The Various Causes Of Psoriatic Arthritis
Psoriatic arthritis is a type of arthritis that affects individuals who have psoriasis, which is an inflammatory skin condition characterized by the development of red and silver scaly patches. The main symptoms of psoriatic arthritis are joint stiffness, pain, and swelling. It usually occurs after psoriasis first develops, but in rare cases, arthritis can form before psoriasis first presents itself. There is no cure for psoriatic arthritis, but the condition can be controlled by medication and other therapies.
Living An Unhealthy Lifestyle

As psoriatic arthritis is classified as an autoimmune disease, it is highly influenced by an individual's environment or how they choose to live. Although genetics can be a strong indication of whether or not an individual will be diagnosed with autoimmunity, their genes are highly influenced by your outside environment as well. For instance, consuming large amounts of alcohol, along with sleep deprivation, unhealthy eating, and overall poor sleeping habits can trigger certain genes that would otherwise not be affected by autoimmunity.
Inflammatory Foods

Although the exact cause of autoimmunity has yet to be confirmed, diet does seem to play a huge role. Inflammatory foods such as processed foods, foods high in refined sugar and sodium, and fast foods aggravate the immune system and form a buildup of toxins in the body's tissues, which causes inflammation and disrupts organ function. Research shows a correlation between eating foods high in antioxidants, plant chemicals that reduce inflammation, and a reduction in arthritis symptoms. Examples of healthier food choices include fresh fruits, green vegetables, and probiotics.
Stress

Stress causes chronic inflammation in the body, which is a prime suspect for causing joint and muscle pain. Inflammation caused by chronic stress may also result in skin conditions such as psoriasis. Quite literally, the stress an individual feels may show up on their skin and can be felt in their joints. It is very important to find healthy outlets for controlling stress so it does not create an acidic environment in the body in which disease and inflammation have free reign. Some examples of activities that will help reduce or eliminate stress include yoga, meditation, reading, writing in a journal, listening to muscle, going for a walk or run, and exercising.
Family History

As with most autoimmune diseases, psoriatic arthritis tends to run in a family's genetic pool. If individuals have a parent or sibling with the disease, they are more likely to develop the disease. Autoimmune conditions tend to spread. In other words, if an individual or someone in their family has already been diagnosed with an autoimmune condition, their chances of developing another autoimmune disease are greater. Blood work can be done to determine if individuals carry high levels of C-reactive proteins or antibodies that put them at an increased risk.
Age And Gender

Although anyone can develop psoriatic arthritis at any age, it is most common in adults around thirty to fifty years old. Thus, in an individual is between thirty and fifty years old and has already been diagnosed with psoriasis, their chances of developing the disease are increased. However, it is not uncommon for children to be diagnosed with this condition as well. Unlike most autoimmune diseases in which women are more prone to developing the disease, psoriatic arthritis occurs equally in both men and women.
Viral Or Bacterial Infection

A viral or bacterial infection may cause changes to the immune system by stripping away the good bacteria in the gut. When this happens, it makes the patient's body an open target for numerous diseases because the body's primary defense mechanism, its immune system, is down. Inflammation and autoimmune conditions may develop shortly after individuals fight off a viral or bacterial infection when the immune system is at its weakest. Patients should be sure to restore immune health by taking a multivitamin and mineral supplement along with a probiotic.
Psoriasis
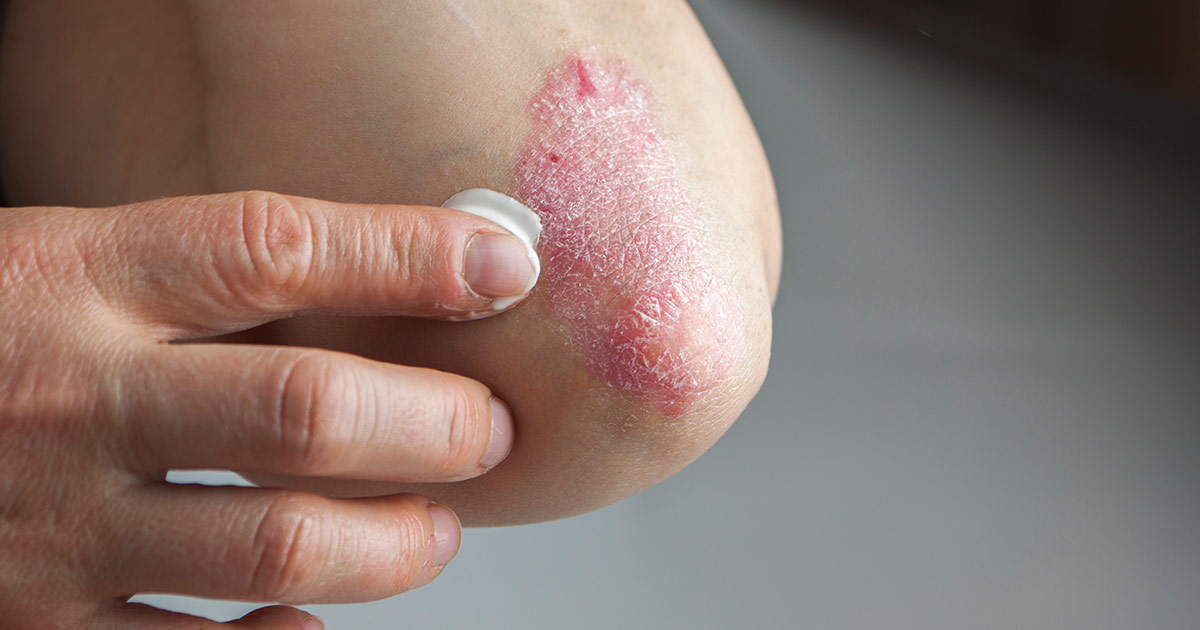
If an individual has been diagnosed with psoriasis, their chance of developing psoriatic arthritis may increase by up to forty-two percent, according to the Annals Of Rheumatic Disease. Individuals who develop psoriasis lesions on their nails have an even higher risk of developing this type of arthritis as well. Patients should talk to their doctor as soon as they notice joint pain or inflammation, especially if they already suffer from psoriasis. As with most autoimmune diseases, this condition may not be irreversible, but it can be effectively controlled and managed.
Physical Trauma Trigger
Psoriatic arthritis can result from a physical trauma trigger, particularly to the skin. When an area of the skin has been injured or traumatized, patients with psoriasis are more prone to exhibiting arthritic symptoms, as well. Examples of such trauma can include mere scratches and sunburn or less superficial triggers, such as vaccinations. When this reaction occurs, it is referred to as the Koebner phenomenon. Research has shown physical trauma greatly increases the onset of psoriatic arthritis among those people affected by psoriasis, in many cases by up to fifty percent. Researchers have yet to find a conclusive recommendation to avoid this risk, but studies continue to investigate the relationship and further causes of psoriatic arthritis.
Certain Medications
Certain medications are also linked with triggering psoriatic arthritis. Lithium, which is commonly used to treat a plethora of psychiatric disorders (such as manic depression), aggravates these arthritic symptoms in nearly half of the psoriasis patients who take it. Antimalarials, which are recommended to only be taken for short periods, may also cause these symptoms to flare up. However, the effect is rarely immediate, presenting typically two to three weeks after the medication is taken. Certain heart medications, like quinidine, has been reported to worsen psoriasis, as have some high blood pressure medicines. The nonsteroidal anti-inflammatory drug indomethacin has worsened some cases of psoriasis, but other anti-inflammatory medications can typically be substituted in to reduce side effects.
Cold Weather

Cold weather is another factor that influences psoriatic arthritis. Cold and dry weather causes the skin to dry out, which naturally puts the skin at a greater risk of flare-ups. In addition to the dry air, decreased sunlight exposure also plays into psoriasis and thus psoriatic arthritis flares. Patients who take care to frequently moisturize their skin and use a humidifier have reported their symptoms were alleviated, at least for some time. By contrast, sunny, hot weather seems to help control symptoms in the majority of individuals. Some patients see improvement in their skin due to the greater availability of natural light, while others enjoy less irritation on the skin due to wearing fewer layers of clothing.
