13 Things to Understand About Generic Medications vs. Brand Name
3. Active Ingredients vs. Inactive Components: Understanding What Really Matters

The distinction between active and inactive ingredients in medications represents a crucial concept for understanding why generic drugs can be therapeutically equivalent to brand-name drugs despite potential differences in their overall composition. Active pharmaceutical ingredients (APIs) are the chemical compounds responsible for a medication's therapeutic effects, and generic drugs must contain identical amounts of the same APIs as their brand-name counterparts, ensuring that patients receive the same therapeutic benefit regardless of which version they choose. However, inactive ingredients—also known as excipients—such as fillers, binders, colorants, flavoring agents, and preservatives, may vary between generic and brand-name formulations, leading some patients to mistakenly believe that these differences affect the medication's efficacy. These inactive components serve important functions including maintaining drug stability, facilitating manufacturing processes, improving palatability, and ensuring proper drug release characteristics, but they do not contribute to the medication's therapeutic action. While most patients experience no difference when switching between formulations with different inactive ingredients, some individuals may have sensitivities or allergies to specific excipients, making it important for patients with known allergies to review ingredient lists carefully. Pharmaceutical manufacturers carefully select inactive ingredients based on their compatibility with the active ingredient, their safety profile, and their ability to maintain drug quality throughout the product's shelf life, ensuring that these components support rather than compromise the medication's therapeutic performance.
4. Cost Dynamics: The Economics Behind Generic Drug Pricing
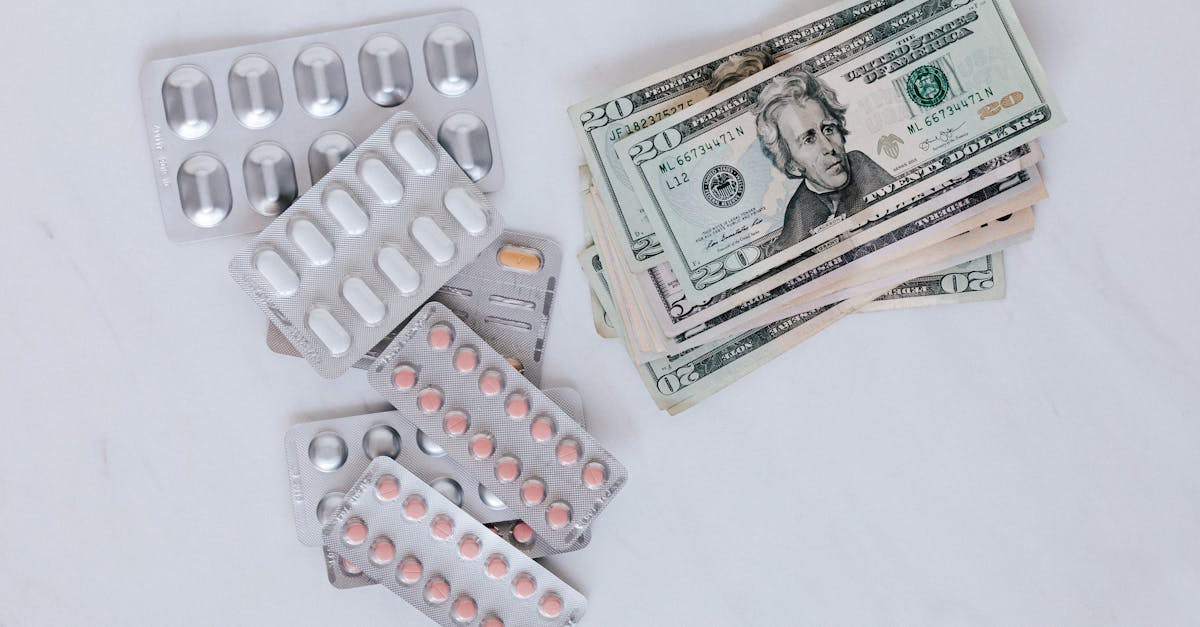
The dramatic price differences between generic and brand-name medications reflect fundamental economic principles of pharmaceutical development, patent protection, and market competition that shape the entire healthcare landscape. Brand-name drug manufacturers invest billions of dollars in research and development, clinical trials, and regulatory approval processes over periods that can span 10-15 years, with patent protection providing exclusive marketing rights that allow companies to recoup these investments through higher pricing during the patent period. When patents expire, generic manufacturers can enter the market without bearing the same development costs, as they only need to demonstrate bioequivalence rather than conducting extensive efficacy and safety trials, enabling them to offer substantially lower prices while still maintaining profitable operations. The competitive dynamics that emerge once multiple generic manufacturers enter the market typically drive prices down further, with studies showing that generic drug prices can be 80-90% lower than brand-name equivalents when multiple competitors are present. However, the economics of generic drug manufacturing also involve complex considerations including raw material costs, manufacturing capacity, regulatory compliance expenses, and market demand fluctuations that can sometimes lead to supply shortages or temporary price increases. Healthcare systems worldwide have recognized the economic value of generic medications, with many implementing policies that encourage or require generic substitution when available, resulting in billions of dollars in healthcare savings annually while maintaining the same therapeutic outcomes for patients.
