Warning Signs Of Gum Disease
Gum disease, also sometimes referred to as periodontitis, is a serious condition that requires proper treatment. With gum disease, bacteria begin growing in the mouth, leading to damage of the gums and tissues around an individual's teeth. Failing to properly treat gum disease can cause patients to permanently lose their teeth because of the damage. Periodontitis is a slightly different condition from gingivitis, otherwise known as gum inflammation. Inflammation of the gums commonly occurs before gum disease, but not all cases of gingivitis will progress to periodontitis. Early gingivitis occurs when the gums are inflamed by bacteria in tooth plaque. Untreated gingivitis can advance to periodontitis, which causes the inner layers of bone and gum to pull away entirely from the teeth.
Bleeding Gums
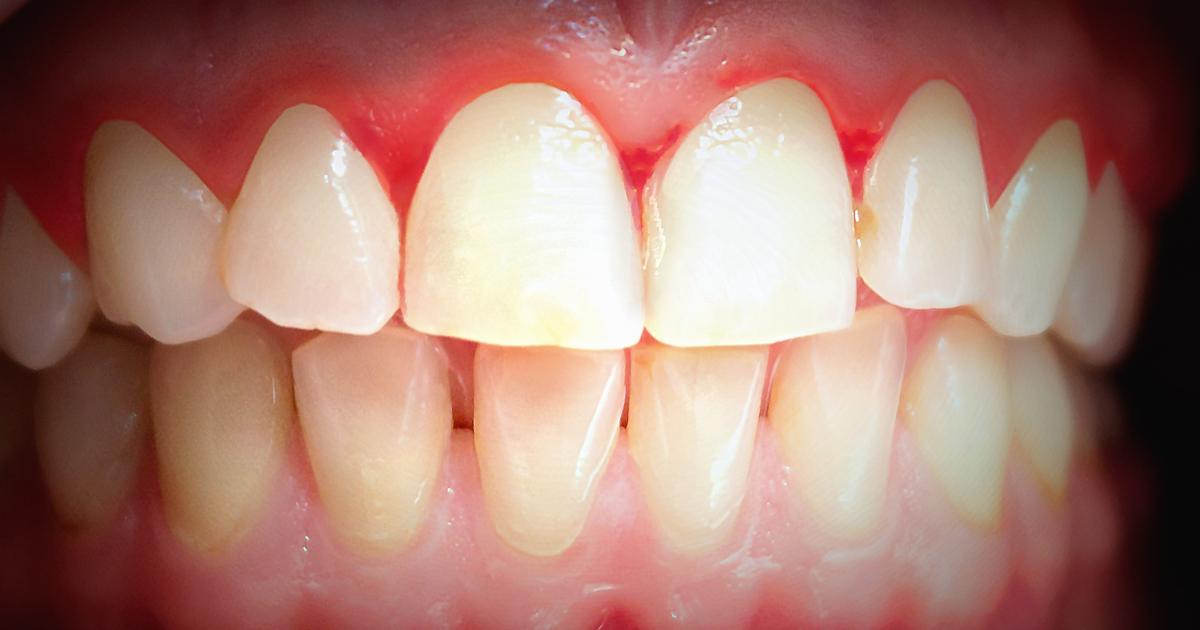
Bleeding gums are the most recognizable sign of gum disease and they can occur with both gingivitis and periodontitis. It's also possible for bleeding gums to be a sign of leukemia, certain vitamin deficiencies, or problems with blood clotting. When plaque stays on gums for too much time, the bacteria cause the gums to become inflamed. Plaque that isn't removed can harden and become tartar. If individuals have tartar on their gums, they're more likely to bleed more. Gum inflammation can cause the gums to bleed, become puffy, and feel sore. The rest of the affected individual's mouth might also feel sore. When the inflammation advances to periodontitis, patients have an infection in their gums that's causing the inflammation. As the bone and gums pull away from the teeth, hollow spaces are formed. These spaces can be filled by bacteria, which cause serious damage to both teeth and gums. If individuals think they may have periodontitis, they should see a dentist or doctor right away. Failing to treat periodontitis in time can cause teeth to become loose and fall out.
Swollen Or Tender Gums
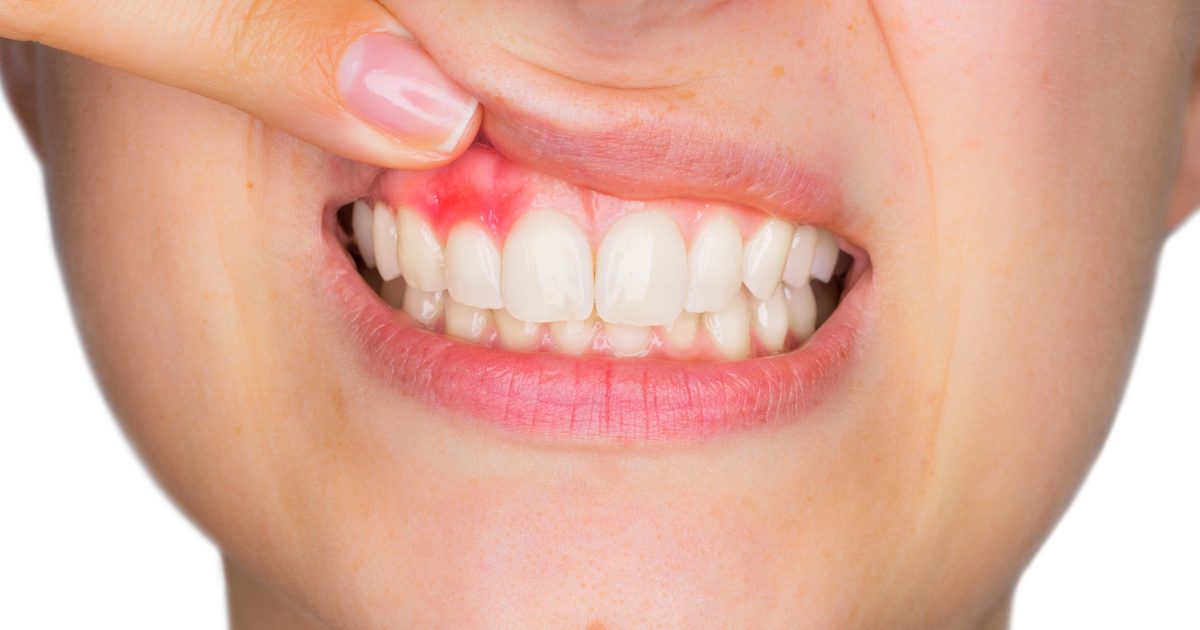
An individual's gums may become tender or swollen if they have gum disease, and they may also look redder than usual. Some patients don't experience pain in their gums as gum disease progresses, even when the disease reaches its late stages. If individuals notice their gums are swollen and red, but they aren't feeling tenderness or pain, it's still a good idea to talk to a dentist. Some patients experience gum disease throughout their gums, but others only have certain teeth affected. Tooth-specific gum disease will often affect the molars. Periodontists and dentists are the only professionals specifically trained in how to diagnose and manage gum disease. Gingivitis and periodontitis can both cause swelling and tenderness in the gums. With gingivitis, the swelling is due to inflammation. Swelling may become worse when the disease progresses to periodontitis, since there is an underlying infection causing further inflammation. Patients can stop gum disease from causing further damage by practicing proper plaque control and seeing a dentist for cleanings twice yearly.
Chronic Bad Breath

Poor dental hygiene is often the cause of bad breath, but other issues can lead to bad breath, and certain foods and lifestyle habits can worsen chronic bad breath. Any foods with strong odors can cause individuals to have worse breath than usual. This odor cannot be eliminated until the foods have completely passed through the digestive tract. If individuals don't floss and brush their teeth daily, bacteria are more likely to grow on their gums and between their teeth. The bacteria is what causes bad breath. If individuals use an antibacterial mouthwash, they may be able to reduce bacterial growth in their mouth. Persistent bad breath can indicate gum disease, especially if it continues even after individuals brush their teeth. The bacteria in plaque lead to gum inflammation, and when the disease progresses to periodontitis, the infection in the pockets of the gums may cause bad breath.
Receding Gums
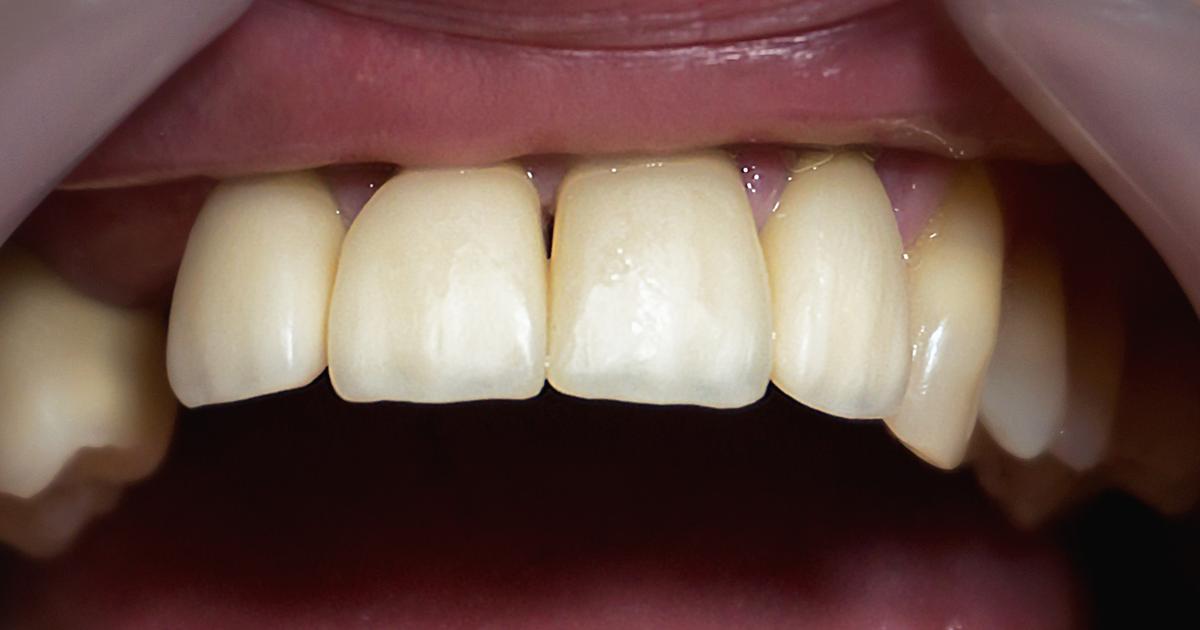
Receding gums are a serious sign of gum disease. With this condition, the affected individual's gums move away from the surface of their teeth, causing the rooted surfaces to become exposed. Individuals will notice these surfaces are much darker than the rest of their teeth because they aren't covered by protective enamel. Receding gums are always a sign of gum disease, and they indicate gingivitis has become periodontitis. If patients don't receive treatment promptly, they could lose their teeth. Varying treatments are available, but the best one will depend on how serious the loss of tissue is. Early treatment is crucial for a good outlook.
Several factors can lead to receding gums, including brushing too aggressively, resulting in damage to the gums. A hardened buildup of plaque can also cause gum damage. Smoking and a family history of gum disease both increase an individual's risk of receding gums. Certain illnesses like HIV and diabetes can lead to receding gums as well. If patients have medication that causes dry mouth, their risk of receding gums becomes higher because their saliva isn't breaking down food the way it should.
Loose Or Shifting Teeth
Loose teeth and shifting teeth are both signs of gum disease. When the gums pull away from an individual's teeth, they create pockets that aren't supposed to be there. The deeper these pockets get, the more serious and advanced the disease is. Bacteria can grow inside and infect these pockets. Part of how dentists diagnose gum disease is by feeling the pockets to check their size. Since the gums aren't keeping the teeth in place, they begin to loosen or shift. If individuals notice a change in their biting pattern, such as their teeth not fitting together how they usually do, this is cause for concern even if their teeth don't feel loose. Shifting teeth indicate periodontitis is progressing rapidly. The tooth tissue becomes destroyed, causing the teeth to be less solidly attached to the jawbone.
Deep Pockets Between The Gums And Teeth
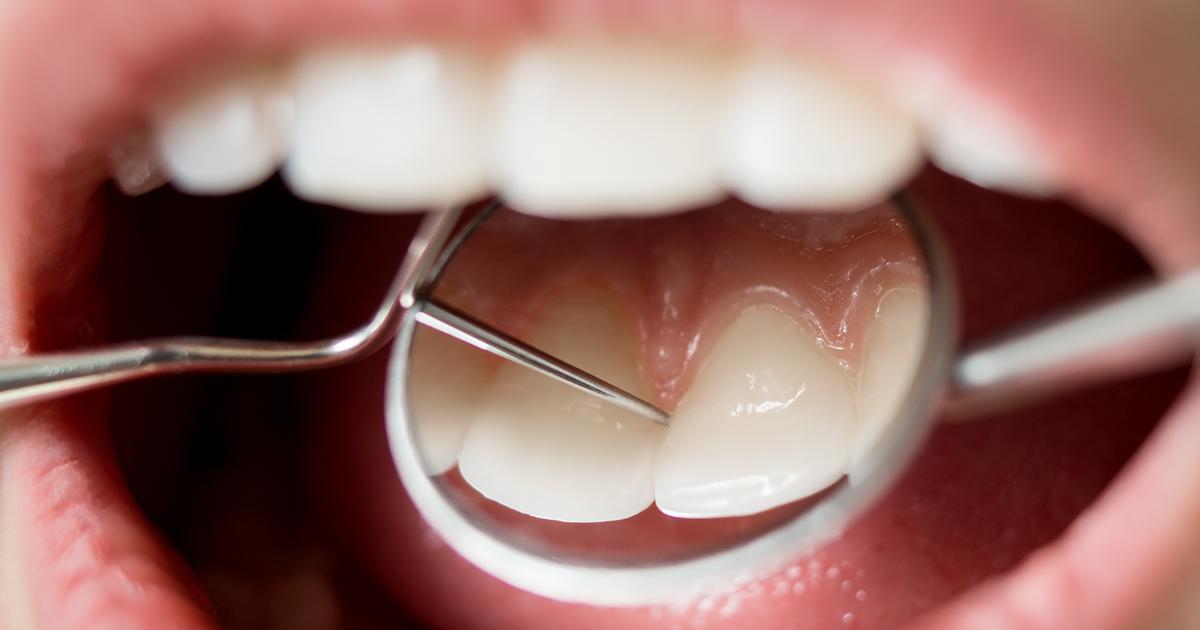
Gum disease can sometimes lead to deep pockets between the gums and teeth, especially when the disease becomes advanced. The gum and bone tissue are meant to be snugly fit around the teeth. As the gums recede and gum tissue is destroyed, this snug fit becomes looser and pockets form surrounding the teeth. When the gum disease continues without treatment, the pockets grow deeper. The deeper they get, the larger the area in which bacteria can fester becomes. When bacteria get inside the gums in places a toothbrush can't reach, they can cause the gum disease to accelerate even faster. In some cases, the tissue destabilizes to a point where there's enough bone loss that the teeth need to be removed. A dentist or periodontist will typically measure a patient's tooth pockets. To prevent further damage from being caused, the dentist will make a plan to remove existing bacteria and minimize the depth of the pockets.
Changes In Bite
When individuals are dealing with gum disease, they might experience changes in their bite as the disease becomes more advanced. Shifts to one's bite can be a sign of several different dental issues, gum disease being just one of them. Patients will notice a change in their bite if their top and bottom teeth aren't aligning properly like they used to, or that it's harder to close their molars together as they bite down. Bite changes sometimes occur due to a wearing down of the teeth. If individuals grind their teeth, clench their jaw, or chew on their tongue, their teeth are more likely to wear down faster. Wearing down the enamel can cause tooth decay and gum disease to progress more rapidly. When the changes aren't related to the teeth themselves, they may be caused by a problem with the hinges of the individual's jaw. Patients might also experience bite changes if their wisdom teeth push their other teeth around, and this shifting can lead to the onset of gum disease.
Pus Coming From The Gums

If individuals notice pus coming from their gums, they should see a dentist right away. Pus in the gums is a sign of a serious bacterial infection called a dental abscess. This typically happens in cases of gum disease where bacteria has gotten into the cavities and pockets of the gums and teeth. Oftentimes, the bacterial infection will accumulate inside the soft tooth pulp. Bacteria can be traced back to plaque. If the plaque isn't regularly cleared from the gum line and the teeth, it can destroy the gum tissue and get underneath the teeth into places a toothbrush won't reach. Three kinds of dental abscesses exist: periapical, periodontal, and gingival. The infection site will often be painful, and patients might have a fever and a bad taste in their mouth. Some abscesses must be treated with a root canal surgery. When dealing with pain from a dental abscess, the best thing individuals can do is avoid cold foods and drinks. It also helps to use an extra soft toothbrush to avoid aggravating the site.
Hard Buildup Of Tartar And Plaque
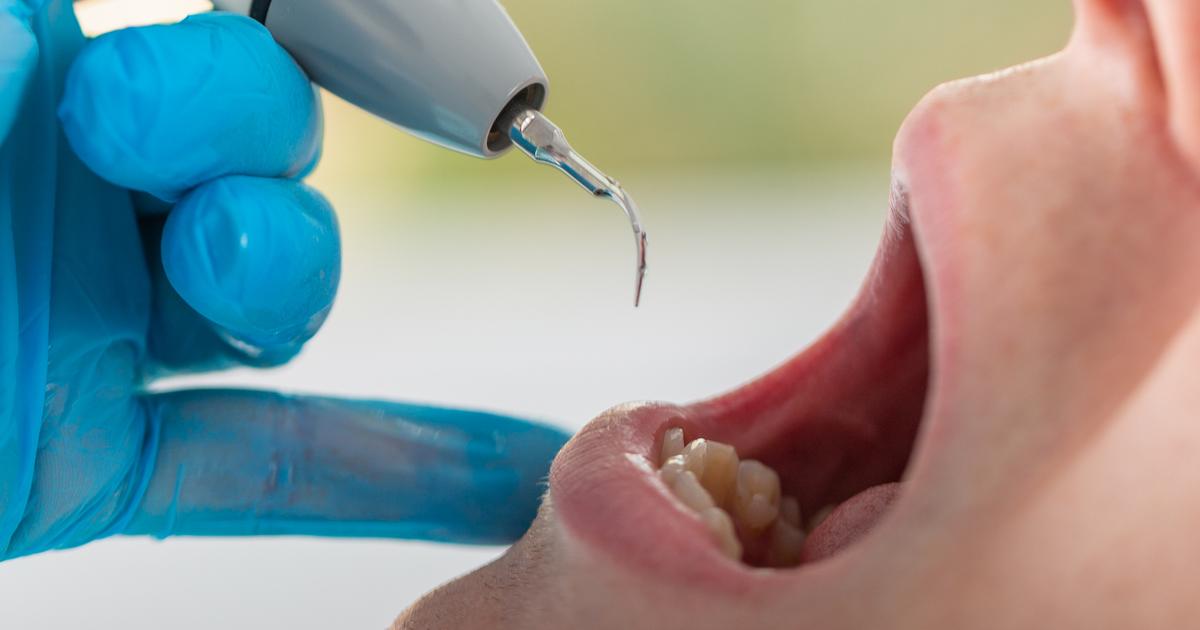
A hard buildup of tartar and plaque can be contributing to gum disease. Tartar is best removed by a dental professional, as it's more difficult to get rid of than standard plaque. Tartar builds up on the teeth when plaque and the minerals found inside saliva harden. In addition to coating the outside of the teeth, tartar can also move below the gum line, which destroys gum tissue and contributes to gum disease. The texture of tartar is similar to a crusty blanket over the teeth. Since the substance is porous, it can be stained by food and drink. Deposits of tartar tend to be brown or yellow, and they're often found between and behind the teeth. Plaque and tartar can lead to bad breath because of the bacteria inside. They can also destroy enamel and gum tissue, which leads to tooth and gum decay. In advanced cases, the tooth decay may become serious enough that an individual suffers tooth loss. Individuals with tartar buildups should get a professional cleaning and analysis.
