural disasters like hurricanes and earthquakes.
Continue to reveal more factors linked to the development of obsessive-compulsive disorder now.
Presence Of Other Mental Health Disorders

Other mental health disorders don't cause obsessive-compulsive disorder by themselves. However, the presence of other mental health disorders has a high correlation with OCD. It's common for obsessive-compulsive disorder patients to have one or more other mental health disorders due to the abnormalities in neurotransmitters causing multiple different symptoms. OCD is classified as an anxiety disorder, and many patients also have another anxiety disorder alongside it. The disorders that might occur alongside OCD include generalized anxiety disorder, separation anxiety disorder, panic attacks, specific phobias, and social anxiety disorder. These disorders all have irrational anxiety and fear as their basis, though the circumstances and presentation of the fear are different. Depression is also very common in obsessive-compulsive disorder patients. The symptoms of major depressive disorder include mood changes, loss of interest in activities, sleep issues, and fatigue lasting more than two weeks. Bipolar disorder can also occur alongside OCD, with the hallmark symptoms being extreme mood and behavioral changes.
Keep reading to learn more about the various causes and complications linked to obsessive-compulsive disorder now.
Autoimmune Causes

There is some research indicating obsessive-compulsive disorder might be correlated with certain autoimmune diseases. An underlying autoimmune condition can potentially trigger OCD in some individuals. Alternatively, both the autoimmune condition and OCD may be related to an unidentified underlying condition. Researchers are still trying to determine the actual link between obsessive-compulsive disorder and autoimmune disorders. Some research shows OCD has a higher prevalence in children who develop streptococcal infections. The theory is OCD symptoms occur because the body undergoes an autoimmune response to bacterial infections. Medical researchers have coined the term PANDAS to talk about children who have unusually sudden OCD behaviors or tics that develop following an infection. PANDAS stands for 'pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections.' Researchers believe genetics likely play a role in an individual's risk of developing PANDAS. They have also noted unusual correlations between certain antibodies in a child's blood and whether or not they develop PANDAS.
Uncover additional causes and complications of obsessive-compulsive disorder now.
Other Pathogens (PANS)

In addition to the link between autoimmune responses and the onset of obsessive-compulsive disorder, researchers have also noted a phenomenon they refer to as pediatric acute-onset neuropsychiatric syndrome (PANS). As a syndrome, it's a clinical disorder that describes a collection of symptoms with no known root cause. The disorder occurs when children suddenly develop OCD symptoms or restrictions in their eating habits, including deterioration in their behavior in a minimum of two of the eight main areas of their lives. The trigger for PANS isn't always known, but researchers believe it is brought on by one or multiple pathogens. PANDAS is a type of PANS, but for a child to be diagnosed with PANDAS, the pathogen must have been a strep infection. In theory, any pathogen has the potential to cause some type of PANS. Researchers believe there's evidence for PANS developing as a result of pneumonia, varicella, influenza, and Lyme disease. Lyme disease is also theorized to cause other psychiatric symptoms.
Discover additional complications and causes of obsessive-compulsive disorder now.
Traumatic Brain Injury
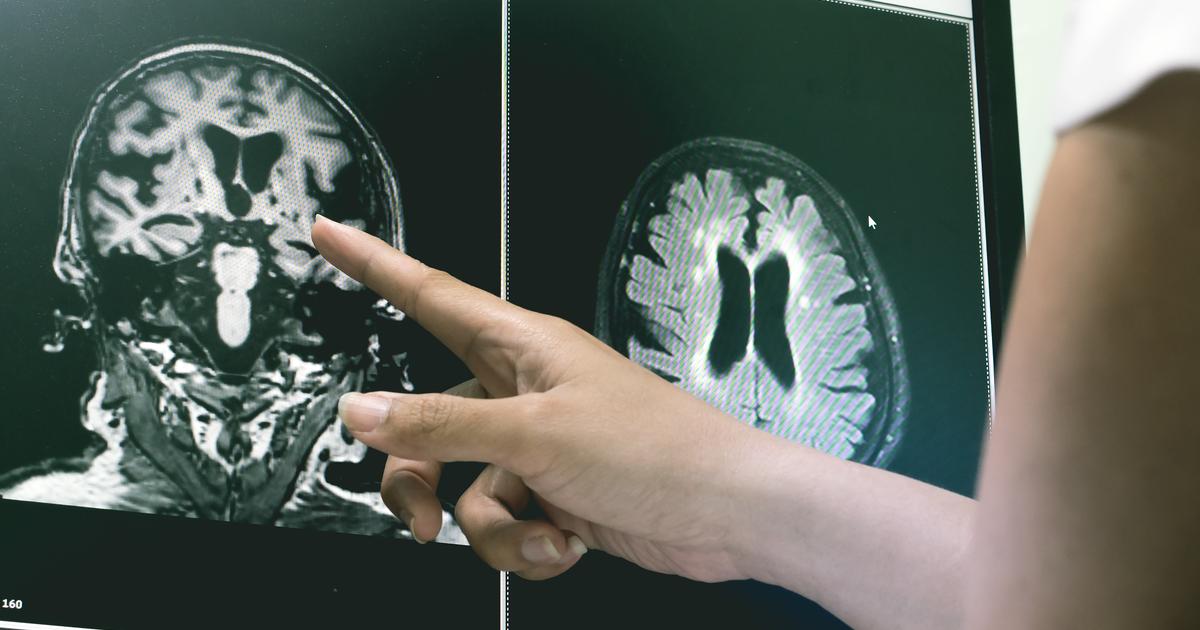
Some patients develop obsessive-compulsive disorder after they suffer a traumatic brain injury. A traumatic brain injury might occur due to a fall, firearm accident, other accident, or motor vehicle collision. These types of injuries have a wide variety of symptoms and can be hard to predict. Some patients experience little to no cognitive issues following a traumatic brain injury. Others might develop psychiatric symptoms like those associated with OCD. Some patients have impaired cognitive functioning, struggle with their memory, or experience reduced concentration. The exact symptoms of the traumatic brain injury vary depending on the severity of the injury and the affected part of the brain. When OCD develops as a result of a traumatic brain injury, the symptoms tend to manifest very soon or immediately following the traumatic event. There have been cases, though, where obsessive-compulsive disorder from a brain injury wasn't professionally diagnosed until months had gone by after the injury. Most individuals who develop OCD after a traumatic brain injury also exhibit the symptoms of major depressive disorder. The reason behind this correlation isn't currently known.
Learn more about triggers and complications of obsessive-compulsive disorder now.
Relationship Issues

Obsessive-compulsive disorder manifests in different ways for everyone. Like any mental illness, however, the symptoms can have a serious effect on interpersonal relationships. Patients might struggle to maintain friendships, romantic relationships, or familial relationships. They might find their relationships are tense and strained. Many patients with obsessive-compulsive disorder have reported their symptoms have hurt their marriage or romantic life. Some patients have trouble with self-esteem and dealing with shame about their symptoms, which can manifest in relationship tension and avoidance. Many individuals with OCD believe they have to hide their symptoms to avoid being rejected by their romantic partner. When depression accompanies OCD symptoms, it can be even harder to maintain healthy relationships. It's also common for obsessive-compulsive disorder patients to have issues with sexual relations connected to their symptoms. Some patients might have disturbing obsessive thought spirals about contamination or sexual assault. When the romantic partner doesn't understand the cause, this can lead to fighting and instability in the relationship.
Uncover additional details on the causes and complications of obsessive-compulsive disorder now.
Inability To Attend Certain Activities

One common complication of OCD is the avoidance of certain activities, places, people, or social situations. There may be a multitude of reasons for this. Some patients might avoid social activities because of the shame they're struggling with. In other cases, certain phenomena might trigger OCD symptoms. If a patient becomes afraid that going to an event or being near a certain individual will cause a bad episode, they might avoid that situation because they believe missing it is better than the potential issue. However, avoiding situations doesn't help with the management of obsessive-compulsive disorder symptoms in the long run. In fact, the more an individual avoids a situation, the greater the anxiety surrounding it will be. Individuals who feel isolated by obsessive-compulsive disorder also tend to experience stronger symptoms of depression due to their isolation. This can be especially brutal if the fears are related to things the patient previously enjoyed like friends, favorite hangout spots, the homes of family members, or hobbies. If the individual does go into a potentially triggering situation and have a bad reaction, this negative association may cause them to avoid it more fiercely in the future.
