Top Eczema Triggers To Avoid
Eczema is a common and painful skin condition affecting up to ten percent of the population, including many children. It is thought to be caused by a combination of environmental and inherited factors. The disorder causes patches of dehydrated skin with itching, flaking, scaling, and redness, and can cause frequent skin infections. Eczema is often associated with food and environmental allergies as well as standard household chemicals. The condition can be managed by paying careful attention to the triggers that can bring about outbreaks. These triggers can also cause existing patches to worsen. Combined with proper practices for at-home care, patients can find some relief from the bothersome symptoms of eczema.
Dry Skin
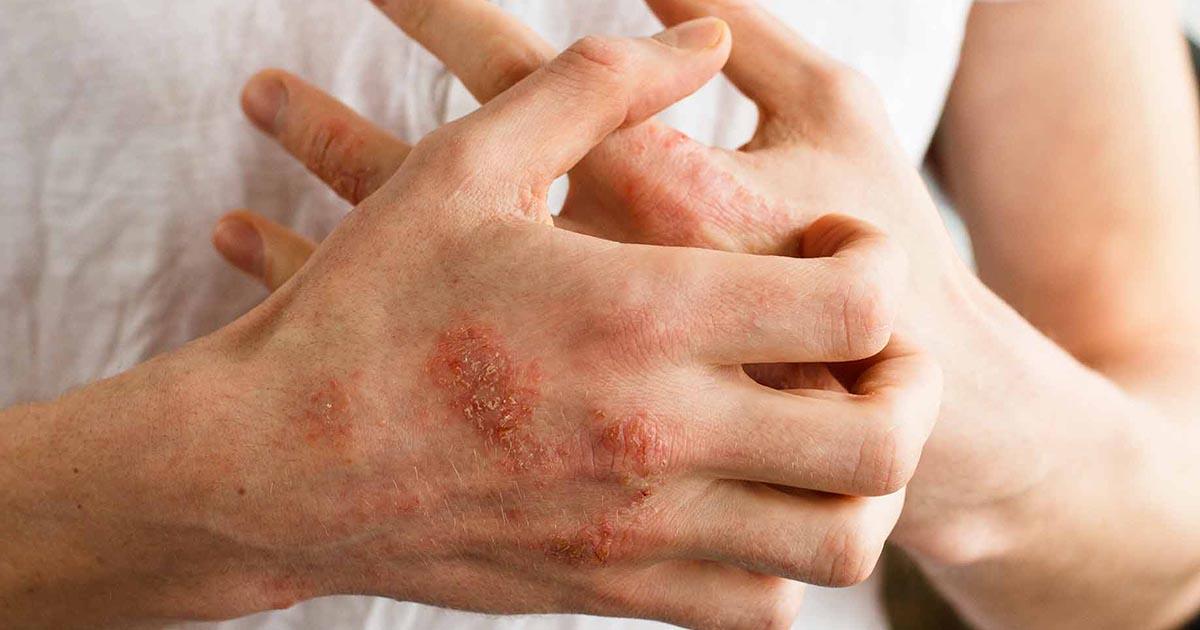
It is imperative to keep eczema-prone skin well moisturized as dehydrated skin is more likely to become cracked and infected. Patients should establish a daily skincare routine as a preventive measure. Bath oils, creams, and lotions are all products for those with eczema should consider using daily. These products should be rich in moisturizing properties and fragrance-free. When bathing or showering, patients should not use excessively hot water. Using cooler water will protect the skin from drying further, and eczema sufferers should use products containing oatmeal or baking soda as they are soothing to the skin. It is best to moisturize within three minutes of getting out of the bath or shower. When using corticosteroid creams, patients should moisturize first to promote optimal absorption into the skin.
Dry Air

Patients living in dry climates or in cold climates where homes are heated in winter may find that their symptoms worsen. At home, patients should use a humidifier to combat the effects of dry air on their skin. The air in the home should be kept between forty-five and fifty-five percent humidity for best results for those living with eczema. Additionally, patients should make sure they are continuously well-hydrated, which is a concern at any time of year. Proper moisturizing will also help protect the skin in dry air conditions. Despite previous medical claims, corticosteroid creams come highly recommended for those with eczema as they contain hydrocortisone steroids that not only reduce inflammation but also effectively reduce itching by locking in surface moisture.
Sudden Changes In Temperature

At any time of year, patients with eczema should avoid rapidly changing temperatures if possible. Going into the cold from a heated car and going from the beach to an air-conditioned house are two typical examples. When these situations cannot be avoided, and particularly in cold weather, be careful to cover the skin with gloves, scarves, hats, and non-binding layers of clothing. Keeping the skin at a more constant temperature will help eczema patients avoid worsening symptoms.
Harsh Soaps And Detergents

Eczema patients are required to be careful with the soaps and detergents they use, both on their laundry and on their skin. Pay particular attention to body soap, as it should be superfatted and non-alkaline. Soaps with added moisturizing cream are the best option for eczema sufferers. Using highly scented or dyed laundry detergents can also cause problems in many patients. Instead, use the mildest product possible to wash clothing; if the patient experiences an outbreak after changing laundry or skin products, avoid using the new product again. People with eczema should also be cautious when using fabric softeners as they contain many unnecessary components that can easily irritate sensitive skin.
Foods

The most common food allergens can often contribute to eczema. Cow’s milk, eggs, soy, gluten, nuts, fish, and shellfish are the top triggers. Patients should try keeping a journal of foods they have eaten and linking them to worsening eczema symptoms, by using an elimination diet to pinpoint the most likely cause of food-related symptoms. Visit an allergist for testing if symptoms are traced to a particular food as some individuals may have related food allergies which could be severe. These need to be diagnosed and treated by a physician to avoid any possible life-threatening reactions.
Environmental Allergens

Pollen, dust mites, mold, dandruff, pet hair, and dander can all cause or exacerbate eczema symptoms. Eczema sufferers should reduce allergens in the home and take an over-the-counter antihistamine to block these reactions. Antihistamines that are known to make the patient drowsy - such as diphenhydramine - may help with nighttime symptoms. Patients should be tested by an allergist to determine whether the pet itself or the dust or pollen it brings inside is the cause of their symptoms. With proper treatment, pets should be able to stay in your home, except in the most extreme cases.
Clothing And Jewelry

Patients with eczema often find that their symptoms worsen when they wear hot, scratchy, or non-breathable clothing such as wool and polyester. Patients should not wear too many layers and should avoid clothing that makes them sweat since sweat can irritate the skin and worsen eczema symptoms. Exposure to metals in jewelry or clothing buttons and snaps can also be a problem; nickel is the most common metal sensitivity that causes eczema outbreaks.
Chemical Irritants

For eczema patients, common household cleaning supplies can cause outbreaks or worsen existing ones. Bleach, latex, cleaning sprays, and air fresheners are all common culprits. When using harsh products, eczema patients should use a cotton-lined cleaning glove while being careful not to work barefoot when using these irritating products, since they can cause eczema on the feet just as easily as on the hands and arms. Cigarette smoke can also be a trigger, so eczema patients should not smoke and reduce their exposure to secondhand smoke whenever possible. Other skin irritants can also include certain types of metals, particularly nickel, fragrances, and antibacterial ointments such as neomycin and bacitracin. Other chemicals include formaldehyde, which is often found in household cleaners, isothiazolinones, which is an antibacterial chemical found in baby wipes, Cocamidopropyl Betaine, which is used to thicken shampoos and lotions, and paraphenylenediamine, which is used in leather dyes and temporary tattoos.
Infection
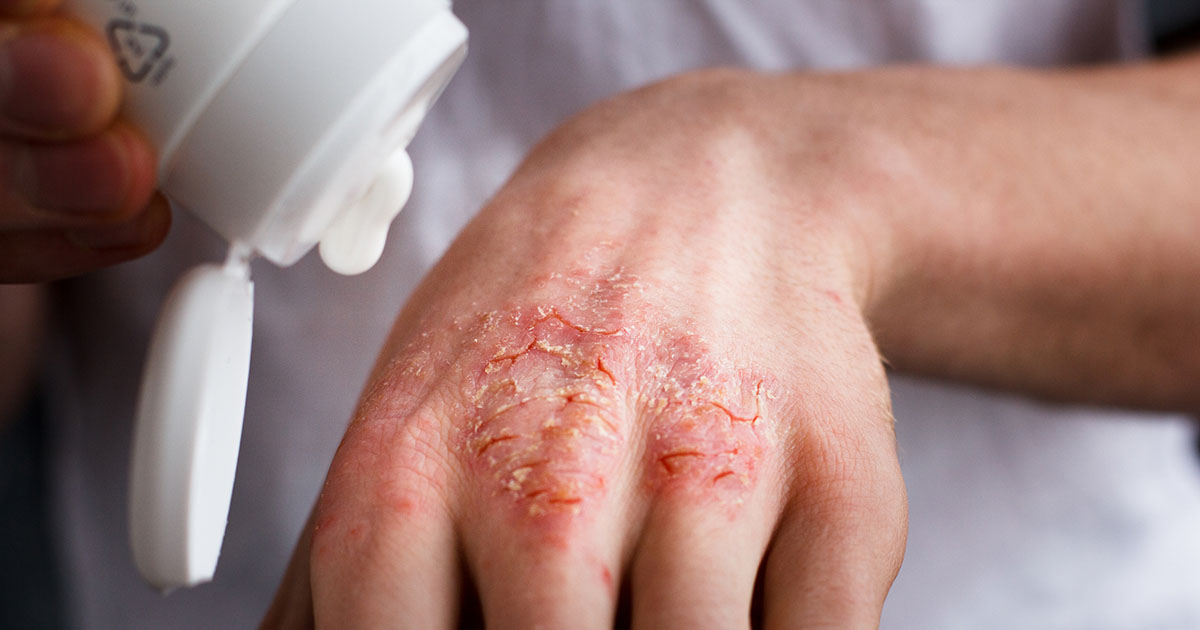
Skin infections can cause a vicious cycle of worsening symptoms. Irritated skin can become infected, which in turn can worsen eczema symptoms. It is vitally important to minimize scratching of eczema plaques as scratching increases the likelihood of these patches becoming infected. Parents should consider putting gloves on eczema-affected children at night to reduce scratching. Signs of infected eczema include worsened itching or burning sensations, blisters, drainage, and the presence of white or yellow pus. The most common types of infections that can trigger an eczema flare-up include Staphylococcus aureus, or a staph infection, the molluscum virus, the herpes virus, and certain types of fungus, such as ringworm or athlete's foot. When skin becomes infected, see a doctor to determine the best course of treatment.
Stress

Stress and anxiety affect immune response and are a proven association with an increase in eczema symptoms. Try to reduce stress whenever possible by using meditation, yoga, or mindfulness techniques. Try to simplify daily routines and schedules as eczema itself can be a cause of stress because it interferes with sleep and causes daily frustration and embarrassment for patients. Patients who work with their doctor to pinpoint the factors which trigger their eczema feel like they have more control over their condition and can find relief from stress.
Hormones

Hormones are chemical properties that naturally occur within the body that can significantly worsen eczema symptoms. Whether the levels of specific hormones increase or decrease in the body, some individuals, especially women, may experience eczema flare-ups. Women can experience increased eczema symptoms when their hormone levels change, especially during their menstrual cycle or during pregnancy.
As previously mentioned, stress happens and can definitely inflame and irritate symptoms of eczema. Cortisol is a naturally occurring hormone that is known as the ‘stress hormone.’ When there is too much cortisol coursing throughout the body, symptoms of numerous conditions can be triggered, including eczema. Hormones and stress are not a direct cause of eczema, but worsen symptoms and often cause the patient to scratch excessively due to these spikes in hormone levels.
Sweat
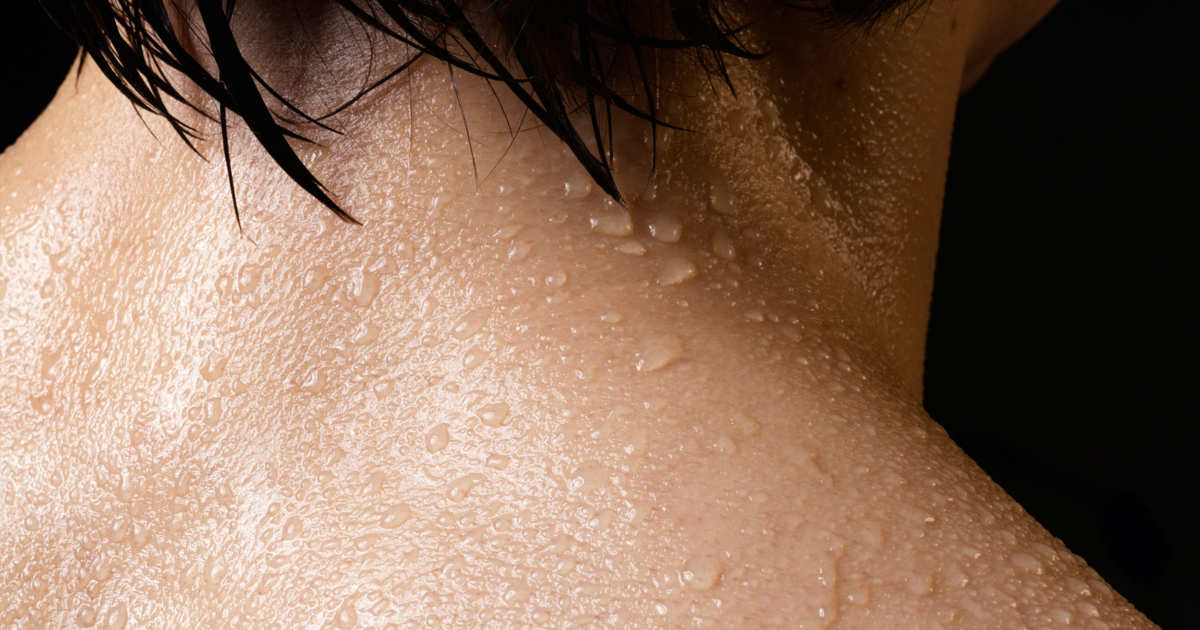
Depending on the severity of eczema, some patients struggle with sweat and climate changes that can cause it, especially during the sweltering months of summer, or even in the middle of a harsh winter from wearing multiple layers of clothing or during a ‘cold sweat.’ Many individuals become itchy or experience a ‘prickly heat’ sensation when they get too hot or begin to sweat, which is often caused by the climate, exercise, or when a person wears too many layers of clothing (especially to bed). An eczema flare-up can also occur when the air is too dry or too humid, which can result in sweating, or if an individual takes long, hot showers or baths.
The simplest way to try and reduce sweating from occurring or causing a flare-up is to wipe up any excess sweat that is noticed on the body, applying lotion or a moisturizer to the affected area, and to try and be conscious of their environment by not under or over-layering their clothing to reduce the chances of excessive sweating.
Primary Causes

Now that you know all the main triggers that can cause an eczema flare-up, why not learn what actually causes this autoimmune disorder to try and further prevent flare-ups from occurring?The truth is, many doctors are not exactly sure what causes eczema to occur in some individuals. The most common type of eczema, atopic dermatitis, resembles an allergy but is not an allergic reaction. Through further research, many medical professionals are beginning to think that eczema is caused by a variety of factors that include genetics, the environment, abnormal function of the immune system, activities that cause the skin to become more sensitive, and defects in the skin’s barrier that doesn’t allow moisturize to be properly absorbed and lets infectious germs in.
