Comprehensive Causes And Risk Factors For Blind Loop Syndrome
When digested food stops moving or considerably slows down through a region of the intestines, the condition is called blind loop syndrome. This results in a bacteria overgrowth in the intestines and causes the body to have difficulty with absorbing nutrients. In blind loop syndrome, the affected part of the intestine is unable to absorb fat and fat-soluble vitamins because the bile salts or the substances required to digest fats do not work correctly. This causes the individual to have excessive fatty stools and a vitamin B12 deficiency. Medical imaging tests such as a CT scan and X-rays are commonly used to diagnose blind loop syndrome. Treatment for blind loop syndrome will most often begin with treating the excess growth of bacteria with antibiotics. If that measure proves ineffective, a surgical procedure may be required to restore the flow of food through the intestines.
There are several causes and risk factors for blind loop syndrome. Learn about them now.
Small Intestine Region Structural Issues
Small intestine region structural issues can cause an individual to develop blind loop syndrome. These types of anatomical abnormalities can be congenital, develop over several years, or could be the result of an abdominal injury. One common structural issue that leads to blind loop syndrome is called diverticulosis. Diverticulosis is when the inner layer of the intestine pushes through vulnerable or weak areas in the intestine's outer lining, which results in little pouches called diverticula that bulge out of the intestine and obstruct the normal flow of food. Another structural issue that can result in blind loop syndrome is jejunal atresia, which is a congenital condition where the membrane connecting the intestines to the abdominal wall is deformed or missing. This often causes the intestines to become displaced to where food is unable to flow through them properly. Gastroschisis is another structural congenital condition that can result in the development of blind loop syndrome. It is a herniated section of intestine that appears on the outside abdominal surface because the abdominal cavity is too small and not covered with a membranous sac. The herniated organs have to be placed back into the abdomen surgically and can result in complications like blind loop syndrome.
Learn more about the causes and risk factors for blind loop syndrome now.
Abdominal Surgery Complications
The development of blind loop syndrome can be triggered by abdominal surgery complications. Most often, these surgical procedures are of the bariatric variation or for the purpose of achieving weight loss. The bariatric procedure that interferes the most with the function and normal flow of food through the intestines is called a gastric bypass. A gastric bypass procedure creates a smaller stomach pouch that bypasses or goes around the first third of the small intestine. While gastric bypass surgery is successful in terms of helping with weight loss, it can easily impair the normal absorption of nutrients and disrupt the flow of food through the digestive tract, both of which can trigger blind loop syndrome. This blind loop can also develop from complications that happen due to surgical procedures that shorten the gastrointestinal tract to treat diseases that affect the intestines and their function. This includes surgery to treat certain kinds of cancers, bowel obstructions, Crohn's disease, ulcerative colitis, diverticular disease, intestinal polyps, bowel twisting, and nerve problems in the intestines.
Uncover more details on the risk factors and causes of blind loop syndrome now.
Scleroderma
An individual who has a disorder called scleroderma is at an increased risk of developing blind loop syndrome. Scleroderma is best described as a group of disorders where the connective tissues and the skin abnormally tighten and harden. It is a progressive, long-term disease that gets gradually worsens. In individuals who have this disease, the immune system attacks its own connective tissues resulting in an excessive collagen overproduction. This causes fibrosis or thick scarring of the tissues. The digestive system is the second most commonly affected system in scleroderma patients. A major complication of this disease is problems with proper dilation and relaxation of blood vessels. As a result, organs and nerves in the digestive system often end up with an insufficient supply of blood. The poor blood supply leads to less mechanical movement and progressive weakening of the muscles that stimulate digestive tract movement. Consequently, food is not propelled properly throughout the gastrointestinal system. The food then stagnates or completely stops at some point in the intestines, and this can trigger blind loop syndrome.
Discover more causes and risk factors for blind loop syndrome now.
Fistulas In The Bowels

An individual with fistulas in the bowels is at an elevated risk for developing blind loop syndrome. A fistula is a term describing an irregular connection between two separate epithelial superficies that allows for their contents to leak between them. The bowel can be connected through a fistula in the gut or intestine to the bladder, vagina, urethra, abdominal membranous sac, and the skin. Fistulas can develop as a complication from Crohn's disease, cancer, pancreatitis, and peptic ulcer disease. Fistulas can also be a result of an injury or trauma to the abdominal region. Fistulas result in what should be the normal flow of food through the intestines to bypass the portion of the bowel that follows the fistula. This can easily result in the manifestation and uninhibited growth of bacteria in the intestine and subsequent development of blind loop syndrome. The risk of developing blind loop syndrome has a compounding effect with every additional fistula present in the gastrointestinal tract after the initial one.
Get the details on more blind loop syndrome risk factors and causes now.
Abdominal Radiation Therapy
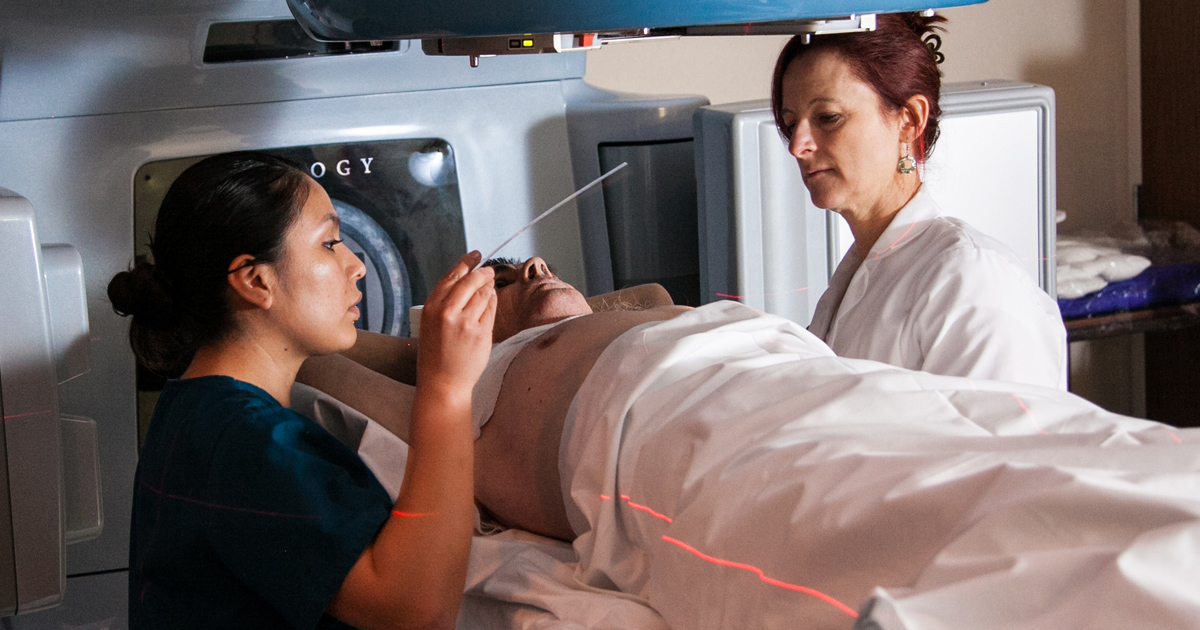
Patients undergoing abdominal radiation therapy to treat cancer or other diseases are at an increased risk of developing blind loop syndrome. Radiation therapy is the use of precisely positioned high-energy beams that cause damage to cancerous or other problematic cells, making it difficult for them to reproduce. While radiation is very helpful in the eradication of cancers and other diseases, it also has adverse effects on healthy cells surrounding the treatment area. When radiation therapy is being applied to the abdominal region, it can cause the sensitive mucosal cells of the esophagus, stomach, and small intestine to become inflamed. Swelling often occurs along with the tissue inflammation due to acute mucosal injury. This can slow the movement of food through the small intestine, and it allows for bacterial overgrowth from a production shortage of bile salt and digestive enzymes. The risk of developing blind loop syndrome increases because of the favorable environment for bacteria to fester formed by radiation therapy.
