Warning Signs Of Inflamed Gums
When thinking about dental health, individuals typically focus on cavity prevention. However, the gums are just as important for maintaining oral hygiene, and failure to take proper care of them can result in a variety of gum diseases. In many instances, inflamed gums are a sign of a problem, such as disease or infection. Whatever the cause, steps can be taken to prevent, treat, and minimize damage and pain. Keeping an eye out for the following red flags can ensure a diagnosis occurs early-on and effective treatment can begin quickly. If an individual notices any of the following warning signs of inflamed gums, they should visit the dentist as soon as possible.
Bleeding Gums
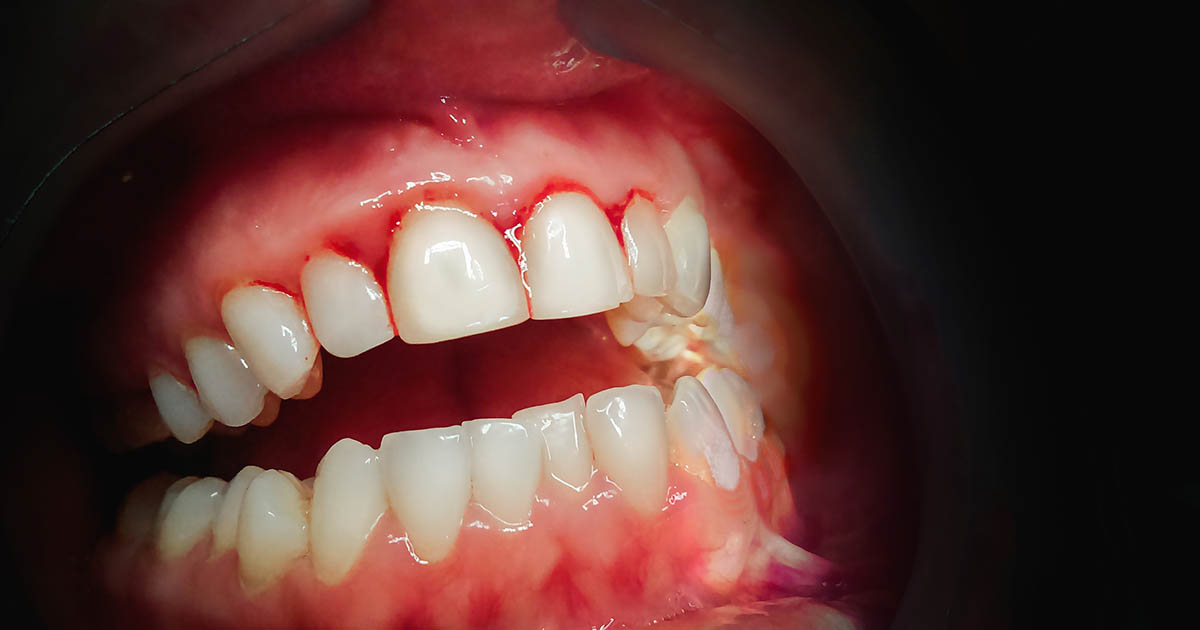
Healthy gums will not bleed when an individual eats hard foods, brushes their teeth, or during flossing. It's normal to accidentally press too firmly while flossing from time to time, causing a bit of blood to drip between the crevices of the teeth. However, if an individual notices blood coming from the gums regularly and seemingly without a cause, it's likely due to bacterial build-up along the line of the gums. This can lead to inflammation of the gums, gingivitis, and, eventually, periodontitis, which must be taken very seriously. Thus, booking an appointment with a dentist as soon as possible when dealing with inflamed, bleeding gums is crucial.
Mouth Sores
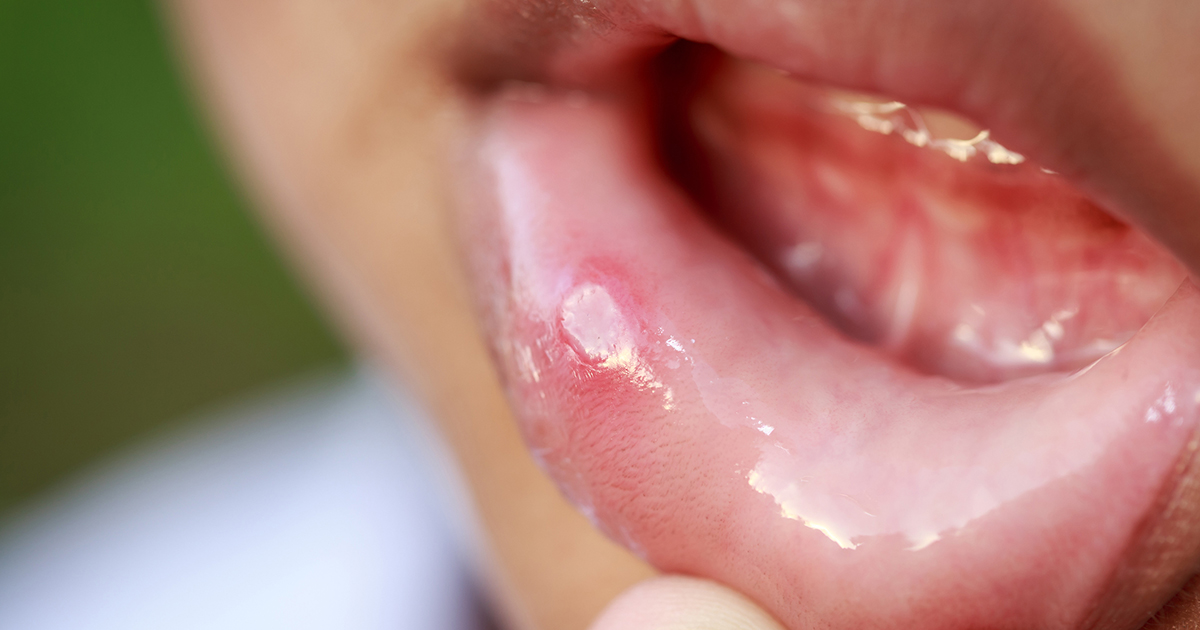
Uncomfortable, unsightly, and often painful, mouth sores are another warning sign of inflamed or infected gums. They can arise in any part of the mouth, from the roof to the cheeks and even the lips. Mouth sores can begin with redness and swelling along the lining of the mouth or develop as single ulcer-like holes. These ulcers occur when the top layer of cellular tissue breaks down, causing a painful opening in the tissue. Some appear red, while others are white due to food debris and dead cells. Some mouth sores are more blister-like, raising from the tissue in mounds filled with a clear fluid. Canker sores may also develop. But no matter what kind of mouth sore they are, their presence can indicate inflamed gums, along with viral or bacterial infection.
Bad Breath

Halitosis, more commonly referred to as simply bad breath, is another common sign of inflamed or diseased gums. Odor-causing bacteria that remain in the mouth after eating, smoking, or due to general poor oral hygiene can multiply and reproduce, negatively affecting the gums. Experiencing a persistent bad taste in the mouth can also be symptomatic of bad breath. However, some individuals may not notice an unpleasant taste; rather, they can smell an odor that, despite brushing the teeth and using mouthwash, just won't disappear. While many habits, such as smoking and drinking coffee, will cause bad breath, individuals who notice it under seemingly inappropriate circumstances should head to the dentist.
Recessed Gum Tissue

Recessed gum tissue is perhaps the strongest indicator the gums are inflamed and possibly infected. Normal, healthy gums border the teeth with plush, pink tissue. When this tissue begins to recede, the teeth appear to lengthen and the lining border becomes thinner. Recessed gum tissue is caused by a bacterial infection that gradually eats away at and destroys the tissue. Gum tissue is unlike other tissues in the body since, once the tissue is gone, it cannot regenerate itself and grow back. However, the process can be slowed down or even stopped with the proper dental care, so patients should consult a dentist at the earliest sign of gum tissue recession.
Red And Swollen Gums
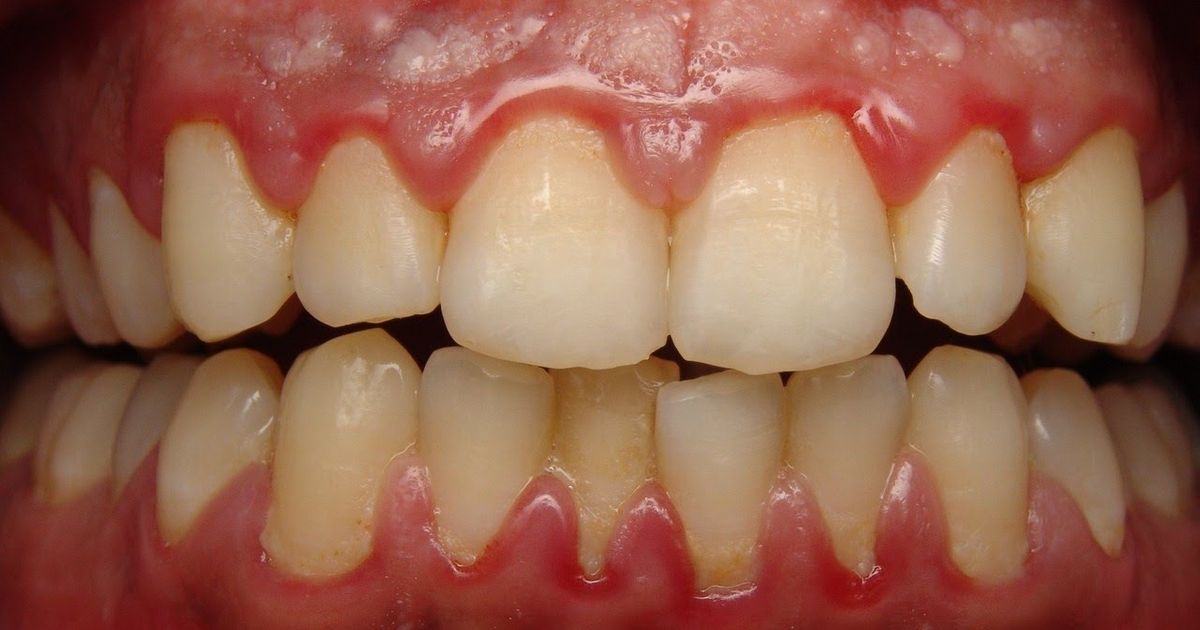
Normal gum tissue is pink, slightly plump, and free from pain. When the coloring or structure of the gums begins to change, patients should be alerted to the possibility of inflammation or infection. Red and swollen gums are another common and easy to spot indicator of an oral hygiene issue. The change in color and painful inflammation can result from the gums attempting to eject bacteria or fight against infection. If the infection is not fought off or treated, it can lead to complete degradation of the gums, damage to the bones, and even eventual tooth loss.
Increased Sensitivity

Patients who have inflamed gums often notice increased sensitivity when eating or drinking. They may experience sharp pain or a tingling sensation that could affect a single tooth, one particular side of the mouth, or several teeth on both sides of the mouth. Some individuals can experience sensitivity throughout the entire mouth. Typically, increased sensitivity is most pronounced when eating ice cream or other cold foods, and patients may also be sensitive to hot foods such as soups. Many individuals with inflamed gums have pain when drinking cold beverages, especially drinks that contain ice. Sometimes, a blast of cold air that hits the teeth could trigger discomfort in individuals with sensitive teeth and gums.
Since increased sensitivity could sometimes be a sign of a more serious dental issue, patients who experience this symptom should see a dentist to determine the cause. To reduce pain and make teeth less sensitive, dentists may be able to apply a solution to the affected teeth, and different kinds of toothpaste, gels, and rinses designed to reduce sensitivity might be recommended for use at home.
Painful Brushing Or Flossing

Individuals with sensitive teeth and gums often experience painful brushing or flossing, and this can happen even for patients who have mild sensitivity. Patients might notice brushing over certain teeth or along particular areas of the gum line causes twinges of sharp pain. For some individuals, this sensitivity might occur over large sections of the mouth, and it could happen every day or only occasionally. Flossing may be especially painful for patients with sensitivity, and the pain is normally most severe at the gum line. To make brushing and flossing less painful, patients should use a brush with soft bristles and a round brush head, and using an electric toothbrush can provide a deeper clean than a manual toothbrush without being rough. Nylon bristles tend to be less harsh than other bristle types. Brushing with a back and forth motion is recommended, and patients need to ensure they brush gently over the site of the sensitivity. When flossing, a slow motion should be used to insert the floss between each tooth; it should not 'snap' into place. Using waxed floss can make it easier to insert the floss in areas that may be painful or hard to reach. Over-the-counter toothpaste is available to gradually reduce tooth sensitivity over time, and brushing twice a day could provide significant relief. Patients may also wish to use a toothpaste designed to heal damaged gums.
Uncomfortable Eating

Uncomfortable eating can make it difficult for patients with sensitive teeth to enjoy certain foods and drinks, and it could also make it hard for them to obtain adequate nutrition. Some individuals might find they are only able to chew on one side of their mouth, and trying to eat hard foods such as potato chips or crackers could cause significant pain. Patients with severe sensitivity could even feel they are unable to attend or find pleasure in social situations that involve eating. To ease the discomfort of eating with tooth sensitivity, patients might want to use a topical anesthetic on the sensitive areas a few minutes before eating a meal. Eating soft foods such as mashed potatoes or puddings could help, and avoiding piping hot meals and icy cold foods could be beneficial as well. Patients who experience uncomfortable eating regularly should speak to a dentist or physician about treatments and ways to obtain necessary nutrients.
