Effective Ways To Treat Thymoma
The thymus gland is responsible for maintaining the body's supply of healthy T-cells, which are vital in our ability to fight off viruses, bacteria, and fungi. In rare instances, a tumor can form in the thymus gland and inhibit its ability to function. In most cases, the tumor remains confined to the thymus gland, but, although it may not spread to other organs, it can do plenty of damage. By affecting the development of T-cells, thymoma can interfere with the immune system's ability to fight off disease. The thymus gland is most active in children and through adolescence, shrinking as we age, but anyone can be affected by a thymoma. Although only one person out of every 1.5 million individuals will develop a thymoma, it is still worthwhile to know the typical treatments for this condition.
Tumor Removal
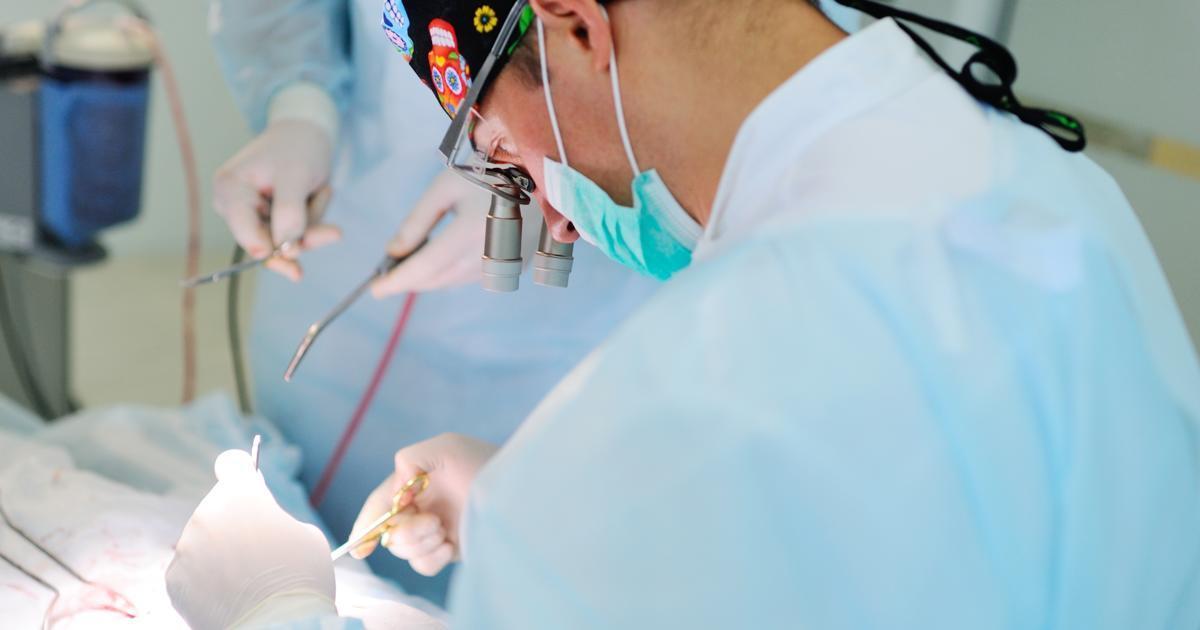
One of the most common treatments for thymoma is the surgical removal of the tumor, which is typically performed by a thoracic surgeon. The procedure involves cutting away the tumor, though some of the surrounding healthy tissue is usually removed as well. This is usually done for early-stage cases of thymoma when the tumor is still small. In these cases, the individual will likely not need to undergo additional treatment. By cutting away the surrounding healthy tissue, the surgeon ensures the tumor has been completely removed, leaving a minimal chance that the tumor will return. In late-stage thymomas, the tumor has grown larger and may have spread to the lungs. In these cases, the surgeon may have to remove a section of the lung as well, and it may not be possible to remove the entire tumor. If this is the case, the surgeon will discuss this with the patient and explain what symptoms may be alleviated through removing a part of the tumor. Even in these cases, surgery is often the preferred method of treatment.
Keep reading to learn about the next method used for treating thymoma now.
Radiation Therapy
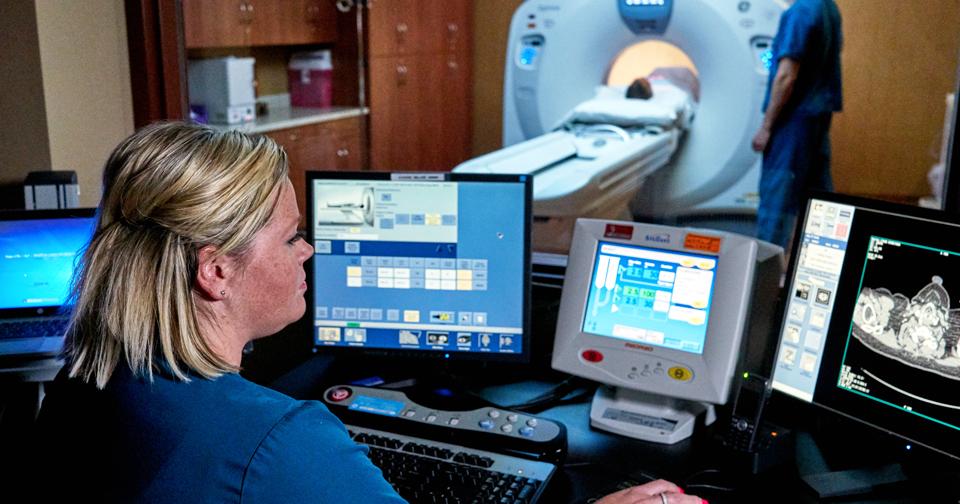
Another treatment option for thymoma is radiation therapy, which involves attacking the tumor with high-potency energy X-rays. This type of procedure is done by a specialist called a radiation oncologist, because it requires focusing an external machine at the tumor within the thymus. This procedure, which is called external-beam therapy, involves administering many radiation treatments over an extended period. Multiple treatments are necessary for maximum effectiveness.
Typically, radiation is used in conjunction with another treatment. For instance, if a surgical procedure failed to remove all of the tumor, radiation therapy may be used to finish eradicating the tumor. Similarly, radiation treatments may be necessary to supplement chemotherapy, depending on the nature of the tumor. Radiation often affects patients and doctors warn them ahead of time that side effects may become severe. The side effects include watery or loose stool, an upset or unsettled stomach, skin rashes, difficulty in breathing, and unexplained fatigue. While these side effects may be troublesome, they're only temporary and often fade as soon as treatment has been completed.
Uncover the next treatment option for thymoma now.
