7 Differences Between Type 1 and Type 2 Diabetes — Explained Clearly
7. Risk Factors and Prevention Potential
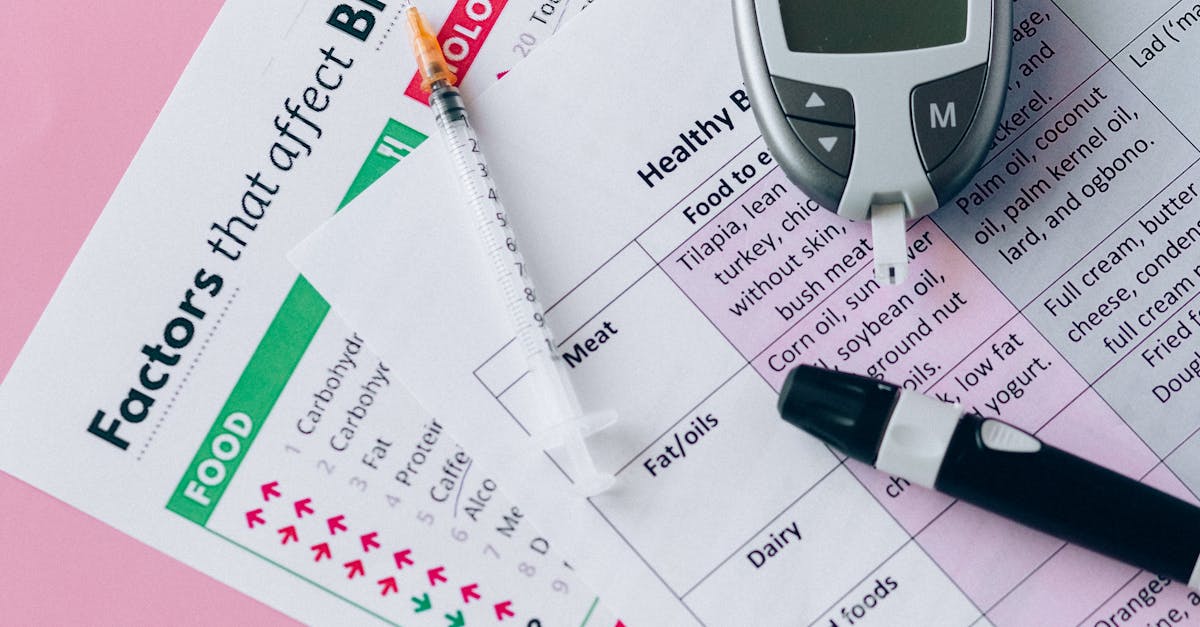

The risk factors and prevention potential for Type 1 and Type 2 diabetes represent fundamentally different scenarios, reflecting their distinct etiologies and development patterns. Type 1 diabetes risk factors are primarily non-modifiable and include genetic predisposition (particularly HLA gene variants), family history of autoimmune diseases, and certain environmental triggers such as viral infections during critical developmental periods. While having a first-degree relative with Type 1 diabetes increases risk, the genetic component is complex, and most people who develop Type 1 diabetes have no family history of the condition. Currently, there are no proven methods to prevent Type 1 diabetes, though research into immunomodulatory therapies and early intervention strategies continues. Some studies are investigating whether delaying or preventing the autoimmune process might be possible in high-risk individuals, but these approaches remain experimental. Type 2 diabetes, in contrast, is largely preventable through lifestyle modifications, making it one of the most preventable chronic diseases. Major modifiable risk factors include obesity (particularly abdominal obesity), physical inactivity, poor dietary habits high in processed foods and added sugars, smoking, and excessive alcohol consumption. Non-modifiable risk factors include age over 45, family history, certain ethnic backgrounds (African American, Hispanic, Native American, Asian American), history of gestational diabetes, and polycystic ovary syndrome. Large-scale studies such as the Diabetes Prevention Program have demonstrated that intensive lifestyle interventions can reduce Type 2 diabetes risk by up to 58% in high-risk individuals, making prevention efforts a critical public health priority.
8. Long-term Complications and Management Challenges
While both Type 1 and Type 2 diabetes can lead to serious long-term complications when poorly controlled, the patterns, timing, and management challenges differ significantly between the two conditions. Type 1 diabetes complications often develop after many years of living with the condition, typically becoming apparent 10-15 years after diagnosis, though excellent glucose control can significantly delay or prevent their onset. The primary complications include diabetic retinopathy (eye damage), nephropathy (kidney disease), neuropathy (nerve damage), and accelerated cardiovascular disease. Individuals with Type 1 diabetes face unique challenges including the constant need for insulin management, risk of severe hypoglycemia from insulin overdose, and the psychological burden of managing a complex medical condition from a young age. The precision required in Type 1 diabetes management means that even small errors in insulin dosing or timing can lead to significant glucose fluctuations. Type 2 diabetes complications may actually be present at the time of diagnosis due to the gradual, often undetected progression of the disease, with studies showing that up to 20% of people have complications when first diagnosed. The same major complications affect both types of diabetes, but individuals with Type 2 diabetes often have additional comorbidities such as hypertension, dyslipidemia, and cardiovascular disease that compound their risk. Management challenges in Type 2 diabetes include the progressive nature of the disease requiring treatment intensification over time, the complexity of managing multiple medications and conditions simultaneously, and the ongoing need for lifestyle modifications that can be difficult to maintain long-term. Both conditions require lifelong management and regular monitoring, but the specific challenges and approaches to optimal care reflect their fundamental differences in pathophysiology and progression.
