15 Best Blood Pressure Monitors for Home Use — Ranked for 2026
In an era where cardiovascular disease remains the leading cause of death globally, affecting over 655 million people worldwide, the ability to monitor blood pressure accurately at home has become more crucial than ever before. The American Heart Association now strongly recommends home blood pressure monitoring as an essential component of comprehensive cardiovascular care, recognizing that clinical readings often fail to capture the complete picture of a patient's blood pressure patterns throughout daily life. White coat hypertension, masked hypertension, and the natural fluctuations in blood pressure that occur throughout the day can only be properly assessed through consistent home monitoring. As we advance into 2026, technological innovations have revolutionized home blood pressure monitors, introducing features like smartphone connectivity, cloud-based data storage, irregular heartbeat detection, and advanced averaging algorithms that provide healthcare professionals with unprecedented insights into their patients' cardiovascular health. This comprehensive ranking of the 15 best blood pressure monitors for home use in 2026 evaluates each device based on accuracy validated against clinical standards, ease of use for patients of all ages, technological features that enhance monitoring compliance, durability for long-term use, and overall value proposition in supporting proactive cardiovascular health management.
1. Understanding Blood Pressure Fundamentals and Why Accurate Measurement Matters

Blood pressure measurement represents one of the most fundamental vital signs in healthcare, consisting of two critical components: systolic pressure (the force exerted when the heart contracts) and diastolic pressure (the pressure when the heart relaxes between beats). Normal blood pressure typically falls below 120/80 mmHg, while readings consistently above 130/80 mmHg indicate hypertension, a condition that silently damages arteries, increases stroke risk, and places tremendous strain on the cardiovascular system. The accuracy of home blood pressure measurements directly impacts treatment decisions, medication adjustments, and long-term health outcomes, making the selection of a reliable monitor absolutely critical. Studies have demonstrated that even small measurement errors of 5-10 mmHg can lead to misclassification of hypertension status in up to 20% of patients, potentially resulting in inappropriate treatment or missed opportunities for early intervention. Modern home monitors utilize oscillometric technology, which detects pressure oscillations in the arterial wall as the cuff deflates, providing automated readings that eliminate human error associated with manual auscultation methods. Understanding these fundamentals helps consumers appreciate why investing in a high-quality, clinically validated blood pressure monitor represents one of the most important health decisions they can make for long-term cardiovascular wellness.
2. Clinical Validation Standards and Accuracy Requirements for Home Monitors

The gold standard for blood pressure monitor validation involves rigorous testing protocols established by organizations such as the British Hypertension Society (BHS), the Association for the Advancement of Medical Instrumentation (AAMI), and the European Society of Hypertension (ESH). These protocols require monitors to demonstrate accuracy within 5 mmHg for at least 50% of readings and within 10 mmHg for at least 85% of readings when compared to mercury sphygmomanometry performed by trained professionals. The validation process involves testing on diverse populations including individuals with different arm circumferences, various blood pressure ranges, and specific conditions like atrial fibrillation or diabetes that can affect measurement accuracy. In 2026, the most advanced home monitors have undergone multiple validation studies, including real-world effectiveness trials that assess performance in typical home environments rather than controlled clinical settings. Additionally, newer validation protocols specifically address the accuracy of monitors in detecting irregular heartbeats, a feature that has become increasingly important as the prevalence of atrial fibrillation continues to rise with an aging population. Consumers should prioritize monitors that display validation seals from recognized organizations and have published peer-reviewed studies demonstrating their accuracy across diverse patient populations, ensuring that their home measurements will be reliable enough to guide important healthcare decisions.
3. Technological Innovations Transforming Home Blood Pressure Monitoring in 2026

The landscape of home blood pressure monitoring has been revolutionized by technological innovations that extend far beyond basic measurement capabilities, creating comprehensive cardiovascular health management systems. Bluetooth and Wi-Fi connectivity now enable seamless data transmission to smartphones, tablets, and cloud-based platforms, allowing patients and healthcare providers to track trends, identify patterns, and make informed treatment adjustments based on comprehensive data analysis. Advanced algorithms incorporate artificial intelligence to detect measurement errors, provide personalized recommendations for optimal measurement timing, and even predict potential cardiovascular events based on blood pressure patterns and other health metrics. Smart cuff technology automatically adjusts inflation pressure based on individual arm characteristics, reducing discomfort while ensuring accurate measurements across a wide range of arm sizes. Integration with electronic health records (EHR) systems allows healthcare providers to access real-time patient data during appointments, facilitating more informed clinical decisions and reducing the time spent manually recording measurements. Voice-activated features and large, high-contrast displays accommodate users with visual or dexterity limitations, while multi-user memory capabilities support entire families in maintaining their cardiovascular health. These technological advances have transformed blood pressure monitoring from a simple measurement tool into a comprehensive health management platform that empowers patients to take active control of their cardiovascular wellness.
4. Cuff Design and Sizing: The Foundation of Accurate Measurements
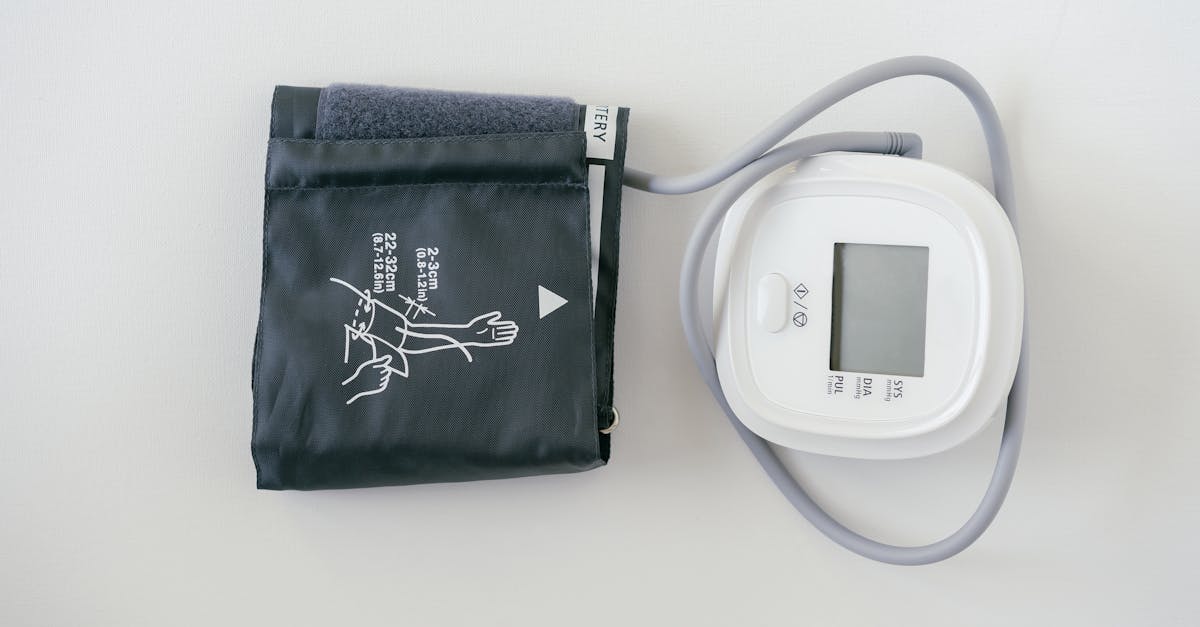
The blood pressure cuff represents the most critical component of any home monitor, as improper cuff sizing or design can lead to measurement errors of 10-40 mmHg, potentially resulting in misdiagnosis or inappropriate treatment decisions. The ideal cuff should encircle 80-100% of the arm circumference, with the inflatable bladder covering at least 80% of the arm's circumference and 40% of its length to ensure even pressure distribution during measurement. In 2026, leading manufacturers have developed innovative cuff designs that accommodate a broader range of arm sizes while maintaining measurement accuracy, including adjustable cuffs with clear sizing indicators and pre-formed shapes that naturally conform to arm anatomy. Advanced cuff materials incorporate breathable fabrics that enhance comfort during extended monitoring sessions, while reinforced construction ensures durability through thousands of inflation cycles. Some premium monitors now feature dual-cuff systems that automatically select the appropriate size based on arm measurements, eliminating user guesswork and ensuring optimal fit for every measurement. The positioning of the cuff relative to the heart level has also been addressed through innovative design features, including built-in positioning guides and smartphone apps that use device cameras to verify proper cuff placement. Understanding the critical importance of proper cuff selection and positioning empowers users to achieve clinical-grade accuracy in their home measurements, making this knowledge essential for anyone serious about cardiovascular health monitoring.
5. Memory Storage and Data Management Capabilities

Modern home blood pressure monitors have evolved into sophisticated data management systems capable of storing thousands of measurements while providing comprehensive analysis tools that transform raw numbers into actionable health insights. The leading monitors of 2026 feature expandable memory systems that can store 2-5 years of daily measurements for multiple users, with advanced sorting capabilities that organize data by date, time, user, and measurement conditions. Cloud-based storage solutions ensure that valuable health data is never lost due to device failure or replacement, while also enabling access from multiple devices and locations for both patients and healthcare providers. Intelligent data analysis features calculate average readings over various time periods, identify trends and patterns that might indicate medication effectiveness or lifestyle impacts, and generate comprehensive reports suitable for sharing with healthcare professionals. Some advanced systems incorporate machine learning algorithms that can detect subtle changes in blood pressure patterns that might indicate emerging health issues, providing early warning systems that could prevent serious cardiovascular events. The ability to annotate measurements with contextual information such as medication timing, stress levels, physical activity, or dietary factors creates a comprehensive health diary that helps identify personal triggers and optimize treatment strategies. These sophisticated data management capabilities transform home blood pressure monitoring from a simple measurement activity into a comprehensive cardiovascular health management system that supports informed decision-making and improved health outcomes.
6. Smartphone Integration and Mobile Health Applications
The integration of blood pressure monitors with smartphone applications has created unprecedented opportunities for comprehensive cardiovascular health management, transforming how patients interact with their health data and communicate with healthcare providers. Leading monitors in 2026 feature dedicated mobile applications that not only receive and store measurement data but also provide personalized insights, medication reminders, and lifestyle recommendations based on individual blood pressure patterns and health goals. These applications utilize advanced analytics to identify correlations between blood pressure readings and various lifestyle factors such as sleep quality, physical activity levels, stress indicators, and dietary choices, empowering users to make informed decisions about their daily habits. Integration with popular health platforms like Apple Health, Google Fit, and Samsung Health creates comprehensive health ecosystems that combine blood pressure data with information from fitness trackers, smart scales, and other connected health devices. Telemedicine capabilities built into these applications enable remote consultations with healthcare providers, allowing for real-time review of blood pressure trends and immediate adjustments to treatment plans without requiring in-person visits. Social features within some applications provide support communities where users can share experiences, challenges, and successes in managing their blood pressure, creating motivation and accountability systems that improve long-term adherence to monitoring routines. The sophisticated smartphone integration available in 2026 represents a paradigm shift toward patient-centered healthcare management that puts comprehensive cardiovascular health information literally at users' fingertips.
7. Irregular Heartbeat Detection and Cardiovascular Risk Assessment

The incorporation of irregular heartbeat detection capabilities in home blood pressure monitors represents a significant advancement in cardiovascular health screening, as atrial fibrillation and other arrhythmias often go undetected during routine medical visits but can be identified through consistent home monitoring. Advanced monitors in 2026 utilize sophisticated algorithms that analyze pulse wave patterns during blood pressure measurement to detect irregularities that may indicate atrial fibrillation, premature ventricular contractions, or other cardiac rhythm abnormalities. These detection systems have been clinically validated against electrocardiogram (ECG) readings and demonstrate sensitivity rates exceeding 95% for identifying clinically significant arrhythmias during blood pressure measurement sessions. The early detection of irregular heartbeats through home monitoring can be life-saving, as undiagnosed atrial fibrillation increases stroke risk by 500% and affects over 6 million Americans, many of whom are unaware of their condition. Some premium monitors now incorporate additional cardiovascular risk assessment tools that analyze pulse wave velocity, arterial stiffness indicators, and other hemodynamic parameters to provide comprehensive cardiovascular health assessments beyond simple blood pressure measurement. Integration with healthcare provider networks enables automatic alerts when irregular heartbeats are detected, facilitating rapid medical evaluation and potential intervention before serious complications develop. The ability to detect and monitor irregular heartbeats through routine blood pressure monitoring represents a significant advancement in preventive cardiovascular care that could prevent thousands of strokes and other serious cardiac events annually.
8. User Interface Design and Accessibility Features

The user interface design of home blood pressure monitors has evolved significantly to accommodate users of all ages, technical abilities, and physical limitations, ensuring that accurate blood pressure monitoring is accessible to everyone who needs it. Modern monitors feature large, high-contrast displays with adjustable backlighting that remains clearly visible in various lighting conditions, while intuitive button layouts with tactile feedback accommodate users with visual impairments or arthritis. Voice-guided operation systems provide audio instructions for proper cuff placement, measurement procedures, and result interpretation, making these devices accessible to users with visual limitations or those who prefer audio guidance. Multilingual support in leading monitors includes not only display languages but also voice prompts in multiple languages, ensuring that diverse populations can effectively use these important health tools. Simplified operation modes reduce complex menu systems to essential functions, while advanced modes provide comprehensive customization options for users who want detailed control over measurement parameters and data analysis features. Color-coded result displays use universally understood traffic light systems (green for normal, yellow for elevated, red for high) to provide immediate visual feedback about blood pressure status without requiring users to interpret numerical values. The incorporation of smartphone apps with accessibility features such as screen reader compatibility, voice control, and large text options ensures that the digital aspects of modern blood pressure monitoring remain accessible to users with various disabilities, promoting inclusive health management for all populations.
9. Battery Life, Power Options, and Portability Considerations

The power management systems of modern home blood pressure monitors have been engineered to provide reliable, long-term operation while maintaining portability for users who need to monitor their blood pressure in various locations throughout their daily lives. Leading monitors in 2026 feature advanced battery management systems that can perform 300-500 measurements on a single set of AA batteries, with low-battery indicators that provide ample warning before power depletion affects measurement accuracy. Rechargeable battery options with USB-C charging capabilities eliminate the ongoing cost and environmental impact of disposable batteries while providing the convenience of charging from laptops, power banks, or wall adapters. Dual power systems that accept both rechargeable and disposable batteries provide flexibility for users who travel frequently or live in areas with unreliable electricity access, ensuring that blood pressure monitoring can continue uninterrupted regardless of circumstances. Energy-efficient designs incorporate automatic shut-off features, optimized inflation algorithms that minimize power consumption, and low-power wireless connectivity options that maintain smartphone integration without draining batteries quickly. Compact, lightweight designs weighing less than 2 pounds make these monitors easily portable for business travel, vacation monitoring, or use in multiple locations within the home, while protective carrying cases provide durability during transport. Solar charging capabilities in some premium models offer completely sustainable power options for environmentally conscious users or those in remote locations, representing the cutting edge of sustainable health technology design.
10. Price Range Analysis and Value Proposition Assessment

The home blood pressure monitor market in 2026 spans a wide price range from budget-friendly basic models under $30 to premium connected health systems exceeding $200, with each price tier offering distinct value propositions that cater to different user needs and priorities. Basic monitors in the $25-50 range provide essential blood pressure measurement capabilities with adequate accuracy for general health monitoring, typically featuring simple displays, basic memory storage, and standard cuff designs suitable for most users. Mid-range monitors priced between $50-100 incorporate enhanced features such as smartphone connectivity, irregular heartbeat detection, multi-user memory, and improved cuff designs, offering excellent value for users who want reliable monitoring with modern conveniences. Premium monitors in the $100-200+ range provide comprehensive health management systems with advanced analytics, cloud storage, multiple validation certifications, superior build quality, and extensive warranty coverage that justifies the higher investment for serious health monitoring. The total cost of ownership analysis reveals that higher-quality monitors often provide better long-term value through improved durability, more accurate measurements that reduce healthcare costs, and enhanced features that improve monitoring compliance and health outcomes. Insurance coverage and health savings account (HSA) eligibility for blood pressure monitors can significantly offset purchase costs, making premium models more accessible to users who prioritize cardiovascular health management. When evaluating value propositions, consumers should consider not only the initial purchase price but also the potential healthcare savings from early detection of hypertension, improved medication management, and reduced need for frequent medical visits enabled by reliable home monitoring.
11. Top 5 Premium Blood Pressure Monitors - Advanced Features and Performance

The premium tier of home blood pressure monitors in 2026 represents the pinnacle of cardiovascular health technology, combining clinical-grade accuracy with sophisticated health management capabilities that transform routine monitoring into comprehensive wellness systems. The Omron HeartGuide 2.0 leads this category as the world's first wearable blood pressure monitor, featuring a smartwatch design that enables 24-hour ambulatory monitoring with clinical accuracy, advanced sleep tracking, and seamless integration with comprehensive health ecosystems. The Withings BPM Connect Pro offers exceptional smartphone integration with a compact, portable design that delivers professional-grade measurements while maintaining simplicity for users of all technical abilities, featuring automatic data synchronization and comprehensive health trend analysis. QardioArm 2026 Edition combines elegant design with powerful functionality, offering wireless connectivity, multi-user support, and advanced analytics that provide personalized health insights and medication adherence tracking through its award-winning mobile application. The A&D Medical UA-651SL represents the clinical standard for home monitoring, featuring validation by multiple international organizations, exceptional accuracy across diverse patient populations, and robust construction designed for healthcare professional use in home settings. Microlife WatchBP Home S incorporates Swiss precision engineering with advanced averaging technology that automatically calculates optimal blood pressure readings while detecting atrial fibrillation with exceptional sensitivity, making it ideal for users with cardiovascular risk factors who require the highest level of monitoring accuracy.
12. Mid-Range Champions - Balancing Features and Affordability

The mid-range blood pressure monitor segment offers exceptional value by combining essential advanced features with accessible pricing, making sophisticated cardiovascular health monitoring available to a broader population without compromising measurement quality or reliability. The Omron 7 Series (BP7350) exemplifies this balance with clinically validated accuracy, smartphone connectivity, dual-user memory, and irregular heartbeat detection at a price point that makes it accessible to most households committed to cardiovascular health management. Greater Goods Smart Blood Pressure Monitor provides comprehensive smartphone integration with an intuitive app design, unlimited cloud storage, and sharing capabilities that facilitate communication with healthcare providers, all while maintaining affordability through direct-to-consumer sales models. The iHealth Track KN-550BT combines compact portability with full-featured monitoring capabilities, including wireless data transmission, comprehensive trend analysis, and integration with popular health platforms, making it ideal for users who prioritize convenience and connectivity. Beurer BM67 offers German engineering quality with advanced averaging algorithms, large display readability, and robust memory storage at a mid-range price point that delivers premium performance without premium pricing. LifeSource UA-789AC provides exceptional accuracy validation with user-friendly operation, making it particularly suitable for older adults or those who prefer straightforward monitoring without complex technological features, while still offering essential memory and averaging capabilities that support effective blood pressure management.
13. Budget-Friendly Options That Don't Compromise on Accuracy
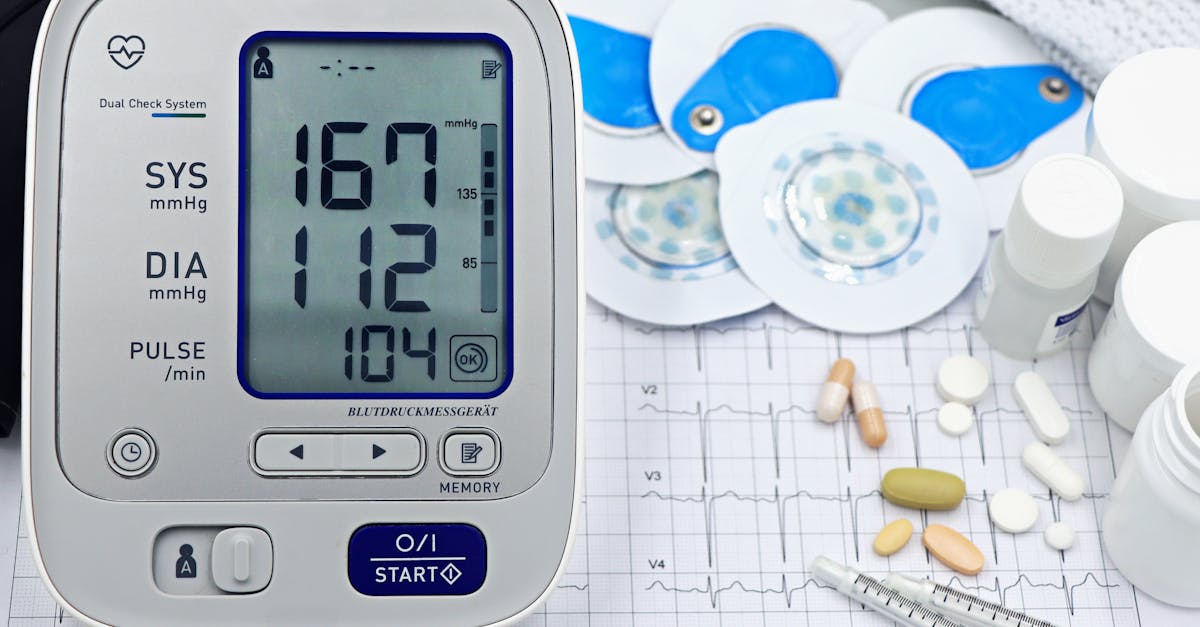
The budget-friendly segment of home blood pressure monitors proves that accurate cardiovascular health monitoring doesn't require significant financial investment, with several models under $50 delivering clinically acceptable accuracy and essential features for effective blood pressure management. The Omron 3 Series (BP7100) provides the reliability of a trusted brand with basic but accurate measurement capabilities, simple operation suitable for all ages, and adequate memory storage for tracking blood pressure trends over time. GreaterGoods Balance Blood Pressure Monitor offers exceptional value through direct sales, featuring a large, easy-to-read display, one-touch operation, and basic memory functions that provide essential monitoring capabilities at an extremely accessible price point. The Paramed
