Causes And Risk Factors Of Nonalcoholic Fatty Liver Disease
A healthy liver contains a limited amount of fat. When fat accumulates to over five percent of the liver's weight, patients have a fatty liver. A fatty liver can induce an inflammatory response, which causes liver tissue damage. The body repairs this damage with scar tissue, which can progress to cirrhosis and cause the liver to fail. Symptoms of fatty liver disease typically do not manifest until late-stage liver scarring. Most cases are discovered with a routine blood test or when the liver appears abnormal on imaging tests conducted for other reasons. To confirm the diagnosis of nonalcoholic fatty liver disease, further blood tests, more imaging tests, and a liver biopsy may be performed.
Nonalcoholic fatty liver disease treatment focuses on preventing further liver damage and failure. Patients should engage in healthy weight loss to improve their liver health. This may include going on a sustainable weight loss diet. Individuals can also benefit from regular exercise as a treatment for fatty liver disease. Of course, they should understand the causes and risk factors as well and work to minimize them.
Obesity

Their obesity can cause nonalcoholic fatty liver disease in an individual. Only ten to fifteen percent of individuals who have a healthy range body mass index have this disease. In contrast, seventy percent of those with a body mass index considered obese have nonalcoholic fatty liver disease. Excess fat is deemed the most prevalent proven cause of nonalcoholic fatty liver disease in obese individuals.
Individuals who are obese consume large amounts of fat, have a body that produces an excess amount of fat, or cannot metabolize fats very efficiently. When individuals consume more fat than their bodies require and can metabolize, the excess fats are put into liver cells for storage. More fat tissue in the liver due to obesity makes an individual more likely to have an adverse immune reaction to the extra fat, which can cause liver damage. Any mechanism that puts more fat in the body than what is needed can cause obesity and fat deposition in liver cells, resulting in nonalcoholic fatty liver disease.
Hyperglycemia
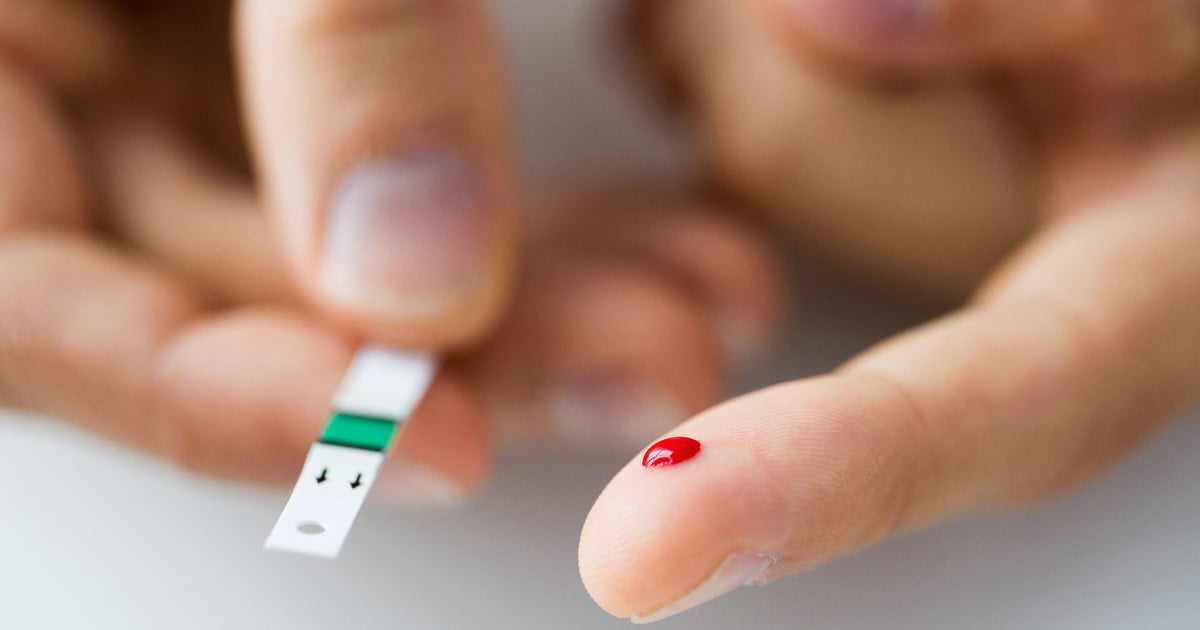
Chronic states of high blood sugar in an individual can cause them to develop nonalcoholic fatty liver disease. Hyperglycemia is defined by an elevated level of sugar in the blood. When large amounts of sugar are consumed, the intestines absorb it into the bloodstream, and blood glucose levels rise. As blood sugar rises, insulin is secreted by the pancreas to transport the glucose to numerous body tissues, including muscle and liver cells. Once glucose reaches the liver, it is converted into triglycerides. The triglycerides hang around in the liver, and some are transported to the adipose tissue or fat tissue around the body for storage.
Frequent states of high blood sugar cause this process to repeat itself excessively, producing significant fat amounts. Glucose builds up in the blood when the liver cannot metabolize the consumed sugars into fat fast enough. All of this occurs when the cells have become resistant to insulin. Fat accumulates in the liver because the fatty tissues become maxed out and deposit fat back into circulation, returning to the liver. This mechanism is what causes an individual with hyperglycemia to develop nonalcoholic liver disease.
Insulin Resistance
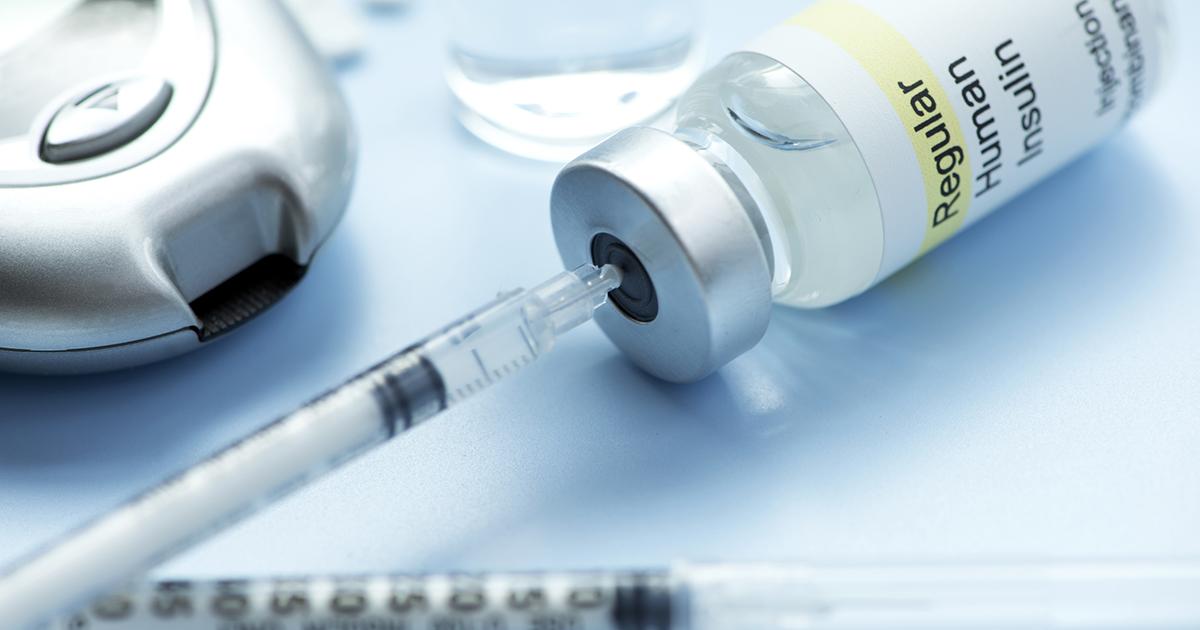
Nonalcoholic fatty liver disease can be caused by insulin resistance in an affected individual. Insulin is a hormone the pancreas produces that moves glucose in the blood to the cells that need it to produce energy. Insulin resistance occurs due to several mechanisms and means the cells do not respond appropriately to rising insulin levels. The pancreas has to make larger amounts of insulin to remove sugar from the blood effectively. After repeating this process over time, the pancreas will no longer produce enough insulin to keep blood sugar levels in a healthy range.
Insulin is essential to reduce the compound required for the adipose cells to release the fatty acids stored within them. In states of starvation, the process of fat release, transport, and conversion to glucose in the liver is imperative. However, insulin resistance in non-fasting conditions causes fatty tissues to release fats back into the blood when the amount of fat exceeds a certain level. The extra fat is then taken up by the muscles and redeposited in the liver, which might cause nonalcoholic fatty liver disease.
High Triglycerides

High triglycerides have been implicated as the cause of nonalcoholic fatty liver disease in some individuals. Triglycerides are a type of unused fat calories converted to be stored until the energy is needed later. High triglycerides in the blood are indicative of building resistance to insulin. Extra sugars and calories are converted and stored in fat cells as triglycerides until the body needs them. In certain circumstances where the body needs them, a mechanism is used to release the fat tissues' triglycerides to be converted to glucose for energy.
Insulin is responsible for stopping the inappropriate release of triglycerides from the adipose cells into the blood. However, when the fat cells ignore insulin's actions, triglycerides in the blood rise because the latter cannot successfully contain them within adipose tissue. The elevated triglycerides in the blood begin depositing in liver cells since they have nowhere to go. When triglycerides are elevated in the blood, it indicates an excess amount of fat that is not being appropriately metabolized, stored correctly, or otherwise with which it has been dealt. High triglycerides are common in individuals who have chronic high blood sugar.
High Cholesterol
Their high cholesterol levels can cause an individual's nonalcoholic fatty liver disease. There are two different kinds of cholesterol found in an individual's body. Low-density lipoprotein cholesterol is the type that binds with other types of fat and often results in the development of plaque in the blood vessels. High-density lipoprotein cholesterol helps move low-density lipoprotein cholesterol out of the blood vessels. The liver manages cholesterol by synthesizing it to be transported to other cells, but it also removes excess cholesterol from the body. The liver does so by converting the cholesterol to a substance called bile salts, which are then synthesized into bile.
Bile moves into the gallbladder and then the intestine when needed for digestion, and the remnants of the bile following digestion are expelled through stool. The liver produces the cholesterol the body needs, so dietary cholesterol contributes to excess. When cholesterol is being consumed faster than the liver can recycle it, it builds up in the liver's cells. This mechanism can result in nonalcoholic fatty liver disease.
Metabolic Syndrome

Another risk factor of nonalcoholic fatty liver disease is metabolic syndrome. This is a group of agents that considerably increases an individual's chances of developing health issues such as type 2 diabetes and chronic kidney disease. The liver determines metabolic abnormalities. Triglycerides and glucose, two crucial metabolic syndrome elements, are excessively produced in individuals with a fatty liver.
Obesity also increases the probability of chances of getting both metabolic syndrome and nonalcoholic fatty liver disease. Some common inherited metabolic disorders are Gaucher disease, Krabbe disease, Niemann-Pick disease, and Hunter syndrome. Nonalcoholic fatty liver disease is often recognized as the manifestation of liver metabolic syndrome. Even though they are not obvious, other metabolic syndrome signs include excessive urination and thirst, blurred vision, and fatigue.
Sleep Apnea

Independent of other risk factors like obesity, recent studies have shown that obstructive sleep apnea is closely linked to nonalcoholic fatty liver disease development. Research has demonstrated that the association between these two health problems is related to the degree of nocturnal hypoxemia, an abnormally low level of oxygen in the blood, in patients with sleep apnea. The latter leads to complex metabolic disturbances commonly present in individuals with nonalcoholic fatty liver disease. For instance, they may suffer from issues such as oxidative stress, overactivation of the sympathetic nervous system, and inflammation.
Sleep apnea is prevalent and is characterized by pauses of a few seconds or even minutes or by episodes of shallow breathing more than once during sleep. Most patients with sleep apnea tend to snore loudly, choke, or snort as their breathing goes back to normal.
Hypopituitarism
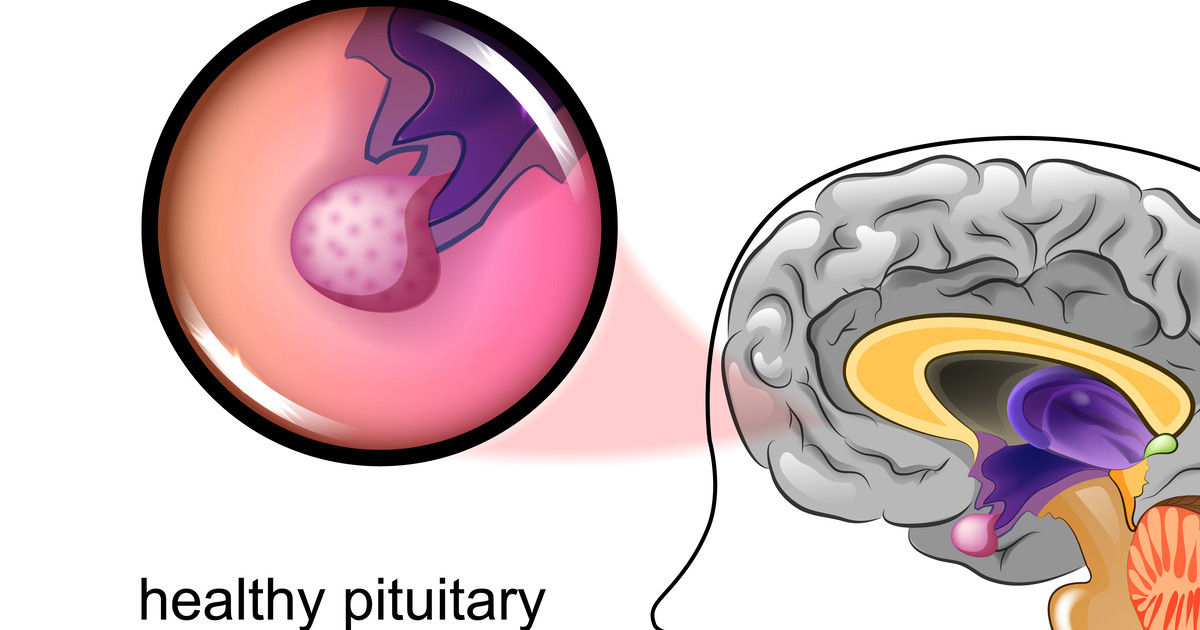
Hypopituitarism is a rare disorder in which the pituitary gland, a tiny gland situated inside the brain, cannot produce one or more hormones, or it does not produce hormones at all. This disorder, especially when it causes a lack of the growth hormone, may result in an insulin-resistant syndrome. Consequences include the development of various conditions, such as hyperglycemia and hypertension. Of course, nonalcoholic fatty liver disease is another one.
Some common signs of this condition are weight loss gain, excessive urination, thirst, dizziness, and headaches. Others are muscle aches, decreased appetite, stomach pain, nausea, constipation, vomiting, and sensitivity to cold. A doctor often diagnoses hypopituitarism after checking a patient's hormone levels or performing an MRI of the pituitary gland.
Polycystic Ovary Syndrome

Frequently, patients with polycystic ovary syndrome suffer from nonalcoholic fatty liver disease mainly because of insulin resistance, obesity, and androgen excess. According to findings published in PLOS Medicine, in female patients who suffer from polycystic ovary syndrome, the risk for nonalcoholic fatty liver is twice as high as in other women. This syndrome can bring fertility complications and might generate severe metabolic complications in the affected patient.
For this reason, females must have integrated health care and screening not only when planning their pregnancy, but throughout their whole life. Some signs of this syndrome are acne or oily skin, excessive hair growth, difficulties getting pregnant, hair loss, thinning hair on the head, irregular or no periods, and weight gain. Many individuals believe that this syndrome is painful, but that is just a myth.
Hypothyroidism
A research paper put to press in the Journal of Gastroenterology and Hepatology claims that the liver is an active participant in the chemical process that creates thyroid hormones. It suggests that untreated hypothyroidism, the insufficient production of thyroid hormone, can conduct to liver complications over time. Some of the most common causes of low functioning thyroid are the surgical removal of the gland, an autoimmune disease such as Hashimoto's thyroiditis, and radiation treatment.
The typical signs of underactive thyroid are muscle cramps, aches and weakness, depression, constipation, slow thoughts and movements, tiredness, weight gain, and sensitivity to cold. Some patients experience anxiety, body shakes, high heart rates, and hair loss as well. In other words, having a defective thyroid slows down metabolism and leads to an increase in thyroid-stimulating hormone levels. All this also generates fat accumulation in the body, which elevates the risk of developing nonalcoholic fatty liver disease.
