14 Common Antibiotic Questions — Answered by Healthcare Professionals
7. What Should I Do If I Miss a Dose of Antibiotics?
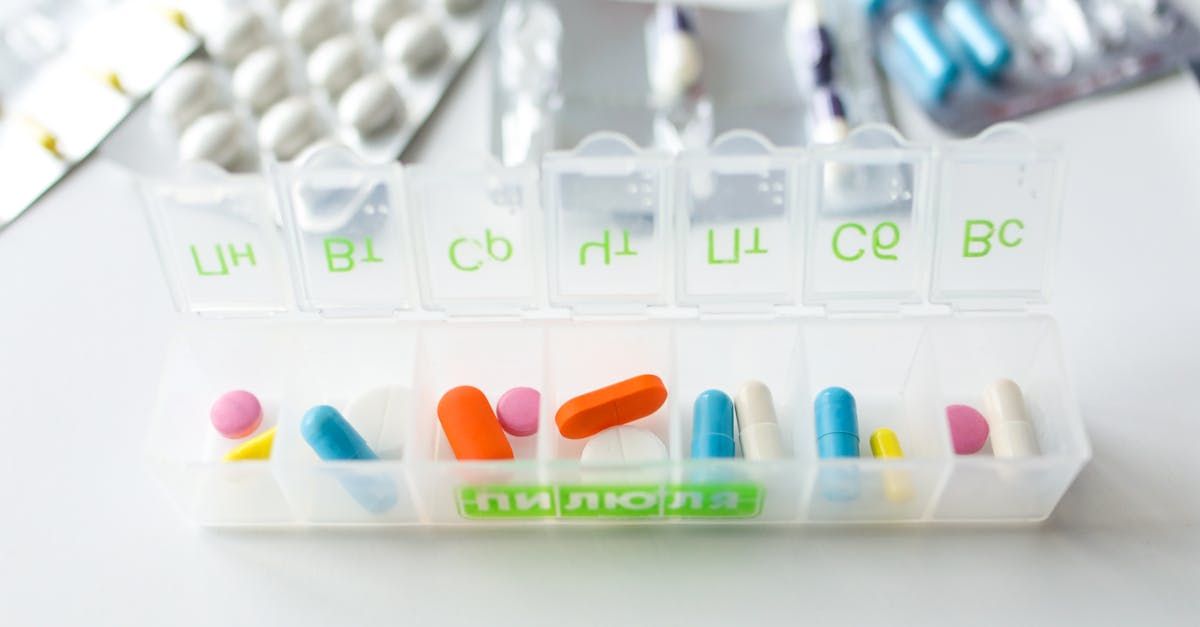
Missing antibiotic doses can significantly impact treatment effectiveness by creating gaps in therapeutic drug levels that allow bacteria to recover and potentially develop resistance, making it crucial for patients to understand proper strategies for managing missed doses. The general rule is to take the missed dose as soon as possible, unless it's almost time for the next scheduled dose, in which case patients should skip the missed dose and continue with the regular schedule rather than doubling up. However, this approach varies depending on the specific antibiotic's half-life, dosing frequency, and the time elapsed since the missed dose. For antibiotics taken multiple times daily, such as amoxicillin every eight hours, a dose missed by a few hours can usually be taken late without significantly disrupting the treatment schedule. However, for once-daily antibiotics or extended-release formulations, the timing becomes more critical, and patients may need to adjust subsequent doses to maintain appropriate intervals. Healthcare professionals emphasize that maintaining consistent antibiotic levels in the body is essential for preventing bacterial regrowth and resistance development, as fluctuating drug concentrations create selective pressure that favors the survival of more resistant bacterial strains. Patients should never double doses to "catch up," as this can lead to toxic drug levels and increased side effects without providing additional therapeutic benefit. Instead, they should contact their healthcare provider or pharmacist for specific guidance, particularly if multiple doses have been missed or if they're unsure about timing. To prevent missed doses, patients can use pill organizers, smartphone reminders, or link antibiotic administration to daily routines like meals or bedtime. Understanding that consistent dosing is as important as completing the full course helps patients appreciate why adherence to the prescribed schedule is crucial for both individual treatment success and broader public health efforts to combat antibiotic resistance.
8. Can Antibiotics Affect Birth Control and Other Medications?

Antibiotic interactions with other medications represent a significant clinical concern that can affect treatment efficacy, increase side effect risks, and lead to unexpected therapeutic failures, making it essential for patients to disclose all medications, supplements, and herbal products to their healthcare providers. The most clinically relevant interaction involves certain antibiotics and oral contraceptives, where antibiotics like rifampin can significantly reduce contraceptive effectiveness by inducing liver enzymes that metabolize estrogen and progestin more rapidly, potentially leading to unintended pregnancy. While most common antibiotics like amoxicillin and azithromycin have minimal impact on birth control effectiveness, healthcare professionals often recommend backup contraceptive methods during antibiotic treatment as a precautionary measure, particularly given individual variations in metabolism and the serious consequences of contraceptive failure. Antibiotics can also interact with anticoagulant medications like warfarin, potentially increasing bleeding risk by altering gut bacteria that produce vitamin K or by affecting liver metabolism of the anticoagulant. Some antibiotics, particularly fluoroquinolones, can interact with antacids, iron supplements, and calcium-containing products, forming complexes that prevent antibiotic absorption and reduce therapeutic effectiveness. Additionally, certain antibiotics can affect blood sugar control in diabetic patients, either by altering gut bacteria that influence glucose metabolism or through direct effects on insulin sensitivity. The timing of medication administration becomes crucial when interactions are possible; for example, separating antibiotic doses from antacids by several hours can prevent absorption problems. Healthcare professionals emphasize the importance of maintaining an updated medication list that includes prescription drugs, over-the-counter medications, vitamins, and herbal supplements, as even seemingly benign products can interact with antibiotics in unexpected ways. Patients should never stop or start medications without consulting their healthcare provider during antibiotic treatment, and should report any unusual symptoms that might indicate drug interactions.
