Can Immunotherapy Treat Other Conditions?
Immunotherapy is a term commonly used in reference to a type of treatment utilized to fight cancer. However, immunotherapy encompasses any manipulation of an individual's immune system to fight or treat disease. The immune system is designed to help defend the body against pathogen invasion, and other harmful substances. Some individuals have an abnormal immune system that reacts to its own body tissues and causes harm. This malfunction can cause a number of conditions that can be described using the umbrella term of autoimmune disorders.
These disorders are classified according to the body tissues they affect. Autoimmune disorders can be challenging to treat, often requiring the use of numerous methods to mediate several systemic symptoms that occur simultaneously. Immunotherapy methods have proven to be helpful in the treatment of several common immune conditions when traditional methods are ineffective.
What Is Immunotherapy?
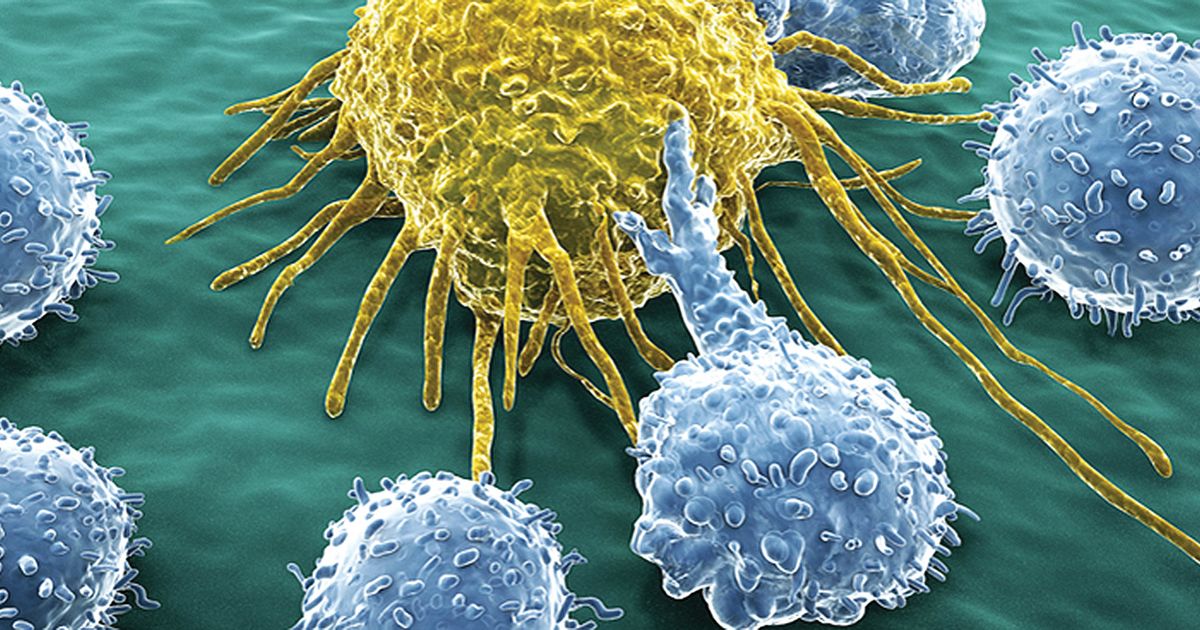
Immunotherapy, by definition, is the utilization of certain characteristics and components of the complex human immune system to treat disease. Immunotherapy can be categorized in several ways. Activation therapies stimulate the immune system activity to fight off diseases such as cancer, while suppression therapies reduce the overactive immune activities to help control autoimmune conditions. Additionally, immunotherapy can be used in the prevention of organ rejection in patients who have received an organ transplant.
Suppression immunotherapy works by reducing the effects of the immune response within a patient's body. This goal can be accomplished by numerous methods that involve reducing the production or action of a certain targeted component of the immune system. This process has been done in several ways, including by the removal and manipulation of cells for the purpose of programming them to target and kill other harmful immune cells.
Rheumatoid Arthritis
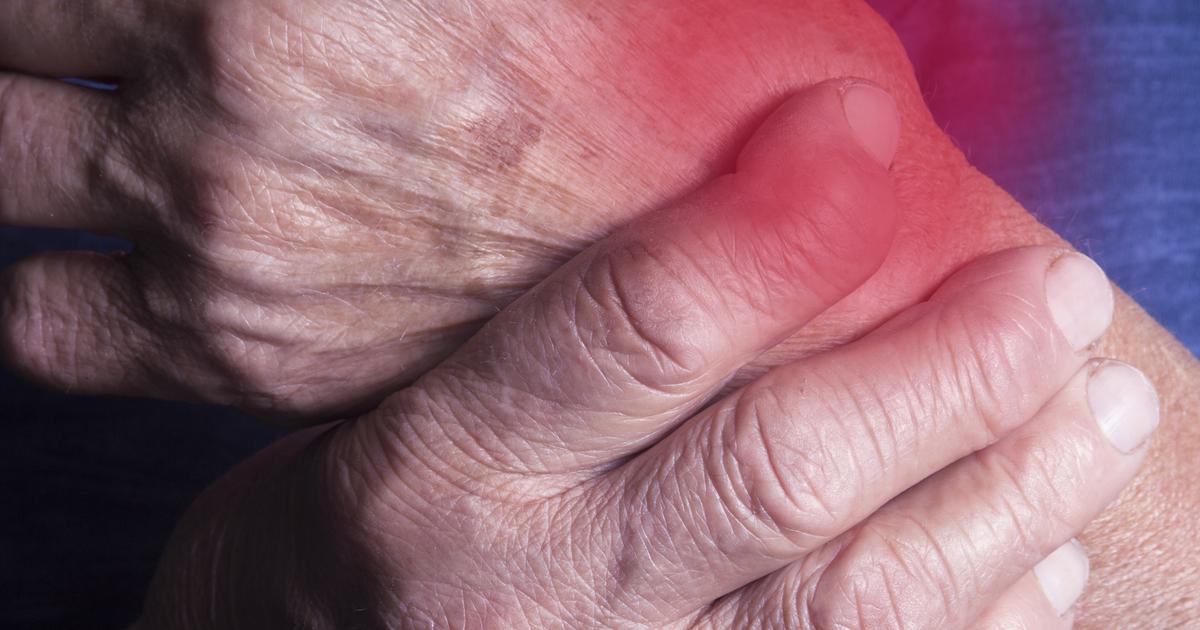
Rheumatoid arthritis is a debilitating inflammatory disorder where the patient's immune system attacks a variety of systems in the body, including the joints, skin, eyes, lungs, blood vessels, and heart. The lining of the joints is one of the most commonly affected areas of the body by rheumatoid arthritis. The immune system attacks the cells in the joint lining, resulting in swelling that can cause joint deformity, severe pain, and bone erosion. While traditional treatments such as non-steroidal anti-inflammatory medications can help with inflammation initially, they do not stop the disease from worsening. If NSAIDs are ineffective, steroids may be used to help slow down the rheumatoid arthritis progression.
When these options are ineffective, an affected individual may need immunotherapy. Immunotherapy treatments for rheumatoid arthritis patients work by interrupting the immune responses that cause their joint inflammation. Biological response modifiers are a natural part of the immune system utilized to treat rheumatoid arthritis. These response modifiers are produced in large portions in a laboratory, and they are placed back into the individual's body. These modifiers then help target the T-cells and a protein called interleukin-1 that are the critical factors associated with rheumatoid arthritis inflammation.
Multiple Sclerosis

Multiple sclerosis is a disease that affects an individual's central nervous system or their brain, spinal cord, and associated nerves. Multiple sclerosis is considered an autoimmune disease because it is a result of the patient's immune system attacking the protective myelin sheath that covers their nerve fibers. This malfunction causes difficulty with nerve communications, widespread nerve damage, and deterioration of the nerves. Treatment aims at reducing the frequency of multiple sclerosis flare-ups and attempting to slow the progression of the disease. Immunotherapy has proven useful for multiple sclerosis patients through a number of mechanisms. Laboratory manipulation of activated T-cells can stop them from commanding immune system macrophages to attack the central nervous system.
Laboratory manipulation of class II major histocompatibility complex-bearing cells can prevent the immune system from tagging its own nerve tissues for immune cell attack. Disruption of immune lymphocyte traffic can stop lymphocytes from reaching their target nerves. Manual removal of immune white blood cells and other serum factors through a machine outside of the body can reduce the inflammatory response on the myelin sheathing. Additionally, laboratory manipulation of antigen-specific cells can reduce the production of antibodies that also attack the central nervous system of an individual with multiple sclerosis.
Other Immune Conditions
Inflammatory bowel disease is among the other immune conditions that can be treated with the use of immunotherapy. Crohn's disease and ulcerative colitis are forms of inflammatory bowel disease where the patient's immune system incorrectly targets and attacks the digestive system lining. This malfunction causes inflammation characterized by debilitating pain and severe diarrhea. Because the immune system abnormalities associated with inflammatory bowel disease have been identified, the immune system can be modulated in several ways to reduce its attacks on the digestive system lining.
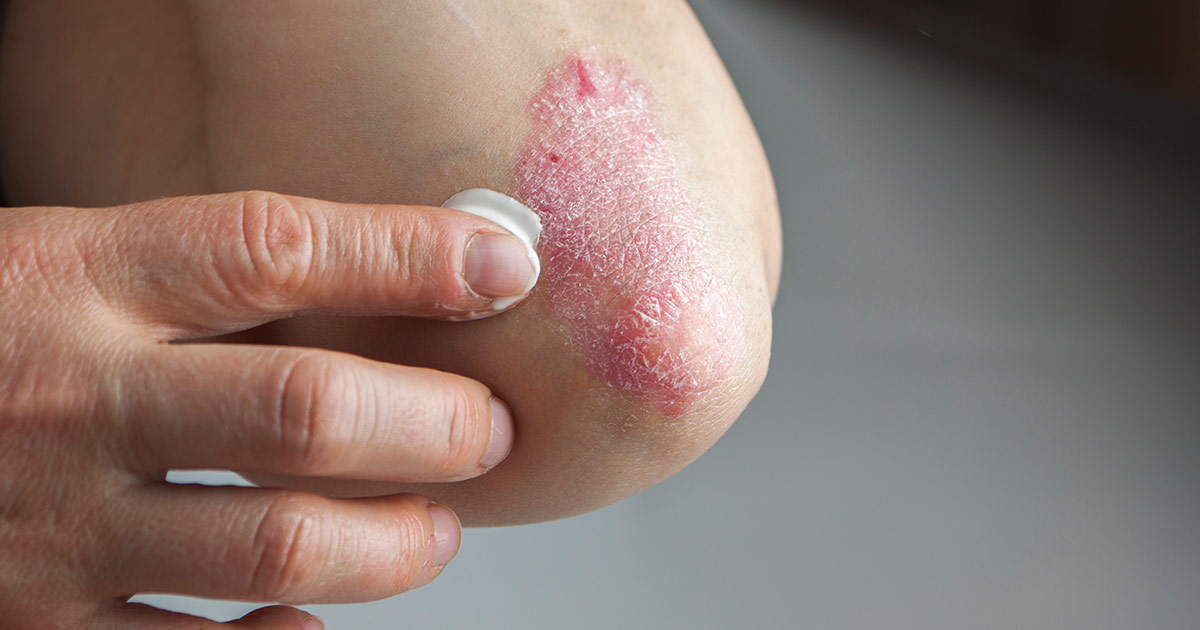
Psoriasis is another inflammatory disease that has been treated with the use of immunotherapy. Psoriasis occurs when the patient's immune system attacks healthy cells of the skin. This malfunction causes an overproduction of skin cells and white blood cells that result in scaly hard skin lesions. Immunotherapy for psoriasis involves the use of the immune system to target the particular inflammatory cytokines abnormally upregulated in individuals affected by psoriasis.
Ongoing Clinical Trials
Ongoing clinical trials for immunotherapy can be helpful to individuals who have tried treatment methods that have been unsuccessful or ineffective. Clinical trials for individuals affected by type 1 diabetes are in progress to try and inhibit the immune system destruction of beta cells or cells that produce insulin. Clinical trials are also ongoing for methods that use a vaccine on individuals who are at a high risk of diabetes to signal the immune system to neutralize the interferon alpha protein that stimulates the production of immune components that attack the beta cells.
Another clinical trial for immunotherapy to fight diabetes is trying to utilize a type of bacteria to signal lymphoid tissues to restore beta cell tolerance in affected individuals. Clinical trials are being conducted for autoimmune encephalitis patients to stop the immune cells from attacking healthy cells in the brain. In addition, an ongoing clinical trial is underway for individuals affected by myasthenia gravis, an autoimmune disease that results in widespread skeletal muscle weakness. The trial aims to stop the production of antibodies that target the neurotransmitter receptor sites.
