Treatment Options For A Port-Wine Stain
A port-wine stain is a birthmark that develops due to swollen blood vessels. The prevalence of port-wine stains is approximately one in every three hundred births. While they can occur anywhere on the body, the stains typically form on the neck, scalp, face, arms, and legs, and they grow in proportion to the child's growth. Port-wine stains start as light pink, and they tend to darken as the child gets older. Initially smooth in texture, they may become thicker once the child is an adult. Port-wine stains are not preventable, and they are not caused by anything that occurred while the baby was in the womb. Like other birthmarks, port-wine stains can usually be diagnosed with a visual inspection. A child who has a port-wine stain on the forehead or near the eye will need to be closely monitored. In rare cases, a port-wine stain could be associated with Sturge-Weber syndrome, a condition that may cause seizures and developmental delays. Due to an increased risk of glaucoma (elevated eye pressure), doctors generally recommend treatment for port-wine stains located near the eyelids. Patients may also choose to have treatment for cosmetic reasons.
The treatment options for port-wine stains are outlined below.
Use A Quality Moisturizer

Port-wine stains tend to feel very dry, and it is often beneficial to use a quality moisturizer on the affected area. For maximum comfort, patients may want to apply a moisturizer at least once or twice a day. Lighter moisturizers can be useful in the summer, and heavier ones are ideal for winter. When selecting a moisturizer, patients may want to choose one designed for sensitive skin to avoid any irritation. Choosing products with natural ingredients free of parabens and sulfates is also recommended. Before using a new moisturizer, doctors recommend performing a patch test on a small area of skin. A small amount of the product should be applied to the inside of the wrist, and the patient should examine the area after twenty-four hours. If the area looks dry, red, or otherwise irritated, the product should not be applied to the port-wine stain. Patients having difficulty finding a moisturizer that works for their birthmark may want to ask a dermatologist for advice.
Continue reading to reveal more options for treating a port-wine stain now.
Pulsed Dye Laser Treatment
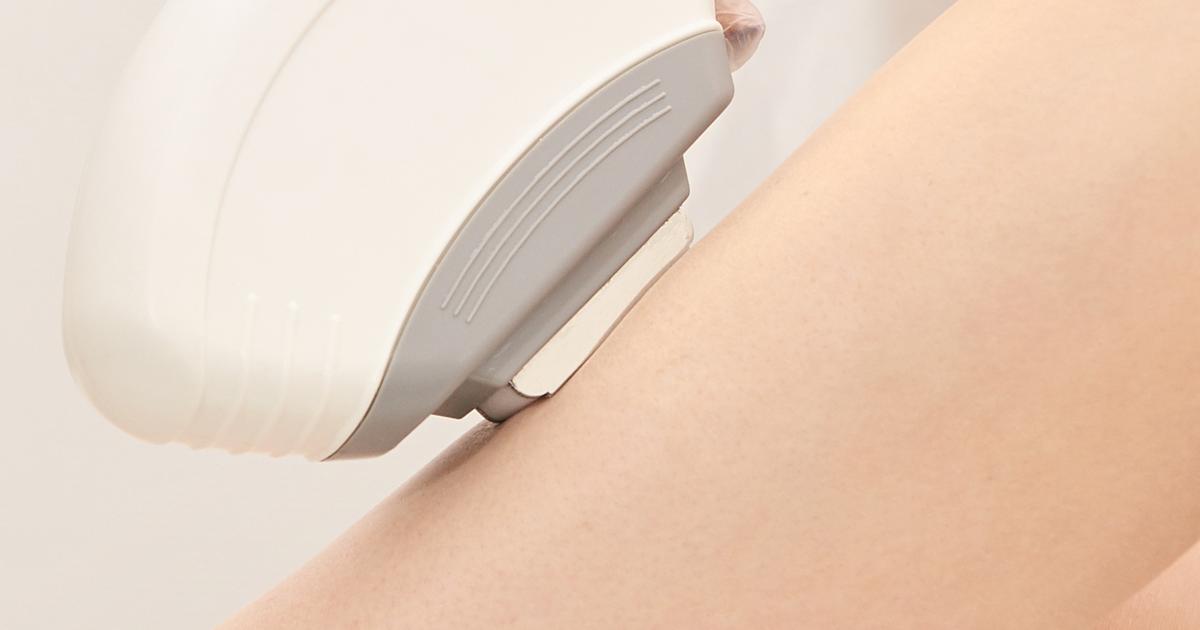
First developed in the 1980s, pulsed dye laser treatment is typically the preferred method for the removal of a port-wine stain. Tiny laser beams are fired at the blood vessels in the affected area, and this causes the vessels to seal. Most patients need six sessions of pulse dye laser treatment over a year, and the treatment has a success rate of more than seventy-five percent. While successful treatment initially makes the port-wine stain significantly lighter, the skin in the affected area could occasionally return to a darker color after ten years. The highest success rates with pulsed dye laser are seen when it is used on pale pink port-wine stains, usually very early in a child's life. As the stains darken to purple with age, this form of laser treatment is less successful.
Uncover more treatments for a port-wine stain now.
Cover Up The Affected Area

Instead of removing the birthmark, some patients may choose to cover up the affected area with camouflage cream. These creams can be helpful in cases where a patient has not completed or has not responded to laser treatment, and they are also useful in instances where the patient desires a bit more coverage than normal makeup can provide. Camouflage creams are designed in waterproof formulations, and some are now available at specialty makeup stores. Dermatologists can help patients with finding the most effective makeup for their needs, and numerous shades can be matched precisely to the patient's skin tone. Patients may need to try several types of camouflage creams before they find one that works for their skin, and they might need to blend several different kinds of concealers. Many formulas provide coverage for at least twelve to twenty-four hours, and they can be easily removed at nighttime with a cleanser or an oil-based makeup remover.
Discover additional ways to treat a port-wine stain now.
Surgery
If laser treatment is unsuccessful in treating a port-wine stain, surgery could sometimes be considered. However, many doctors prefer to use laser treatments, and surgery is only used as a last resort. Patients typically have their surgery performed by a plastic surgeon or dermatologist, and general or local anesthesia may be used. Before the surgery, the patient will have a pre-op appointment to check their general health. Doctors may perform blood tests or an electrocardiogram at this appointment, and the surgeon will explain the risks of the procedure, including bleeding and scarring. Most surgeries for port-wine stains can be performed on an outpatient basis. After the procedure, patients will need to have the dressings on the area changed regularly, and they will need to monitor the site for any excessive bleeding or infection. Follow-up appointments will be scheduled in the week or so after the surgery.
Read more about effectively treating port-wine stains now.
Other Laser Treatments
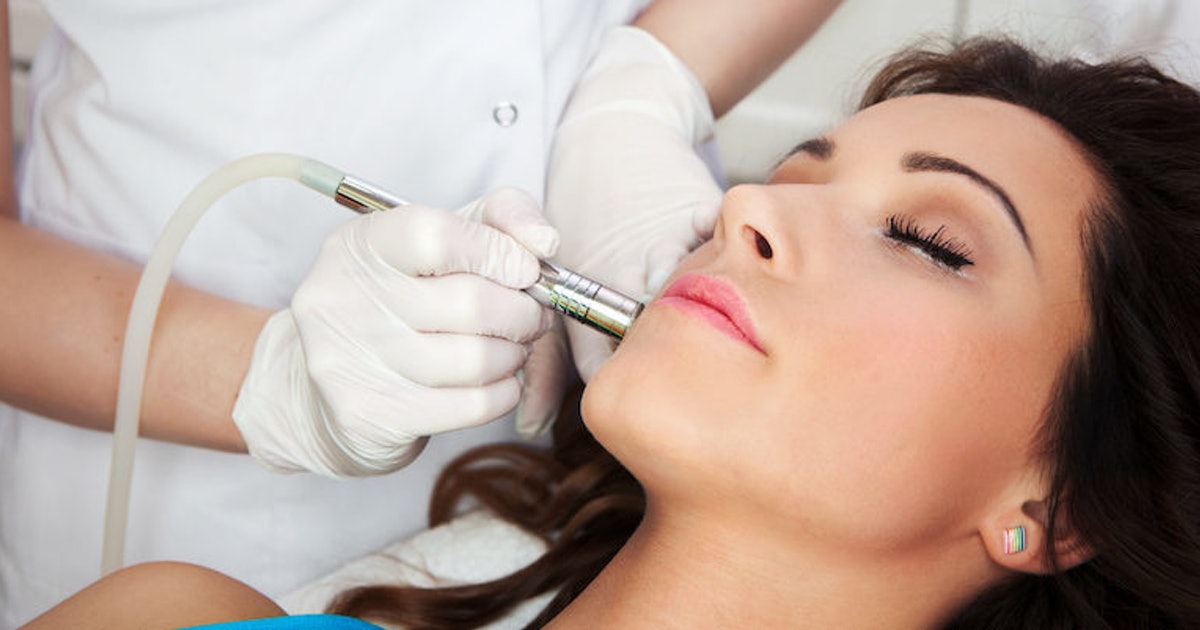
Depending on the location and specific characteristics of a patient's port-wine stain, doctors might recommend other laser treatments instead of pulsed dye laser therapy. Sometimes, other laser treatments might also be combined with pulsed dye lasers. A combination of laser therapy types could be most appropriate for the treatment of mature port-wine stains that are dark purple or lumpy. To reach the thicker areas of a mature port-wine stain, some dermatologists use 532 nm lasers or alexandrite lasers in conjunction with pulsed dye lasers. 532 nm lasers are diode-pumped solid-state lasers, and alexandrite lasers are a type of red light laser. Patients may want to ask several different dermatologists about the types of laser treatments that could be effective for their needs. After undergoing any type of laser treatment, patients should remain vigilant for potential side effects, and these should be reported promptly to the treatment provider.
