11 Signs a Medication May Not Be the Right Fit for You
9. Skin Reactions and Dermatological Changes
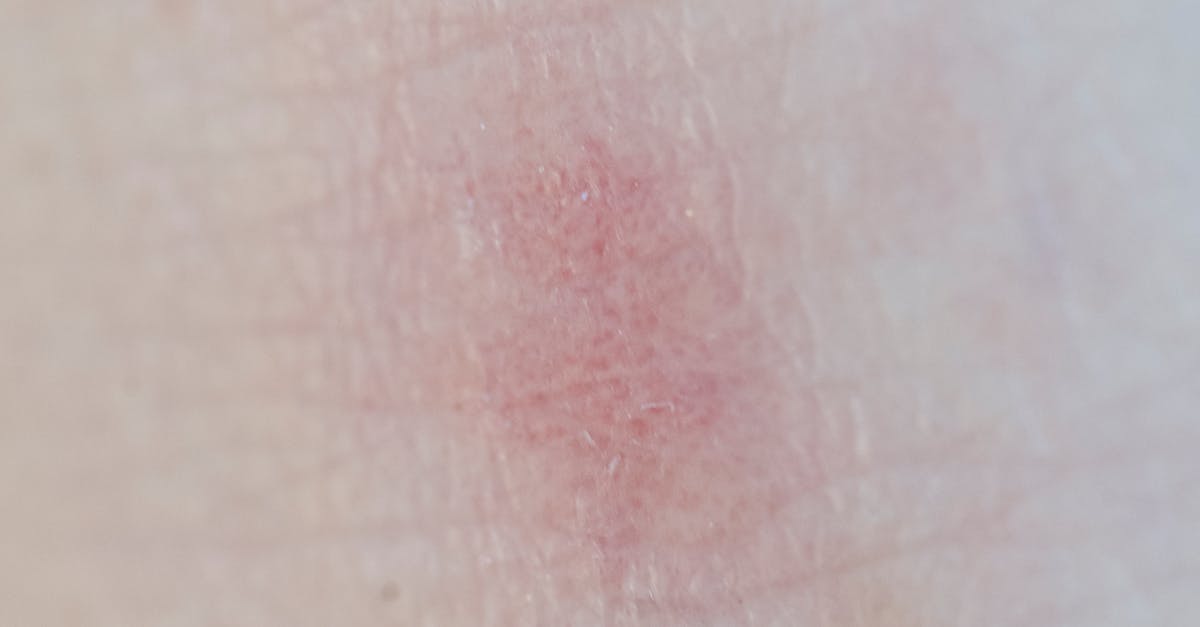
The skin often serves as a visible indicator of how well your body is tolerating a medication, with various dermatological reactions potentially signaling incompatibility or adverse effects. Skin reactions can range from mild rashes and itching to severe conditions like Stevens-Johnson syndrome or toxic epidermal necrolysis, which require immediate medical attention. Common medication-induced skin problems include photosensitivity reactions, where the skin becomes unusually sensitive to sunlight, acne-like eruptions, hair loss, or changes in skin pigmentation. Dermatological research has identified numerous medications associated with skin reactions, including antibiotics, anticonvulsants, NSAIDs, and chemotherapy agents. Some skin reactions may appear immediately after starting a medication, while others may develop weeks or even months into treatment, making the connection to the medication less obvious. The severity and type of skin reaction can provide important clues about the underlying mechanism and potential seriousness of the adverse effect. For instance, widespread rashes accompanied by fever or other systemic symptoms may indicate a serious hypersensitivity reaction that requires immediate discontinuation of the medication. Even seemingly minor skin changes should not be ignored, as they may be early signs of more serious reactions or may significantly impact quality of life and self-esteem. Certain populations, including those with existing skin conditions, autoimmune disorders, or genetic predispositions, may be at higher risk for medication-induced skin reactions. If you develop any new or unusual skin symptoms after starting a medication, it's important to document the appearance, timing, and any associated symptoms, and to seek medical evaluation to determine whether the medication should be continued, modified, or discontinued.
10. Laboratory Test Abnormalities and Biomarker Changes

Regular monitoring of laboratory values and biomarkers is essential for detecting medication-induced changes that may not be immediately apparent through symptoms alone. Abnormal blood tests, liver function changes, kidney function deterioration, or alterations in other important biomarkers may indicate that a medication is causing internal damage or dysfunction that requires immediate attention. Many medications require routine laboratory monitoring specifically because they can affect organ function in ways that are not immediately symptomatic but could lead to serious complications if left unchecked. Clinical laboratory medicine research emphasizes the importance of baseline testing before starting medications and regular follow-up monitoring to detect early signs of toxicity or adverse effects. For example, certain cholesterol medications can cause liver enzyme elevations, while some blood pressure medications may affect kidney function or electrolyte balance. Chemotherapy agents often require frequent blood count monitoring due to their effects on bone marrow function, and many psychiatric medications require periodic monitoring of metabolic parameters like glucose and lipid levels. The interpretation of laboratory abnormalities requires medical expertise, as some changes may be temporary and acceptable, while others may indicate serious toxicity requiring immediate intervention. Genetic testing is increasingly being used to predict how individuals will metabolize certain medications, helping to identify those at higher risk for adverse effects before they occur. If your healthcare provider identifies concerning laboratory abnormalities during routine monitoring, this may indicate that the medication is not suitable for continued use, even if you're not experiencing obvious symptoms. It's important to keep up with recommended laboratory monitoring and to understand what tests are being performed and why they're necessary for your specific medications.
