Serious Side Effects Of Blood Thinners
Blood thinners are designed to allow smooth blood flow through the cardiovascular system. They can prevent the formation of blood clots or keep existing blood clots from growing. Most blood thinners are prescribed to treat heart defects, certain types of heart disease, and any medical condition that increases the likelihood of dangerous blood clots. Blood thinners can reduce the risk of a heart attack or stroke in some patients. However, they can also have potentially dangerous side effects, many of which are connected to bleeding in some fashion.
In addition to understanding the benefits of taking blood thinners, patients should also be well aware of the potential side effects they may experience so they are better able to discuss options with their doctor. Learn about the common side effects of blood thinners now.
Bleeding Gums
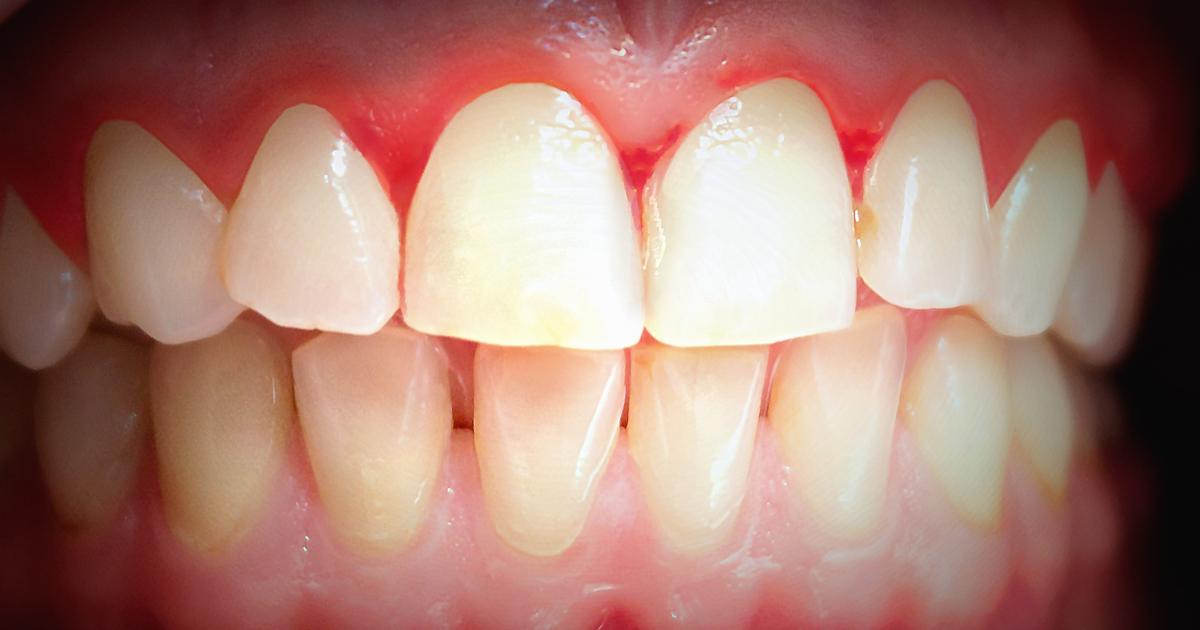
Bleeding gums, which can be a side effect of blood thinners, is usually not a medical emergency. However, affected individuals may need to call their dentist if the bleeding continues without ceasing for a significant period. While bleeding gums can occur due to blood thinners, it's also important to note other factors might be at play. For instance, individuals just starting to floss may experience bleeding gums at first, and those who brush a little too hard may also see a little bit of blood.
Of course, patients on blood thinners may experience more bleeding because of their medication, though they typically won't experience blood loss severe enough to warrant emergency medical attention. Regular and unexplained gum bleeding can be a sign of an underlying dental condition. Some types of gum disease that cause bleeding are easily treated, while others can lead to serious infection and decay.
Nosebleeds
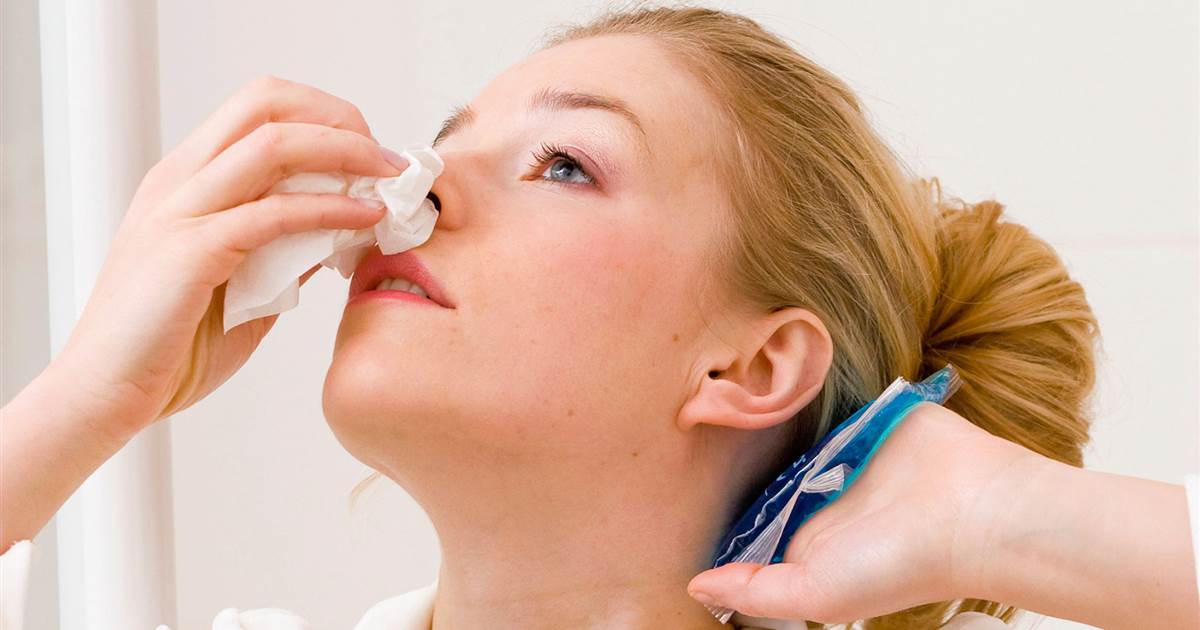
Severe nosebleeds are classed as any nosebleed that causes significant blood loss. If an individual has certain conditions that cause severe nosebleeds, blood thinners might cause dangerous side effects. The lack of clotting factors involved when taking blood thinners can make patients more susceptible to nosebleeds, and those who already experienced nosebleeds might find they increase in severity or frequency when on blood thinners.
With that said, some causes of nosebleeds can't be predicted or adequately avoided, though to comm triggers include dry air and nose picking. Dried nasal membranes are more vulnerable to infections and bleeding. To avoid nosebleeds while on blood thinners, patients should stop any picking habits and consider investing in a humidifier. They should also avoid frequent use of nasal sprays if possible. Chemical irritants can lead to nosebleeds, so affected individuals should avoid directly breathing in chemical fumes and use organic cleaning products where possible.
Dizziness

Increased bleeding is the most common side effect of blood thinners, and due to this, another possible side effect is dizziness due to an individual's blood cell count dropping below a healthy average. Individuals experiencing dizziness due to their blood thinners may also be at risk of anemia, which can come with other symptoms such as fatigue and shortness of breath.
Those who experience dizziness when taking blood thinners should speak to their doctor, who will likely do a blood test to check for potential deficiencies resulting from increased bleeding. Doctors may adjust a patient's blood-thinning medication to help deal with this issue, or add other supplements to help counteract its effects. This includes iron, which is lost when individuals bleed, and when levels are low, can cause dizziness.
Prolonged Wound Bleeding
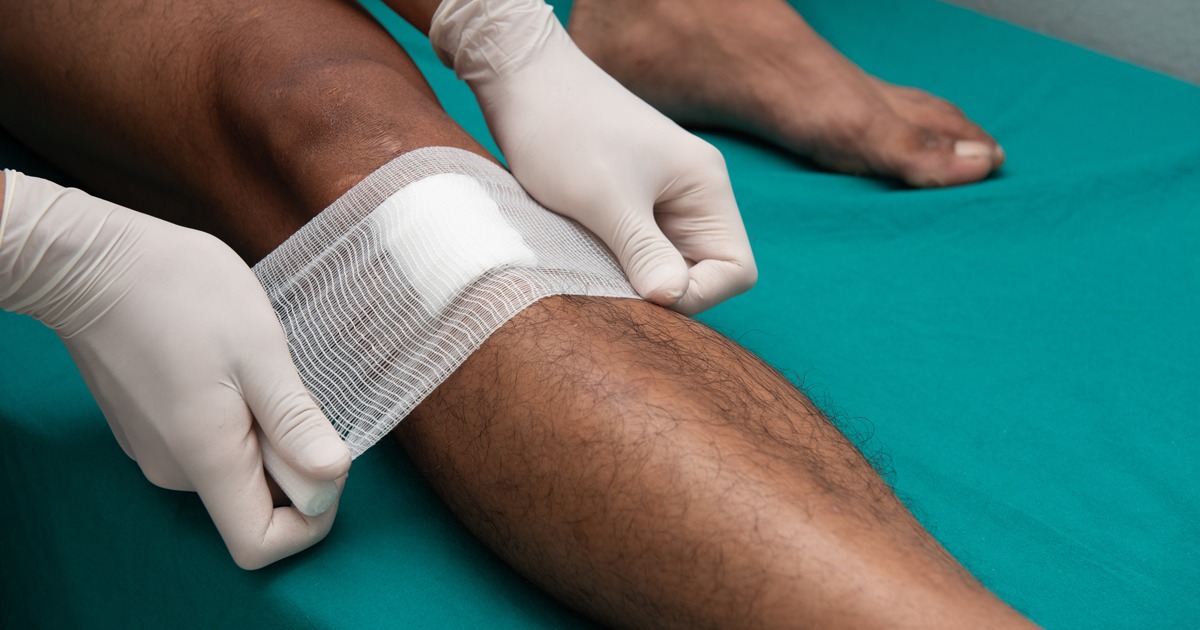
Prolonged wound bleeding is a common side effect of blood thinners, and depending on the severity of the wound, this can lead to complications from blood loss. While prolonged bleeding isn't necessarily an emergency, it can become an emergency if the wound bleeds for long enough. While individuals taking blood thinners may find superficial wounds like scratches and pinpricks bleed more than they usually do, these conditions can be treated.
If patients experience a wound deep enough or large enough to require stitches, they should make sure the doctors treating them are aware they're on blood thinners. In rare cases, blood thinners might cause internal bleeding, so patients taking blood thinners should inform their doctor about any odd bruises, strange internal symptoms, and falls or seemingly-unrelated injuries they have sustained.
Muscle Weakness

Muscle weakness can occur for various reasons in individuals taking blood thinners. Depending on the type of medication and the area of the weakness, this may or may not be a potential emergency. For instance, blood thinners can cause some individuals to develop anemia, and one of the symptoms of this condition is muscle weakness. The red blood cells are responsible for carrying oxygen and nutrients to the muscles, and when there aren't enough red blood cells, the muscles aren't being supplied with adequate nutrients or oxygen, which means they don't have usable energy and this can cause muscle weakness.
Anemia-related muscle weakness tends to pervade the entire body since it's caused by a problem with blood cell count. If an individual's muscle weakness is localized to one area, they may have a dangerous blood clot. Weakness and numbness in the lower back and extremities is an indicator of a spinal blood clot, which needs emergency medical attention.
Blood In Urine Or Stool
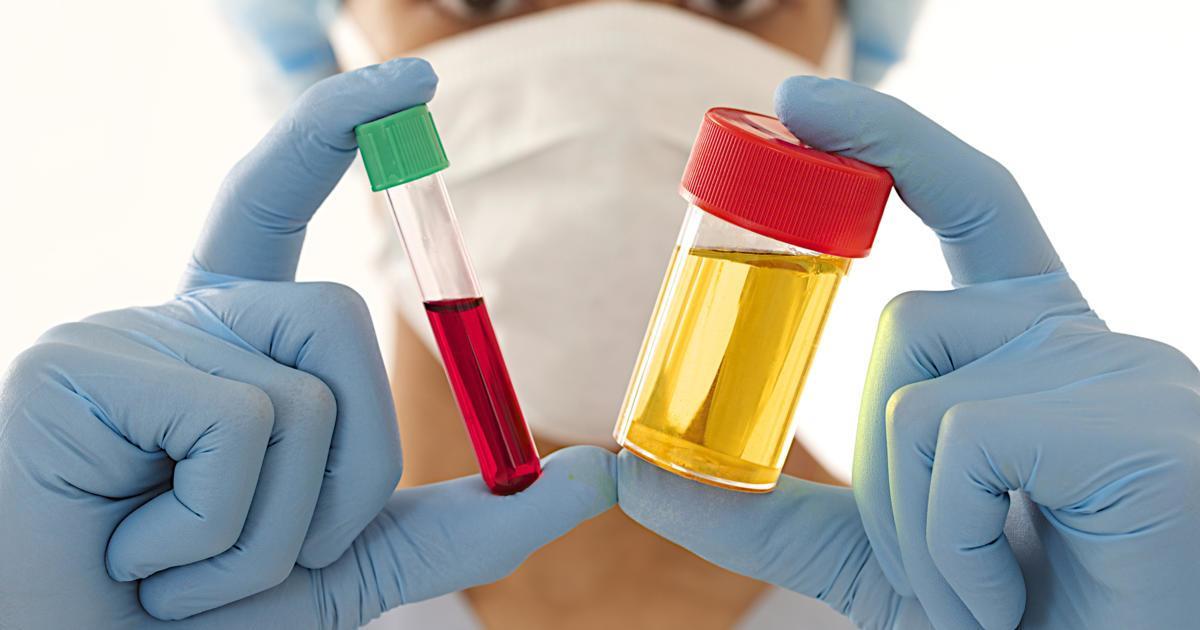
Blood in the urine or stool is a potentially serious side effect of blood thinners. It is a sign of excessive bleeding, and patients should seek immediate medical attention if they experience this side effect. When blood is present in the urine, it might appear red or brown. Blood in the stool typically makes the stool appear red or black, and patients might also see drops of blood on the toilet paper or in the toilet bowl after having a bowel movement.
To investigate blood in the urine or stool, doctors will order blood tests, and it may be necessary to take urine or stool samples and do a rectal exam. If doctors determine the symptoms are caused by the patient's medication, this may be stopped temporarily until symptoms resolve. The patient may also be switched to a different blood thinner to see if it does not cause this side effect.
Hair Loss

Some patients notice hair loss while taking blood thinners. Although this is not considered a serious side effect, it can be distressing for the patient. Patients might find their hair comes out more easily or in larger clumps when brushed, and the use of heated styling devices, hairspray, and hair gels could damage the hair and worsen hair loss. To ensure hair loss is the result of the blood thinners and is not due to an underlying medical condition, patients should speak to a doctor.
Blood tests will be performed, and patients should mention when they first noticed the hair loss and if they feel it is getting worse. The physician may want to examine the scalp to assess the extent of the hair loss. In some cases, patients may be able to take a medication that stimulates hair growth, and doctors will recommend the safest option available. It might also be helpful to consider hairstyles and accessories that could camouflage existing hair loss.
Stomachache Or Headache

A stomachache or headache might develop during treatment with blood thinners, both of which could be a sign of excessive internal bleeding. Patients who experience severe pain in their head or stomach should go to an emergency room right away. If headaches or stomachaches cause mild or moderate pain regularly, patients should make an appointment to discuss these symptoms with their doctor as soon as possible.
To evaluate these symptoms in patients who are taking blood thinners, doctors will begin with a physical examination. They will lightly press on the patient's abdomen to check for areas of tenderness, and they will also check for any areas of bruising. Imaging tests such as CT scans or MRI scans will be needed to check for internal bleeding. If internal bleeding is detected, treatment will depend on how severe it is. Mild internal bleeding may be treated with rest and symptom management, and severe internal bleeding will typically require surgery.
Unusual Bruising
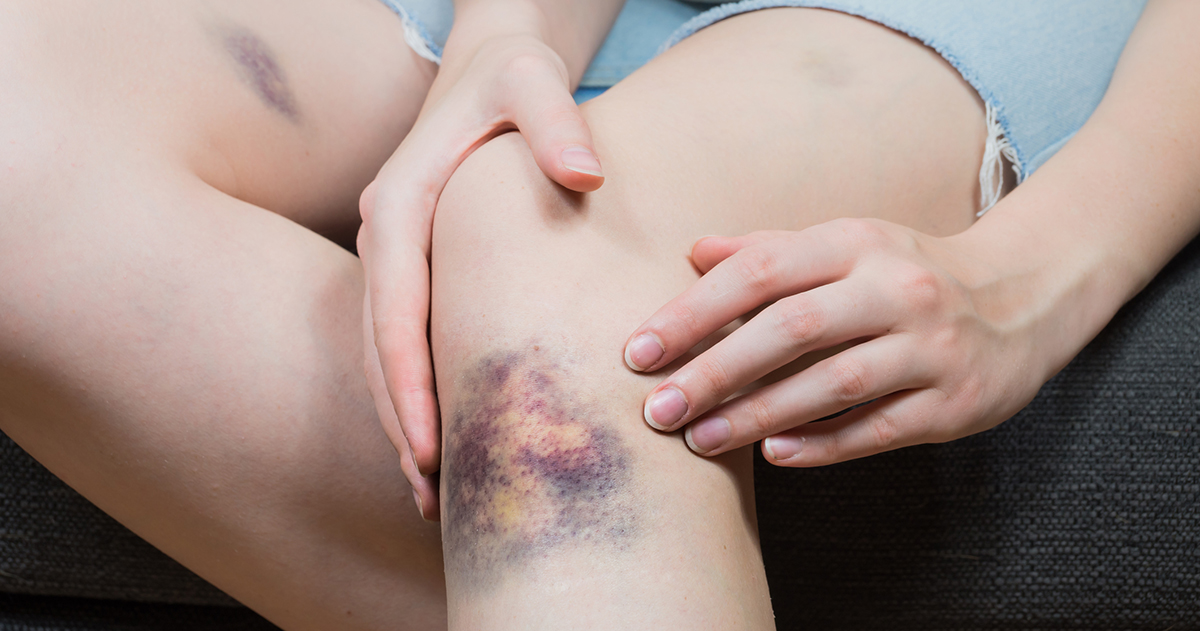
Unusual bruising is a common side effect of blood thinners. Patients often develop bruises through simple bumps or touching that would not otherwise result in bruising. For example, simply resting or lightly bumping an arm up against a table or countertop could be enough to cause a bruise. Typically, the patient cannot remember a specific injury that led to the bruise. Bruising may occur frequently in patients who take blood thinners, and the bruises could be large, painful, and slow to heal. To protect against bruising, patients should be very careful when handling sharp or abrasive objects, including kitchen utensils.
Patients might wish to wear long sleeves or long pants to provide an extra layer of cushioning against small bumps or knocks that could produce bruises. It is especially important to avoid contact sports and to take precautions to prevent falls that could result in bruising and internal bleeding. Patients should ensure they have adequate lighting at home, and any throw rugs and other trip hazards should be removed. If bruises are painful or increase in size, patients should see a doctor. It may be helpful to photograph bruises to measure how long it takes them to heal and to document their size.
Vomiting Blood

Vomiting blood is a sign of serious internal bleeding, and patients with this symptom need to seek emergency medical attention. When blood is present in vomit, it may take on a black or dark brown color similar to coffee grounds. It could also be bright red, and patients might cough up tiny flecks of blood. Once at the emergency room, doctors will do a complete evaluation to determine the cause of this symptom, and the patient must inform staff they are taking blood thinners. It can be helpful to let staff know how long the vomiting has been happening and when the blood was first noticed.
Imaging studies may be performed to check for signs of internal bleeding, and patients might need surgery to correct this. Vomiting blood may cause the patient to go into shock, which can produce additional symptoms such as dizziness upon standing, as well as shallow and rapid breathing. Patients should be taken to an emergency room by ambulance in this case.
