Why Everyone Should Be Aware Of Plantar Fasciitis
Plantar fasciitis can happen to anyone, from an active runner or athlete to a worker who is on their feet all day. Many may not be aware, but the foot is made up of numerous complex tissues, muscles, and bones that can become damaged quite easily if the foot is not properly cared for. The foot has a thick, fibrous band of tissue called the fascia that reaches from the heel to the toes and provides support to the muscles and arch of the foot. When this tissue becomes overly stretched, tiny tears can occur on the surface, resulting in pain and inflammation.
What Causes Plantar Fasciitis?
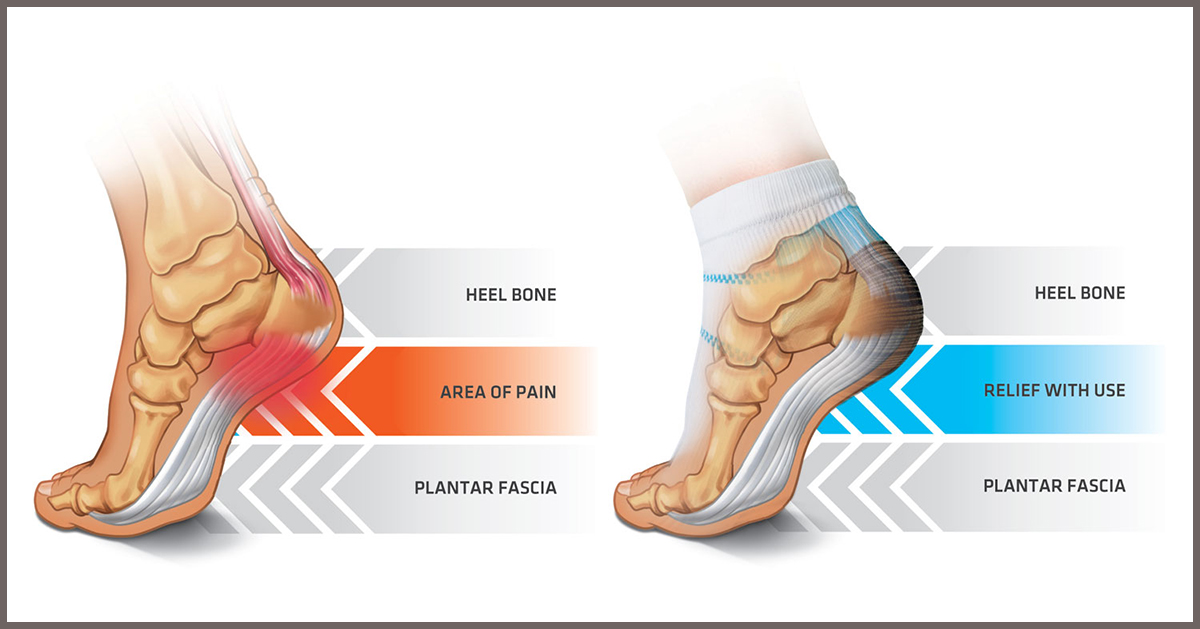
Plantar fasciitis is described as a painful condition predominantly caused by inflammation of the bands of tissue connecting the heel to the toes. Numerous factors can contribute to an individual developing plantar fasciitis. While men can developing this condition, it is more often seen in women, as well as individuals who are older, overweight, who are on their feet for several or more hours a day, have an unusual walk, or have an atypical foot position.
Plantar Fasciitis Support Compression Socks are recommended for individuals looking to relieve pain and reduce soreness. There is no definite cause for plantar fasciitis, as anyone can develop it from active runners and athletes to fast-paced workers, but certain individuals are more at risk if they meet some of the above criteria.
Structural Risk Factors

In terms of foot structure, individuals are more at risk of developing plantar fasciitis if they have one of the following foot structures. The first, as many might suspect, is a flat foot. The arch in the typical foot protects the plantar fascia and enables it to manage the demands of daily use. A flat foot, unfortunately, puts the plantar fascia under additional stress when walking and may cause small tears, which can eventually result in the irritation and inflammation associated with plantar fasciitis.
Extremely high arches, another abnormality in foot structure, also puts more stress on the plantar fascia. Individuals are also at an increased risk of developing plantar fasciitis if they have tight Achilles tendons (heel cords), once again because of the stress tight Achilles tendons put on the feet.
Shoes And Plantar Fasciitis

Shoes play a larger role in an individual's risk of developing plantar fasciitis than many realize. For one, individuals with flat feet often need specialized shoes, ones with more supports, or even orthotic inserts. Individuals who wear worn-out shoes or ones with thin soles are not getting the support they need to prevent putting too much stress on their plantar fascias, particularly if they have flat feet, which greatly increases their risk of ending up with plantar fasciitis.
In addition, individuals who wear high heels quite a lot, particularly if it is for extended periods at a time, are putting more stress on their foot as they continue to walk. It is this additional stress that, as is evident by this point, significantly boosts the risk of plantar fasciitis.
Diagnosing Plantar Fasciitis
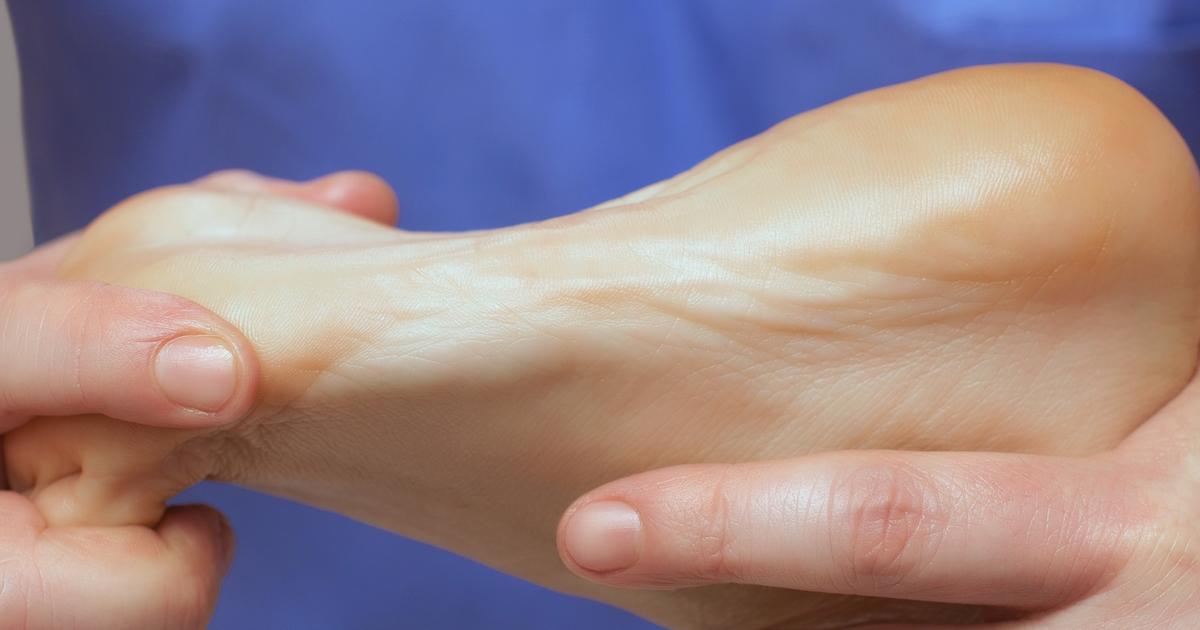
In diagnosing plantar fasciitis, doctors normally begin with a health history and physical examination. During the health history, doctors will ask the patient questions about the location of their pain. The patient may also be asked about whether the pain is worse in the morning and if it increases with prolonged standing. This information could help the clinician distinguish between plantar fasciitis and other foot conditions. During the physical exam, the doctor will gently palpate the patient's foot to check for any areas of tenderness.
The painful foot may be compared to the unaffected foot. The physician might bend the patient's toes up toward their shin to see if this causes any pain, and they will also feel along the bottom of the patient's foot. While x-rays and other imaging studies are not typically indicated, they could help the doctor eliminate other conditions such as tarsal tunnel syndrome, stress fractures of the heel bone, and reactive arthritis.
Signs & Symptoms To Look For
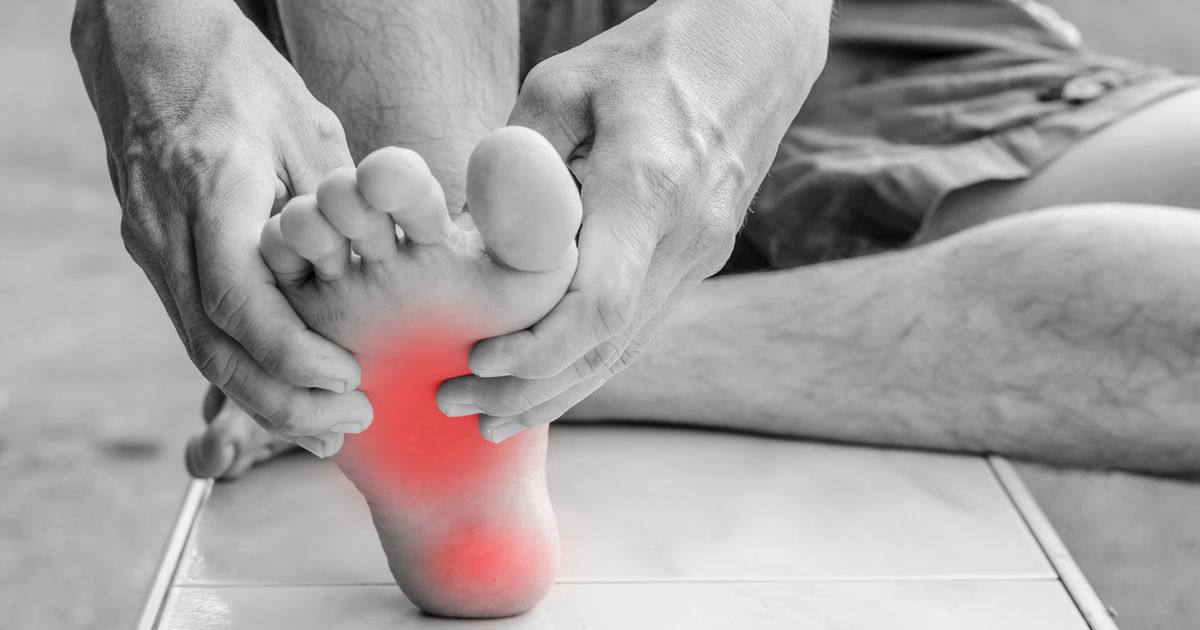
The most predominant symptom patients will experience when it comes to plantar fasciitis is pain in the bottom of their foot, or at the front or center of the heel bone. For some individuals, they might notice the pain is excruciating and at its worse first thing in the morning, known as 'first-step pain.' Pain can also occur when the patient is standing after having sat for a long time, and right after exercise as well. Topical treatments can be used at this time to reduce pain.
A physician can typically tell if a patient has this condition by checking for tender areas in the foot, and can often pinpoint what is causing the pain based on its location. In rare instances, a doctor may suggest an X-ray or MRI to rule out other conditions, such as a pinched or compressed nerve or stress fracture within the heel. However, in most cases, a doctor can diagnose an individual with plantar fasciitis by just examining their foot and location of their pain.
Treatment Through Medication

Fortunately, plantar fasciitis normally will relieve itself after a few months, but resting and taking over-the-counter pain medication can alleviate swelling and help patients feel more comfortable. However, individuals dealing with this condition should consult their doctor if their condition does not improve or if they notice redness or bruising on the heel.
Medications used to treat this condition include nonsteroidal anti-inflammatory drugs to ease the pain and reduce inflammation. Steroid injections are taken if the pain is severe and the patient does not respond to prescribed medications. The steroid is injected into the most painful part of the plantar fascia, and will help to ease the pain for approximately a month but can keep inflammation at bay for even longer.
Apply Compression

An excellent way to relieve the pain and speed the healing of plantar fasciitis is to compress the affected area. Compression helps increase blood flow (improving circulation) to the affected area, which permits the plantar fascia to stretch and loosen, thus relieving the pain associated with this uncomfortable condition. Compression can also provide additional support to the foot and plantar fascia in particular, which makes walking much easier.
One of the best ways to use compression when dealing with plantar fasciitis is to wear compression sleeves or socks. These can be worn both during the day as well as at night, which provides the pain relief and healing on demand. In fact, reports indicate wearing compression socks at night is the best time to heal plantar fasciitis! Yes, compression sleeves and socks do work when individuals are inactive and lying down.
Rest And Ice

Perhaps the simplest methods of managing plantar fasciitis, and the first methods individuals should turn to, are resting the foot and icing the affected area. When plantar fasciitis develops, patients can immediately start to relieve some of their pain by avoiding the activities that make their feet hurt (so cutting down on sports). Patients should also consider avoiding running or walking on hard surfaces (e.g., concrete).
When resting their feet, patients can begin to reduce the inflammation and continue pain relief by placing an ice pack or similar cold compress on the affected area. Cold compresses and ice have long been known to reduce inflammation and pain from countless injuries, including plantar fasciitis and conditions such as sprained or twisted ankles, sore jaws, stubbed toes, and banged-up knees.
Physical Therapy And Stretching

If medication, rest, compression, and ice do not seem to ease pain and inflammation, physical therapy is the next best step, as the patient will learn exercises to stretch and strengthen the plantar fascia, Achilles tendon, and lower leg muscles. Physical therapists also typically recommend patients to wear a night splint, which can be used while they are sleeping to hold the plantar fascia in a better position for healing. In addition to recommending night splints, physical therapists also often employ contrast baths, massage, and ultrasonography during sessions with patients to promote long-term healing of plantar fasciitis.
Surgical And Medical Treatment Options
If treatment does not yield positive results after several months, a doctor can recommend a more involved procedure or even surgery. These options include shock-wave therapy, Tenex procedure, and surgery. Shock-wave therapy is a form of therapy that literally shocks the patient's plantar fascia with sound waves, as this stimulate blood flow in the foot and helps the damaged tissue to heal. It also stuns the nerves to stop the pain.
The Tenex procedure is when the doctor makes a small incision is made and uses an ultrasound to target and remove scar tissue, allowing the patient to get back to their routine within a week or so. Surgery is the final option, and the operation focuses on removing the plantar fascia from the heel bone. The patient may need to wear a boot or splint after surgery and not put any weight on their foot for a period.
Unproven Plantar Fasciitis Treatments
The standard treatment options for plantar fasciitis, as discussed, normally consist of anti-inflammatory medication, physical therapy, rest, and wearing a brace or orthotics. Steroid injections, extracorporeal shock wave therapy, and Tenex procedures may also be effective for certain patients. Despite the abundance of safe treatment options, there are numerous unproven plantar fasciitis treatments that could cause harm to patients and exacerbate symptoms. Injections of both botulinum toxin and platelet-rich plasma are currently unproven treatments, and they are considered controversial.
Prolotherapy, an alternative medicine practice that relies on injections of a variety of substances selected by the clinician, is also unproven. Although dry needling is currently being investigated as a possible treatment for plantar fasciitis, studies have suggested it has limited effectiveness. The technique is similar to acupuncture, and it involves inserting a thin needle directly into the affected muscle to release trigger points. Experts state many of the studies on dry needling are not of a high enough scientific standard to conclusively determine whether this treatment is beneficial in plantar fasciitis or not.
How To Prevent Plantar Fasciitis

The following preventative steps can help to stop plantar fasciitis from developing or from the condition from worsening. First, individuals should take care of their feet by wearing shoes with good arch support and heel cushioning that provide the feet with proper support. ConsiderGravity Defyershoes for pain relief of plantar fasciitis and foot pain. Doing exercises to stretch the Achilles tendon at the back of the heel is essential before sports or for non-athletes. Staying active, maintaining a healthy weight, and establishing good exercise habits all are things individuals can do to prevent plantar fasciitis.
Runners should alternate running with other sports that do not cause heel pain, and avoid going barefoot or wearing slippers can greatly help, as the feet are not receiving the proper support they need in these instances. Lastly, individuals can apply ice to wherever they are experiencing pain for fifteen to twenty minutes three or four times a day, or after an activity, as ice can help to reduce pain and inflammation associated with the condition.
Complications Of Plantar Fasciitis
The potential complications of plantar fasciitis vary depending on how long the patient may have gone untreated. If this condition is ignored for a while, the patient could experience chronic heel pain that might interfere with their daily activities in the long term. Running could become extremely painful, and walking might be difficult too. Some patients try to change the way they walk in order to mitigate the pain and other symptoms of this condition. However, making alterations to one's gait could cause other problems with the foot, and it may cause some individuals to develop issues with their knees, hips, and back.
There is also a risk that the patient's plantar fasciitis might progress to plantar fasciosis, a related condition that needs a different set of treatments. If the patient develops severe plantar fasciosis, they may need surgery to relieve the pressure on the fascia. To reduce the risk of complications from plantar fasciitis, patients should always follow the advice of their specialists and physical therapists.
