Methods Of Treating And Preventing Molluscum Contagiosum
Molluscum contagiosum is a contagious skin infection caused by a virus. It is most commonly diagnosed in children and in adults with compromised immune systems. The virus produces clusters of painless and firm pink or flesh-colored bumps. Sometimes, the bumps may be itchy. Typically, most patients develop between ten and twenty bumps, and scratching these may cause additional bumps to form in the surrounding areas. This infection can occur anywhere on the body, and the virus can be transferred to other individuals through skin-to-skin contact and through touching objects used in an infected area. Doctors can normally diagnose molluscum contagiosum with a physical exam and visual inspection, and occasionally, a biopsy may be taken. While the bumps generally go away on their own without treatment, it can take up to a year for them to fade. For patients with conditions that weaken the immune system, the bumps will not resolve if left untreated.
The steps outlined below can help in the prevention and treatment of molluscum contagiosum.
Effective Personal Hygiene

In some cases, effective personal hygiene may prevent the development of molluscum contagiosum, particularly if the individual has recently had close contact with someone who has it. Individuals should wash their hands with warm water and soap for at least twenty seconds, though an alcohol-based hand sanitizer can also be used. Hands should be washed before cooking and eating, after going to the bathroom, and both before and after any contact with infected skin or a potentially infected object. Persons who have or who are treating an individual who has the infection should wear gloves to avoid skin contact. To minimize the spread of molluscum contagiosum, any clothing, towels, or bedding that has come into contact with an infected area should be washed separately, and the use of a bleach solution may be beneficial.
Uncover more methods of treating and preventing molluscum contagiosum now.
Keep Bumps Clean And Covered

Patients should keep bumps clean and covered to reduce the risk of developing additional bumps and transmitting the virus to others. This can be done by using adhesive bandages or sterile gauze pads, and dressings should be changed at least once every three or four days. Alternatively, patients may wish to simply cover the bumps with clothing, perhaps by wearing long sleeves or long pants. Keeping the bumps covered will discourage scratching, which can spread the bumps to other areas of the body, and it will also eliminate the risk of accidentally contacting someone else's skin with the infected area, particularly if the bumps occur on the arms. Patients should examine their skin several times a week to check for the presence of any new bumps, and they should also look for potential signs of infection in existing bumps. For example, any swelling, warmth, redness, discharge, or pain from the bumps should be reported to a primary doctor or dermatologist.
Learn more about how to treat and prevent molluscum contagiosum now.
Cryotherapy
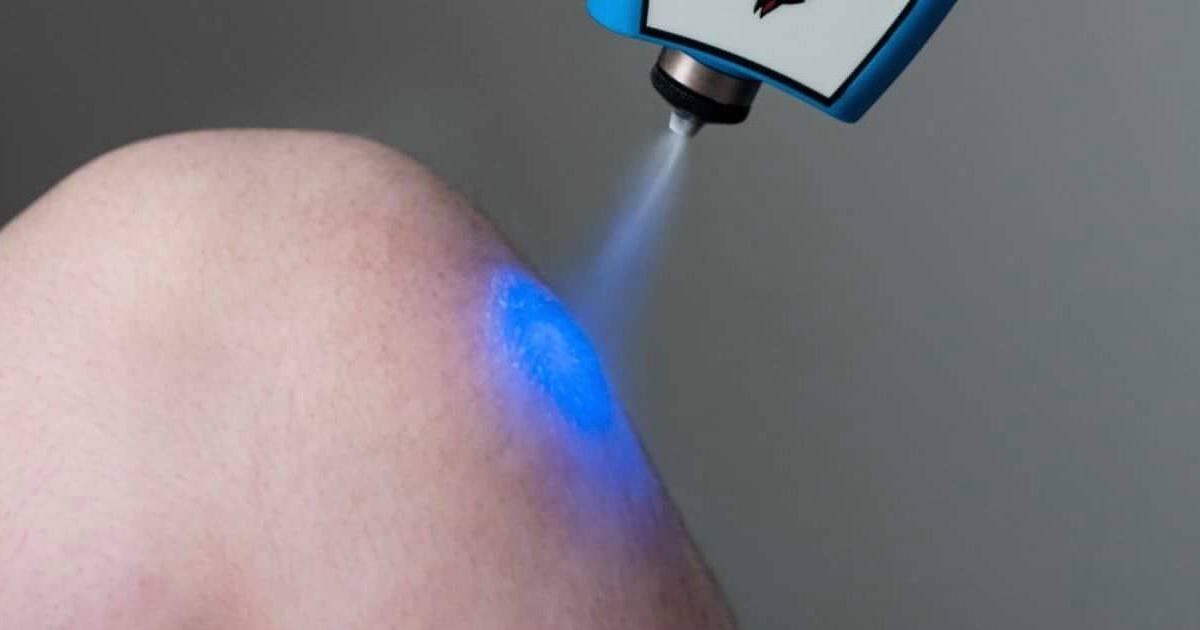
Cryotherapy is a treatment used to remove molluscum contagiosum bumps by freezing them off. This is usually done by spraying liquid nitrogen, an extremely cold substance, onto the affected area. Before the procedure, patients may need to remove makeup from the area, and they may need to stop using lotions or powders a few days before treatment. Patients normally do not need any type of anesthesia for the procedure, and the freezing is done in segments lasting less than thirty seconds each. Shortly after the procedure, patients may notice the affected area turns red or begins to blister. This is considered entirely normal, and patients should not disturb any blisters that form. Clear discharge from the affected area may also occur, and this is considered normal. Generally, the area will heal in around ten days, and the treatment normally leaves no scars. Dermatologists may advise patients to wash the treated area with soap and water at least once a day, and petroleum jelly may be applied if a scab forms. Areas with active discharge will need to be covered with a bandage.
Discover more options for treating and preventing molluscum contagiosum now.
Laser Therapy
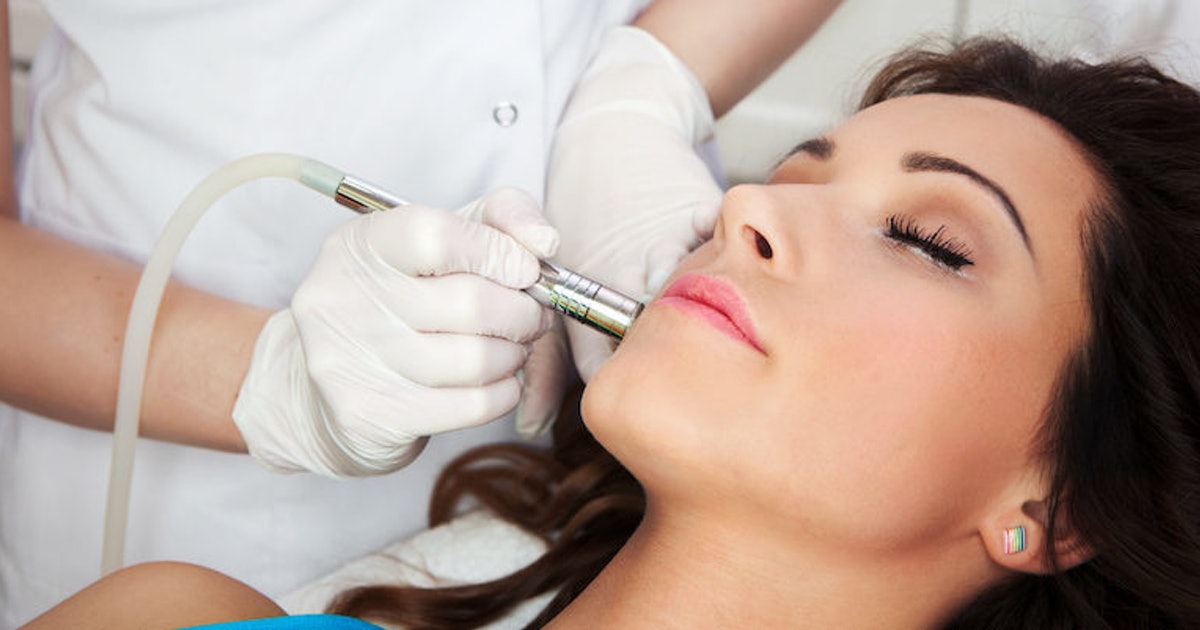
Laser therapy can be a particularly effective treatment for molluscum contagiosum, especially for individuals who have compromised immune systems. Individuals with weakened immune systems, including those with cancer, may develop more than one hundred bumps from molluscum contagiosum. Unlike other therapies, laser treatment can cover a large surface area in a short amount of time and provide faster and more complete relief for complex cases. It is especially beneficial for the treatment of infections involving the genital area. For these types of infections, dermatologists typically use the pulsed dye laser. In one study of forty-three patients, pulsed dye laser treatment completely resolved all of the bumps, and thirty-five percent of the treated patients had no new bumps after two laser sessions. There were no complications associated with the use of the laser, and no anesthetic was needed. Laser treatment should always be performed by licensed personnel, and protective eyewear should be worn by both patients and staff during treatment sessions.
Continue reading for more molluscum contagiosum treatment options now.
Curettage
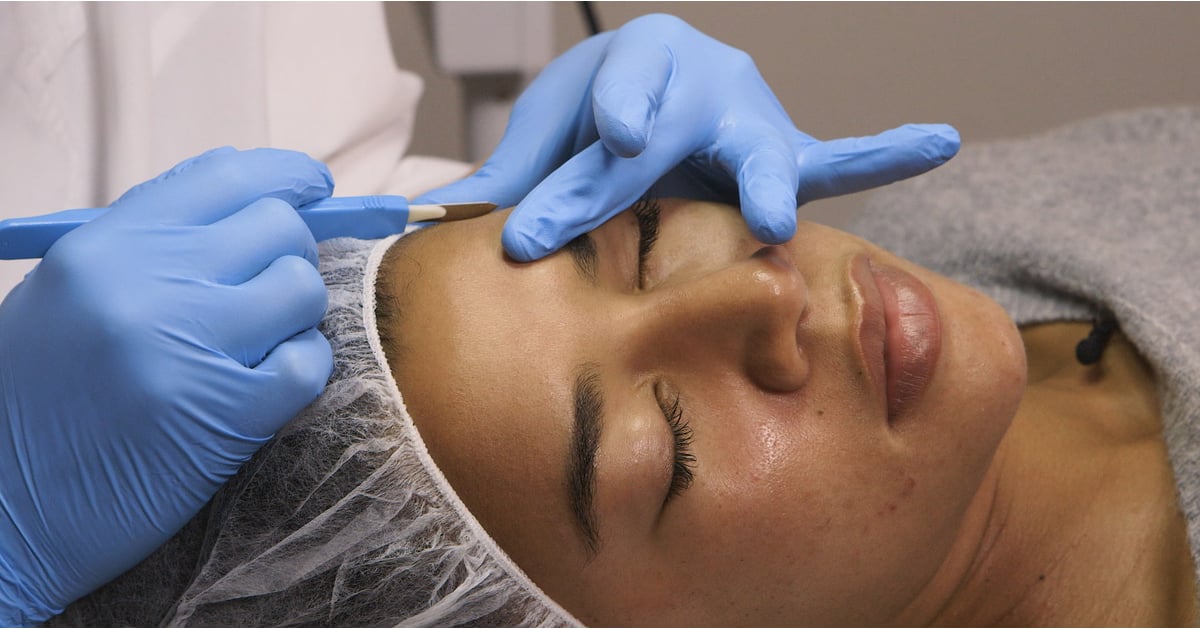
Curettage involves using a device known as a curette to physically remove skin lesions. The curette is shaped like a spoon, and dermatologists use it to pierce the center of each molluscum contagiosum bump. After piercing it, they then scrape away any fluid or other material inside the bump. Local anesthetic is normally used for this procedure, and sutures are not normally needed. Curettage can cause pain, swelling, redness, bleeding, crusting, and scarring at the treatment site. Generally, no recovery time is needed after the procedure, and patients can drive themselves home and resume all normal activities. The dermatologist will provide special aftercare instructions regarding how to clean and bandage the treated area, and patients typically return for a follow-up appointment within a week or two. Depending on the number of bumps involved, patients may need to have the procedure carried out at multiple appointments.
