What To Expect From A Pancreas Transplant
A pancreas transplant is a surgical procedure to normalize an individual's blood glucose by removing diseased pancreatic tissue and replacing it with pancreatic tissue from a donor. A pancreas transplant is not a common surgical procedure and is only utilized in cases where other methods of treatment have been ineffective, and it is a last resort. Most pancreas transplants are performed on patients who have uncontrollable type 1 diabetes, but they also may be done on those with type 2 diabetes and some forms of cancer.
The donor pancreas tissue typically comes from an individual who is alive physically but has been declared brain-dead. The pancreatic tissue that is transplanted has to match certain criteria to ensure it is immunologically compatible with the recipient's body. Just like any other organ transplant, there is a risk the patient's body will reject the transplanted pancreatic tissue.
Why It's Done
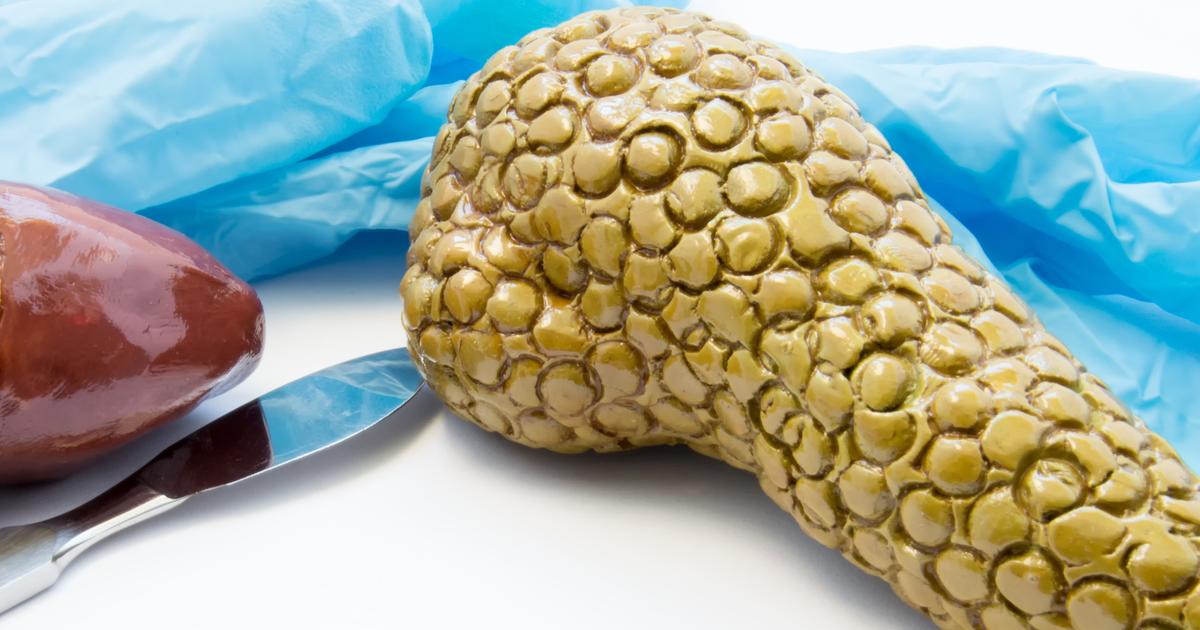
A pancreatic transplant is a procedure performed to restore function to an individual's pancreas. In rare cases, pancreatic transplants are performed on patients who have had to have their entire pancreas and possibly other organs removed due to a malignancy. However, most individuals who are candidates for a pancreas transplant procedure have type 1 diabetes that has caused numerous complications that affect several other organs and organ systems in the body. These complications usually include kidney damage, eye problems, and nerve damage.
Individuals who have a pancreas transplant tend to have diabetes that cannot be controlled even with the most diligent attempts at medical treatment. Pancreas transplants are most common among diabetes patients who have developed atherosclerosis or heart disease as a result of their diabetes. A pancreas transplant makes it possible for a diabetes patient to be able to live without taking daily insulin injections. A transplanted pancreas also allows the patient to consume a normal diet and reduces their future risk of kidney, nerve, and cardiovascular damage.
Types Of Transplants
Some individuals who have experienced complications from diabetes that involve damage to their kidneys may need to have what is called a simultaneous pancreas and kidney transplant or a surgical procedure where the pancreatic tissues and a kidney are replaced at the same time. When a patient who needs a pancreas transplant progresses into end-stage renal disease, a pancreas after kidney transplant may be needed. In such cases, the transplantation of the kidney is performed before the pancreas because a living kidney donor is being used. Following the living donor kidney transplant, the patient waits until a donor transplant from a deceased individual to become available.
The factors that determine what type of pancreatic transplant a patient will need depends on their health and the amount of time they can afford to wait for donor organs to become available. On average, a patient who undergoes a simultaneous kidney and pancreas transplant has a waiting time of one to two years. An individual who needs to have a pancreas transplant alone may have a wait time that exceeds two years. An average wait time of over two years is also typical in patients who undergo a pancreas after kidney transplant.
How The Procedure Works
During a pancreatic transplant, the patient will be put under general anesthesia. The surgeon makes an incision down the middle of the abdomen and then places the new donor pancreas and a trivial segment of the donor's small intestine into the recipient's abdominal cavity. The recipient's small intestine or bladder is attached to the segment of the donor's small intestine, and the vessels that supply the legs with blood are attached to the donor pancreas. The diseased pancreas is typically left in its place unless it has already been removed or contains a malignant lesion.
At this point, the surgeon connects blood vessels to the donor's kidney in recipients receiving a simultaneous kidney and pancreas transplant. The donor kidney ureter is then secured to the recipient's bladder, and the old kidney is left in place unless it contains a malignant lesion, causes infection, or produces high blood pressure. The pancreatic transplant usually has a length of between three and six hours. The results of a pancreatic transplant are immediate, and recovery from the procedure can take between one and two months.
Risks Of The Procedure
A pancreatic transplant is no exception to the standard of surgical procedure-related risks a patient should be aware of before undergoing this surgery. Uncommon but significant complications can occur with a pancreatic transplant, including the development of blood clots, excessive bleeding, development of infection, high blood glucose or other metabolic issues, frequent urinary tract infections, leakage of urine, failure of the donor pancreas, and rejection of the donor pancreas.
Some risks come along with the medications that must be taken for life following the transplant to prevent the recipient's body from rejecting the donor pancreas. Osteoporosis or bone thinning, frequent nausea, diarrhea, sensitivity to sunlight, frequent vomiting, high blood pressure, and high cholesterol are side effects that may occur with anti-rejection medications. More possible side effects include excessive loss of hair, swollen gums, puffiness, excessive growth of hair, frequent acne breakouts, and weight gain.
Recovery Process
Following a pancreatic transplant, the patient will remain in the intensive care unit of the hospital to have close vital monitoring for several days. Once the patient's vitals balance out and their body reaches a stable state, they are moved into the transplant recovery unit. The patient stays in the transplant recovery unit of the hospital for around a week to help control their pain and begin the recovery process. Following discharge from the hospital, the patient will be closely monitored by their physician for a period of between three and four weeks and must stay in a location close to the transplant center during this time.
Even after the patient has fully recovered from their pancreas transplant, they will need to take immunosuppressive medications for the rest of their life. This mechanism ensures the patient's immune system is unable to attack and reject the donor pancreas. Patients who experience high blood pressure and frequent infections following their transplant may need to stay on additional medications for the long term.
