13 Things to Understand About Living With an Autoimmune Condition
3. The Complex Relationship with Medications and Treatment
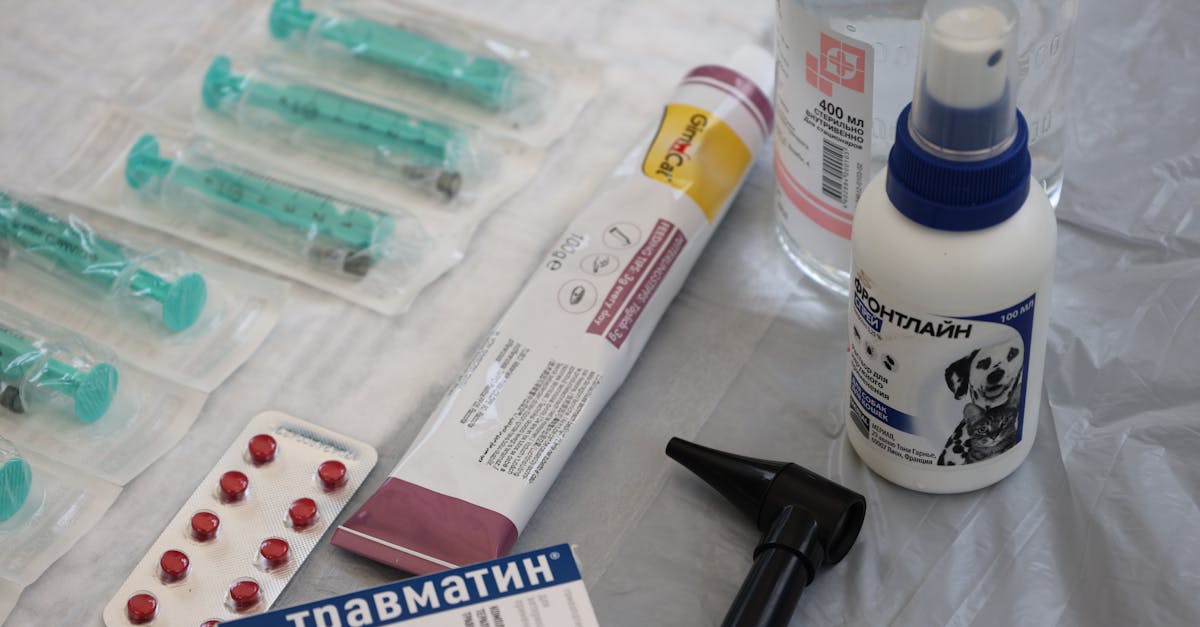
Managing an autoimmune condition typically involves a complex medication regimen that can include immunosuppressants, biologics, corticosteroids, and various symptom-specific treatments, each carrying its own benefits and potential side effects. The relationship between patients and their medications is often complicated, as the drugs designed to help manage their condition can also create new challenges and concerns. Immunosuppressive medications, while effective at reducing autoimmune activity, can increase susceptibility to infections and may require regular monitoring through blood tests to ensure safety. Many patients struggle with the psychological impact of long-term medication dependence, feeling frustrated by the need for daily pills or regular injections while also fearing what might happen if they stop treatment. The process of finding the right medication combination can be lengthy and frustrating, often involving trial and error as doctors work to balance effectiveness with tolerability. Side effects such as weight gain, mood changes, increased infection risk, or gastrointestinal issues can significantly impact quality of life, sometimes making patients question whether the treatment is worth the trade-offs. Additionally, the financial burden of autoimmune medications can be substantial, with some treatments costing thousands of dollars per month, creating additional stress and forcing difficult decisions about healthcare priorities. Understanding that medication management is an ongoing process requiring patience, communication with healthcare providers, and regular adjustments helps patients maintain realistic expectations about their treatment journey.
4. Navigating Healthcare Systems and Building Your Medical Team

Successfully managing an autoimmune condition requires building and maintaining relationships with multiple healthcare providers, often including rheumatologists, primary care physicians, specialists, and various allied health professionals. The complexity of autoimmune diseases means that patients frequently need to coordinate care across different medical specialties, each focusing on specific aspects of their condition or its effects on different organ systems. This coordination can be challenging, particularly when providers don't communicate effectively with each other or when patients feel caught between conflicting recommendations. Building a strong medical team requires patients to become active participants in their healthcare, learning to advocate for themselves, ask informed questions, and communicate effectively about their symptoms and concerns. Many patients find it helpful to maintain detailed records of their symptoms, medications, and treatment responses to share with their healthcare providers, as this information can be crucial for making informed treatment decisions. The relationship between patient and doctor in autoimmune care is particularly important, as these conditions require long-term management and frequent adjustments to treatment plans based on changing symptoms and life circumstances. Patients often need to educate themselves about their condition to have meaningful discussions with their healthcare providers and to make informed decisions about treatment options. Finding providers who listen, take concerns seriously, and work collaboratively with patients can make a significant difference in both treatment outcomes and overall quality of life.
