Symptoms Of Selective IgA Deficiency And Related Conditions
Selective IgA deficiency is a condition of an individual's immune system where they do not have enough of an antibody or protein with the function of fighting infections called immunoglobulin A (IgA). Selective IgA deficiency is characterized by indiscernible levels of immunoglobulin A in a patient's secretions and blood. Individuals affected by this deficiency do not typically have a deficiency of any other immunoglobulin proteins. Different immunoglobulin proteins are present in different defense mechanisms in a patient's body.
Most of an individual's immunoglobulin A is present in the mucosal surface secretions such as colostrum, respiratory secretions, saliva, gastrointestinal secretions, tears, and genital secretions. These body regions in healthy individuals are well protected from pathogens because of immunoglobulin A presence. An estimated one out of every five hundred Caucasians is affected by selective IgA deficiency. Half of the affected individuals experience symptoms related to increased infection susceptibility.
Ear Infections

Frequent and recurrent ear infections can be a symptom manifestation in an individual affected by selective IgA deficiency. The most common type of ear infection in affected individuals is one of the middle ears called acute otitis media. Bacteria and viruses can enter and colonize an individual's middle ear space through the Eustachian tube and nasopharynx. The most common viruses responsible for the recurrent ear infections in selective IgA deficiency patients include adenovirus, respiratory syncytial virus, rhinovirus, and bocavirus.
The types of bacteria that most commonly cause selective IgA deficiency precipitated ear infections are Hemophilus influenzae, Streptococcus pneumoniae, and Moraxella catarrhalis. The presence of immunoglobulin A in a patient's upper respiratory tract and inner ear lining of epithelial cells is imperative to prevent the growth and spread of viruses and bacteria that cause ear infections. Recurrent ear infections because of this immune deficiency can cause an affected individual to experience hearing loss.
Pneumonia

Recurrent pneumonia can be indicative of selective IgA deficiency. Pneumonia infections that do not resolve or return frequently are one of the most common symptoms in individuals affected by this primary immune deficiency. The prevalence of this symptom is so great that most patients who have a primary immune deficiency are diagnosed with it when they encounter a pulmonologist or specialized doctor that works with the pulmonary system. Pneumonia is an infection that occurs in an individual's lungs when their alveoli accumulate pus or fluid. This pus or fluid build-up makes it difficult for the affected individual to move oxygen from the air they breathe into their bloodstream.
Pneumonia can occur in just one lung or both lungs. Pneumonia is a contagious infection where the bacteria or virus that causes it can easily spread to another individual. Oftentimes, a flu virus or a cold virus will cause a patient to develop pneumonia. Individuals affected by selective IgA deficiency may have a harder time recovering from viral pneumonia because even the strongest antibiotics are unable to help their immune system overcome the pathogen.
Sinusitis

Patients who experience recurrent sinusitis infections may have selective IgA deficiency. The sinuses are air pockets that sit just within the bones of an individual's face that surround their nose. Typically, these pockets are hollow and function to produce mucus that subsequently drains into the nose. However, the sinuses can easily become blocked, which makes a nice place for pathogens to colonize. The immune system responds to this pathogenic invasion, and the result is sinusitis. The blockage that begins the cascade of events leading to sinusitis can be caused by allergies.
The mucus that lines the nasal passages and sinuses does not contain immunoglobulin A in individuals who have selective IgA deficiency. This malfunction means their natural defenses to a pathogenic invasion of these areas are impaired. Oftentimes, sinusitis can be challenging to treat in selective IgA deficiency patients because topical intranasal beclomethasone, antibiotics, and N -acetylcysteine are ineffective at reducing sinus inflammation and eradicating pathogens.
Rheumatoid Arthritis
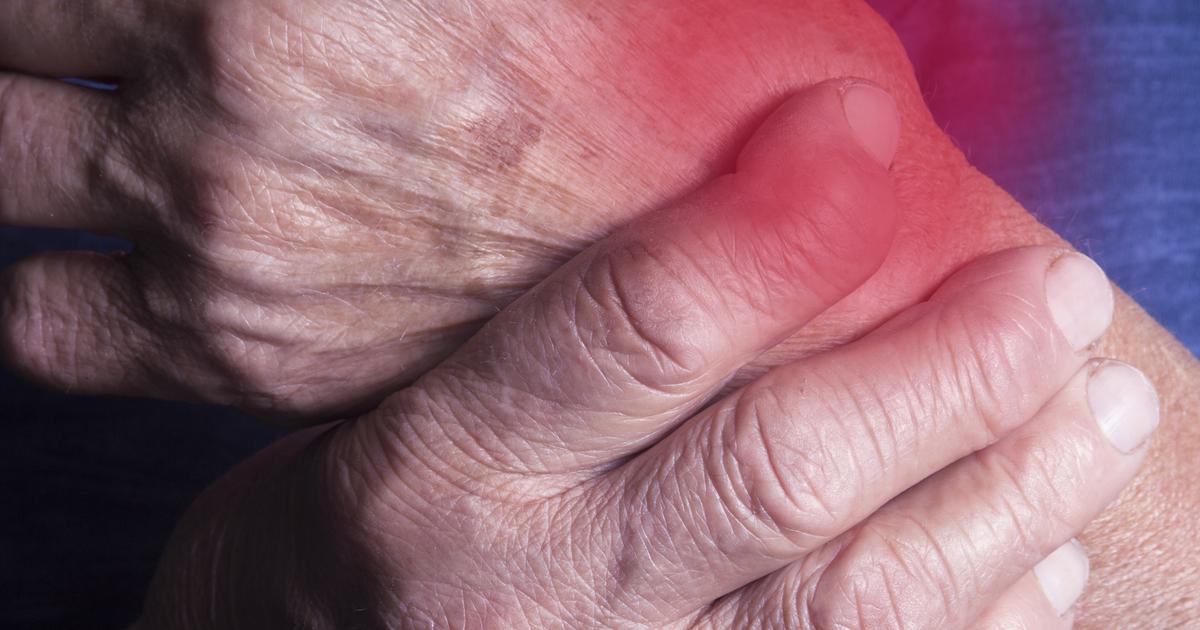
Rheumatoid arthritis can be indicative of selective IgA deficiency due to the fact both disorders are associated with each other. Patients with selective IgA deficiency may produce a small quantity of immunoglobulin A that induces the production of anti-IgA antibodies. These antibodies are the result of a defective immunological response analogous to the incidence of rheumatoid factors in individuals who have autoimmune disorders such as rheumatoid arthritis. Between twenty-five and thirty-three percent of selective IgA deficiency patients are also affected by an autoimmune disorder.
Individuals affected by rheumatoid arthritis have immune systems that produce antibodies and T-cells that mistakenly attack the tissues of the synovium or lining of their joints. This immune response results in redness, swelling, pain, bone deformities, and bone erosion in the affected joints. A patient's smaller joints are typically impacted by rheumatoid arthritis at first, like the joints in the toes, feet, fingers, and hands. The disease then progresses on to affect the knees, elbows, shoulders, wrists, ankles, and hips.
Chronic Diarrhea

Chronic diarrhea is a common symptom seen in individuals affected by selective IgA deficiency. The most extensive lymphoid organ in the body, the gastrointestinal tract depends on the immune component immunoglobulin A to help protect it from pathogen-induced infections. The gastrointestinal tract is exposed to parasites, viruses, and bacterial antigens on a constant and regular basis. The balance between tolerance of the presence of good gut bacteria and the presence of detrimental pathogens is carefully maintained by the immune factors such as immunoglobulin A that are present in a healthy digestive system.
This balance is impaired and out of sync in selective IgA deficiency patients. The autoimmune factors present in some cases of selective IgA deficiency can result in the incidence of gastrointestinal related autoimmune disorders such as inflammatory bowel disease. Between five and fifty percent of individuals affected by primary immunodeficiencies develop gastrointestinal disorders that produce symptoms including chronic diarrhea.
Allergies

An individual who experiences frequent allergies may be affected by IgA deficiency. Immunoglobulin A is a type of antibody produced by the immune system that is critical for the proper function of the mucous membranes. Mucous membranes keep foreign substances and pathogens out of the internal tissues of the body and are located in the mouth, esophagus, nose, stomach, intestines, lungs, and vagina. Allergies occur when an allergen enters the airways and triggers an abnormal immune system reaction.
Immunoglobulin A helps prevent inflammation by populating the mucous membranes around an individual's body and protecting them. It is this mechanism that is disrupted in selective IgA deficiency patients, making them more vulnerable to the inflammatory effects of other immune system components. The unprotected mucous membranes of an affected individual can allow allergens to reach the lung tissues and trigger an abnormal inflammatory allergic reaction.
Asthma

Asthma is a respiratory condition characterized by bronchial spasms in an individual's lungs that cause problems with breathing, produce inflammation, and increase the production of mucus. Asthma occurs when irritants make it into the lungs, and the immune system has a hypersensitive reaction to the irritant. Symptoms of asthma include wheezing, chest tightness, and coughing. The exact causes of asthma are not clear, but it is known that the inflammatory process in the lungs is what produces asthma attack symptoms.
Healthy individuals have mucus that lines the inside of their airways and lungs that helps expel and keep irritants out of the body. Selective IgA deficiency patients have mucus that does not work as well, predisposing them to immune-mediated hypersensitivity to irritants that are not immediately expelled or have reached underlying tissues.
Gluten Intolerance

An individual with selective IgA deficiency may also be affected by celiac disease, which is characterized by gluten intolerance. Individuals affected by immunoglobulin A deficiency are between ten and twenty times more likely than an unaffected individual to develop celiac disease. The unique connection stems from the fact a test for celiac disease may turn up a false negative result in an individual affected by immunoglobulin A deficiency and celiac disease.
An immunoglobulin A deficiency can cause the tests for anti-tissue transglutaminase antibodies, anti-endomysium antibodies, and anti-deamidated gliadin peptide antibodies to come up negative when the antibodies are actually present in an individual's body. Patients who have an immunoglobulin A deficiency should be tested for IgG anti-tissue transglutaminase antibodies instead of IgA anti-tissue transglutaminase antibodies because the test performed on immunoglobulin A will not provide accurate results.
Lupus

Selective IgA deficiency patients may also have an autoimmune disorder referred to as systemic lupus erythematosus, which has adverse effects on many organ systems of the body. Numerous types of autoantibodies are created in the body of an individual who has systemic lupus erythematosus against nuclear antigens deposited in multiple organs, including the kidneys, joints, and skin. The main method of treatment used for systemic lupus erythematosus patients is medications that suppress the immune system. Systemic lupus erythematosus typically manifests following an infection that has triggered its characteristic symptoms.
Those affected by selective IgA deficiency are included in the population of individuals who experience frequent infections because they are missing a critical component of their immune system. Because infection is one of the most prevalent causes of systemic lupus erythematosus, individuals who develop infections more frequently than others are at a greater risk of developing this autoimmune disease.
Inflammatory Bowel Disease

A selective IgA deficiency patient is more likely to develop or be affected by inflammatory bowel disease than a healthy individual. Inflammatory bowel disease is a condition characterized by chronic digestive tract inflammation, and it is often separated into ulcerative colitis and Crohn's disease. Both forms of inflammatory bowel disease cause a patient to experience abdominal pain and cramping, severe diarrhea, unintended weight loss, and fatigue. Inflammation in the intestinal tract develops when there is a breach in the protective mucus layer that lines the interior of the intestines.
Furthermore, the patient's immune system can attack its own digestive tissues and produce such breach and inflammatory process in the intestinal linings. Individuals affected by selective IgA deficiency have mucous membranes exposed to damage because the deficient immunoglobulin A is a critical component in mucus. The mucus layer is intended to protect the inside of the mouth, stomach, lungs, vagina, and intestines. This protection is diminished in selective IgA deficiency patients, putting them at a higher risk of developing inflammatory bowel disease.
