Diagnosis, Prevention, And Treatment For Diabetic Ketoacidosis
Diabetic ketoacidosis, diabetic acidosis, is a serious complication related to diabetes. The condition is considered a medical emergency and results from an excessive amount of ketones in the bloodstream. Symptoms of diabetic ketoacidosis include weakness, abdominal pain, blurred vision, shortness of breath, nausea, vomiting, excessive thirst for more than one day, and confusion. Frequent urination, dry skin or a dry mouth, and muscle stiffness could also be present. Some patients may notice their breath has a fruity odor, and it may also smell like acetone, commonly found in nail polish remover. Patients should see their doctor if they are having trouble keeping liquids down and if their blood sugar readings are above three hundred. They should also see a doctor if ketones, which can be detected with at-home-urinalysis testing strips, are present in their urine. If left untreated, diabetic ketoacidosis may lead to coma, which can cause death. The steps outlined below may be helpful in the prevention and treatment of diabetic ketoacidosis.
Electrolyte Replacement

Electrolyte replacement is done to replenish electrolytes that may be lost due to the frequent urination and vomiting caused by diabetic ketoacidosis. These symptoms often lead to dehydration, which can cause the body's electrolytes to become unbalanced. Electrolytes are ionized substances within the body with the capacity to conduct electricity. The proper balance of electrolytes keeps the cardiovascular system and other body systems functioning correctly. Common electrolytes include sodium, potassium, bicarbonate, and chloride. Doctors can measure electrolyte values with blood tests. If electrolytes are low, they can be replaced through certain foods and drinks, such as sports drinks, electrolyte replacement drinks, and water with added electrolytes. Foods high in electrolytes include bananas, avocados, dates, beans, lentils, spinach, and potatoes. If at-home measures are not enough to adequately restore electrolyte levels, doctors can do so through the use of IVs at the hospital.
Keep reading for another method of treating diabetic ketoacidosis.
Fluid Replacement

As with electrolyte replenishment, fluid replacement is also necessary with this condition due to the dehydration it causes. Fluids allow the body to remove the excessive ketones from the blood, reducing its acidity. They also help reduce blood glucose levels. If the patient is alert and able to drink, they should be encouraged to drink as much fluid as is tolerable, ideally in the form of water. Orange juice or other sugary drinks like soda should be avoided as they will raise blood glucose levels even more. Patients in more advanced stages of diabetic ketoacidosis should be taken to the hospital. Doctors there will be able to provide fluid replenishment intravenously, and they may also recommend patients continue drinking fluids by mouth while they are receiving the intravenous ones. Intravenous fluids will be given until doctors determine the patient is adequately rehydrated, a process that can take several hours.
Get to know the next option for treating ketoacidosis now.
Insulin Therapy
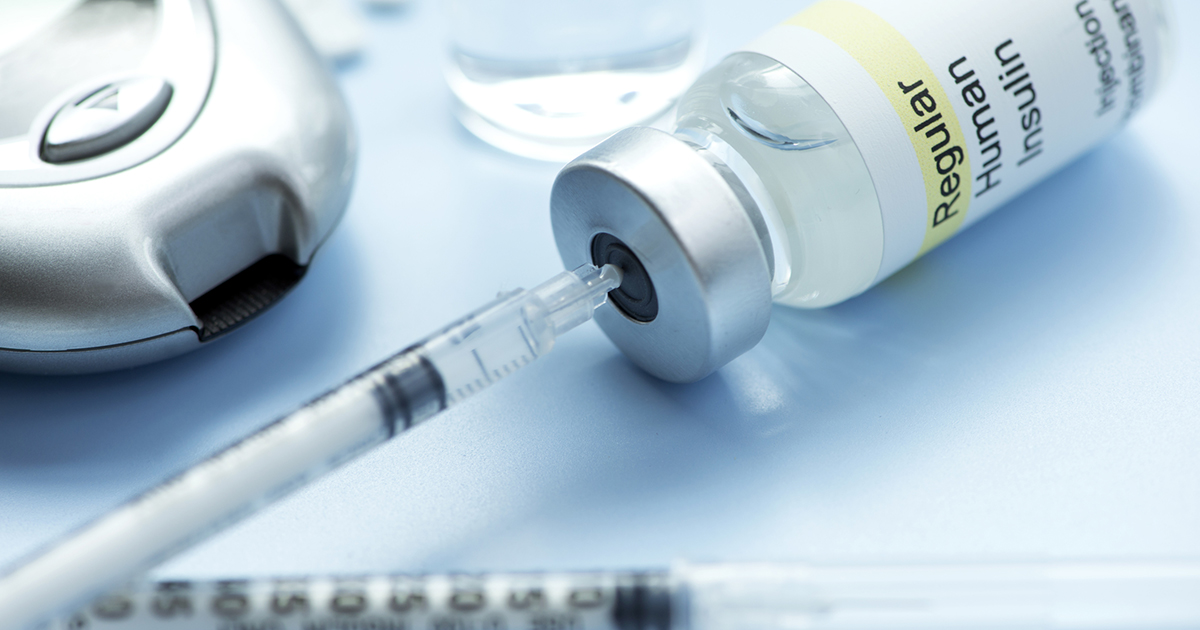
Insulin therapy is used on a daily basis by many diabetes patients. Insulin is a hormone that regulates blood glucose. In type 2 diabetes, the pancreas is still capable of producing insulin, but it does not produce enough of it. Thus, patients with diabetes must often use insulin injections to achieve adequate levels. Patients with diabetic ketoacidosis typically have very high blood glucose levels, often above three hundred mg/dL. Insulin is key to reversing the process that leads to this dangerous condition. It is generally given in the hospital to allow for appropriate blood glucose and cardiac monitoring. Patients are given insulin intravenously until their glucose levels fall to below two hundred mg/dL and ketones are no longer present in their blood. Once blood glucose is back within the normal range for diabetes patients, they may be allowed to go home. They will be given instructions about when and how to resume their normal insulin injections at home. Patients should always take their required doses of insulin on the schedule set by their doctors to prevent diabetic ketoacidosis.
Understand how to properly prevent and treat diabetic ketoacidosis now.
Consistently Test Blood Sugar

Patients with diabetes need to consistently test blood sugar levels throughout their lives. Regular testing can help manage medication doses and allow patients to plan their meals more easily. This regular monitoring can alert patients to when their numbers are dangerously high or low, enabling them to receive medical attention urgently and before serious complications develop. Blood sugar levels are routinely tested at home with a blood glucose meter, test strips, and a lancet device. Patients draw a drop of blood from their finger or forearm and place it on a testing strip. After inserting the strip into the meter, a glucose reading will be displayed. Depending on the type and severity of a patient's diabetes, doctors may recommend testing as often as ten times per day. Patients with more minor forms of the condition may be able to test two or three times a day, and others who do not require insulin may be able to check their glucose readings once every two or three days. Patients who have trouble testing regularly can sometimes use a special monitor placed under the skin of the upper arm by a nurse. This device continuously monitors glucose and is typically left in place for up to a week. Doctors routinely use it for diagnostic purposes and when they are considering making medication changes for patients.
Reveal the next method of treating and preventing diabetic ketoacidosis now.
Take Medication As Directed
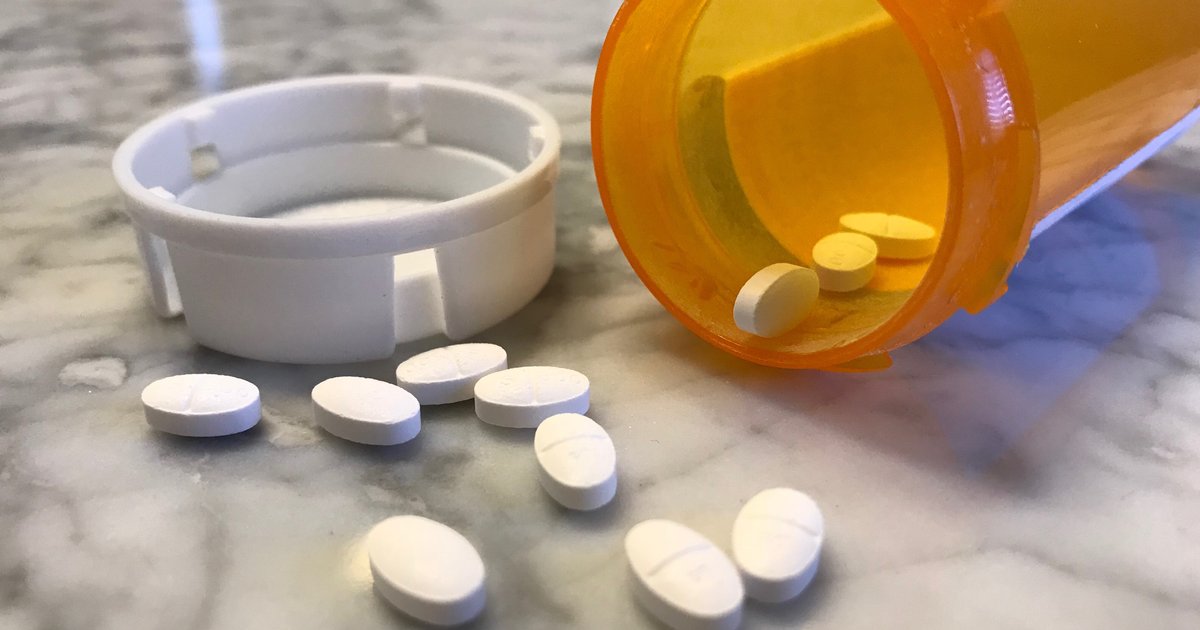
Patients with diabetes should always take medication as directed by their doctors to prevent diabetic ketoacidosis as well as other complications of diabetes. Some patients may be on multiple medications, including oral tablets and injectable medicines, and the dosing schedule can sometimes be confusing. Patients may need to use a pill organizer for their oral medications, and keeping a log of their injections can help. Some online apps are designed to help with medication reminders, and wearable fitness watches often do too. Some pharmacies will provide pre-packaged bags containing all of the patient's medicines sorted by day and time. If they are having trouble understanding medication dosages or schedules, patients should always ask their doctors for help. Any side effects should be reported so any available alternative medications can be explored.
Get more information on preventing, treating, and even diagnosing diabetic ketoacidosis now.
Ketone Level Tests

Ketone level tests may be used to diagnose an individual with diabetic ketoacidosis and treat it in current patients. Ketones can be tested and measured through an affected individual's urine and blood. An individual's physician may test for ketones in the urine or blood if the level of glucose in the blood exceeds 240 milligrams per deciliter or symptoms of diabetic ketoacidosis are present. Three different types of ketones exist in an individual's blood referred to as acetone, 3-β-hydroxybutyrate, and acetoacetate. Blood tests for ketones show if all the ketone levels are low to normal, medium to moderate, or high to large. A patient who has a high glucose level on a blood test, as well as high ketone levels on a ketone test, will be diagnosed with diabetic ketoacidosis. Some diabetes patients have a regular issue with ketone buildup in their blood and may be instructed to use urine ketone tests regularly as part of their treatment plan.
Read more about diagnosing and treating diabetic ketoacidosis now.
Urinalysis
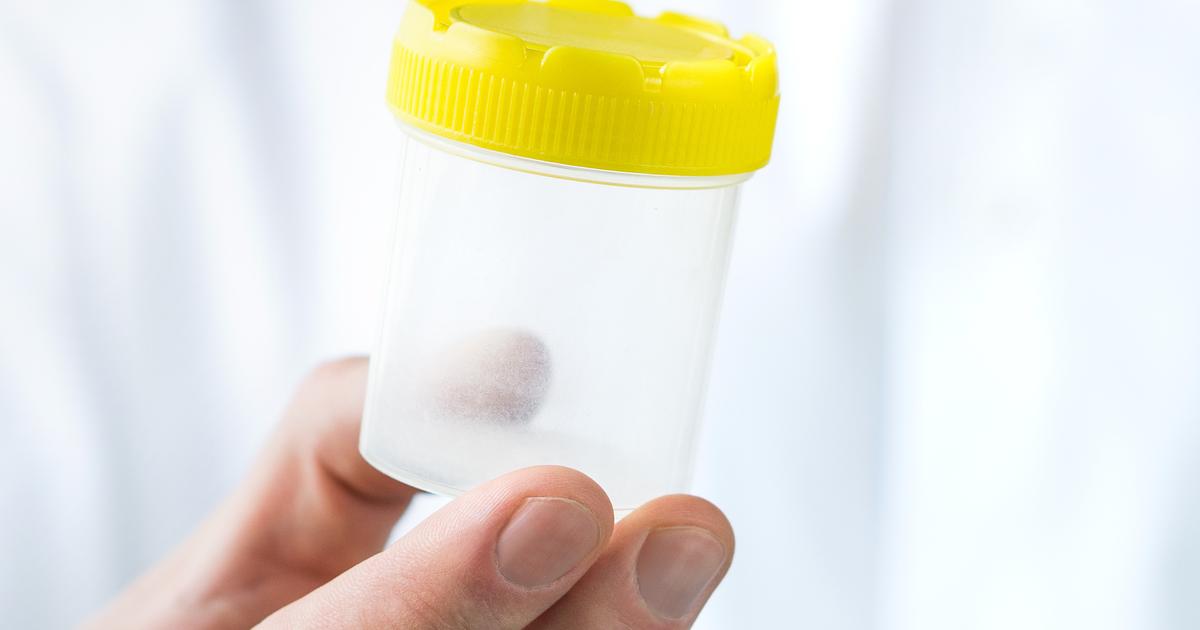
An individual who is suspected of having diabetic ketoacidosis may need to undergo a urinalysis to check for ketone presence in their urine. A diabetes patient who does not manage their glucose levels properly will develop diabetic ketoacidosis because there is not enough insulin to carry out the process of ATP production from glucose. When the cells cannot produce cellular energy from glucose because there is no insulin present, they have to utilize fats to produce energy instead. The process the cells use to make energy out of fats is referred to as ketogenesis in the medical community. Ketones are acids produced as a byproduct of the ketogenesis process. When insulin is not supplied to the body of a diabetes patient, their body will carry out excessive ketogenesis processes to produce energy the cells can use. An individual's kidneys are responsible for filtering waste products from their blood like ketones so they can be excreted through the urine. High levels of ketones in the blood are directly correlated with high levels of ketones in the urine.
Read more about treating and preventing diabetic ketoacidosis now.
Check Ketones Regularly
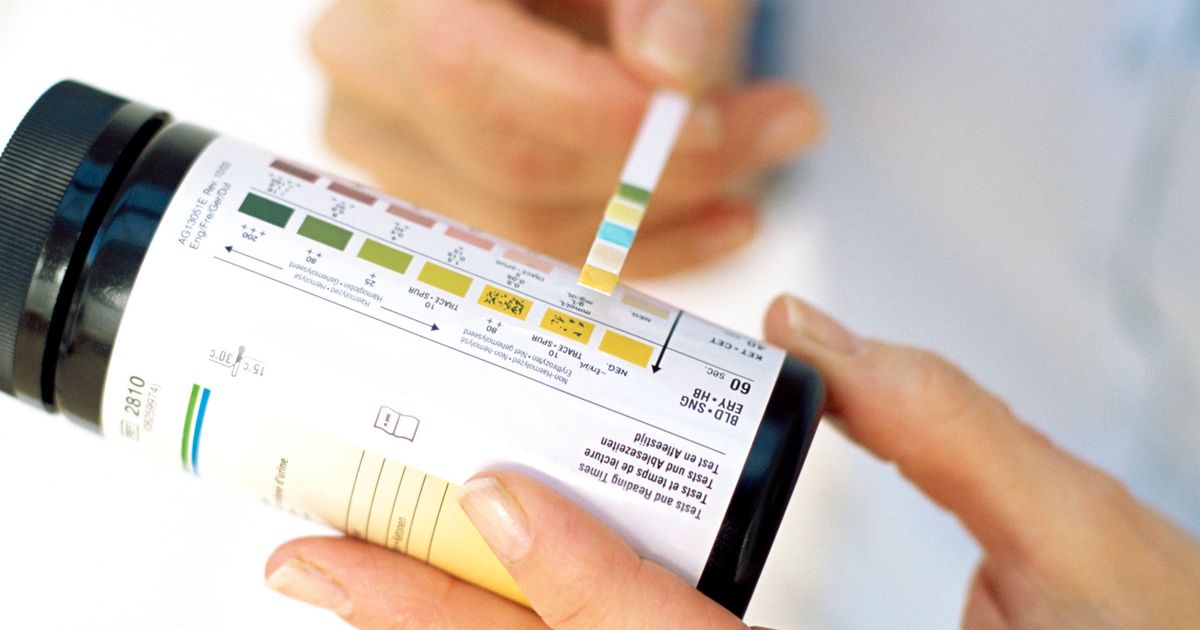
Aside from regular ketone checks on their blood and urine at their physician's office, an individual may need to check for ketones regularly at home to keep their diabetes from progressing to diabetic ketoacidosis. The American Diabetes Association recommends that each diabetes patient check their urine ketone levels when their blood sugar levels exceed 240 milligrams per deciliter. When individuals who have diabetes become sick or ill, it is recommended that they check their ketone levels by their blood monitor or urine dipstick every four to six hours. An individual who has diabetes and feels they are experiencing symptoms of diabetic ketoacidosis such as frequent urination, excessive thirst, abdominal pain, nausea, vomiting, fatigue, weakness, confusion, fruity-smelling breath, and shortness of breath should also use their blood monitor or urine dipsticks to check their ketone levels. Being proactive and having knowledge of when ketone levels rise can help an individual prevent complications caused by a state of ketoacidosis.
Uncover more ways to prevent and treat diabetic ketoacidosis now.
Exercise Regularly

A diabetes patient can help prevent the development of diabetic ketoacidosis by exercising regularly at a mild to moderate level. When an individual is exercising, the cells use up more glucose than they would otherwise if the levels of insulin in the body are stabilized. Regular exercise can contribute to an overall lower blood glucose level over time and help prevent sudden blood sugar spikes. High blood sugar levels that are consistent over time are what causes the development of diabetic ketoacidosis, so regular exercise can reduce someone's risk of experiencing ketoacidosis. However, individuals need to understand exercising is dangerous if they are already in a state of diabetic ketoacidosis. An individual who has a high level of glucose in their blood before when they intend to exercise should test for ketone presence in their blood and or urine before they begin their workout. It ketones are present, a patient should avoid vigorous exercise and contact their physician.
