Common Causes And Risk Factors For Gingivitis
When plaque accumulates on the teeth and under the gums, it hardens into a substance called tartar that extends below the gum surface and causes the development of a bacterial infection. This bacterial infection causes the inflammation of the gums, or what is referred to as gum disease and gingivitis. Symptoms of gingivitis include red gums, bleeding when brushing the teeth, loose teeth, gums that have pulled away from the teeth, tender gums, pain when chewing, swollen gums, bleeding when flossing, pus between the teeth and gums, foul-smelling breath, malocclusion, poorly fitting partial dentures, and sensitive teeth. Diagnosis of gingivitis is made with gum measurements, mouth x-rays, and an oral examination. Treatment of gingivitis may include deep cleaning the teeth with the use of scaling, root planing, and laser techniques. Treatment may also include the use of antiseptic and antibiotic medications.
There are several risk factors and causes of gingivitis. Get familiar with them now.
Accumulation Of Plaque
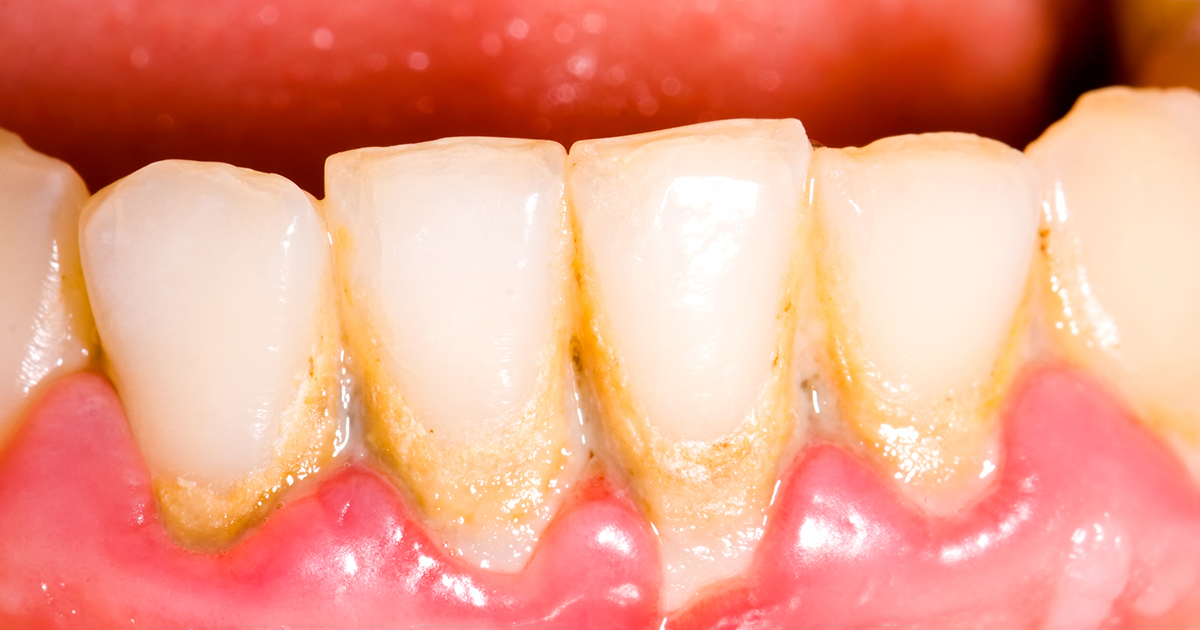
The main cause of gingivitis is the accumulation of plaque on the teeth. Plaque, which is comprised of bacteria, is a sticky film that naturally develops on teeth. The bacteria that live in the plaque on the teeth utilize sugars from the food an individual consumes to make acids that are corrosive to the tooth enamel. These corrosive acids break down the enamel of the tooth. When plaque is not removed from the teeth, it hardens into tartar, a substance that is more difficult to remove from the teeth. The bacteria and plaque continue to build off of the existing tartar on the teeth. The bacteria in the plaque produce byproducts that are toxic and irritating to the gum tissues. The gums can become puffy, red, and inflamed when tartar and plaque accumulate on the teeth and are not removed properly. Accumulation of plaque can occur in an individual who brushes their teeth every day, as it is easy to miss plaque around the gumlines. An individual can floss regularly, attend regular dental cleanings, and use products that help illuminate plaque on the teeth to ensure they are removing all of it regularly.
Read more about the risk factors and causes linked to gingivitis now.
Poor Oral Hygiene

An individual who has poor oral hygiene habits can develop gingivitis. Oral hygiene refers to the practice of keeping the teeth and mouth clean to avoid painful dental issues. Poor oral hygiene occurs when an individual fails to form good oral hygiene habits, like regular flossing and brushing of the teeth to remove any tartar and plaque stuck to them. Poor oral hygiene can also be caused by an individual's habits of using tobacco products, whether it is smoking cigarettes, using chewing tobacco, or any other method of consumption involving the mouth. There are thousands of chemicals in tobacco and cigarette smoke that throw off the entire balance and natural cleaning processes of the mouth. Poor oral hygiene can also occur when an individual consumes a diet high in acidic and sugary foods. Proper oral hygiene and the prevention of gingivitis can be accomplished by quitting smoking, consuming a healthy diet, brushing and flossing the teeth twice per day, using mouthwash twice per day, and getting annual cleanings by a dentist.
Get more details on the causes and risk factors of gingivitis now.
Poor Nutrition

Gingivitis may be caused by receiving poor nutrition through the diet. Many nutrients the body relies on to carry out its homeostatic processes come from the food an individual consumes. Many minerals and vitamins the body requires cannot be produced by the body and must come from food. In particular, the immune system requires numerous minerals, vitamins, and other nutrients to perform at an optimal level. The immune system is responsible for fighting off harmful pathogens and foreign substances that attempt to invade the tissues of the body. An individual with poor nutrition may develop gingivitis due to the impaired functioning of their immune system. Plaque that accumulates on the teeth contains different types of bacteria that attempt to use the gum tissues to enter the body. A healthy individual may not develop an infection in their gums from the bacteria in plaque because their immune system can keep the bacteria at bay. An individual who does not receive enough nutrients and vitamins in their diet will have an impaired immune system that cannot fight the bacteria off as easily.
Keep reading for more information on risk factors of developing gingivitis now.
Dry Mouth
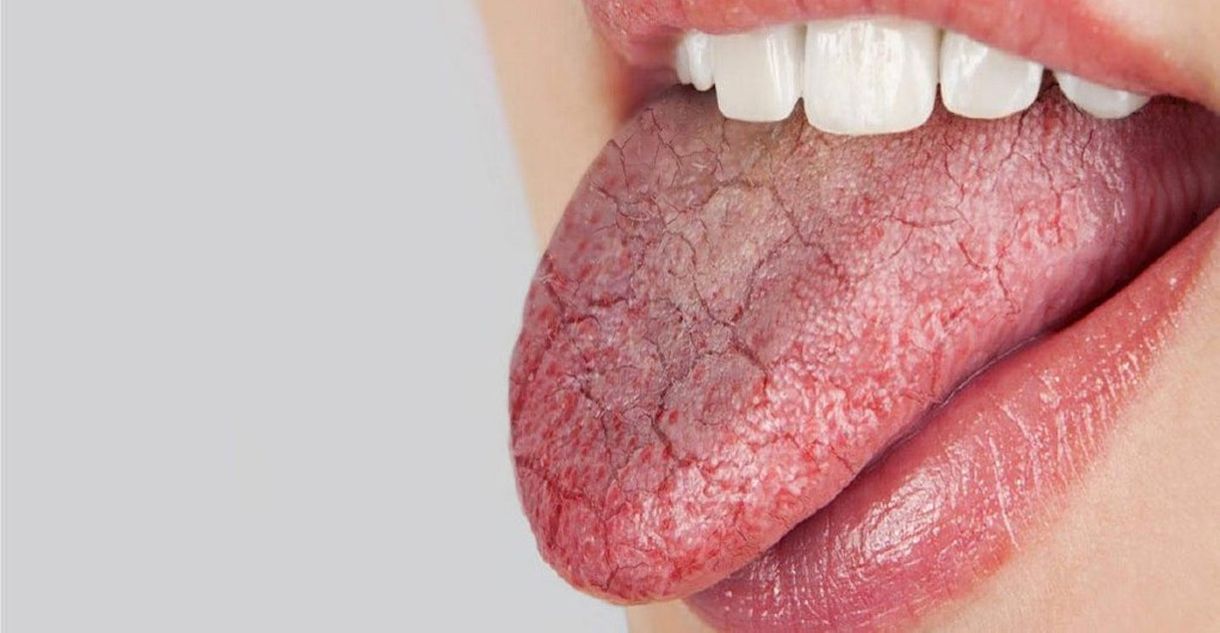
An individual who experiences dry mouth is at an increased risk of developing gingivitis. Dry mouth and xerostomia are terms used to describe when an individual's salivary glands in their mouth do not produce a sufficient amount of saliva to keep the mouth wet at all times. Several factors can cause an individual to develop dry mouth, such as taking certain medications, cancer therapy, aging, nerve damage, tobacco use, recreational drug use, alcohol consumption, metabolic disease, dementia, Sjogren's syndrome, AIDS, and snoring. Dry mouth causes an individual to have a dry or sticky feeling in their mouth, bad breath, difficulty chewing, sore throat, hoarseness, grooved tongue, changed sense of taste, difficulty speaking, thick and stringy saliva, and problems swallowing. Saliva is produced by the salivary glands in an individual's mouth and prevents the decay of teeth by interfering with the harmful acids bacteria in the mouth produce. Enzymes in the saliva help digest food and wash away food particles. Without enough saliva, it is easier for plaque and tartar to accumulate at the base of the teeth and cause the development of gingivitis.
Learn more about risk factors associated with gingivitis now.
Hormonal Changes

An individual undergoing hormonal changes is at an increased risk of developing gingivitis. Women experience unique hormonal changes that make them especially susceptible to oral health problems. Fluctuations in hormones can cause individuals to have changes in the blood supply to the tissues of the gums. Hormonal fluctuations also alter the way an affected individual's body responds to the toxins released by the bacteria that live in the plaque on the teeth. When a female hits puberty, the production of progesterone and estrogen skyrockets, producing changes in the gum tissues. During menstruation every month, a woman experiences an increase in progesterone that can cause their salivary glands to operate differently. A female who uses birth control pills is more susceptible to gum disease because of the extra progesterone they are putting into their bodies. Females who are pregnant or going through menopause are also at an increased risk because of fluctuations in hormones.
