What Causes Pain In The Lower Left Abdomen?
It can be difficult to pinpoint the cause of an individual's pain in their abdomen. However, the location of the pain can provide a relative idea of what the cause could be. Pain can be described as a sharp feeling, or as a deep and persistent ache. Pain in the lower left abdomen and upper left pelvis can come on suddenly and severely, or it can be chronic and gradually worsen over time.
The source of an individual's lower left abdominal pain can be pinpointed through the use of physical examinations, blood tests, urine tests, x-rays, abdominal ultrasound, computerized tomography scans, and MRI scans. The management and treatment of lower left abdominal pain are highly dependent on its underlying cause. The methods used include pain medication, gas relief medication, antacid medication, surgery, and diet changes.
Indigestion

Indigestion describes a sensation of discomfort in an individual's upper abdominal area. However, indigestion is felt differently from one person to the next and may have several other accompanying symptoms. Most individuals experiencing indigestion tend to have painful sensations in their upper abdominal region. This sensation can be caused by a build-up of acid following the consumption of a meal. An individual's stomach produces acid to help digest food, and this acid can irritate their bowel, stomach, or esophagus.
Indigestion can also be the result of eating too quickly, drinking too much alcohol, swallowing air while eating, certain medications, and pregnancy in some cases. The feeling of indigestion is described by many as a slight pain, mild discomfort, bloating, heartburn, a burning sensation, or gas. Indigestion tends to worsen or occur more frequently when the affected individual is under stress. Because indigestion manifests differently in everyone, some individuals may feel it as pain in their lower left abdomen.
Diverticulitis
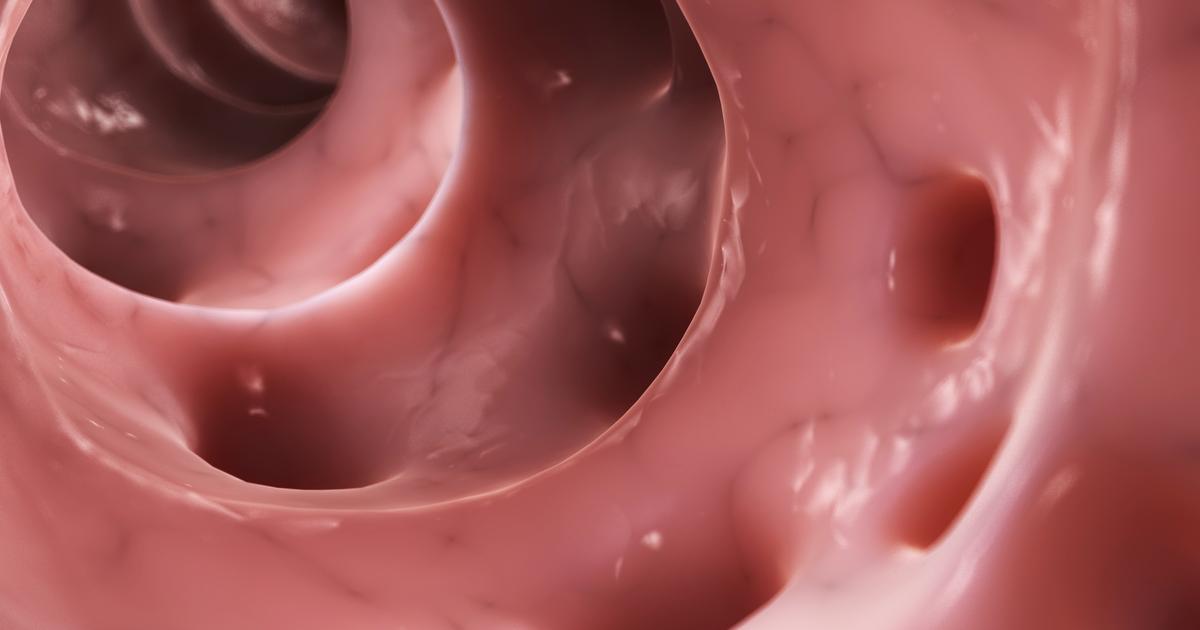
Diverticulitis is an illness where an individual's diverticula, pouches that can develop in an individual's intestinal lining, become inflamed and infected. Diverticula most commonly form in an individual's large intestine or colon but can develop at any point in the intestines. In most individuals, they are benign and do not cause problems.
However, the diverticula in some individuals may tear open or become compressed by injury or other structures. These mechanisms can cause the diverticula to become inflamed as the body attempts to repair the damaged tissue, or become infected as a virus or bacteria invade and colonize in the tissue. Pain that occurs from diverticulitis is most commonly located on the lower-left side of an individual's abdomen. Diverticulitis pain is persistent and may last for several days.
Hernia

A hernia is a condition where an individual's abdominal wall becomes weakened or torn, allowing the internal organs to bulge out of it. An individual's abdominal lining consists of muscular tissue that keeps all of the internal organs in their places. The type of hernia most likely to produce pain in an individual's lower left abdominal region is called an inguinal hernia, which occurs when part of an individual's intestines protrude through their lower abdominal wall into their groin or inguinal region.
This type of hernia is known to produce the most pain in the lower left-hand abdominal quadrant when the affected individual performs certain actions and activities. Lifting heavy or cumbersome items, bending over, coughing, or straining with a bowel movement are all activities known to produce painful sensations. If a patient's hernia becomes strangulated or incarcerated, the pain they experience from the hernia becomes more severe.
Celiac Disease

Celiac disease is a condition where an affected individual has a severe immune response when they consume a substance called gluten. Gluten is a protein typically found in foods that have rye, wheat, and barley. The immune response in celiac disease patients affects their small intestine. Over time, the lining of the individual's small intestine becomes too damaged to be able to absorb nutrients properly.
This malabsorption and damage cause the patient to have multiple digestive symptoms, including bloating, diarrhea, pain in the abdomen, nausea, vomiting, constipation, and weight loss. The abdominal pain in affected individuals is not always focal and can radiate to different regions of the abdomen. Therefore, an individual who has celiac disease and intestinal damage may present with pain in the lower left abdomen.
Crohn's Disease

Crohn's disease is a type of inflammatory bowel disease, and affected individuals have extensive inflammation in different parts of their gastrointestinal tract. The inflammation that occurs in Crohn's disease is so severe that it can penetrate deep into the patient's bowels. The area of the digestive tract most commonly affected by such inflammation is the ileum or last segment of the small intestine. The ileum is located on the lower left side of an individual's abdomen, just above their appendix.
Symptoms that occur in Crohn's disease patients include diarrhea, fatigue, bloody stools, poor appetite, anal pain, anal drainage, fever, abdominal pain, abdominal cramping, mouth sores, and weight loss. Crohn's disease alone can cause significant pain in the lower left abdomen, and several complications that can occur due to this condition are also known to produce pain in this region.
Gas

Gas is produced by the digestive system as it breaks down food, and gas is also produced as a result of swallowing air. The body expels gas through burping and flatulence. On average, most people pass gas at least twenty times per day. Beans, broccoli, cabbage, onions, fruit, and soft drinks are most likely to produce gas when consumed, and excessive gas is a leading cause of pain in the lower left abdomen. To reduce pain associated with gas, patients may wish to take an over-the-counter medication such as simethicone.
Patients who are pregnant or breastfeeding should check with their doctor before using this medicine. Some individuals prefer to take probiotics or digestive enzymes for gas relief. If gas causes persistent pain, patients should see a doctor for an evaluation. It can be beneficial to keep a food diary to share with the doctor, as this information may help with determining the underlying cause of the patient's symptoms.
Kidney Stones

Kidney stones are mineral and salt deposits that can form inside the kidneys. They are often caused by dehydration, kidney infections, and hormonal or dietary changes. Patients with kidney stones generally experience sharp, severe pain in the abdomen, back, and sides, and they might have blood in the urine or fever as well. To detect kidney stones, doctors perform blood tests, urine tests, and an ultrasound. Some patients might be asked to have more advanced imaging studies, including an abdominal MRI scan or an intravenous pyelogram.
Some kidney stones may be small enough to pass through urination, but larger stones often require surgical procedures. Doctors may choose to perform a lithotripsy to break up kidney stones, and tunnel surgery or a ureteroscopy could be used to surgically remove the stones. Once the stones have been removed, most patients experience a significant reduction in their pain.
Menstrual Cramps

Menstrual cramps can occur at any point during menstruation, and they often vary in severity and duration. Some women may experience cramping only on the first or second day of their cycle, and others may have cramps for the majority (or all) of their menstrual period. Menstrual cramps often feel like a dull, throbbing ache, and some women experience stabbing pain with cramps as well. Cramps can cause pain in the abdomen and thighs. To relieve the pain of menstrual cramps, doctors suggest applying a heating pad to the thighs and lower abdomen.
Taking ibuprofen or another nonsteroidal anti-inflammatory medication may help, and natural remedies such as thyme and primrose oil are beneficial for certain patients. Taking a short walk or engaging in other gentle exercises such as yoga could ease menstrual cramps, and eating a low-sugar diet is believed to reduce cramping overall. If menstrual cramps are severe or last more than two or three days, patients should see their primary care doctor for an assessment, and any case of new or severe pain in the lower abdomen should be evaluated promptly. Doctors may need to perform ultrasounds or other imaging studies to check for fibroids or underlying conditions such as endometriosis.
Lactose Intolerance

Lactose intolerance is a condition in which the patient is unable to properly digest the sugar (lactose) in dairy products. This usually develops due to a deficiency in an enzyme known as lactase. Lactose intolerance is more common in patients born prematurely and those who have had chemotherapy. Patients with lactose intolerance have abdominal cramps, nausea, bloating, gas, and diarrhea, and these symptoms normally begin between thirty to 120 minutes after eating. To diagnose this condition, doctors will perform a lactose tolerance test, stool acidity test, or hydrogen breath test.
Patients who have severe lactose intolerance may benefit from the use of lactase enzyme tablets or drops. These medications are taken immediately before eating a meal with dairy products, and they make it easier to digest lactose. Patients typically benefit from lifestyle modifications such as reducing dairy intake or using lactose-free products. Most individuals with lactose intolerance can tolerate a small amount of dairy products in their diets.
Shingles
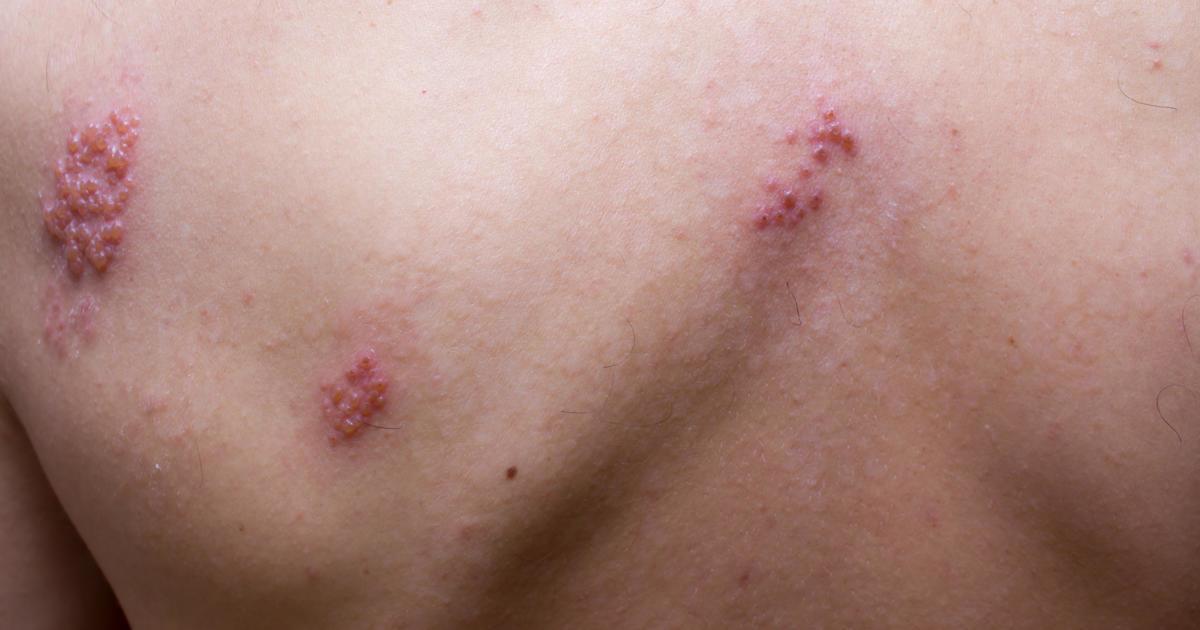
Shingles is a viral infection caused by the varicella-zoster virus. This infection produces a painful, blistering rash that can cover large areas of the body. Patients with shingles could develop a fever, and they may also have stomach upset, swollen lymph nodes, fatigue, nausea, and body aches. The shingles rash can be extremely itchy, and some patients experience a burning, tingling sensation. Complications from shingles include bacterial skin infections, hearing and balance issues, neurological problems, and postherpetic neuralgia. When shingles occurs around the eyes, it can trigger an eye infection that may lead to vision loss.
Several vaccinations are available to prevent shingles, and they are recommended for individuals over sixty years old. To diagnose shingles, doctors take the patient's health history and perform a physical examination to check for a rash or blisters. A tissue scraping might be necessary. Treatment for shingles involves antiviral drugs such as acyclovir and valacyclovir. Since the pain from shingles can be severe, doctors may prescribe a combination of pain relievers, including numbing creams, capsaicin topical patches, and local anesthetic injections.
