What Causes Heel Pain?
The ankle and foot are some of the most complex parts of the body. There are twenty-six bones, more than one hundred tendons, and thirty-three joints in each foot and ankle. The largest bone in the foot is the heel. Heel pain often occurs when the heel is injured or overused. Pain in the heel can range widely in severity, with some pain being mild and other pain being so disabling that walking is difficult or impossible. If rest and home remedies don't relieve the pain, individuals might need to see a podiatrist or their general practitioner to diagnose the underlying cause. The vast majority of heel pain issues are treatable, and many of them are curable.
Sprains Or Strains

Heel pain can be caused by sprains or strains, which most individuals get while exercising or engaging in other physical activity. Strains and sprains are both common, and the severity can vary widely from case to case. Some individuals with a muscle strain or sprain affecting their heel may just need to rest for a day and avoid walking when possible. Others may have serious and disabling complications that last for weeks to months.
Sprains occur when ligaments, which connects bones at a joint, become torn or overstretched. Ankle sprains are the most common kind of sprain, and they can cause heel pain. Strains occur when tendons, which connect muscles to bone, or muscles become torn or overstretched. Though strains and sprains involve injury to different types of soft tissue, they present with many of the same symptoms. Sprains frequently present with difficulty moving the joint, limitations on flexibility, pain, swelling, and bruising. Strains mimic these symptoms almost exactly, but instead of bruising, they cause muscle spasms.
Fractures

A fracture is commonly known as a broken bone. Individuals who think they may have broken a bone in their foot should seek emergency medical care. Some fractures are thin cracks, but others cause complete breaks in a bone. The majority of bone fractures happen when a bone is hit by more pressure or force than it can manage. The pain from a fracture tends to be intense, although not everyone experiences the same pain levels from the same injuries.
If an individual's heel bone or any of their ankle bones are fractured, they will likely feel pain in their heel. Affected individuals often experience worse pain when they touch or move the hurt area. Depending on the bone that was injured, patients may not be able to put pressure on their foot at all. A fracture may be accompanied by a visible deformity, swelling, bruising, and redness around the area of injury. Some individuals hear a grinding or snapping sound when the injury first happens.
Plantar Fasciitis

Plantar fasciitis is among the most common causes of heel pain. This condition occurs when pressure on an individual's feet leads to damage to their plantar fascia, which is the ligament connecting their heel to the front of their foot. The plantar fascia helps with walking and supports the arches of an individual's feet. Normal day-to-day activities can cause wear and tear on the plantar fascia, especially if individuals wear unsupportive shoes. If there's too much pressure on an individual's feet, it can lead to tearing or damage in the ligament, which in turn causes inflammation. The inflammation is what causes the stiffness and pain in the heel.
The hallmark symptom of plantar fasciitis is intense pain on the underside of the heel. This pain is often worse in the morning right after getting up. Over time, some individuals gradually develop additional pain at the underside of their arches, which can range from a dull ache to sharp and stabbing pain. Burning sensations have also been reported. Plantar fasciitis can make it difficult to climb stairs because of the stiffness in the heel.
Achilles Tendonitis
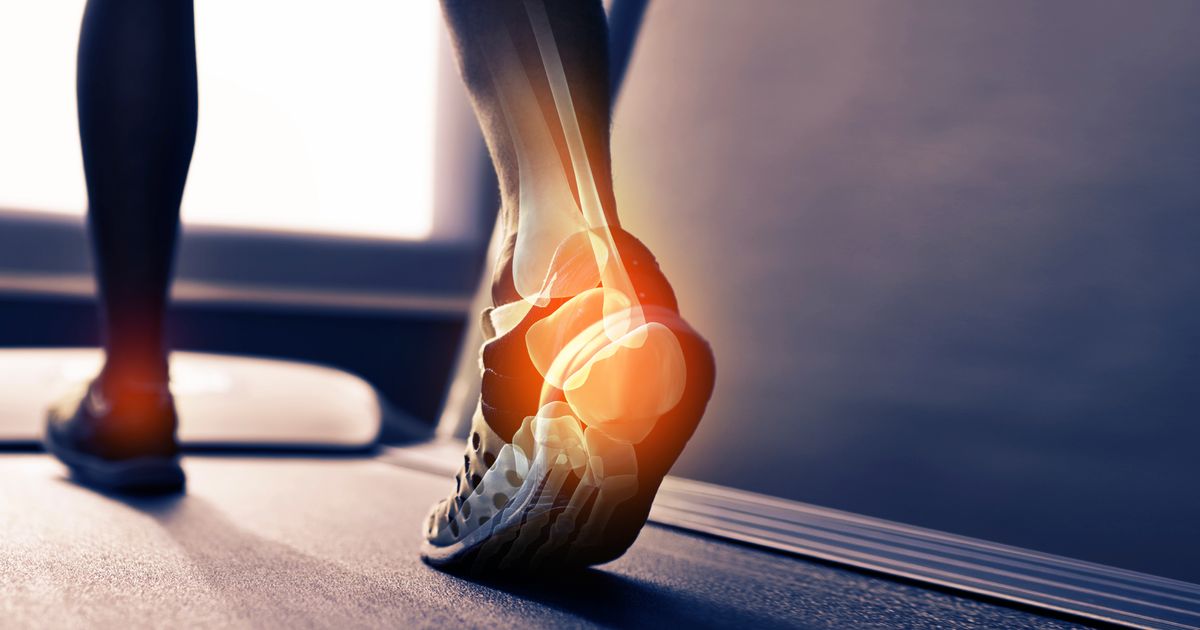
Achilles tendonitis is a condition that occurs when the Achilles tendon becomes inflamed or injured due to overuse. The Achilles tendon is responsible for connecting the heel to the calf muscles. It's necessary for standing on tiptoe, running, walking, and jumping. The majority of cases of Achilles tendonitis occur due to continuous and intense exercise or other physical activity, such as intense running sessions or jumping routines.
The condition has two subtypes. The insertional subtype of Achilles tendonitis affects the part of the tendon that attaches to the heel bone. The noninsertional subtype affects certain fibers in the midsection of the tendon. Younger athletes and fitness buffs are more likely to develop noninsertional tendonitis than insertional. The first line of treatment for Achilles tendonitis is to rest and use basic home remedies for the pain. But if the injury doesn't seem to be healing, affected individuals should see a doctor. Worsening tendonitis can lead to a tear in the tendon, which might require surgery and medication to treat.
Bursitis

Bursae are small and fluid-filled sacs responsible for cushioning joints and absorbing shock. They can be found in the areas in which muscle tissues, skin, and tendons attach to bones. When the bursae become inflamed, it is called bursitis, a painful condition that can occur at varying points in the body. Though the condition most commonly affects the hip, elbow, and shoulder, it can also affect the heel, knee, and big toe.
When it affects the heel, it often results in heel pain. The condition usually develops around joints that undergo continuous and repetitive motions. The main form of treatment is to rest the joint and keep it from undergoing more trauma. The majority of cases clear up after just a few weeks. With that said, it's common for patients to experience recurring flare-ups of bursitis after the initial inflammation.
Reactive Arthritis
Reactive arthritis is arthritis that develops in response to an infection. While it can be triggered by an infection anywhere in the body, it is most frequently caused by infections of the urinary tract, intestines, or genitals. Patients with this condition experience inflammation, pain, and swelling, and the feet, ankles, and knees are among the most common sites for these symptoms. The urethra, skin, and eyes could also be affected in some cases. A rash might form on the soles of the feet or the palms of the hands, and patients may notice swollen fingers or toes. Some individuals report heel pain and lower back pain as well.
The frequency of urination may increase, and patients could experience discomfort during urination. Reactive arthritis usually occurs as a result of a sexually-transmitted or foodborne bacterial infection. Sexually-transmitted infections such as chlamydia may trigger it, and food contaminated with salmonella or campylobacter is another recognized cause. Patients generally experience intermittent symptoms with reactive arthritis, and the condition usually resolves completely within one year. Treatment methods may include antibiotics to treat the bacterial infection, and patients might be prescribed corticosteroids or medications normally used in the treatment of rheumatoid arthritis.
Ankylosing Spondylitis

Ankylosing spondylitis is a type of arthritis that affects the spine. It produces inflammation and causes the vertebrae to gradually fuse together. This condition is more common in men, and symptoms generally start in early adulthood. Patients with ankylosing spondylitis have reduced flexibility in the spine, and they may adopt a posture that hunches forward. If the condition affects the patient's ribs, it might become difficult to take deep breaths. In addition to the spine, the hips, shoulders, and heels are often affected. At first, symptoms may only be present in the morning or after periods of inactivity. They may worsen over time, and some patients experience temporary remission or improvements in symptoms as well. Doctors will perform a physical exam and imaging studies to diagnose ankylosing spondylitis.
During the exam, the patient will be asked to take a deep breath so the doctor can check if the chest expansion is normal. The patient's range of motion will be examined, and the physician may press on the pelvis or move the legs into specific positions to check for pain. MRI scans can detect signs of this condition at earlier stages than other types of imaging studies, and x-rays may be performed as well. Treatment options usually center around medication. Doctors may prescribe non-steroidal anti-inflammatories like naproxen and indomethacin, and patients might be prescribed an interleukin-17 inhibitor or a TNF blocker. Physical therapy may help patients with maintaining posture and flexibility in the joints.
Osteomyelitis
Osteomyelitis is a serious bone infection triggered by bacteria or fungi. It is more common in men, and it may be life-threatening. In some cases, patients with this condition might not display any symptoms. The symptoms that do occur are often similar to other conditions that are not as serious, making osteomyelitis difficult to diagnose. Patients may notice pain in the infected portion of the bone, and this often worsens with movement. The infected area could appear red or swollen, and it might be warmer than the surrounding tissue.
Chills and a high fever could develop too. Infection with the Staphylococcus bacteria is the most frequent cause of osteomyelitis, and bacteria may enter the bloodstream through severe bone fractures, open wounds, or operations on the bones such as bone implants. Blood tests, imaging studies, and a biopsy may be necessary to diagnose this condition. Treatment may include antibiotics or antifungals, and patients might need to have surgical procedures to remove the infected bone. Amputation may be used as a last resort to stop the infection from spreading.
Rheumatoid Arthritis

Rheumatoid arthritis is an autoimmune condition that causes joint pain and inflammation. While other forms of arthritis are caused by wear and tear on the joints, this form of arthritis affects the lining of the joints, and it could eventually lead to erosion of the bones and joint deformities. In general, patients experience symptoms in the same joints on both sides of the body; for example, both wrists may show symptoms at the same time. The smaller joints of the fingers and toes are typically affected first, and the condition may cause symptoms such as a fever, loss of appetite, or fatigue. Some patients may experience symptoms that affect the skin, heart, lungs, kidneys, and eyes as well.
To diagnose rheumatoid arthritis, doctors often perform blood tests that check the patient's erythrocyte sedimentation rate and C-reactive protein levels. Both of these tend to be elevated in individuals with this form of arthritis. Rheumatoid factor tests may be conducted, and MRI scans or ultrasounds are used to determine the severity of the condition. Treatment methods include biologic agents such as adalimumab, etanercept, and tofacitinib, and patients might also take disease-modifying antirheumatic drugs such as methotrexate. Physical therapy could help maintain joint flexibility, and physical therapists often teach patients modified ways of completing tasks with less pain.
Heel Spurs
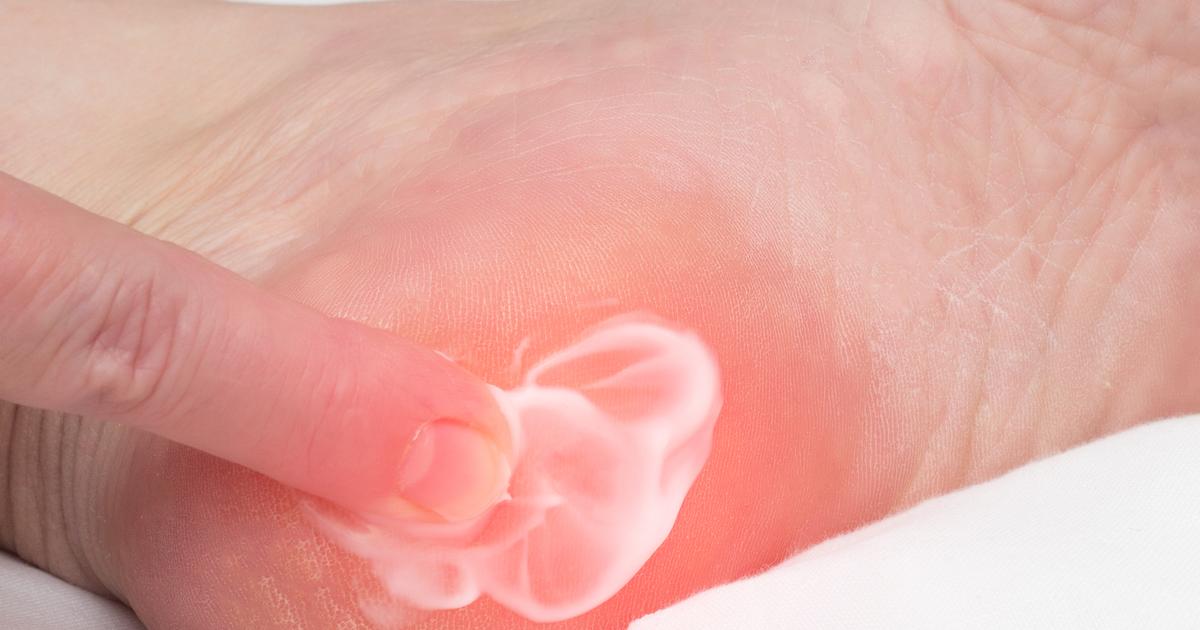
Heel spurs occur when a calcium deposit forms in the area between the heel bone and the arch of the foot. They typically begin at the front of the heel or just underneath it. Symptoms of heel spurs include swelling and pain in the heel, and the heel might feel warmer than other areas of the foot. A tiny protrusion of bone might be visible on the heel itself; however, a heel spur can be present without any visible changes to the bones or soft tissues.
Patients could develop heel spurs as a result of obesity, arthritis, walking issues, or bruises on the heel, and they may occur if the patient frequently wears footwear that does not properly support the foot. X-rays are used to detect heel spurs, and recommended treatment methods include rest, over-the-counter pain medications, cold compresses, and physical therapy. In severe cases, heel spurs might be treated with corticosteroid injections.
