Treatment Options For Gastroparesis
In the United States, it is estimated over 1.5 million individuals have gastroparesis, also called delayed gastric emptying. Approximately 100,000 patients have severe symptoms. Gastroparesis is characterized by food moving abnormally slow through the stomach, which can result in chronic, severe vomiting, fullness, abdominal pain, nausea, bloating, and early satiety. Since eating can be very uncomfortable, patients may purposely reduce their food intake to find relief from symptoms, which could result in malnutrition.
Other possible complications include severe dehydration, worsening of diabetes, and food becoming hard masses, resulting in vomiting, nausea, and stomach obstruction. This condition is incurable, but there are treatment options to help alleviate the symptoms to help patients live more comfortably.
Changes To Diet

One of the first and most important treatments for this condition is changes to diet. In many cases, the right dietary changes are enough to help keep the patient's symptoms under control. General recommendations include eating more often, but making meals smaller, avoiding carbonated drinks, considering liquid foods when solid foods are especially irritating, and reducing dietary fat and fiber intake. Vegetables and fruits should be cooked very well or ran through a juicer when possible. This allows patients to get critical nutrients but reduces fiber, so these foods are easier to digest.
Every day, drink one to one and a half liters of water to reduce the risk of dehydration. After eating, gentle exercise is often beneficial to encourage digestion, and it is also important patients do not lie down for approximately two hours after they finish eating. Lastly, doctors might recommend a high-quality multivitamin to reduce malnutrition risk. Doctors often recommend patients work with a nutritionist or dietitian for the dietary changes.
Medications

Gastroparesis may respond to several drugs to reduce the impact this condition has on patient's lives, however, it is important to note it may take some trial and error to see which drugs are most effective in individual cases. For some patients, more than one medication may be needed to decrease their symptoms. Metoclopramide may be prescribed to help stomach emptying and to encourage muscle contractions in the stomach, and it might also be helpful for alleviating vomiting and nausea.
Erythromycin is an antibiotic, but it may be used to help patients with gastroparesis due to its ability to promote stomach emptying, which it does by increasing stomach muscle contractions. If patients have certain especially bothersome symptoms or complications associated with this condition, medications that target these may be prescribed. For example, for vomiting and nausea, patients might benefit from an antiemetic medication. Medicines may also be injected via endoscopy if the patient has a bezoar in their stomach due to food building up and creating an obstruction.
Surgical Intervention
If the cause of this condition is due to a vagus nerve injury, doctors may suggest surgical intervention in the form of a pyloroplasty. Between the small intestine's duodenum and the stomach's pylorus is the pyloric sphincter, which acts as a valve that controls how much food flows between these two digestive system components. The vagus nerve plays a role in this valve's function, so damage to it can interfere with the stomach muscles' ability to contract efficiently. This surgical procedure allows faster stomach emptying by relaxing and widening the pyloric sphincter.
To see if the patient may benefit from this surgery, the doctor might first inject the sphincter with Botox to relax and paralyze it temporarily. If this injection does help to improve the patient's symptoms, there is a strong chance pyloroplasty will be effective in alleviating their gastroparesis symptoms over the long term. This procedure can be done laparoscopically or as open surgery.
Gastric Electrical Stimulation

Food moving significantly slowly through the stomach is what causes gastroparesis symptoms but stimulating the stomach muscles may allow food to move more efficiently through the stomach and into the small intestine. With this treatment option, patients receive a device implanted into their body, which is what stimulates the muscles. For most individuals who have this condition due to diabetes, this treatment appears to be beneficial even though studies show mixed results.
While larger studies are necessary, the Food and Drug Administration does let doctors implant this device using the exemption for compassionate use. However, only patients who have severe symptoms uncontrolled by medications or diet changes usually qualify. A similar device, called gastric pacing, is currently in the clinical trial phase. The general premise is the same as it also stimulates the stomach muscles, but researchers hope the contractions it produces will be closer to normal stomach contractions compared to gastric electrical stimulation.
Tube Feeding

Patients who are unable to tolerate liquids or food by mouth may benefit from a feeding tube. The tube is plastic and soft, so doctors place it into the small intestine's midsection through the abdominal skin. This type is referred to as a jejunostomy tube since it is inserted into the jejunum component of the small intestine. If gastric contents are causing pressure to accumulate in the stomach, gastric tube venting may be recommended to alleviate pressure. In some cases, feeding tubes may be passed into the small intestine via the mouth or nose.
When this treatment method is used, it is typically only temporary. Doctors might recommend it if the patient's blood sugar cannot be controlled any other way or when their symptoms are especially severe. One other option is an intravenous tube placed directly into a chest vein. This is typically reserved as a last resort if all other tube feeding options do not benefit the patient.
More Intravenous Feeding
One of the potential treatments for gastroparesis is called total parenteral nutrition, which is a method of supplying the body with all nutritional needs by going around the digestive system and intravenously feeding a nutrient solution into an individual's vein. Intravenous feeding is recommended for patients who can't get nutrition through eating.
These circumstances include patients with obstructed intestines, small intestines that cannot absorb nutrients, or digestive systems with abnormal connections. It can also be used in cases where an individual's bowels must rest and not have food moving through them. In patients with gastroparesis, total parenteral nutrition is used on a more permanent basis because their digestive systems can't properly break down food.
Venting Gastrostomy
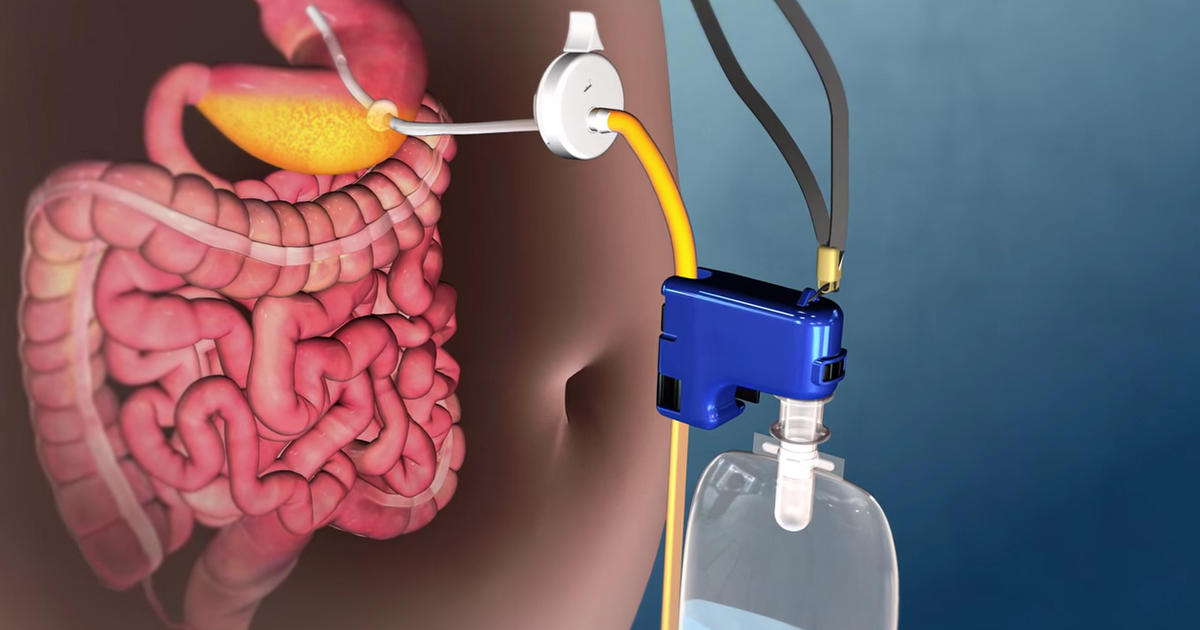
Gastrostomy tubes are tubes used to provide nutritional support. They are the preferred method of helping patients with functional guts take in nutrition if they cannot eat for more than a few weeks. For patients who have mechanical bowel obstruction, a venting enterogastrostomy is used to decompress the bowel and alleviate the symptoms. Gastrostomy tubes are sometimes used for patients who have inoperable and cancerous obstructions of the esophagus and have undergone a failed stent placement. Venting gastrostomy is always used for decompression of cancerous bowel obstructions. Gastrostomy tubes will be placed radiologically or endoscopically while the patient is consciously sedated.
Managing Blood Sugar

Managing blood sugar is an important part of managing type 1 and type 2 diabetes, and it becomes even more important when gastroparesis is in play. With gastroparesis, the stomach is delayed in emptying its contents. The condition tends to have a certain level of unpredictability, which can make it difficult to maintain blood sugar. If food sits in the stomach for too long, there may be a dip in blood sugar akin to a missed meal. But if food is unexpectedly digested in a timely manner, the sugar spike can be equally dangerous. Blood sugar can be managed through dietary changes, oral medications, and insulin. Intravenous feeding and feeding tubes are reserved for extreme cases where blood sugar is uncontrollable due to the digestive system's slowness and unpredictability.
Other Underlying Condition Treatment

Sometimes, gastroparesis presents without an underlying condition that doctors can find. In these cases, it's called idiopathic gastroparesis. The most common cause of the condition is diabetes, a disease that causes the body to be unable to process glucose properly. Untreated diabetes can lead to nerve damage. There are important nerves in the stomach called the vagus nerve and associated special cells. These control the movement of stomach muscles and overall digestive process.
If diabetes damages the vagus nerve, it won't be able to function fully, which leads to delays in digestion. Other potential underlying causes of gastroparesis are hypothyroidism, autoimmune diseases like scleroderma, nervous system disorders like multiple sclerosis and Parkinson's disease, viral infections in the stomach, and injuries to the vagus nerve related to digestive system surgery.
