10 Common Medications That Work Differently Depending on When You Take Them
The human body operates on a sophisticated internal clock system known as circadian rhythms, which regulate everything from hormone production to cellular repair processes throughout a 24-hour cycle. This biological timekeeper doesn't just influence when we feel sleepy or alert—it fundamentally affects how our bodies process, absorb, and respond to medications. The emerging field of chronotherapy has revealed that the timing of medication administration can dramatically impact drug efficacy, side effects, and therapeutic outcomes. Research spanning decades has demonstrated that many common medications work significantly better when taken at specific times of day, aligning with our body's natural rhythms. From blood pressure medications that are more effective when taken at bedtime to cholesterol-lowering drugs that work optimally during evening hours, the "when" of medication timing has proven to be just as crucial as the "what" and "how much." This revolutionary understanding challenges the traditional one-size-fits-all approach to medication scheduling and opens new possibilities for personalized medicine. Understanding these timing-dependent effects can help patients maximize therapeutic benefits while minimizing adverse reactions, ultimately leading to better health outcomes and improved quality of life.
1. Blood Pressure Medications - Nighttime Dosing for Maximum Cardiovascular Protection
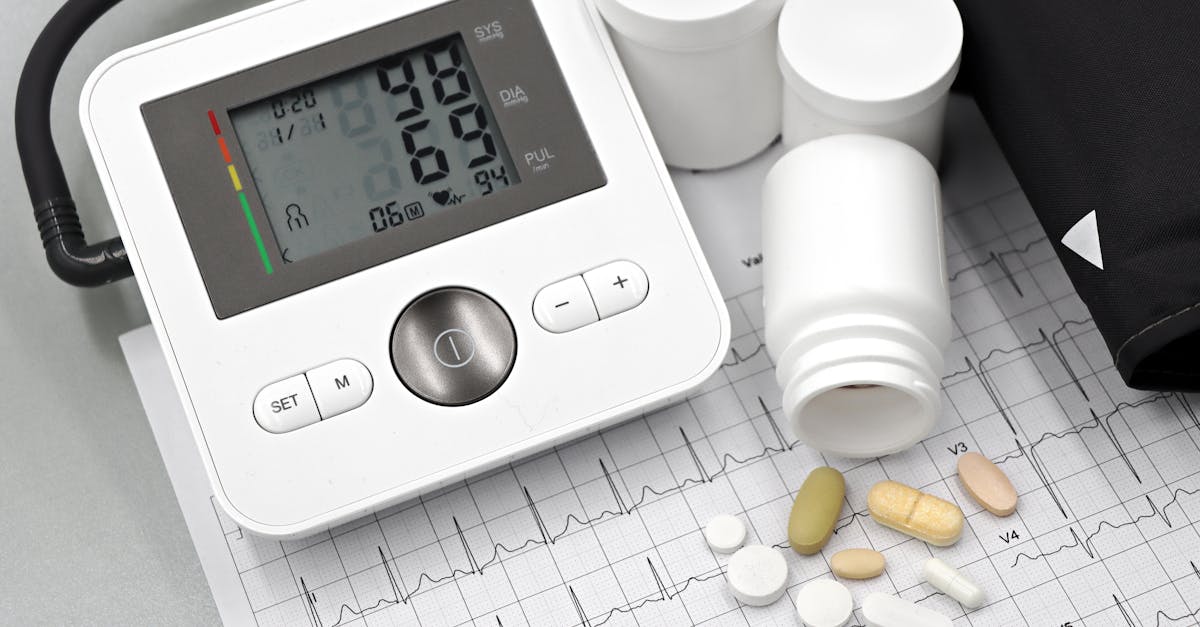
Blood pressure medications represent one of the most compelling examples of chronotherapy in action, with mounting evidence suggesting that bedtime dosing provides superior cardiovascular protection compared to morning administration. The landmark MAPEC study, involving over 3,000 patients followed for more than five years, demonstrated that taking at least one antihypertensive medication at bedtime reduced the risk of cardiovascular events by 61% compared to taking all medications in the morning. This dramatic difference stems from the body's natural circadian blood pressure pattern, where pressure typically dips during sleep and surges in the early morning hours. ACE inhibitors, ARBs (Angiotensin Receptor Blockers), and calcium channel blockers show enhanced efficacy when taken at night, as they can better control the dangerous morning blood pressure surge that coincides with increased heart attack and stroke risk. The kidneys also exhibit circadian variations in sodium handling and renin production, making evening dosing particularly effective for medications that target the renin-angiotensin system. Additionally, nighttime dosing helps counteract the natural reduction in nitric oxide production that occurs during sleep, maintaining better vascular function throughout the night. Patients who switch to bedtime dosing often experience not only better blood pressure control but also improved sleep quality, as the medications help maintain more stable cardiovascular function during rest periods.
2. Statins - Evening Administration for Optimal Cholesterol Management
Cholesterol-lowering medications, particularly statins, demonstrate remarkable timing-dependent efficacy that directly relates to the body's natural cholesterol production cycle. The liver produces approximately 70% of the body's cholesterol, with peak synthesis occurring during the early morning hours between 2 AM and 6 AM when dietary cholesterol intake is minimal. This nocturnal cholesterol production surge makes evening or bedtime administration of statins significantly more effective than morning dosing. Short-acting statins like simvastatin and lovastatin show the most pronounced timing effects, with studies revealing up to 30% greater cholesterol reduction when taken in the evening compared to morning administration. The enzyme HMG-CoA reductase, which statins inhibit, exhibits peak activity during these overnight hours, making the medications more potent when present in higher concentrations during this critical window. Longer-acting statins like atorvastatin and rosuvastatin show less dramatic timing effects due to their extended half-lives, but even these medications often perform better with evening dosing. The timing advantage extends beyond cholesterol numbers—patients taking statins in the evening often experience fewer muscle-related side effects, possibly due to better alignment with natural muscle repair cycles. Furthermore, evening statin administration may provide additional cardiovascular benefits by reducing inflammatory markers and improving endothelial function during the vulnerable overnight period when many cardiac events occur.
