How To Treat Acute Disseminated Encephalomyelitis
Acute disseminated encephalomyelitis is an autoimmune disorder that affects the nervous system. More common in children than in adults, the condition causes brief episodes of severe inflammation in the spinal cord and brain, and it often develops within two to four weeks after a viral or bacterial infection. Symptoms of this illness generally include fevers, severe headaches that last for an extended period, and neurological signs such as weakness in the arms and legs, coordination difficulties, unsteadiness, drowsiness, swallowing issues, and confusion. Some patients may experience blurred or double vision, and falls might occur. MRI scans and lumbar punctures are needed to diagnose this condition.
The methods described below are recommended in the treatment and management of acute disseminated encephalomyelitis.
Intravenous Corticosteroids
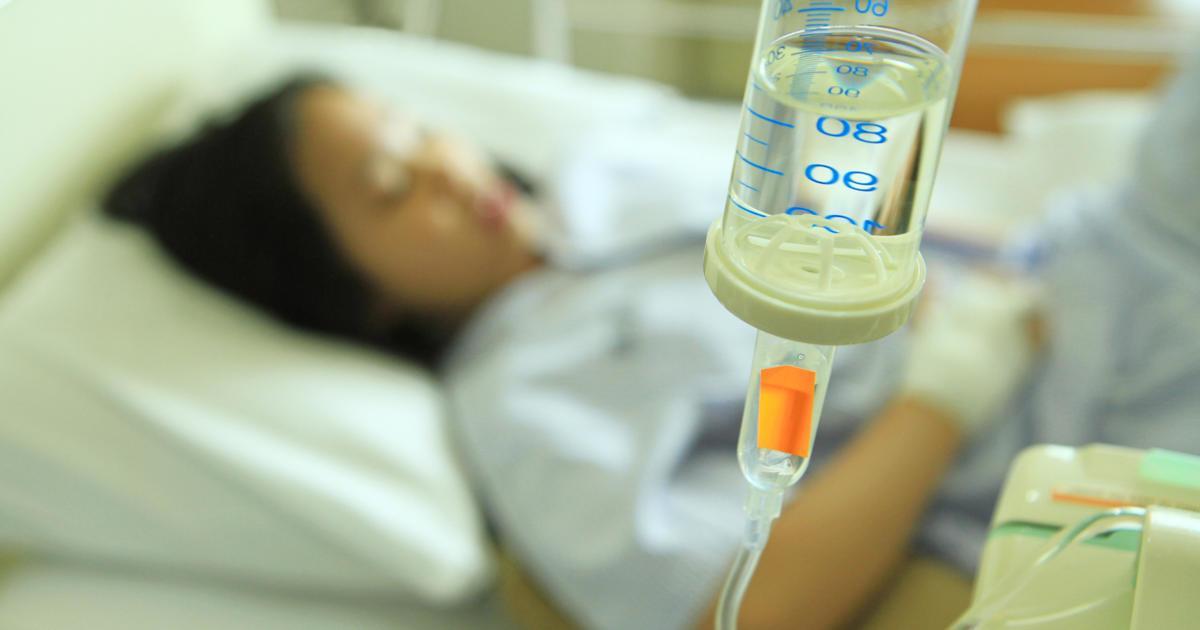
Intravenous corticosteroids are the first line of treatment for this disorder. Patients are normally started on a course of methyl-prednisolone given over five to seven days. This medication helps to reduce inflammation and promote healing after a symptomatic episode. Patients taking methyl-prednisolone may experience side effects, including irritability, anxiety, swelling of the face, facial flushing, and weight gain. Some individuals might develop a metallic taste in the mouth, and infants and young children taking this medicine could exhibit an increase in fussiness or crying. Since steroids can cause changes in blood levels, patients will need to have regular blood tests during their treatment to check for elevated glucose and reduced potassium measurements. Doctors will also ask about the patient's sleep quality; steroid use can sometimes cause disrupted sleep. After completing the course of intravenous steroids, the patient will be given a short course of oral steroids to safely taper off of these drugs.
Learn more about how to treat acute disseminated encephalomyelitis now.
Plasmapheresis

Plasmapheresis helps reduce the activity of the immune system by temporarily removing certain components of this body system from the patient's overall circulation. The procedure involves filtering the patient's blood through a machine, and it is normally performed in a hospital setting. The procedure removes specific antibodies from a portion of the patient's blood known as plasma, and it generally takes several hours to complete. Patients with acute disseminated encephalomyelitis have a plasmapheresis session once every other day over the course of ten to fourteen days.
Prior to having the first session, the patient may need to have a minor surgical procedure to insert a central venous catheter, a device that allows blood to be removed and transported into the plasmapheresis machine much more rapidly than other methods. Nurses and hospital staff will closely monitor the patient's blood pressure, temperature, and pulse during each session, and they will also check for any abnormal bleeding or signs of infection. The most common side effect of this treatment is discomfort while blood is being taken, and patients might experience a drop in platelet count that could make them more vulnerable to infections and increase the risk of bruising or internal bleeding.
Read more about treating acute disseminated encephalomyelitis now.
Intravenous Immunoglobulin
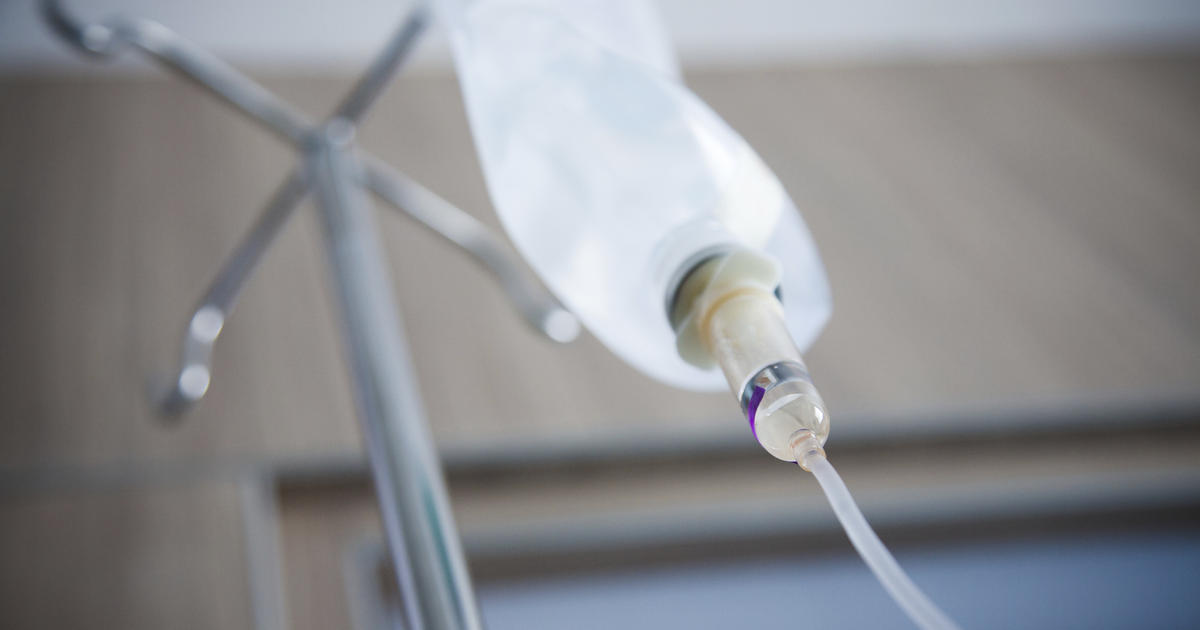
Intravenous immunoglobulin is a second-line treatment typically recommended for patients who have not responded to intravenous steroids. Immunoglobulin is a type of blood product that provides a highly concentrated dose of antibodies. The antibodies used for immunoglobulin are collected from thousands of donors and can offer patients a broad spectrum of protection from immune system attacks and foreign substances. The intravenous antibodies stop the patient's immune system from attacking itself. Intravenous immunoglobulin treatments are given in certain doctor's offices and in hospitals, and the infusions usually take around an hour. The dose is calculated based on the patient's weight. Patients receiving this treatment for acute disseminated encephalomyelitis are given more immunoglobulin per dose than those receiving this treatment for other conditions; however, individuals with acute disseminated encephalomyelitis typically need fewer treatments overall.
Doctors will be able to properly assess the effectiveness of immunoglobulin treatments after as little as one dose, and patients will be informed as to if they will need additional immunoglobulin or if they should try other treatment options instead. Shortly after receiving immunoglobulin, some individuals may develop chills, nausea, vomiting, fatigue, and headaches. They could also experience fevers, muscle aches, or pain in the joints. These side effects are most likely to happen if the patient is receiving treatment for the first time or switching to a new brand of immunoglobulin. Additional side effects that may develop within two days of treatment include kidney issues, skin rashes, and reduced platelet counts. Very rarely, a patient might develop a blood clot, and individuals receiving treatment will be told about the potential signs of a clot. Patients should immediately inform their treatment center about any new or worsening side effects.
Get more details on how to treat acute disseminated encephalomyelitis now.
Physical Therapy

Physical therapy can be beneficial in helping patients regain muscle strength and coordination after an episode of acute disseminated encephalomyelitis. During a physical therapy session, the therapist will teach the patient certain stretches and movements that can increase range of motion, flexibility, and endurance. Some exercises may be performed with the patient's own body weight as resistance, and elastic bands can be added to increase resistance and grip strength. Since acute disseminated encephalomyelitis may cause problems with walking and other voluntary muscle movements, therapy sessions might concentrate on building balance skills and teaching the patient effective ways to use stairs and walk with a more even, comfortable, and steady gait.
Continue reading to reveal more acute disseminated encephalomyelitis treatments now.
Speech Therapy

Speech therapy is frequently recommended for individuals who have experienced swallowing difficulties during their illness. During the initial speech therapy session, the therapist will assess how well the patient's muscles move while they attempt to swallow. The doctor may observe the patient eating and drinking as well. Using this information, the doctor will be able to suggest specific exercises tailored to the patient's needs. For example, exercises to strengthen the tongue might be advised, and patients could also be shown methods that will build strength in the muscles responsible for chewing. The therapist may recommend adjustments in the patient's head posture and the way they sit while eating, as these changes could make it easier for the patient to eat. Speech therapy sessions generally include advice about choosing thicker drinks and softer foods that could promote easier swallowing too.
