Causes And Risk Factors Of A Baker's Cyst
If you notice a soft lump behind your knee, you may have what is known as a Baker's cyst. Damage to the joint of the knee, either due to disease or injury, can lead to the leakage of the lubrication that fills the area of the joint, called synovial fluid. This fluid can collect within the tissue, forming a sac that may feel like it is the size of a golf ball. Also called a popliteal cyst, a Baker's cyst can cause pain and a feeling of tightness when you bend your knees during activities. There are several causes and risk factors for developing a Baker's cyst. These cysts typically go away on their own, especially if the underlying cause is addressed.
Joint Swelling

If there is inflammation or swelling within a joint, this can lead to an increase in the body's production of synovial fluid. If the swelling becomes too severe, the excess synovial fluid can leak out and form the tell-tale sac behind the knee of a Baker's cyst. The cyst itself can form when the extra synovial fluid moves to the back of the knee and is cut off to form a sac by the pressure of the bones pressing together. If you notice the development of this type of cyst, find out the exact cause of joint swelling that is leading to excess inflammation.
Arthritis

Perhaps one of the most common causes of swelling in the knees is arthritis. Rheumatoid and osteoarthritis are the most common forms of this disease that can lead to the development of a Baker's cyst. This is because these forms of arthritis are degenerative, causing the body to respond with inflammation and the development of excess synovial fluid as an effort to lubricate and protect the degrading joint tissues. When a Baker's cyst is caused by such a degenerative condition, there is a possibility that surgery may be required to drain or remove the cyst due to the chronic inflammatory nature of the disease.
Knee Joint Injury
Another factor that can increase inflammation and lead to a Baker's cyst is an injury to any portion of the knee joint. The two main bones of the leg come together to form the knee joint, with the kneecap loosely arranged in front. There is also connective tissue in the way of ligaments that keep the bones arranged properly. Falling directly on a knee, being hit in the side of the leg, or shifting the leg in the wrong direction, such as while playing certain sports, can all become risk factors for a knee joint injury and the further development of a Baker's cyst.
Torn Meniscus

Rotating the knee while it is in use can result in the tearing of one of the pieces of cartilage that cushion your leg bones where they meet at the knee. It more commonly occurs while playing certain sports, such as basketball, soccer, or football, though it can occur during any activity. A torn meniscus can result in pain, swelling, and a reduced range of motion in the knee. The swelling can lead to an increase in synovial fluid as the body attempts to protect the joint. Thus, a Baker's cyst can form. Even after your knee has healed following a tear in the meniscus, the injury can lead to osteoarthritis, another risk factor to Baker's cysts.
Other Knee Problems
There are some other conditions that might affect the knee that can contribute to the development of a Baker's cyst. Basically, anything that causes inflammation in the knee increase the risk of an individual developing a Baker's cyst. Bursitis is an excess of swelling that may occur from overuse of a joint. Patellar subluxation involves the abnormal movement of the kneecap. An infection may also occur beneath the kneecap. Each of these other knee problems has been shown to give individuals an increased risk of experiencing the formation of a Baker's cyst.
Gout

Gout is an inflammatory form of arthritis caused by an accumulation of urate crystals in the joints. Symptoms of this condition generally include severe pain in the knees (what typically results in a Baker's cyst), ankles, elbows, and wrists, and patients may also have swelling, redness, and reduced range of motion in the affected areas. Gout symptoms usually occur at night, and the condition typically flares up for a few days before subsiding; patients may go months or years between symptomatic episodes.
Diets high in alcohol, seafood, meat, and fructose increase the risk of gout, and patients with obesity, cardiovascular disease, kidney issues, and hypertension have an elevated risk of this ailment. Treatment options include anti-inflammatory medicines, colchicine, and corticosteroids. Individuals who have several gout episodes each year may be advised to take medications such as febuxostat or allopurinol to block the production of uric acid.
Hemophilia

Hemophilia is a condition that causes abnormalities in blood clotting. Approximately seventy percent of cases are inherited, and patients may also develop the condition as a result of pregnancy, cancer, autoimmune conditions, or multiple sclerosis. The symptoms of hemophilia vary depending on the patient's level of clotting factors in the blood. Individuals who have clotting factors that are only mildly reduced might have issues after surgery or trauma.
Patients with significant reductions in clotting factors could experience more severe symptoms such as nosebleeds with no known case, bleeding after minor dental work, or prolonged bleeding after an injection. Blood might also be present in the urine or stool, and joint damage has been observed. Treatment methods include replacement of clotting factors, the use of fibrin sealants for wounds, and medications such as desmopressin and antifibrinolytics (medicines that prevent the breakdown of clots).
Psoriasis
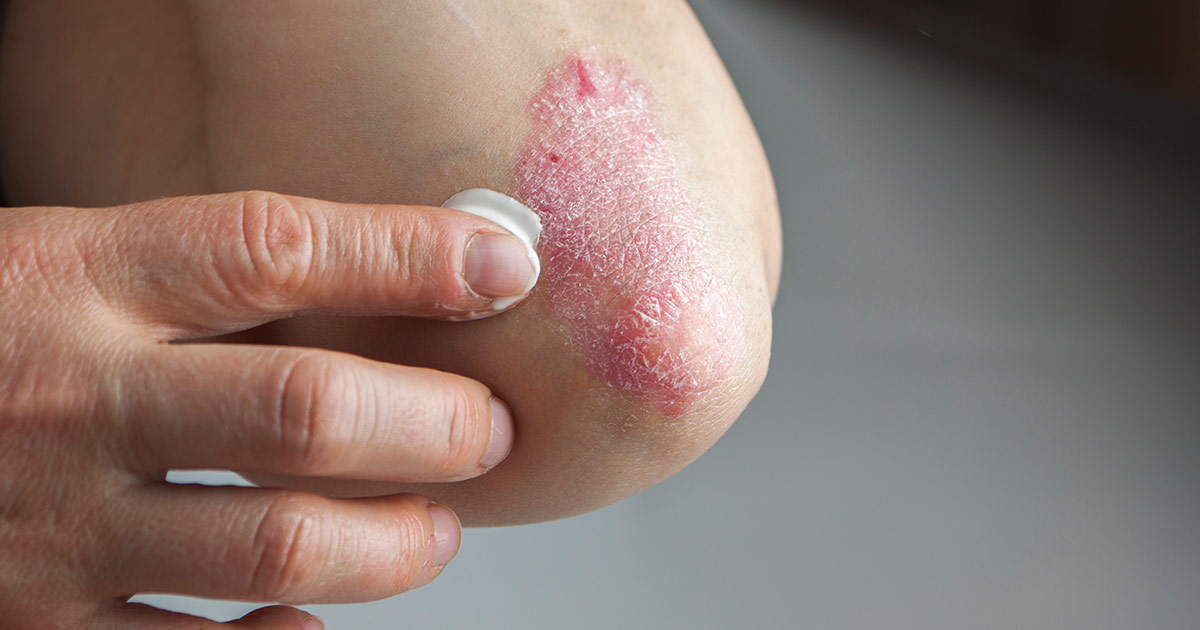
Psoriasis is a type of chronic skin condition that may develop in patients who have an overactive immune system. Individuals with this condition may have patches of inflamed, red, and itchy skin, and some patients also have scaly plaques. Nail pitting is frequently seen, and the nails may sometimes crumble or detach from the nail bed. An estimated ten to thirty percent of patients with this ailment will develop psoriatic arthritis, a condition that leads to joint inflammation, pain, and damage. The joint inflammation, which it surrounds the knee, is primarily what increases an individual's risk of a Baker's cyst.
To diagnose psoriasis, the doctor will examine the patient's skin and nails, and a skin biopsy may be performed to confirm the condition. During the exam, the physician will assess the patient for signs of psoriatic arthritis. They will palpate the patient's knees, ankles, elbows, and wrists to check for tenderness or swelling, and their sensation and range of motion may also be evaluated. X-rays and other imaging studies can help distinguish between psoriatic arthritis and other forms of arthritis. Treatment options for psoriasis include steroid and non-steroid prescription creams, phototherapy, methotrexate, and biologics. For patients who also have psoriatic arthritis, immunosuppressants, TNF-alpha blockers, and newer medications such as ustekinumab, secukinumab, and apremilast may be appropriate.
Lupus

Lupus is an autoimmune condition that causes systemic inflammation throughout the body. The disease can affect the heart, kidneys, brain, joints, and lungs. Patients may experience fatigue, headaches, anxiety, weight loss, joint pain, and depression. Some might also develop a facial rash across the cheeks and the bridge of the nose; this is sometimes referred to as a butterfly rash. Anemia, chest pain, mouth ulcers, and hair loss have been observed. To diagnose this condition, doctors will perform a complete blood count to check for low hemoglobin, a reduced white count, and a reduced platelet count. An erythrocyte sedimentation rate test that measures the hourly rate at which a patient's red blood cells settle in a test tube could also aid diagnosis. Kidney and liver function tests and a urinalysis might be ordered too.
If lupus is confirmed, patients may be treated with immunosuppressants, anti-malarial drugs, or corticosteroids. Intravenous infusions of belimumab help to reduce symptoms for some patients. Potential side effects from the infusion include nausea, vomiting, arm or leg pain, and insomnia. Another medication, rituximab, is also given by intravenous infusion, and this medicine can help patients who have not been successful with other treatments.
