Causes, Risk Factors, And Complications Of Shingles
Shingles is a viral condition that results in a painful rash, though other symptoms include being sensitive to touch, itchy skin, numbness and tingling, as well as fluid-filled blisters. Patients may also deal with a fever, headache, persistent fatigue, as well as increased sensitivity to light. Most cases of shingles are found as strips of the rash and blisters around the left or right side of a patient's torso, though it can occur anywhere on the body. Shingles is not a life-threatening illness, but it can cause a great deal of pain. Vaccines reduce the risk of contracting shingles.
Varicella-Zoster Virus
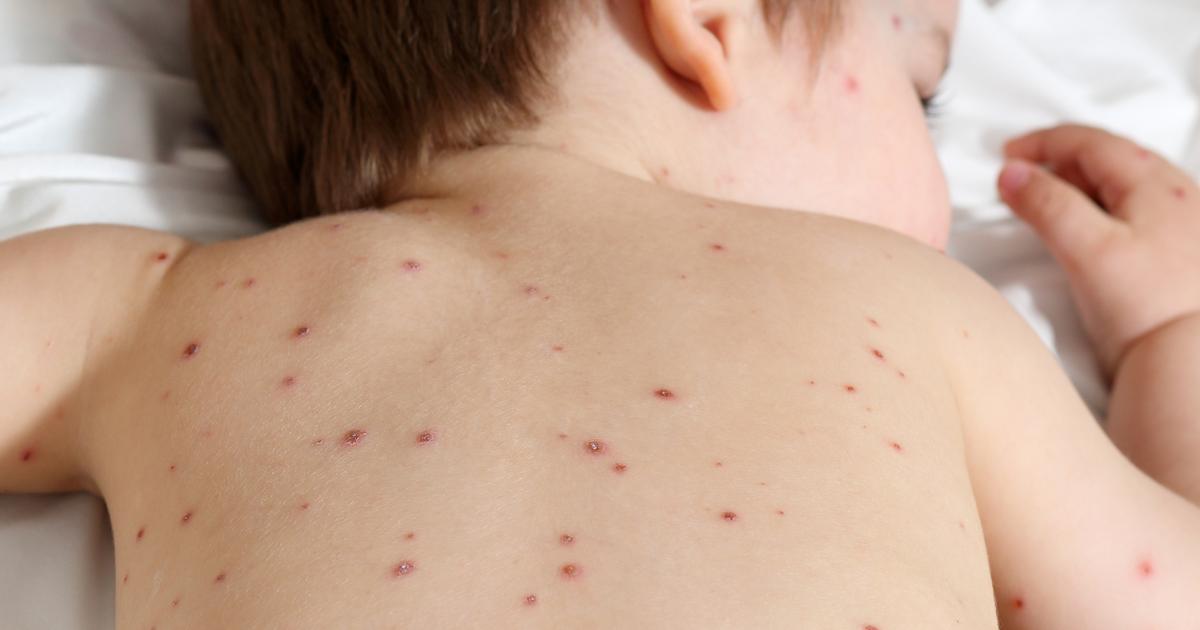
Shingles is a product of the varicella-zoster virus, which also causes chickenpox. Chickenpox is medically referred to as varicella, while shingles is medically referred to as herpes zoster. When an individual contracts chickenpox as a child, the virus doesn't leave the body after it stops causing symptoms. Instead, it stays in nerve tissues around the brain and spinal cord, though it remains dormant. For reasons currently unknown to doctors, some patients experience a reawakening of the virus, where it travels along the nerve fibers and reaches the skin, causing the blisters and other shingles symptoms. If someone had chickenpox as a child, therefore, they are at a higher risk of contracting shingles as an adult.
Age Of Individual

The age of the individual has an impact on their risk factor for developing shingles. If an individual is older than fifty, their chances of contracting shingles or having the virus become non-dormant are significantly higher. According to some researchers, at least half of all individuals who are eighty years old and older have had or will contract shingles. A patient's risk becomes increasingly higher the older they get. Most cases of shingles happen after age fifty, but there have been reported cases where individuals younger contract the disease.
Shingles almost always occurs in individuals who previously had chickenpox, and it's unlikely to show up in those who have not had it. Some studies indicate one in three individuals in the United States will develop shingles at some point during their life, and about a million cases of the disease are reported every year. Getting vaccinated against chickenpox can prevent patients from developing shingles later. If individuals haven't been exposed to the varicella-zoster virus, they cannot develop shingles later in life.
Certain Medications

If the shingles virus is already dormant in an individual, certain medications can increase their chances of developing the condition. Some drugs are designed to keep the body from rejecting transplanted organs, and these have been shown to increase a patient's risk of developing shingles. In addition, prolonged use of prednisone and other steroids can increase an individual's risk of developing shingles. They might be at a higher risk of developing shingles if they take certain medications for psoriatic arthritis or rheumatoid arthritis as well.
One study found rheumatoid arthritis patients had a much higher risk of developing shingles when they took prednisone or other steroid medications. For patients with psoriatic arthritis, there was an increased risk of shingles if they took both DMARD and TNF drugs. At the same time, the risk of shingles didn't appear to develop if the patient took either DMARD or TNF medications alone. There is not significant data to explain why the combination of these medications can increase an individual's risk of developing shingles.
Cancer Treatment
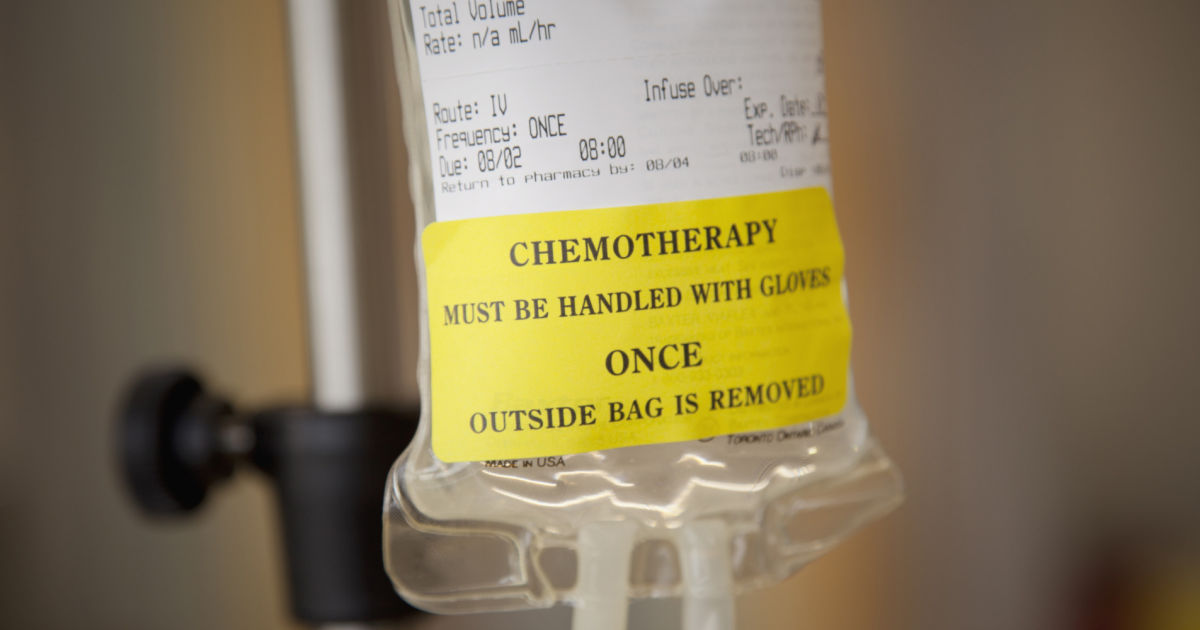
Cancer treatment has the potential to increase an individual's risk of developing shingles. This is because certain cancer treatments can lower a patient's ability to fight off diseases and infections. If a patient already has the shingles virus in their body, therefore, undergoing cancer treatments has the potential to cause the virus to spread to their skin, resulting in the blisters and other painful symptoms. Researchers found individuals who have recently received a cancer diagnosis have a much higher chance of developing shingles. This is particularly true of patients who have undergone chemotherapy or who have blood cancers.
The findings are being used for shingles prevention by giving patients with increased risk better access to shingles vaccines. Cancer patients appeared to have about a forty percent higher chance of developing shingles than individuals without cancer. In addition, patients with blood cancer were more than three times as likely to develop shingles as patients without cancer. The analysis indicated that in some individuals, the shingles vulnerability was present for at least two years before being diagnosed.
Conditions That Compromise The Immune System

If individuals have certain conditions that compromise the immune system, they have a much higher chance of developing shingles. Cancer, HIV, AIDS, and other autoimmune diseases all increase this risk. When an individual's immune system isn't holding the virus at bay, there's a larger chance it will reactivate and spread to the tissues in their skin. One other concerning thing is that a study showed patients with autoimmune diseases might have a higher chance of having a stroke after developing shingles.
Researchers are still looking into the factors that may have caused the increased stroke risk. Autoimmune diseases occur when the immune system mistakenly believes parts of the body are invading pathogens that must be destroyed. This leads to the immune system attacking healthy tissues throughout the body. One of the most common autoimmune diseases is rheumatoid arthritis, but there are many others as well.
Skin Infections
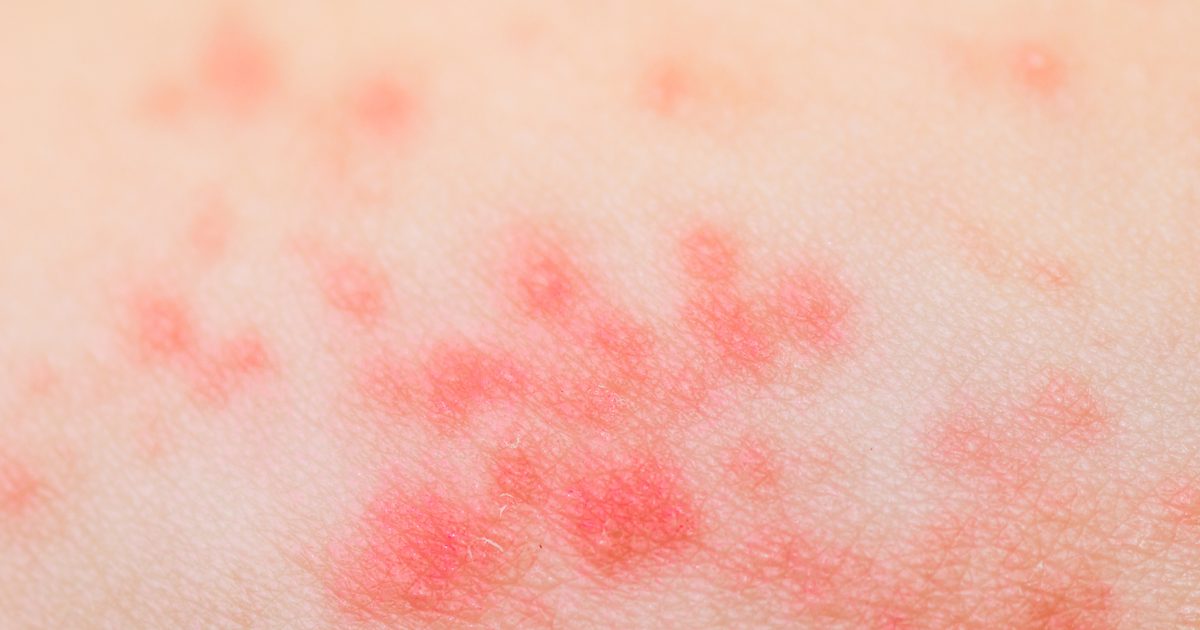
One of the potential complications of shingles is the development of skin infections. These are infections that exist independently of the overall infection with the shingles virus. It's important to treat shingles blisters properly and make sure they're kept clean and away from potential bacteria exposure. If bacteria get into the abrasions, bacterial skin infections can develop. Viral and fungal infections can also take root in the skin, but these are less likely than bacterial infections.
If the infection is mild, patients may be able to treat it using basic over-the-counter medications, but it is also possible they will need a course of antibiotics to combat the bacteria. Mild bacterial skin infections will typically be treated by using topical antibiotics, but if the infection is more advanced, patients might need a course of oral antibiotics. Some of the most common types of bacterial skin infections are leprosy, boils, impetigo, and cellulitis.
Vision Loss
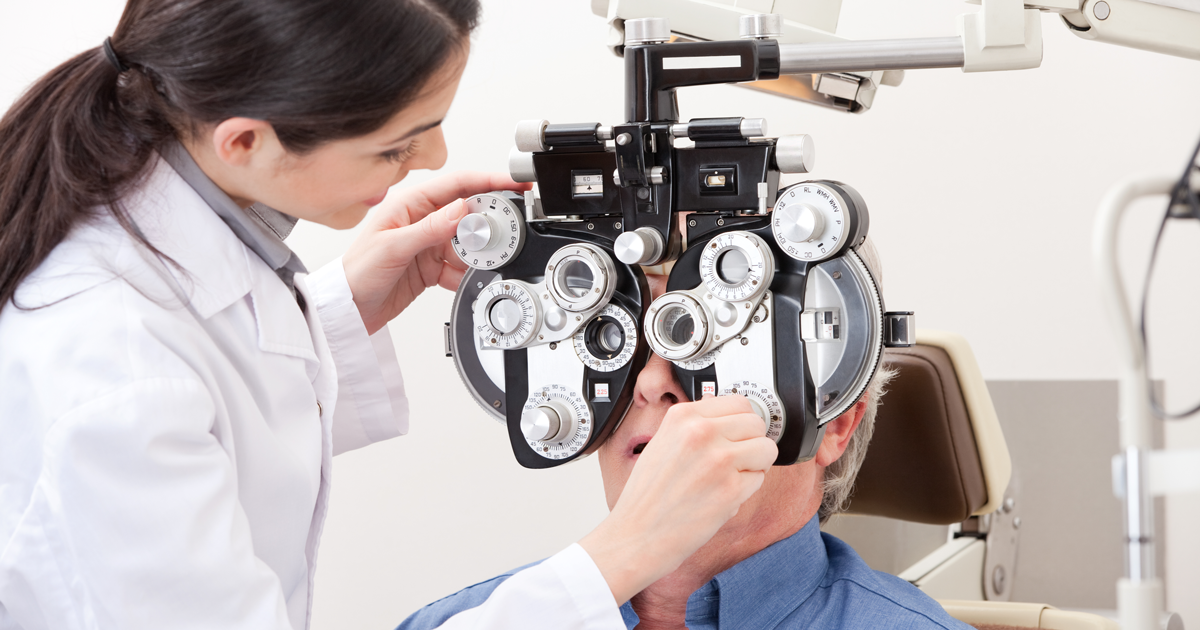
One serious potential complication of shingles is vision loss. While this won't be a potential issue for everyone, studies show somewhere from ten to twenty percent of individuals with shingles will develop a rash around and inside the eye. This type of shingles, medically known as ophthalmic herpes zoster, is caused by the same virus that causes the regular shingles virus. However, since it has different treatment methods and potential complications, it is considered a different type of shingles. Shingles in the eye can lead to vision loss, scarring, and long-term issues even after the rash has resolved.
Individuals over fifty years old can prevent vision complications from shingles by getting a vaccination. Patients with shingles of the eye will typically experience rashes and blisters that form on the eyelids, forehead, and side or tip of the nose. This might coincide with skin blisters. They'll also experience eye-related symptoms like burning and throbbing pain in the eye, redness around the eye, irritation in the eye, blurry vision, tearing, watery eyes, and increased light sensitivity.
Postherpetic Neuralgia
Postherpetic neuralgia is a shingles complication that affects the skin and nerve fibers. This condition occurs when patients continue to experience shingles pain even after their rashes and blisters have resolved. It's estimated that around twenty percent of individuals with shingles also experience postherpetic neuralgia. Neuralgia is the medical term for neuropathic pain occurring along the nerve. The most common underlying cause is damage or irritation to the nerve that leads to an alteration of the neurological function or structure. The feeling might be of intense stabbing or burning, and patients might feel as though the pain is shooting along their affected nerve.
Neuropathic pain is generated inside the nervous system rather than being a reaction to outside stimuli. The treatment for this kind of pain depends on the type and severity of the pain, along with the patient's overall health. Some individuals call neuropathic pain a pinched nerve, but pinching isn't always the reason for the pain in cases of postherpetic neuralgia. There have been rare cases where patients also experience muscle paralysis or weakness because the affected nerve controls certain movements.
Encephalitis
The chances of developing neurological issues vary widely depending on the presentation of symptoms. Some patients experience an inflammation of the brain, which is known as encephalitis. This can be a very serious condition that requires immediate medical treatment. Encephalitis isn't always caused by shingles. The most common cause, however, is an underlying viral infection like the shingles virus. It is common for encephalitis patients to experience symptoms similar to a mild case of the flu, including a headache and fever.
Some patients do not have any symptoms whatsoever. Individuals with encephalitis may also have neurological symptoms like seizures, issues with their senses, impaired motor function, or confused thought processes. There are rare cases in which encephalitis can become life-threatening. It's important to diagnose and treat the problem promptly since encephalitis can have such widely different effects on different individuals. If patients start experiencing neurological symptoms like seizures or cognitive distortion, they should seek emergency medical treatment.
Facial Paralysis
Another neurological complication that can occur in individuals with shingles is facial paralysis. There's a condition known as Ramsay Hunt syndrome, otherwise called herpes zoster oticus, caused by a shingles outbreak affecting one of the facial nerves. This nerve is located near the ear. On top of the painful rash, damage to the nerve might lead to both facial paralysis and hearing loss in the affected ear. If individuals experience shingles rashes on the face, especially if the pain is accompanied by neurological issues, patients need to get medical treatment right away.
The faster they are treated, the smaller the chances of permanent complications like deafness and facial paralysis are. Patients might find their face is weak or paralyzed on the same side of the face as their affected ear. The rash tends to be painful, red, and have fluid-filled blisters around and inside the ear. The paralysis and rash tend to come on at the same time. There have been rare cases in which the paralysis occurs without a visible rash.
