Health Risks Of Dental Implants
Dental implants are artificial tooth roots surgically placed into the jaw to hold a bridge or a replacement tooth. Many individuals get dental implants if they have lost a tooth or if they have had periodontal disease. There are two different kinds of dental implants including endosteal and subperiosteal. Endosteal is the most typical kind of dental implant and includes placing screws, cylinders, or blades into the jawbone. The implant holds the prosthetic teeth and is generally the type of implant patients use if they have removable dentures.
Subperiosteal implants place a metal framework on top of the jaw with posts coming through the gum to hold the prosthetic teeth. These implants are used when patients do not have enough bone height, or they cannot wear normal dentures. Before considering dental implants, it is vital to understand the benefits and risks. Most implants have a ninety-five to ninety-eight percent success rate, though some patients have complications or side effects. Reveal the risks now.
Implant Breakage
Implant breakage used to be more common in early dental implants when the materials used and the implant design was not as advanced. However, with the technological advancements and the difference in the material used to reduce the risk of dental implants breaking. These days, dental implants are typically made with titanium alloy. This metal is not just one of the strongest metals available, but it is also highly compatible with the bone. Titanium implants are typically used to replace the root of the missing tooth. However, even titanium can break if it is impacted with enough force. The most likely place for the implant to break is at the weakest point called the abutment screw.
The abutment screw connects the dental implant with the dental crown. Though this can bend or break, it is very easy to fix. The dental crown can also break, as they are not made of titanium and are more likely to break than the titanium implants. However, they have also become extremely durable because of the advancements in ceramic technology. Implant breakage might occur with excessive teeth grinding or a sudden blow to the face.
Tissue Necrosis
Tissue necrosis occurs when there is a lack of oxygen and blood to the tissue. It may happen when there is thin tissue around the implant or when there is some form of mechanical trauma to the tissue. It may also be the result of pressure from the inadequate rebase of a removable denture. Tissue damage may also occur when there is too much or too little tension on the suture, causing the blood supply to become impaired. Compression of the bone debris may cause tissue necrosis as well because it gathers at the bottom of the implant site when the implant is inserted with excessive force.
Nerve Damage
Nerve complications will occur if the dentist is inexperienced. However, a skilled implant expert will be able to find any issues when they check the X-rays and CT scans and minimize the chances of damage. It is more likely to occur when the surgery occurs in the lower jawbone because there is a nerve that runs along the lower jawbone called the inferior alveolar nerve. Nerve damage can happen when the implant is placed too close to it.
If patients feel pain, numbness, or a tingling sensation, they may have nerve damage. These symptoms may be present in the facial areas such as the cheek, chin, lips, or tongue, as well as in the gums. Nerve damage may be temporary, but patients may also need to have the dental implant extracted as well.
Sinus Problems

Sinus problems are more serious when it is perforated. The sinuses are located above the upper teeth, called the maxillary sinuses. Sinus perforation is when the dental implant is placed on the upper jaw and pierces through the sinus. Patients will notice pressure in their sinuses or a stuffy nose. Though piercing through the sinus sounds serious, it is generally easy to fix with a collagen membrane. The tissue can often heal on its own depending on the size of the perforation. However, the risk is only a bad sinus infection, though the dental implant may need to be removed to properly fix the area and repair the perforation. The CT scan will ensure the sinus has not been perforated.
Infection At Implant Site

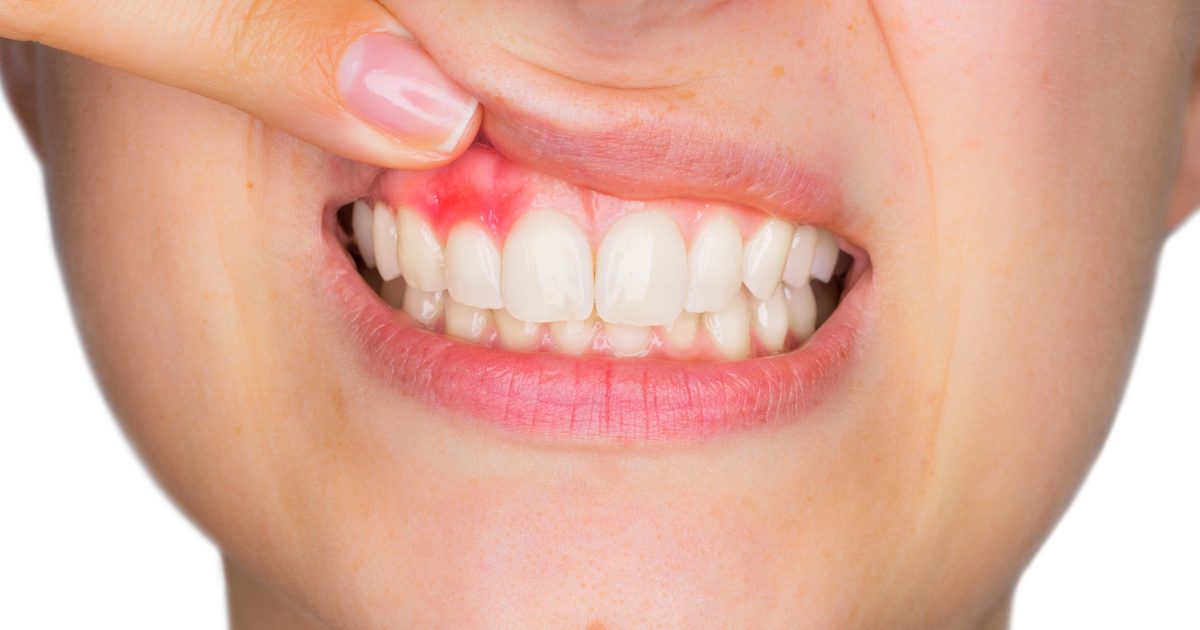
Infections at the dental implant site often happen when the immune system triggers the inflammation response to attack the surrounding bone and gum tissue. It can also occur when peri-implantitis causes the gum and bone surrounding the implant to become inflamed and may cause the loss of bone density in the surrounding bone. This occurs when bacteria is introduced to the surgical area. Bacteria can be introduced throughout the different stages of operation if the dentist does not observe the proper protocol for dental hygiene. It may happen if the equipment is not sterile or if the implant is contaminated.
It may also occur if the patient has an untreated infection. Peri-implantitis often occurs years after the surgery and is more likely to happen in individuals who smoke or have diabetes, poor immune systems, thin gums, or poor dental hygiene. If patients notice their gums look red or purple, if there is pus coming out from the implant, or abnormal bleeding at the gum line, they may have peri-implantitis. The dentist will need to reopen the gums to clean the area to remove the bacteria. A bone graft might also be necessary if there is bone loss, and severe cases might need to remove the dental implant.
Bone Loss
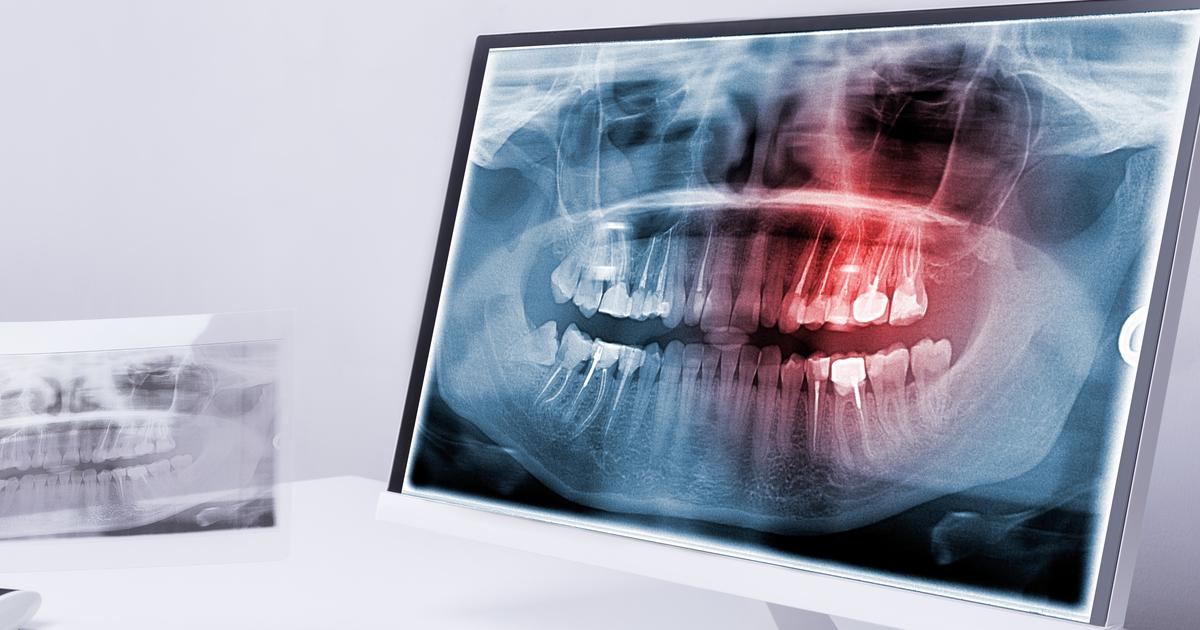
The placement of dental implants may put an individual at an increased risk of having bone loss in the years following the installation. Peri-implantitis is an infection that affects the soft tissue around the bone-integrated implant. The pathophysiology of this particular type of infection is known to be associated with a disruption in the equilibrium between an individual's defense system in the body and the microflora in their oral cavity. Plaque with microbial properties can form on the surface of an individual's dental implant the same way it can build up on the natural tooth surface. The soft tissues around the implant abutment become infected and inflamed due to the tissue's response to the bacterial presence. This infection can spread into the actual tissues of the bone itself around the implant fusion.
Peri-implantitis often results in the breakdown of alveolar bone that surrounds the implant. It is estimated between ten and twenty percent of all patients who have a dental implant installed experience alveolar bone loss after the implant has been functional for about a decade. Bone loss following implant installation is technically defined by a bone loss of 1.5 millimeters as referenced on a radiograph within the first year or greater than 0.2 millimeters of bone loss for each subsequent year. Early treatment of this infection can prevent dental implant-associated bone loss.
Gingival Recession

The placement of a dental implant can increase an individual's risk of gingival recession around the implant following its installation. Both technical and biological factors contribute to the occurrence of this complication. Physiologic reactions to the implant itself by the individual's soft gum tissue can cause an alteration in the gingival margin level or bone level that surrounds the dental implant. The labial plate inside of the bone starts a process of reabsorption of tissues following the extraction of a tooth. As a result of this mechanism, soft tissue recession of the gums surrounding the implant naturally occurs.
However, the recession of gingival tissue occurs more often as a result of technical factors at play. Many of these technical factors that lead to gum recession around the implant are highly preventable by the dentist facilitating the dental implant process. The diameter of the implant, the timing of the delivery of final restoration, excess cement, implant placement, biologic violation of width, and alcohol contamination are all factors that can contribute to post dental implant gingival recession.
Hyperplasia
Individuals who have a dental implant placed are taking the risk of developing gingival overgrowth (hyperplasia) following the installation around the peri-implant mucosa. This type of tissue overgrowth around the dental implant causes extreme difficulty with proper hygiene practices of the implant and surrounding teeth. Hyperplasia around an implant is thought to be the result of an abnormal and exaggerated allergic reaction to the materials of the implant. Usually, titanium and nickel mixtures used in the final prosthesis can cause these types of reactions. Soft tissue reactions and eczema are also associated with the use of beryllium and aluminum in dental implant materials that may result in gingival overgrowth.
The mechanism behind these allergic reactions is the result of the tissue rebuilding process that occurs when the body repairs its own damaged tissues. This process is similar to what occurs when scarring forms on internal organs or the skin after the body has repaired damaged tissues. In the majority of individuals who experience hyperplasia as a result of dental implant installation, the cause is not related to technical factors involving the implant placement technique.
Excessive Bleeding
Excessive bleeding is an immediate complication that can occur in individuals who assume the risk of having a dental implant installed. The floor of an individual's mouth is often the site of such excessive bleeding. The mandible or jawbone is supplied by the branches of the submental and sublingual arteries that are located near the lingual cortical plate. During the process of implant placement or drilling in the procedure, the lingual cortical bone can become damaged. Excessive bleeding from dental implant placement is much less prevalent in installations that take place in an individual's upper jaw.
While imaging and careful surgical preparation are designed to prevent such complications by locating critical structures, the oral arrangement and anatomy are not exactly the same in each patient who has a dental implant placed. Most cases of excessive bleeding occur in the region where the lower canine teeth are located because it is the general point where the arteries run the closest to the individual's alveolar crest and lingual plate. Usually, longer implants that exceed fourteen millimeters are involved in cases complicated by excessive bleeding. The best course of prevention is the use of shorter implants in any part of the anterior mandibular section to lower the risk of blood vessel-related complications.
Dehiscence
Individuals who have a dental implant installed assume the risk of alveolar bone loss on the facial part of the tooth or what is known as dehiscence. This complication leaves a root exposed defect below the gumline of the dental implant prosthesis. This defect appears as an isolated region where the root of the implant has become exposed and is not covered by bone. This type of defect can extend all the way down the root of the implant, or it can be limited to a few millimeters from the gumline. While the implant root is denuded of bone covering in the affected region, it is still covered by a thin layer of soft tissue. The implants placed in the canines and incisors are more susceptible to this complication.
The mechanism that causes dehiscence to occur around dental implants is thought to be related to the placement of an implant into bone tissue that is too thinned out or weak to support it. Additionally, an excessive burden on the implant over time can cause some individuals to develop this deformity after the installation of their dental implant. The replacement of the missing bone around the implant with specialized bone-like graft products by an experienced provider can help treat this complication. Ensuring there is a sufficient amount of bone to support the implant prior to the placement can lower the risk of dehiscence occurrence.
